Case
M, aged 27 years, has chronic eczema. She describes a history of typical eczema on the back of her knees and crooks of her elbows as a child that was treated with 1% hydrocortisone and then more potent TCS. As a young adult, she developed eczema on her face and nipple/areola areas, which were treated with TCS on an increasingly frequent basis. Frustrated with her deteriorating condition, M turned to the internet for advice. She read about red skin syndrome, diagnosed herself with topical steroid addiction and is now three months into TCS withdrawal. M comes to you for advice about a possible skin infection to her areola areas, which have been red and oozing for the past four weeks.
Independently published international guidelines recommend TCS as the first-line anti-inflammatory therapy for eczema,1,2 and its efficacy is well established.2 While the incidence of TCS side effects is considered low, there have been few long-term studies.2 One potential long-term complication is TCS addiction and withdrawal. It was first described in 1979 by Kligman and Frosch,3 and there have been limited articles on the topic in the medical literature since then. However, the US National Eczema Association received sufficient patient enquiries about the condition to justify the formation of a Scientific Advisory Committee Task Force to conduct a systematic review, which was published in 2015.1
Clinical features
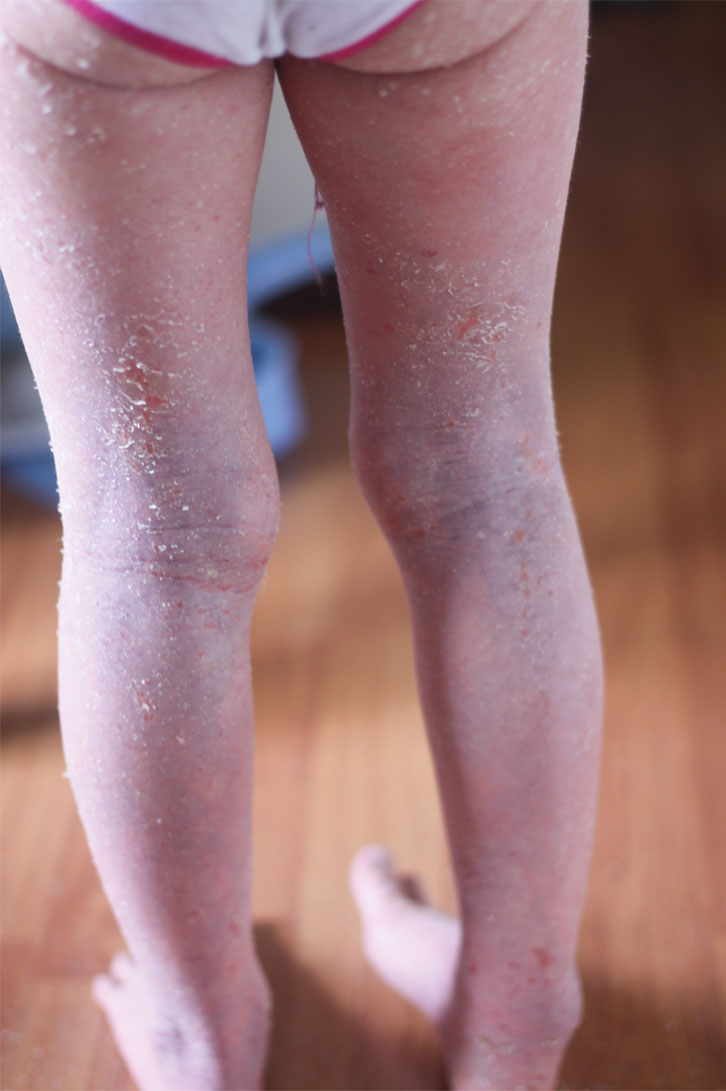
When patients with TCS addiction cease TCS, they may develop widespread redness (Figures 1 and 2), burning pain, peeling skin, oozing areas (Figure 3) and severe itch.
 |
 |
| Figure 1. Widespread redness to lower limbs, oedema to ankles and some exfoliation |
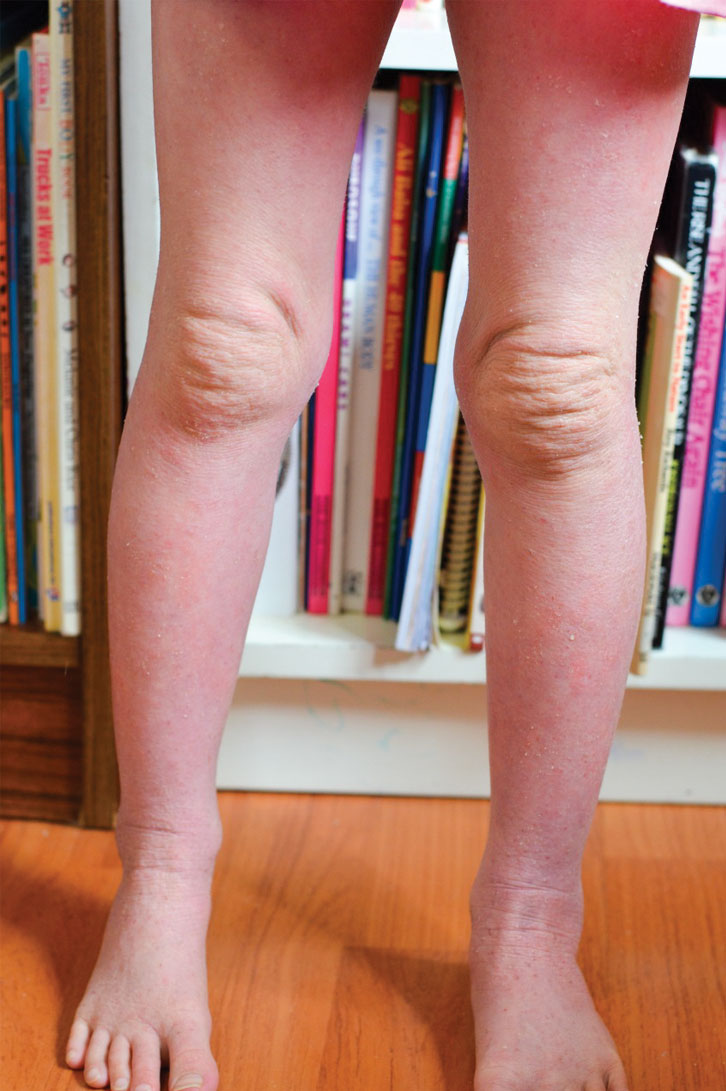
Figure 2. Widespread redness to lower limbs and ‘elephant wrinkles’ to anterior knees |
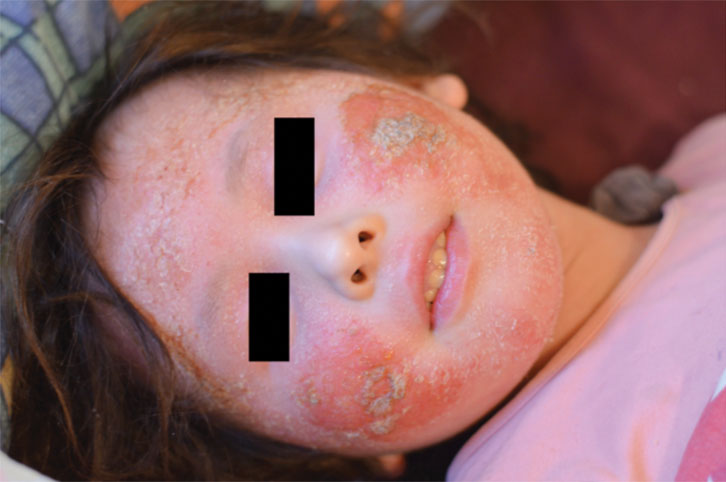 |
| Figure 3. Serous exudate and crust formation to cheeks, ‘headlight sign’ – clear nose and peri-oral area, exfoliation to forehead and chin |
Erythema typically spreads from the original eczematous areas locally – for example, from the face to the neck and then the upper limbs.4,5 Areas never treated with TCS can also become involved.4,5
The severity and pattern of symptoms seen can vary significantly between patients. Some will experience ‘flares’ and ‘breaks’, where their skin cycles through periods of abnormal and then relatively normal skin.4 Others have more persistent symptoms for prolonged periods.4 Table 1 provides details of clinical features described in the literature. While an affected patient is still using TCS, their skin can look normal or well controlled,5 or it may appear atrophic or demonstrate telangiectasia.4
Table 1. Features seen in topical corticosteroid withdrawal
|
| Red skin1,4,5 |
- Can be severe (see Figures 1 and 2)
- Present in 92% of cases1
|
| Burning pain or stinging1,4,5 |
- Reported in 95% of patients with the ‘erythemoedematous’ type of TCS withdrawal1 (most eczema patients fit in this category)
- In the early withdrawal phase, almost all topical products can ‘burn’ when applied to the skin4
|
| Itch1,4,5 |
- Can be severe
- Present in 45% of all patients1
|
| Skin peeling or exfoliation1,4,5 |
- Said to occur at the end of a ‘flare’4
- Occurs in one-third of all patients1
|
| Oozing areas1,4,5 |
- Can take months for serous exudate to ‘dry up’ (see Figure 3)
|
| Oedema1,4,5 |
- Especially eyelids, ankles, hands and ankles (Figure 1)
|
| Papulopustules1 |
- Seen in over 80% of patients who used TCS for pigmentary disorders or acne1
|
| Hives |
|
| Excessive sweating |
|
| Depression5 |
- Psychological support for these patients is essential and may be required for many months
|
| Insomnia4 |
- At least in part due to pain and itch
|
Definitions
Several different names have been used to describe this condition in the literature. TCS addiction/withdrawal syndrome, topical steroid addiction and red skin syndrome all refer to essentially the same entity.
Hajar et al described TCS withdrawal (‘steroid addiction’) as a distinct adverse effect of TCS misuse, ‘[resulting] from prolonged, inappropriate and frequent use of moderate-to-high potency TCS primarily on the face and genital area in most cases’.1 They identified two distinct morphological syndromes:
- erythematoedematous type – most commonly seen in eczema patients
- papulopustular type – more often present in patients who used TCS for acne or pigmentary conditions.
Fukaya et al defined topical steroid addiction as ‘the situation where skin develops more severe or diverse skin manifestation after withdrawal from topical corticosteroids than at pre-application’.5 Rapaport and Rapaport used the name ‘red skin syndromes’ to collectively group the erythema syndromes in the literature, which they attributed to topical steroid addiction.4 This group includes chronic recalcitrant eczema in addition to:4
- red face syndrome
- prolonged post peel or laser erythema
- status cosmeticus
- red scrotum syndrome
- vulvodynia
- perianal atrophoderma
- chronic actinic dermatitis.
Epidemiology and aetiology
The incidence and prevalence of TCS addiction and withdrawal are unknown.1,5 Atopics are most at risk,4 and in a systematic review, eczema was the initial indication for TCS use in one-third of cases.1 The same review found that 81% of those affected were female; 97% of patients had applied TCS to the face; and 94% of cases were where mid-to-high potency TCS were used.1 Using more potent TCS for longer periods
of time increases the risk of developing
TCS addiction.5
Pathophysiology of the ‘red skin’
The widespread red skin seen in this condition is thought to be the result of prolonged fixed vasodilatation. TCSs have a suppressive effect on nitric oxide in the endothelium and the release of accumulated endothelial nitric oxide stores results in hyperdilatation of vessels.4
Diagnosis
Clinical signs seen in TCS withdrawal
Possible TCS withdrawal signs include:
- Headlight sign – nose and perioral area spared from redness seen on rest of face (Figure 3).4 Erythema often ends at the mid-cheek with normal skin present from the mid cheek to the ears.
- ‘Red sleeve’ – rebound eruption to extremities stopping abruptly at the margin of the dorsal and palmer (or solar) sides.5
- ‘Elephant wrinkles’ – reduction in skin elasticity, for example, to the anterior knees (Figure 2), extensor elbows and/or neck.
Signs of skin damage from TCS such as skin atrophy and telangiectasia have been reported in patients with TCS addiction prior to cessation of TCS.4,5
Differential diagnoses
The three main differentials are allergic contact dermatitis,1,4 infection5 and an eczematous flare.1 Allergy to TCS, components of TCS, other prescription topical products, moisturisers and cosmetics may be excluded by patch testing and, possibly, photopatch testing.
Hajar et al suggested that TCS withdrawal is more likely than underlying eczema if:1
- burning is the prominent symptom
- confluent redness occurs within days to weeks of ceasing TCS
- there is a history of frequent, prolonged TCS use on the face or genital region.
Management
Supportive measures are indicated for physical and psychological symptoms. Patients can trial oral antihistamines for their itch. Burning pain may be alleviated with ice or cool water compresses or possibly gabapentin.4 Sleeping aids and anxiolytics may be appropriate in some cases.4 Oral immunosuppressants and light therapy have been reported to help selected patients.4 Calcineurin inhibitors and oral antibiotics (eg doxycycline, tetracycline and erythromycin) have been used mostly in patients with the papulopustular subtype.1 Prevention and treatment of any secondary infection are prime concerns of both patients and doctors.
The prolonged withdrawal period (months to years) can take a significant toll on the patient’s mental health. Multiple telephone calls and visits for reassurance have been recommended.4 Some patients are unable to manage and resume their use of TCS.4
Discussion
Why would my patient with eczema want to cease TCS?
Patients may want to cease TCS for a combination of concerns about continuing to use (often potent) TCS regularly and indefinitely with diminishing clinical benefit, and the anticipation of improved skin following completion of the TCS withdrawal process. Steroid phobia is a separate issue and is not applicable in these patients: TCS addiction is thought to be the result of TCS misuse1 (overuse and not underuse of TCS). After complete withdrawal, a patient with TCS addiction can expect normal skin4 or the original eczema symptoms.5
Safe use of TCS
Concern about the possibility of TCS addiction should not prevent adequate and appropriate treatment with TCS when indicated.1 Australian guidelines recommend using TCS once or twice a day, as per the product information, to all of the inflamed skin until the eczema is cleared.6
Preventing TCS addiction/withdrawal syndrome
While research is very limited to date, avoiding prolonged use of moderate-to-potent TCS on the face may be prudent as this is a highly significant risk factor for the development of TCS addiction and withdrawal. Avoiding continuous use of TCS for longer than two weeks has been suggested by Fukaya et al,5 and the US National Eczema Association has advised the following:7
Do not use TCS continuously for more than two to four weeks – then frequency should be tapered to twice weekly use. Your provider should strive to help create a safe and effective long term treatment plan that does not include daily use of TCS, especially on more sensitive areas.
Case continued – six months later
M monitored herself for signs of infection – fever, tenderness or pain and expanding areas of redness to surrounding skin. She washed the area daily with a Chinese herbal tea, and applied vaseline under non-stick dressings before putting on clothing. Her symptoms remained stable until spontaneous clearing of areola skin five months later. At this point, her face, neck and arms were still exhibiting TCS withdrawal symptoms. M had negotiated with her employer to work from home and reduce her hours. In addition, she was now seeing a psychologist.
Conclusion
TCS can cause TCS addiction and withdrawal in some eczema patients with a history of moderate to high potency TCS use, especially to the face or genital area. Appropriate treatment of eczema is essential and general practitioners (GPs) might counsel patients at risk of developing TCS addiction by being mindful of this condition. GPs can play a key role in supporting diagnosed patients through the challenging withdrawal period. Consultations about this issue may become a more frequent scenario for GPs as increasing numbers of patients research their symptoms online. Rational and informed discussions about TCS addiction and withdrawal would be very helpful for patients searching for answers from a trusted source.
Author
Belinda Sheary BMed, FRACGP, General Practitioner, Royal Randwick Medical Centre, Randwick, NSW. Belinda.sheary@ipn.com.au
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.