Case
A previously healthy teenager, aged 16 years, presented with a sudden appearance of a slightly itchy rash located on his trunk and extremities. The eruption was characterised by multiple, well-demarcated, discrete, drop-like, salmon-pink papules and plaques, some with a fine scale (Figure 1). The patient described a history of tonsillitis about five weeks earlier, which was positive for group A ß-haemolytic streptococcus (GAS). At that time, the patient was treated with amoxycillin and paracetamol with good clinical response.
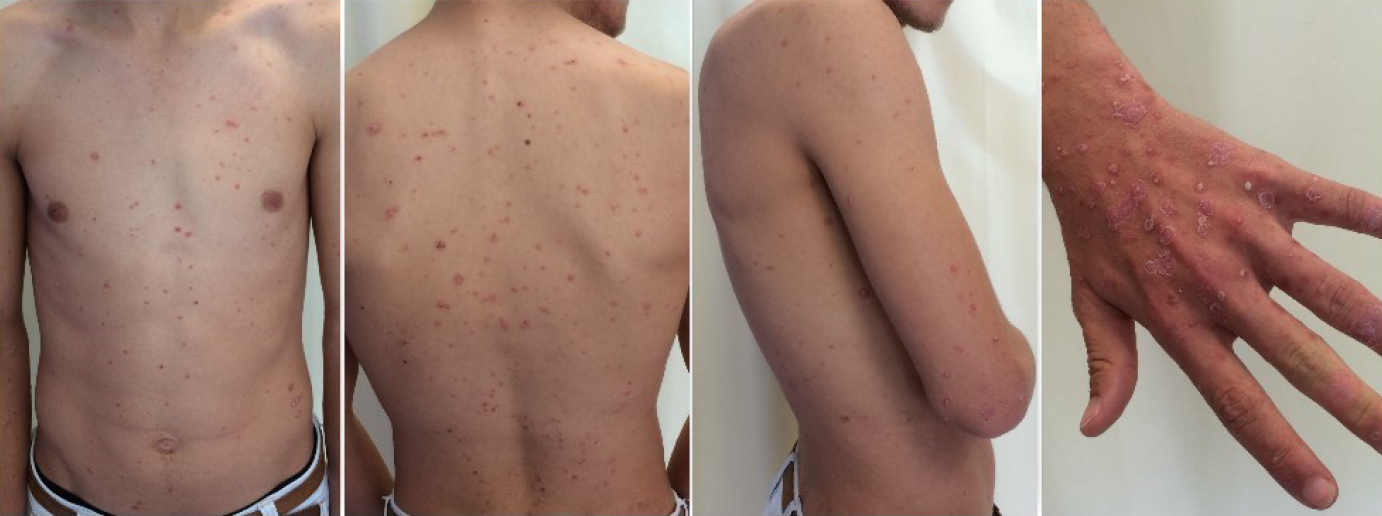 |
| Figure 1. Clinical appearance of the patient |
Question 1
What is the most likely diagnosis in this patient?
Question 2
What is the aetiology of this condition?
Question 3
How is this condition diagnosed?
Question 4
What differential diagnoses should be considered?
Question 5
What is the appropriate management of this condition?
Question 6
What is the prognosis?
Answer 1
The most likely diagnosis is guttate psoriasis, a rare form of psoriasis that accounts for approximately 2% of all psoriasis cases and tends to affect children and people under the age of 30 years. It is the second most common psoriasis variant in children.1 Named after the Latin word for drop (gutta), this skin condition can occur as the initial manifestation of psoriasis in previously healthy individuals, or as an acute exacerbation in individuals with chronic plaque psoriasis.2 Guttate psoriasis affects people of all ethnicities and both sexes equally.1
Answer 2
An upper respiratory tract infection (eg pharyngitis or tonsillitis) caused by GAS usually occurs two to three weeks before the eruption of guttate psoriasis.3 This psoriasis can also be associated with perianal streptococcal infections.4 However, the exact pathophysiological mechanism is unclear. The disease is believed to result from an immune reaction triggered by a previous streptococcal infection, usually in patients with susceptible genotypes (positive HLA-Cw*0602 allele).1 A family history of psoriasis, viral infections, acute stressful life events, injury to the skin, and certain drugs (including anti-tumour necrosis factor-α [TNF-α] biologic agents) and vaccines may also represent risk factors for the onset of guttate psoriasis.5,6
Answer 3
Guttate psoriasis is diagnosed clinically, and a biopsy is usually not needed. Characteristically, initiation of the skin lesions is acute, and multiple papules appear on the trunk and the proximal extremities; however, it can have a generalised distribution, involving the face, ears and scalp. Examination of the skin reveals multiple well-demarcated papules, with diameters of 1–10 mm, colour from salmon-pink to erythematous, and with a round-to-oval form.1,2 Lesions usually spread centripetally and, after development, may have a fine scale. Palms and soles are rarely affected, and if they are, syphilis serology should be requested. The exanthema is frequently accompanied by mild itching. Cases related to acute streptococcal infections may have pharyngeal or perianal erythema.1,4 Laboratory tests can reveal elevation of antistreptolysin O (ASO), anti-DNase B and streptozyme. Bacterial cultures from the throat or perianal area may be helpful to isolate the organism in some cases.1
Answer 4
Table 1 shows conditions to be taken into account in the differential diagnoses of guttate psoriasis. Other diagnoses that may be considered include tinea corporis, cutaneous T-cell lymphoma and lymphomatoid papulosis.1
Answer 5
There is insufficient trial evidence to establish treatment of acute guttate psoriasis, therefore it is guided by expert opinion. The rash often resolves within a few weeks to months without treatment, so emollients can be sufficient.7 Topical agents, such as corticosteroids, vitamin D3 analogues and coal-tar preparations, may be useful; however, they can be difficult to administer if there is extensive involvement. In prolonged cases, prudent sunlight exposure or narrowband ultraviolet B (UVB) phototherapy can contribute to a faster resolution. In cases where the patient is resistant to topical therapy, referral for a dermatological opinion should be considered.7 There is insufficient evidence to support a recommendation for antibiotic treatment, routine investigation for streptococcal infection, or tonsillectomy for patients with recurrent or chronic guttate psoriasis.8
Answer 6
Guttate psoriasis often has a self-limiting course, mainly in children, and complete remission without treatment occurs in 12–16 weeks. About one-third of patients progress to the chronic plaque form in 10 years.9 Patients of younger age and with elevated ASO titres have a better prognosis, whereas a family history of psoriasis is associated with a poorer prognosis.10 Post-inflammatory pigmentary alterations (hypopigmentation or hyperpigmentation) may occur in previously affected areas. Recurrent episodes are possible, especially in patients carrying GAS in the pharynx.
Table 1. Conditions to consider in the differential diagnosis of guttate psoriasis1,2
|
Disease
|
Differentiating features
|
|---|
|
Pityriasis rosea
|
- Usually starts with a single plaque (‘herald patch’), with colour from salmon to erythematous, followed by a generalised eruption after several days
- Lesions tend to be oval with collarette scaling
- Distribution in the trunk following the rib-line can produce the characteristic ‘Christmas tree’ pattern
|
|
Secondary syphilis
|
- Clinically can resemble guttate psoriasis but with more systemic complaints
- If the diagnosis is uncertain, consider syphilis serology, especially in the case of palmoplantar and facial involvement
|
|
Nummular dermatitis
|
- Mainly affects the distal extremities
- Plaques have coin-shaped form, are less numerous and more pruritic than those of guttate psoriasis
|
|
Pityriasis lichenoides
|
- Polymorphic eruption
- Compared with those seen in guttate psoriasis, papules have a smaller size
|
|
Small plaque parapsoriasis
|
- Lesions are flatter and have an elongated, finger-like form (digitate pattern) that are typically found on the flanks
|
|
Viral and drug exanthems
|
- Take a careful clinical history regarding recent illness and current or recent medications taken by the patient
|
Case continued
The patient was treated with a fixed combination of calcipotriol/betamethasone dipropionate gel, emollient and UVB phototherapy. At the follow-up visit four weeks later, complete resolution of the skin condition was observed.
Authors
Sofia Madanelo MD, Family Medicine Trainee, Unidade de Saúde Familiar (USF) Santa Joana, Aveiro, Portugal. sofia.madanelo@hotmail.com
Ana Baptista MD, Family Medicine Trainee, USF Viseu-Cidade, Viseu, Portugal
Joana Ribeiro MD, Family Medicine Trainee, USF Aveiro-Aradas, Aveiro, Portugal
Paulo Morais MD, Consultant Dermatologist, Department of Dermatovenereology, Centro Hospitalar Tondela-Viseu, Viseu, Portugal
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.