Prepare
Every university has its own general practice teaching protocols. These vary in length of placement, experience and level of student, payment and rostering, what they expect from the student and practice, and administrative and educational requirements. Research this and make sure it fits with your practice.
Decide in advance what you think you want to teach and how; you will know your own strengths and weaknesses, both in terms of knowledge and style. Universities are very keen for their students to receive quality teaching and are generally very supportive, so you can also call on their resources.
Develop your own curriculum. Dr Alice's example of an in-house curriculum is shown in Figure 1.
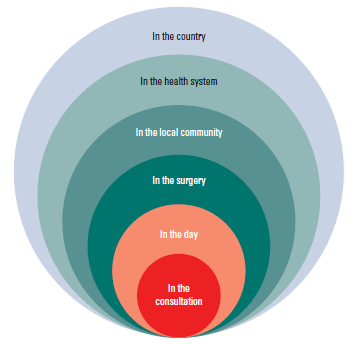
Figure 1. Dr Alice's medical student teaching curriculum
In the consultation
- Communication
- How to build rapport
- Language – use of jargon, use of 'scripts' for common problems
- Use of humour and tone
- Signposting through a consultation
- Blocking behaviours: purposeful and nonpurposeful
- How to summarise and reflect
- Structure
- Consultation structure – openers and the space before openers
- Eliciting patient concerns 'Is there anything else?'
- Patient expectations – 'statements of orientation'
- Winding up: 'Are you happy with that?'
- Acute/chronic phase of chronic disease management
- Clinical
- Paediatric development
- Immunisations and the 'anatomy of a vaccination consultation'
- Autism
- Asthma
- Diabetes
- Ischaemic heart disease risk factors – hypertension, dyslipidaemia, risk factor calculators
- Depression
- Mental state examinations.
In the day
- Time management
- Appointments and booking.
In the surgery
- Use and role of registered nurses and team care management
- Interaction with the front desk
- Interaction with other doctors.
In the community
- Aged care facility visits and home visits
- Interaction with pharmacies
- Use of allied health
- Referring to specialists
- Interactions with hospitals and emergency departments.
In the Australian healthcare system
- Medicare and billing
- What different doctors earn
- GP training and career pathways
- Different types of general practices
- History of Australian general practice
- Interaction with pharmaceutical and representatives visits
- What we spend on health and how
- What we spend on the Pharmaceutical Benefits Scheme (PBS)
- The seven 'national health priorities'.
Dr Alice was very organised and Dr Greg found her a little intimidating. He actually didn't understand some of the terms in her curriculum. She reassured him this didn't matter as it was her curriculum, but she did suggest he use the overall structure as she found it worked quite well. She also explained that she had a particular interest in communication techniques and paediatrics, whereas Dr Greg's strengths were in musculoskeletal problems and geriatrics, so his curriculum should reflect more of those areas.
She suggested he develop his own list and print it out at the beginning of the placement, get the student to bring it in each day, and if an opportunity to discuss a topic appeared, get the student to tick it off the list. She kept on using the word 'structure'. Dr Greg was still intimidated.
A few weeks later, Dr Alice met up with Dr Greg, who had developed his own curriculum. Actually, he was quite chuffed with himself! He hadn't realised how many topics he could confidently talk about until he had written them out within a structured format. However, just as his confidence was rising, Dr Alice outlined her next phase.
Implement
Dr Alice explained that it is all very well to know what you want to talk about, but you also need to know how you are actually going to do it. She explained that most of the time, medical students in general practice are sitting in the corner of a consultation room, not really understanding a lot of the subtleties going on. The best way for them to learn is for them to get involved and actually do stuff. We learn best by doing.
However, the realities of general practice often get in the way of this. 'We can't just stop what we are doing and go "blah blah blah: about diabetes and asthma," we've got patients to see,' protested Dr Greg. Dr Alice pointed out that 'you know, you can actually use these usually clever young things to your own advantage and also make their learning experience so much better.' Dr Alice explained her methods.
You first need to think about what you want and also what they want, as described in Table 1. Dr Alice explained she had developed this plan over many years and reassured him that he would be fine.
Dr Greg now felt armed and ready. He had his curriculum and he had informed his colleagues and staff about how he was going to implement the process.
When his first medical student arrived the next day, Dr Greg found he was nothing like Alistair. Actually, Rob was very keen. He turned up early, wanted to be either a GP or a paediatrician, and was great with the patients, especially the kids. Rob was pleasantly surprised Dr Greg had gone to so much effort and really liked the idea of the in-house curriculum.
Dr Greg found that while initially it was a little hard to 'let go' of his patients and prompt them into speaking with Rob first, this effort paid a handsome dividend. It was like having an intern. Rob actually contributed, loved being able to actually do something, and the patients seemed to like it. This teaching stuff was not so bad afterall!
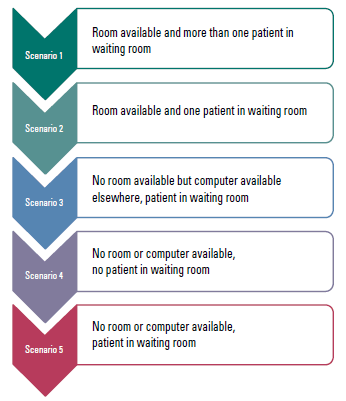
Scenario 1. Room available and more than one patient in waiting room
- MS takes second patient into spare room after doctor informs patient and obtains consent: MS looks at notes
- MS takes history and appropriate examination, enters notes into patient file and develops suggested management plan
- When doctor is ready for patient, doctor buzzes room, MS closes notes and brings patient in
- Doctor reads MS notes and MS presents findings to doctor
Scenario 2. Room available and one patient in waiting room
- Doctor and MS see patient: take history, examine, enter notes, suggest management plan. Otherwise, MS observes doctor seeing patient
Or:
- MS goes through history of next patient and if that patient arrives before doctor finishes current consultation, asks the patient's permission to take them into another room and do the 'work-up'
Scenario 3. No room available but computer available elsewhere, patient in waiting room
- Doctor and MS see patient together, and if time allows, MS takes history, examines, enter notes, suggests management plan and presents to doctor. Otherwise, MS observes doctor seeing patient
Or:
- MS goes over history of the next patient
Scenario 4. No room or computer available, no patient in waiting room
- Doctor and MS take go through the curriculum, do role plays; otherwise MS presents previous patient's findings to doctor
Scenario 5. No room or computer available, patient in waiting room
- Doctor and MS see patient together, and if time allows MS takes history, examines, enters notes, suggests management plan and presents to doctor. Otherwise MS observes doctor seeing patient
Figure 2. Different scenarios (in descending order of quality learning)
Table 1. Dr Alice's medical student teaching objectives
- To maximise learning process for medical student (MS)
- To minimise impact on teaching doctor and practice
- To maximise benefits to practice from teaching process
|
At start of placement
- Practice orientation and paperwork completed
- Orientation to clinical software (hopefully by nurse or administration staff)
|
At start of shift
- Appointment page to have the MS location entered
- Other doctors and nurses on shift to be sent a message before shift that the MS is present and to be alert to any interesting clinical presentations for the MS
- Supervising doctor to look through day-sheet to see what rooms are taken and when, and what patients are coming in that may be of interest (including the patients of other doctors/nurses) (Figure 2)
|
Conflict of interest: none declared.