Case study
Mr A, a Malay man, 31 years of age, presented with 2 months of fever and a skin lesion on his right flank (Figure 1).
The skin lesion started as a small nodule, which after a week became weepy, before drying and developing a thick black scab. The lesion was painless. At presentation Mr A had had a fever for 1 week. He had also experienced three episodes of fever in the past 2 months: each episode lasting 2 weeks, subsiding for 1 week and occurring again. The fever was associated with headache, myalgia and generalised aches. He had no loss of weight or appetite and had normal bowel and urinary function.
Mr A did not have any other medical problems. He had no history of contact with tuberculosis, animal or insect bite, or any history of travelling outside of Malaysia. He denied taking any traditional or over-the-counter medication.
Mr A was not sexually active. None of his family members or friends had similar symptoms.
Physical examination was unremarkable other than the fever and skin lesion. On three separate clinic visits Mr A's temperature was 38.4°C, 38.5°C and 38.9°C.
In view of the prolonged fever, Mr A was admitted to hospital. The diagnosis remained uncertain, despite extensive investigations that included blood tests, endoscopic retrograde cholangiopancreatography (ERCP), computerised tomography (CT) of the abdomen, and skin and lymph node biopsy. The ultrasound scan showed slightly dilated left intrahepatic duct with hepatosplenomegaly but the ERCP showed that the hepatic duct was normal in size.
Mr A underwent a laparotomy for suspected pelvic abscess, which revealed multiple inflamed patches at the terminal ileum and enlarged mesenteric lymph node. His serum ferritin level was 179 pmol/L (almost 16 times the upper limit of normal). Liver biopsy was performed to assess for evidence of haematological malignancy infiltration but the result was reported as chronic inflammatory changes. Skin biopsy was inconclusive as it was reported as chronic inflammatory changes. He remained febrile (Figure 2).
Two weeks later a skin biopsy was repeated. This showed an ulcer with dermal lymphoid infiltration compatible with non-Hodgkin lymphoma. The histopathological report confirmed the diagnosis of non-Hodgkin lymphoma NK/T cell lymphoma – nasal type.
Mr A received intravenous chemotherapy, but died 9 days after his diagnosis was confirmed.
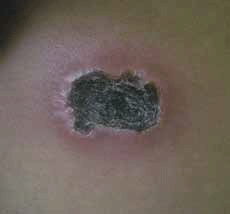
Figure 1. The skin lesion at the right flank region
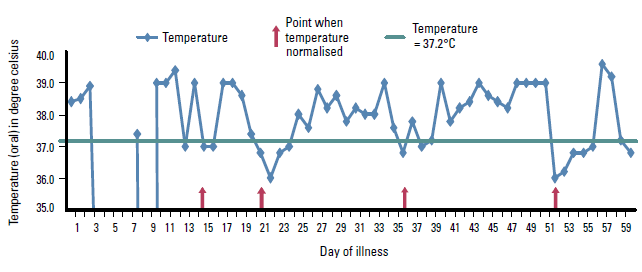
Figure 2. Temperature chart illustrating the patient's relapsing fever pattern
Discussion
Investigation of fever of unknown origin (FUO) can be carried out in the outpatient setting.1–4 The diagnosis of FUO traditionally comprised three components: fever >38.3°C, presence of fever for 3 weeks and cause unknown, despite a 1 week investigative period.1,5 However, it has been argued that the '1 week investigation period' can produce bias in identification of FUO, as the time taken and tests used to investigate FUO vary between centres. It has been proposed that a list of standard investigations should be performed to ensure a standardised definition of FUO.1,3
How to investigate FUO
Cunha and others have proposed a threephase diagnostic work-up for FUO.1,2,5–8
The first phase includes taking a relevant history, performing a thorough physical examination and conducting basic laboratory investigations. This phase aims to narrow down the possible diagnoses and determine the direction of subsequent investigations.
The second phase is carried out on patients who remain undiagnosed. It includes a further focused history, physical examination and additional relevant laboratory tests. The aim of this stage is to refine the diagnosis possibilities.
The third phase of the FUO assessment is based on the potential diagnostic cues, which are retrieved from the history, physical examination and tests. The definitive diagnostic work-up includes specific laboratory testing and biopsy. The aim of this stage is to confirm the diagnosis.
What important history should be taken?
Pattern of fever
In the initial phase, fever should be confirmed by objective temperature measurements, including the pattern of fever and range of temperatures.1,2 The fever pattern can be categorised into: continuous, intermittent, remittent and relapsing. The characteristic and aetiology of fever is summarised in Table 1.1,7,9 The list of differential diagnoses can be shortened based on the pattern of fever.
Table 1. Characteristics and aetiology of fevers1,7,9
| Type of fever | Characteristics | Positive aetiology |
|---|
| Continuous fever |
Fever does not remit |
Typhoid
Typhus
Drug fever
Malignant hyperthermia |
| Intermittent fever |
Fever occurs with daily spikes and returns to normal |
Pyogenic infections
Lymphomas
Miliary tuberculosis |
| Remittent fever |
Fever occurs daily with a spike of temperature of >2°C but, unlike intermittent fever, does not return to normal |
Not a characteristic of any illness |
| Relapsing fever |
The febrile and afebrile periods occur in cycles. The fever returns to normal for a few days but rises again |
- Infectious diseases:
recurrent bacteraemia, melioidosis, salmonellosis, syphilis, malaria, relapsing fever of Borrelia recurrentis, brucellosis, tuberculosis, leptospirosis
- Inflammatory diseases:
lymphoma, colon carcinoma, craniopharyngioma, sarcoidosis, vasculitis, hemophagocytic syndrome
- Miscellaneous causes:
cyclic neutropenia, drug fever, hypertriglyceridaemia
|
Systemic review
Potential diagnostic cues could be obtained by taking a detailed history.2,9 The systemic review should include skin and joints, and the respiratory, cardiovascular, neurological, gastrointestinal, genitourinary and haematological systems. The complete history should also include occupational, travel, sexual and drug histories and any contact with animals.1,2,9
Physical examination
Physical examination should be repeated as part of management, as the findings leading to the diagnosis are numerous and may have been missed during previous examinations.1–3,10 Furthermore, new signs may evolve as the disease progresses. Physical examination should include:
- assessment of the patient's general status
- vital signs
- presence of jaundice
- lymph nodes
- temporal arteries
- mucous membranes
- entire skin surface for rashes
- neurological, cardiovascular, lung, abdominal and genitalia examinations.1–3
Investigations
Initial investigations are listed in Table 2. This is followed by the second and third phase of investigations listed in Table 3 to arrive at a diagnosis.5,8
Table 2. Initial diagnostic work-up for fever of unknown origin
- Erythrocyte sedimentation rate (ESR) or C-reactive protein (CRP)
- Full blood count and differential count
- Renal profile
- Liver function test
- Lactate dehydrogenase
- Creatinine kinase
- Antinuclear antibody
- Rheumatoid factor
- Urinalysis
- Urine culture
- Blood culture (x 3)
- Chest X-ray
- Abdominal ultrasound
- Mantoux test
|
Table 3. Second and third phase of investigation for fever of unknown origin
| Phase | Investigations | Setting |
|---|
| Second phase |
Bone marrow biopsy, temporal artery biopsy in patients aged more than 55 years, funduscopy, abdominal CT and chest CT |
Inpatient |
| Third phase |
Invasive procedures: biopsies, laparoscopy/ laparatomy, endoscopic examinations
Noninvasive procedures: hematologic, serologic tests, cultures, radiological examinations |
Inpatient |
A rise in serum ferritin more than two times the normal level is an important clue for rheumatic (eg. systemic lupus erythematosis, adult Still disease, temporal arteritis) and neoplastic disorders (eg. lymphomas, chronic lymphoblastic leukaemia, chronic myeloid leukaemia, myeloproliferative disorder).6,11 The presence of a high level of serum ferritin (>11.23 pmol/L) renders infections less likely.6,11 Hence, the subsequent investigation should be targeted to detection of neoplastic and rheumatic problems.
Common causes of FUO are listed in Table 4. In the case study, the diagnosis of lymphoma was confirmed through a skin biopsy.
Table 4. Common causes of fever of unknown origin6
| Category | Most common causes |
|---|
| Infectious diseases |
Subacute bacteria endocarditis
Intra-abdominal abscesses
Pelvic abscesses
Renal/perinephric abscesses
Typhoid/enteric fever
Miliary tuberculosis
Renal tuberculosis
Tuberculosis meningitis |
| Rheumatic/inflammatory disorders |
Adult Still disease
Polymyalgia rheumatica
Temporal arteritis |
| Neoplastic disorders |
Lymphoma (Hodgkin or non-Hodgkin)
Hypernephromas |
| Miscellaneous disorders |
Drug fever
Alcoholic cirrhosis |
Should empirical treatment be given for FUO?
Empirical treatment of FUO should be avoided as the antimicrobial therapy may delay or obscure the diagnosis.12 Therapy should be withheld until the cause of fever is identified.4,12 However, empirical therapy may be instituted in the following situations:
- antibiotic for culture negative endocarditis
- low dose corticosteroid for presumed temporal arteritis
- antituberculous drugs for suspected miliary tuberculosis in elderly patients
- naproxen for suspected neoplastic fever.12
Studies have found that, in general, cases of FUO without a precise diagnosis despite intensive investigations and prolonged observation often carry a favourable prognosis.4,12 In a prospective study 11% of 199 patients with FUO did not have any definitive diagnosis after 5 year follow up.12 The attributable mortality for those cases was only 3.2%.12
Summary
This case illustrates the importance of having a systematic approach to the assessment and management of FUO. The pattern of fever, repeated clinical assessment and use of diagnostic investigation are helpful in making an early diagnosis.
Conflict of interest: none declared.