There has been little published research about the rate of management of musculoskeletal injuries (eg fractures, sprains/strains) in Australian general practice. There has been a national increase in hospital admissions for all injury types (including falls, poisoning and drowning) from 1736 per 100,000 population in 1999–2000 to 1888 in 2012–13.1 A previous Bettering the Evaluation and Care of Health (BEACH) study showed a significant increase in total imaging rate for selected musculoskeletal conditions managed at general practitioner (GP) encounters between 2002–03 and 2011–12 and it analysed imaging requests for various musculoskeletal injuries.2
This study provides an overview of the types and rates of musculoskeletal injuries and associated patient characteristics seen at general practice encounters nationally, and reports trends over 15 years in their frequency of management and associated imaging requests.
Methods
We analysed data collected in the BEACH program from April 2000 to March 2015. Musculoskeletal injury problems were defined using International Classification of Primary Care, version 2 (ICPC-2) and ICPC-2 PLUS codes.3 BEACH methods have been described in detail previously.4 Each year, a random sample of about 1000 GPs are instructed to record at least one, and up to four, problems managed at each of 100 encounters with consenting patients. Encounters involving management of at least one musculoskeletal injury problem are referred to as ‘musculoskeletal injury encounters’.
The P values for differences in patient characteristics were calculated using Wald chi-square, and the P value for the yearly trend slope using linear regression analysis. The extrapolated national estimates of number of GP encounters involving musculoskeletal injuries per year were calculated using the method described by Britt et al5 using published Medicare claims data6 and the estimated resident population for June each year.7
Results
Of 1,471,600 BEACH encounters, 53,316 (3.62%; 95% confidence interval [CI]: 3.57–3.67) were musculoskeletal injury encounters, involving management of 53,933 musculoskeletal injury problems. By extrapolation, the annual number of GP musculoskeletal injury encounters nationally was estimated to be 4.05 million (95% CI: 4.00–4.11), and the annual number of musculoskeletal injury problems managed at these encounters was 4.10 million (95% CI: 4.04–4.16).
For every 1000 GP encounters, on average, about 37 musculoskeletal injury problems were managed, of which approximately 40% were sprains or strains (equivalent to about 1.6 million sprains or strains managed by GPs nationally each year), and almost 30% were fractures (almost 1.2 million per year). Anatomically, more than one in six musculoskeletal injuries were spinal (Table 1).
Table 1. Rate and estimated number of musculoskeletal injury (MSKI) problems managed in Australian general practice nationally per year, by type and site (BEACH data, April 2000 to March 2015)
|
| Rate of MSKI problems managed per 1000 encounters (n = estimated number of MSKI problems managed nationally each year [thousands]*) |
| |
Type of MSKI |
|
|
|
| Site of MSKI |
Sprain/strain |
Fracture |
Other MSKI† |
Total |
| Spine |
4.4
(490) |
0.7
(80) |
1.5
(170) |
6.5
(730) |
| Shoulder |
2.3
(250) |
0.1
(10) |
1.7
(200) |
4.1
(450) |
| Knee |
0.5
(60) |
0.1
(10) |
3.0
(340) |
3.7
(410) |
| Ankle |
2.1
(230) |
0.6
(60) |
0.5
(50) |
3.1
(350) |
| Other or not specified |
5.2
(580) |
8.9
(1000) |
5.2
(580) |
19.3
(2160) |
| Total |
14.4
(1610) |
10.4
(1160) |
11.9
(1330) |
36.6
(4100) |
*Rounded to the nearest 10,000
The national extrapolation is based on a yearly average of 111.9 million Medicare-claimed GP consultations across the study period
†‘Other MSKI’ includes dislocations, tears or MSKIs of unspecified type |
Characteristics of patients at musculoskeletal injury encounters and characteristic-specific likelihood of attendance for these problems are shown in Table 2. The consultation rate for musculoskeletal injury was significantly higher among patients who were male, aged 5–24 years, not holding a healthcare card, and from an English-speaking background.
Table 2. Patient characteristics at musculoskeletal injury (MSKI) encounters: Frequency distributions and characteristic-specific rates (BEACH data, April 2000 to March 2015)
|
| Characteristic | Characteristic value | n | Per cent (95% CI) | Characteristic-specific rate per 100 specific encounters* (95% CI) |
|---|
| All patients |
All patients |
53,316 |
100.0 |
3.62 (3.57–3.67) |
|
Sex (missing n = 478)
|
Males |
26,899 |
50.9 (50.4–51.4) |
4.53 (4.45–4.61) |
| Females |
25,939 |
49.1 (48.6–49.6) |
3.00 (2.95–3.05) |
|
Age group (missing n = 420)
|
<1 year |
53 |
0.1 (0.1–0.1) |
0.18 (0.13–0.23) |
| 1–4 years |
510 |
1.0 (0.9–1.1) |
0.79 (0.71–0.86) |
| 5–14 years |
4001 |
7.6 (7.3–7.8) |
5.02 (4.85–5.19) |
| 15–24 years |
6772 |
12.8 (12.5–13.1) |
5.21 (5.05–5.36) |
| 25–44 years |
15,578 |
29.5 (29.0–29.9) |
4.53 (4.44–4.63) |
| 45–64 years |
15,661 |
29.6 (29.2–30.1) |
3.91 (3.83–3.99) |
| 65–74 years |
4834 |
9.1 (8.9–9.4) |
2.58 (2.49–2.66) |
| ≥75 years |
5487 |
10.4 (10.0–10.7) |
2.45 (2.37–2.53) |
|
Commonwealth healthcare card holder (missing n = 7573)
|
Yes |
16,982 |
34.9 (34.3–35.5) |
2.85 (2.79–2.90) |
| No |
31,681 |
65.1 (64.5–65.7) |
4.17 (4.10–4.24) |
|
Non–English-speaking background (missing n = 5706)
|
Yes |
3719 |
7.8 (7.4–8.2) |
3.30 (3.15–3.44) |
| No |
43,891 |
92.2 (91.8–92.6) |
3.61 (3.56–3.67) |
| *The average number of encounters at which MSKI was managed for every 100 specific encounters. For example, MSKI was managed, on average, at three out of 100 encounters with female patients. Within each characteristic, the characteristic-specific rates are significantly different from each other (P <0.0001) |
From 2000–01 to 2014–15, the proportion of encounters that involved management of musculoskeletal injury problems decreased from 4.2% of all encounters to 3.5%. Linear regression showed a significant decrease (P <0.0001).
However, because of the increase in the number of GP encounters over the study period,6 the absolute number of musculoskeletal injury encounters increased. In 2000–01 there were approximately 4.2 million musculoskeletal injury encounters, which decreased to 3.6 million in 2003–04 and then increased to 4.8 million in 2014–15. Linear regression showed this was a significant increase over the 15-year period (P <0.0001). Given the population increase over the 15 years, the number of musculoskeletal injury encounters per capita remained reasonably constant at approximately 20 per 100 head of population each year (no linear change, P = 0.56; data not shown).
On average, 30.9 (95% CI: 30.4–31.5) imaging tests were requested per 100 musculoskeletal injury problems managed, comprising diagnostic radiology (23.5 per 100 musculoskeletal injury problems), ultrasonography (4.9 per 100 musculoskeletal injury problems), computerised tomography (CT; 1.0 per 100 musculoskeletal injury problems), magnetic resonance imaging (MRI; 1.0 per 100 musculoskeletal injury problems) and nuclear medicine imaging (0.5 per 100 musculoskeletal injury problems). There was a significant linear increase in the annual rate of imaging test orders from almost 26 to almost 36 per 100 musculoskeletal injury problems managed over the study period (Figure 1).
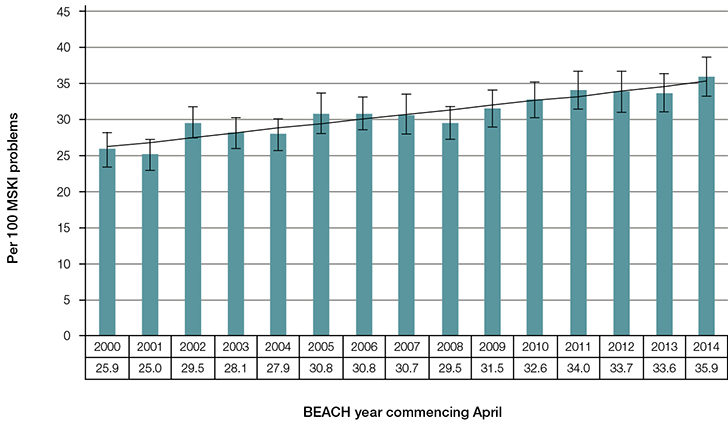 |
Figure 1. Annual rate of imaging ordered per 100 musculoskeletal injury (MSKI) problems managed at GP encounters (95% CI and linear trend), BEACH years April 2000 – March 2015
Note: The linear trend is 0.64 per 100 increase per year (P <0.0001) |
Discussion
These musculoskeletal injury descriptive and analytical results quantify a broad range of common problems managed in Australian general practice. The frequency distributions of patient characteristics reflect the caseload at encounters, and the characteristic-specific rates help identify at-risk groups. The lower rates of musculoskeletal injury at encounters with female patients, the elderly, healthcare card holders and those from a non–English-speaking background may be due to a higher proportion of non-musculoskeletal injury conditions (eg chronic disease) per 100 encounters, or may be affected by statistical confounders. Conversely, for example, among younger males (who have fewer encounters for chronic disease than older patients), sporting and other injuries are managed at a higher proportion of their encounters. A study of the age-specific and sex-specific rates of all hospitalised injury in Australia showed higher rates among males than females up to the age of 65 years, and among people aged 70 years or older than younger age groups.1 By contrast, older age groups had lower management rates for musculoskeletal injury in our study, suggesting that older patients with injuries more often present to hospitals than to general practice. Overall, we found that in general practice, the number of musculoskeletal injury encounters per capita remained constant over time.
The increased number of imaging orders per 100 musculoskeletal injury problems over time is consistent with the findings of the BEACH imaging study.2 For example, it showed increased use of ultrasonography for shoulder conditions, and of magnetic resonance imaging for back and knee, which may have contributed to the higher testing rate in the broader group of musculoskeletal injuries reported here.
Conclusion
Musculoskeletal injuries are commonly managed in Australian general practice – an estimated 4.1 million encounters each year on average. Over time, the management of musculoskeletal injuries has formed a smaller proportion of GP workload, because of the national increase in GP attendances. Overall, GPs are managing the same number of musculoskeletal injuries per head of population in 2014–15 as 15 years earlier.
Authors
Allan J Pollack MBBS (Hons), MBiomedE, FRACS (Orth), Research Assistant, Family Medicine Research Centre, Sydney School of Public Health, Sydney Medical School, University of Sydney, Parramatta, NSW. allan.pollack@sydney.edu.au
Clare Bayram BAppSc (HIM) (Hons), PhD, Project Manager, BEACH program, Research Fellow, Family Medicine Research Centre, Sydney School of Public Health, Sydney Medical School, University of Sydney, Parramatta, NSW
Graeme C Miller MBBS, PhD, FRACGP, Associate Professor and Medical Director, Family Medicine Research Centre, Sydney School of Public Health, Sydney Medical School, University of Sydney, Parramatta, NSW
Conflict of interest: None.
Provenance and peer review: Commissioned, externally peer reviewed.
Acknowledgements
We wish to thank the general practitioners who participated for their generosity. During the data collection period of this study, the BEACH program was funded by the Australian Government Department of Health, Australian Government Department of Veterans’ Affairs, AstraZeneca Pty Ltd (Australia), Novartis Pharmaceuticals Australia Pty Ltd, bioCSL (Australia) Pty Ltd, AbbVie Pty Ltd, Merck Sharp & Dohme (Australia) Pty Ltd, Pfizer Australia Pty Ltd, National Prescribing Service Ltd, GlaxoSmithKline Australia Pty Ltd, Sanofi-Aventis Australia Pty Ltd, Bayer Australia Ltd, Janssen-Cilag Pty Ltd, Abbott Australasia Pty Ltd, Wyeth Australia Pty Ltd, and Roche Products Pty Ltd.
Funding organisations had no editorial control over any aspect of this article.