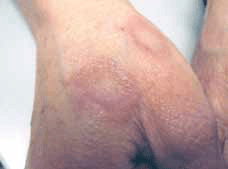
Figure 1. Ringed lesions with raised margins on dorsum of hands
Question 1
What are the differential diagnoses and why?
Question 2
Results of skin scrapings for fungal hyphae are not diagnostic. You empirically prescribe a topical antifungal cream twice daily for 4 weeks but there is no improvement. What do you do next?
Question 3
Pat uses some of her husband's high potency steroid cream, which led to a dramatic improvement. What is the most likely diagnosis?
Question 4
What is the most appropriate management and prognosis?
Answer 1
The differential diagnoses of annular skin lesions include tinea corporis, a fixed drug eruption, granuloma annulare, erythema multiforme and erythema chronicum migrans.
Pat's contact with farm animals and soil may support the diagnosis of tinea corporis. Fixed drug reaction is possible with her recent use of citalopram. Granuloma annulare can mimic tinea corporis, with similar lesions that are sometimes clinically indistinguishable. Erythema multiforme typically presents with multiple annular lesions of variable sizes with erythematous margins and centres which classically resemble targets. Mucosal involvement is common and the patient is often quite ill. Erythema chronicum migrans presents with a solitary oval or quasi-annular erythematous rash with constantly extending margination and possible central clearing. It is due to acute infection with Borrelia burgdorferi bacteria from the bite of an Ixodes tick. Patients are usually systemically unwell.
Answer 2
Skin biopsy to confirm a diagnosis. Also consider changing citalopram to another class of antidepressant.
Answer 3
Granuloma annulare is the most likely diagnosis; a very potent topical corticosteroid can result in regression of both granuloma annulare and tinea corporis. However, in tinea corporis the lesions will often flare-up during or after a course of steroid treatment, which leads to a complicated form of tinea called 'tinea incognito'. For granuloma annulare, clinical improvement with potent corticosteroids has been described.1
Answer 4
The skin lesions were causing Pat stress and stigmatism and she requested treatment to expedite recovery. After considering the pharmacological options described for granuloma annulare,1 Pat was prescribed a combination of potent topical corticosteroid creams with a 6 month course of oral dapsone.
On review after 3 months, the annular lesions were almost completely resolved (Figure 2).
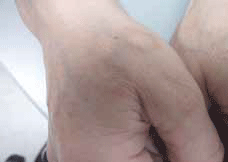
Figure 2. The annular lesions after 3 months treatment with topical corticosteroids and oral dapsone
Discussion
Granuloma annulare is a benign skin condition commonly diagnosed before 30 years of age, with a female-to-male prevalence ratio of 2.3 to 1.2 It can be subdivided into four clinical forms: localised, disseminated, subcutaneous and perforating. The localised and disseminated forms are the most common.2 The aetiology is unknown.
Associations with diabetes mellitus, viral infections such as human immunodeficiency virus (HIV) and Epstein-Barr virus (EBV) and lymphoma have been reported.1,2 Clinically, granuloma annulare presents as erythematous annular, semi-annular, papular or plaque lesions with central clearing. The lesions may be solitary or may number in the hundreds with a preferred distribution over trunk and limbs. They can be mildly pruritic and may progressively enlarge.
Histologically, it is characterised by layers of granulomas formed by histiocytes and epitheloid cells surrounding necrobiotic collagen bundles.3 Very rarely the subcutaneous variant of granuloma annulare can present on the penis,4,5 with 10 cases reported in the medical literature.6,7
Granuloma annulare is usually self limiting and resolves without treatment within 6–24 months.8 For the localised form of granuloma annulare, reassurance is often adequate. For more widespread and complicated lesions, various pharmacological treatments have been described including potent corticosteroid cream, cryotherapy, psoralen and ultraviolet A therapy, dapsone, infliximab, calcineurin inhibitors1 and a combination of rifampicin, ofloxacin and minocycline.9 Intra-lesional injection of steroids10,11 and interferon12 may also bring about resolution. Surgical removal is an option for nodular lesions of the subcutaneous variant of granuloma annulare.7,13
Key points
- Annular skin rash is a common condition seen in general practice, with tinea infection the most likely diagnosis.
- Poor response to antifungal treatment should prompt consideration of alternative diagnoses including granuloma annulare.
- Clinically, tinea infections may be difficult to distinguish from granuloma annulare and skin biopsy remains the definitive diagnostic procedure.
- Watchful waiting and reassurance is sufficient for localised granuloma annulare. For widespread and more complicated involvement, various pharmacological options are available with no consensus for best evidenced treatment. Topical corticosteroids and oral dapsone can be considered as first line treatment when indicated.
Conflict of interest: none declared.