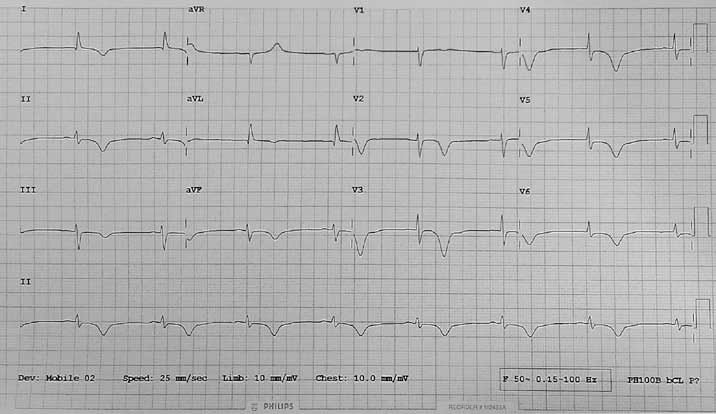
Figure 1. ECG showing deep T-wave inversion in all leads
Question 1
Based on the history and investigation findings, what is the most likely diagnosis? What are the differential diagnoses?
Question 2
Which of the following statements about Edith's troponin result is most correct?
- This degree of troponin elevation is always associated with acute coronary syndrome
- Edith's troponin result suggests that she was experiencing an acute myocardial infarction, as troponin testing has a sensitivity and specificity of almost 100%
- Troponin elevation of this level can be seen in almost all forms of myocardial injury.
Question 3
What features of Edith's history are associated with takotsubo cardiomyopathy?
Case study continued
Edith was transferred to a tertiary hospital where a echocardiogram confirmed an akinetic left ventricular apex with preserved basal systolic function. An urgent coronary angiogram (Figure 2) was arranged which revealed normal coronary arteries.
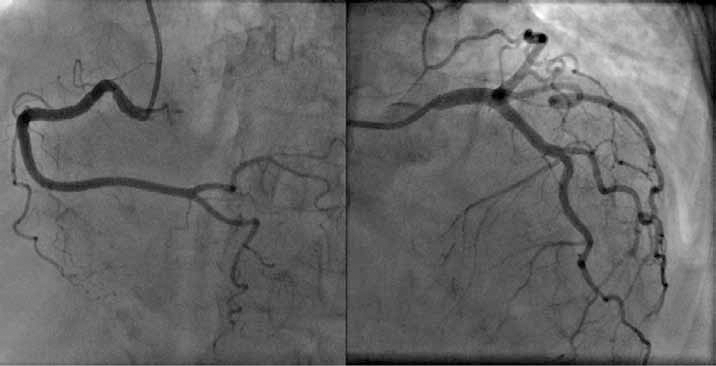
Figure 2. Angiogram showing normal coronary arteries
Question 4
By what other names is takotsubo cardiomyopathy known?
Question 5
What are the pathogenesis, prognosis and possible complications of takotsubo cardiomyopathy?
Question 6
Outline the key elements in the diagnosis and management of Edith's presentation?
Answer 1
Many conditions show abnormal findings on ECG, and in some cases without clinical correlation, these may be difficult to distinguish. In this case, takotsubo cardiomyopathy (TTC) is the most likely diagnosis.
Differential diagnoses include early acute ST elevation myocardial infarction (STEMI), acute non-ST elevation myocardial infarction or acute pulmonary embolism.
The most common acute ECG findings of takotsubo cardiomyopathy are ST segment elevation in the praecordial leads and T-wave inversion in most leads.1 Unlike in acute myocardial infarction, ECG changes in takotsubo cardiomyopathy are not limited to one coronary vascular territory.
This differs from the typical ECG changes in an acute STEMI, which include elevation of the ST segments in contiguous leads accompanied by reciprocal ST depression in leads remote from the site of an acute infarct. This pattern is a highly sensitive indicator of an acute STEMI.
Electrocardiogram changes that may be seen in pulmonary embolism include sinus tachycardia, complete/incomplete (R) bundle branch block, S1Q3T3 pattern (deep S-wave in lead 1, pathological Q-wave and T-wave inversion in lead 3), ST elevation/T-wave inversion in inferior /septal leads.
Characteristic ECG findings in takotsubo cardiomyopathy are shown in Figure 3. Electrocardiogram changes are often dramatic and not in proportion with the changes in troponin levels.
Takotsubo cardiomyopathy was first described by Sato et al2 in 1990. It is described as a depression of the contractile function of the mid and apical segments of the left ventricle with compensatory hyperkinesis of the basal walls. This leads to ballooning of the ventricular apex with systole. It was given the name 'takotsubo' due to the visual similarities with a traditional Japanese octopus-catching pot (in Japanese 'takotsubo' means 'fishing pot for trapping octopus'). Prevalence has been shown to be between 1.2–2.2% of all patients that present with suspected acute coronary syndrome.3
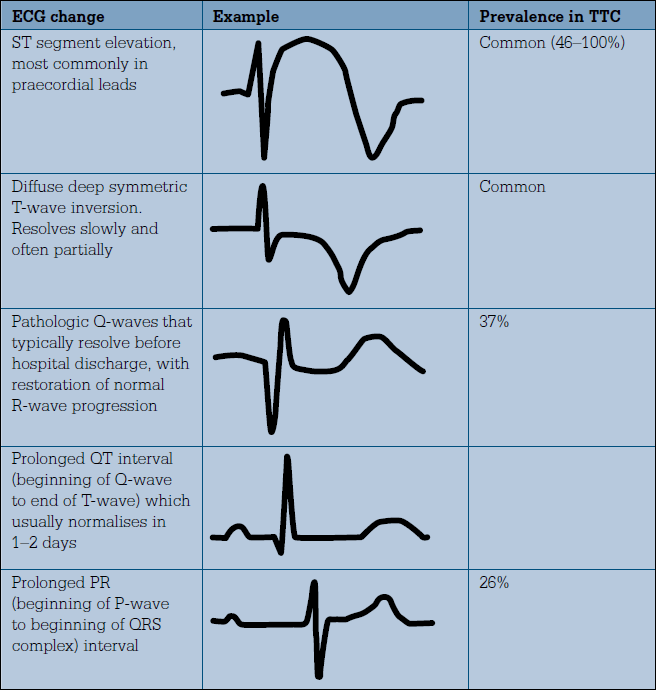
Figure 3. ECG changes in takotsubo cardiomyopathy (TTC)14
Answer 2
Option C is correct. Although the troponin assay is a highly sensitive test for diagnosis of acute myocardial infarction, it lacks specificity. A number of clinical conditions (such as acute pulmonary embolism, heart failure, sepsis, pericarditis and stroke) can cause an elevation in troponin in the absence of acute coronary syndrome.4 Troponin is generally a sensitive biomarker of myocardial injury and in most situations indicates adverse prognosis.
Unlike in acute myocardial infarction, most patients with takotsubo cardiomyopathy have a small but rapid increase in cardiac enzyme and biomarker levels. Although some series report a 100% incidence of troponin elevation, the absence of elevation does not exclude the diagnosis of takotsubo cardiomyopathy.
Ramaraj et al suggested that if the levels of troponin T are greater than 6 ng/mL and troponin I are greater than 15 ng/mL, the diagnosis of takotsubo cardiomyopathy is unlikely and acute coronary syndrome should be considered as the primary diagnosis. Troponin T also showed a significant inverse correlation with initial ejection fraction.5
Answer 3
Takotsubo cardiomyopathy mimics acute coronary syndrome in presentation and is seen most commonly in postmenopausal women following intense emotional or physical stress. Cases in the literature report a wide range of triggers including an unexpected death in the family, gambling and financial losses, receiving a devastating medical diagnosis, motor vechicle accidents, stress caused from public speaking, acute physical trauma, robbery and major surgical procedures.3 However, approximately 20–35% of cases may not reveal any obvious precipitant.6
The most common presenting symptom in takotsubo cardiomyopathy is acute chest pain. The patient may also present with dyspnoea, palpitations, syncope, cardiac arrest or changes on ECG. Although a chest X-ray may be normal, patients can present with acute pulmonary oedema and cardiomegaly. Takotsubo cardiomyopathy can be classified into four types depending on the location of the contractile dysfunction (Table 1).
Table 1. Types of takotsubo cardiomyopathy based on wall motion abnormality7
| Type | Description |
|---|
| Classic, apical ballooning or takotsubo type |
Apical ballooning (most commonly reported) |
| Reverse apical ballooning or reverse takotsubo type |
Hyperdynamic apex and akinesia of the base of the left ventricular wall (uncommon) |
| Midventricular type |
Involves the mid left ventricular wall, sparing the base and the apex |
| Local type |
Localised wall motion abnormality affecting a segment of the left ventricular wall. Most often affects the anterior wall |
Answer 4
As takotsubo cardiomyopathy is usually triggered by physical or emotional stress, the alternative terms 'stress cardiomyopathy' and 'broken heart syndrome' are often used. It has also been called 'apical ballooning syndrome' as a result of the balloon-like appearance of the left ventricle during systole on echocardiography or ventriculogram (Figure 4).
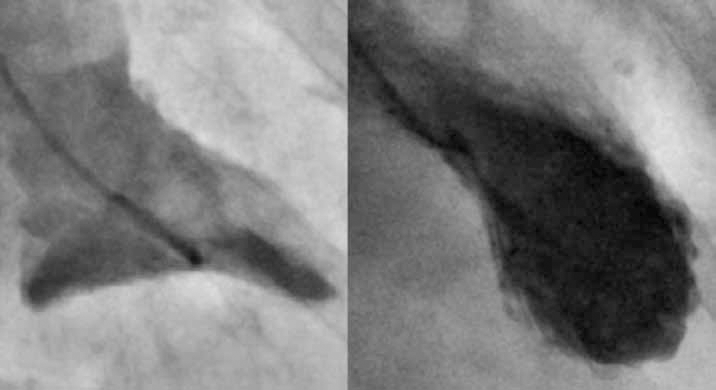
Figure 4. Ventriculogram of contractile phase of normal left ventricle (left) contrasted against a takotsubo cardiomyopathy ventriculogram showing apical ballooning of the left ventricle (right)
Answer 5
The most commonly postulated pathogenesis of takotsubo cardiomyopathy is that an intensely stressful emotional or physical trigger causes an excess of circulating catecholamines, which cause both direct myocardial toxicity and microvascular spam/dysfunction leading to myocardial stunning and consequent contractile dysfunction. The more dense distribution of adrenoceptors at the apex might explain why the apex is usually affected while the base of the ventricle is spared.7 Oestrogen down regulates cardiac adrenoceptors and attenuates their response to activation, providing a plausible reason why the condition is largely confined to postmenopausal women.8
The prognosis of takotsubo cardiomyopathy is generally good. Patients that survive the acute episode typically recover normal ventricular function within 1–4 weeks. Reported inpatient mortality rates for takotsubo cardiomyopathy range from 0–8%. In a study with a mean follow up of 4.4–4.6 years, there was no difference in survival for patients with an acute episode of takotsubo cardiomyopathy compared to an age and gender matched population.9
Heart failure with or without pulmonary oedema is the most common clinical complication and was reported in 38 of 215 patients (17.7%).10 Complications of takotsubo cardiomyopathy include:11
- left heart failure with and without pulmonary oedema
- cardiogenic shock
- dynamic intraventricular obstruction with left ventricular intracavitary pressure gradient generation
- mitral regurgitation resulting from chordal tethering and systolic anterior motion of the mitral valve apparatus
- ventricular arrhythmias
- left ventricular mural thrombus formation
- left ventricular free-wall rupture
- death.
Answer 6
The proposed 'Mayo Clinic' diagnostic criteria for takotsubo cardiomyopathy include: echocardiographic or angiographic evidence of transient hypokinesis, akinesis or dyskinesis of the left ventricular apical and/or mid segments; absence of obstructive coronary disease or angiographic evidence of acute plaque rupture; new ECG abnormalities or modest elevation in troponins; and absence of phaeochromocytoma or myocarditis.14
Without the use of coronary angiography it can be difficult to objectively distinguish takotsubo cardiomyopathy from acute coronary syndrome. When the diagnosis is in doubt, takotsubo cardiomyopathy should be treated as acute coronary syndrome until proven otherwise. Most patients should be hospitalised for confirmation of the diagnosis and subsequent management.
Treatment of takotsubo cardiomyopathy is usually supportive. Despite the fact that a ß-blockade is widely considered to have an important role in treatment, there is a lack of large randomised controlled trials to support its routine use. In haemodynamically stable patients, a ß-blocker should be considered and diuretics given as necessary for volume overload. ß-blockers may block the effects of the catecholamine excess, which is a potential mechanism of takotsubo cardiomyopathy. Moreover, ß-blockers have an essential role in reducing left ventricular outflow tract obstruction by decreasing basal segment hypercontractility.11 Patients without a left ventricular outflow tract gradient should be prescribed an angiotensin converting enzyme inhibitor (ACEI) or an angiotensin receptor antagonist to prevent cardiac remodelling.13 In a rodent model, takotsubo cardiomyopathy could be prevented with an α-blockade or ß-blockade.12
Case follow up
Edith remained well on day three and was discharged on a small dose of a ß-blocker and ACEI. Follow up was arranged with her general practitioner in 7 days and with a cardiology clinic 4 weeks after a repeat ECG.
Key points
- Takotsubo cardiomyopathy should be suspected in any postmenopausal woman presenting with chest pain and dyspnoea following intense emotional or physical stress.
- ECG changes are often dramatic and not in proportion with the rise in troponin levels.
- Acute coronary syndrome is an important differential diagnosis and suspected cases should be referred to hospital.
- Diagnosis can be confirmed by findings of normal coronary arteries and apical ballooning of the left ventricle on coronary angiography.
- Heart failure with or without pulmonary oedema is the most common clinical complication of takotsubo cardiomyopathy.
- The prognosis of takotsubo cardiomyopathy is usually good, with a mortality rate of 0–8%. Most patients that survive the initial episode will regain normal ventricular function with 1–4 weeks and have a good long term prognosis.
Conflict of interest: none declared.