Case
A Nigerian man aged 30 years presented with multiple itchy and hyperpigmented patches affecting the complete body surface (Figure 1). He had emigrated from Nigeria one month ago, and the lesions had appeared two months earlier. There were no associated symptoms such as fever, malaise, headache or arthralgia. Physical examination revealed oval and lichenoid patches with a well‑demarcated border, as well as black dots on his abdomen (Figure 1). The lesions had an asymmetric distribution.
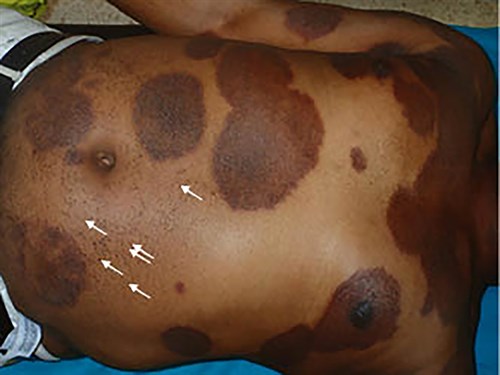
Figure 1. Lichenoid and hyperpigmented patches with a well-demarcated border on the abdomen, the chest and the arms. Black dots can be observed on the left hemiabdomen (white arrows)
Question 1
What is the most likely diagnosis?
Question 2
What tests are indicated?
Answer 1
The most likely diagnosis is disseminated tinea corporis. Skin diseases pose a significant public health threat in Africa and the developing world in general, and are mainly a result of common preventable infections and infestations.1
Dermatomycoses are fungal infections of the skin, hair and nails caused by dermatophytes. These infections result in dermatophytoses or tinea, a contagious skin disease characterised by the formation of ring-shaped eruptive patches. Less commonly, infections can be caused by yeasts or, only occasionally, by moulds, the latter particularly affecting toenails.
Answer 2
The diagnosis of dermatomycoses is based on microscopic detection of fungi using a potassium hydroxide preparation together with a mycological culture. Another option is histological fungal detection with periodic acid–Schiff (PAS) staining, which has a high sensitivity,2 but is more expensive and uncomfortable for the patient as it requires a skin biopsy. Clinical suspicion of tinea corporis is essential to avoid unnecessary skin biopsies.
To perform an ideal skin scraping, no ointment should have been previously applied. Using a blunt scalpel or a curette, firmly scrape the border of the lesion. The best result will come from scraping a recent lesion. In tinea barbae, tinea capitis and tinea of vellous, hair it is necessary to include hair in the sample. If vesicles are present their liquid should be obtained and included as well.
Case Continued
Potassium hydroxide (KOH) examination of scales scraped from the lesion showed multiple segmented hyphae and arthrospores (Figure 2). Trichophyton tonsurans was isolated in culture (Figure 3). A serological test for infection with the human immunodeficiency virus was negative.
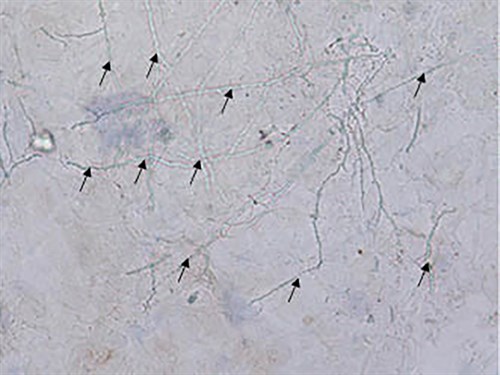
Figure 2. Potassium hydroxide examination of lesions (20X) Potassium hydroxide examination of scales scraped from the lesion showed multiple segmented hyphae (black arrows) and arthrospores
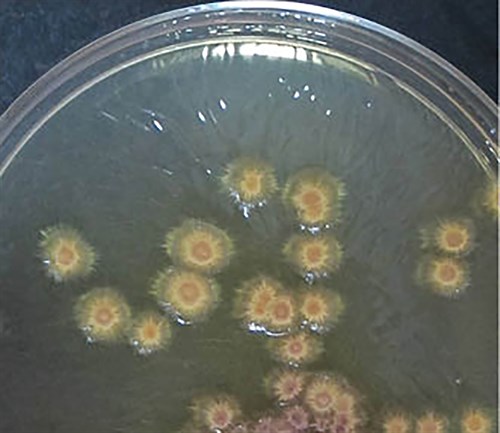
Figure 3. Sabouraud dextrose agar culture Trichophyton tonsurans isolated in Sabouraud dextrose agar
Question 3
What are the differential diagnoses?
Question 4
What empirical treatment can be used for this condition?
Answer 3
A clinical diagnosis of tinea corporis can be difficult, especially in dark‑skinned patients,1–4 and often requires differential diagnoses with other dermatoses. These include atopic eczema, impetigo, seborrheic dermatitis, psoriasis, systemic lupus erythematosus, granuloma annulare or pityriasis rotunda.
Answer 4
Treatment with terbinafine 250 mg/day and topical miconazole for two months is recommended.
Case Continued
The patient was treated as described above and the cutaneous lesions resolved.
Question 5
What is the explanation for the term ‘ringworm’? What is the explanation for the black dots?
Answer 5
Dermatophytoses on the skin appear as centrifugally growing, erythemato-squamous, scaly plaques. This explains the English term ‘ringworm’.2 In the US, Latin America (Mexico), and UK, the anthropophilic species T. tonsurans is the second most common pathogen of tinea corporis after T. rubrum. In Africa, T. violaceum and M. audouinii play a crucial role.2
Black dots have been described in tinea capitis with trichosporic parasitation, although they can be found on other bodyparts as well3 (Figure 1). These black dots correlated with numerous arthroconidia on degenerated hair observed under direct microscopy.
Authors
Elisabeth Gómez Moyano MD, PhD, Dermatologist, Department of Dermatology, Hospital Regional Universitario de Málaga, Pza Hospital Civil s/n.29009, Málaga, Spain. elisabeth.gomez.moyano@gmail.com
Leandro Martínez Pilar MD, Dermatologist, Department of Dermatology, Hospital Regional Universitario de Málaga, Pza Hospital Civil s/n.29009, Málaga, Spain
Silvestre Martinez Garcia MD, PhD, Dermatologist, Department of Dermatology, Hospital Regional Universitario de Málaga, Pza Hospital Civil s/n.29009, Málaga, Spain.
Sara Simonsen, MD, PhD, Dermatologist, Department of Dermatology, Hospital Regional Universitario de Málaga, Pza Hospital Civil s/n.29009, Málaga, Spain.
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.