Case
A woman aged 34 years presented with skin lesions and recurrent diarrhoea during the previous 2 weeks. The lesions first appeared on her legs then extended to her feet, arms and perineum. She had no other known comorbidities. There was no history of gastrointestinal disturbances and she consumed 50 g of alcohol per day. On physical examination, we observed multiple bilateral erythematous plaques with irregular margins and some erosions on her feet, perineal area, arms, legs and thighs (Figure 1). Her scalp showed diffuse hair loss. She had a low serum zinc level of 22 µg/dl (normal range 70–130 µg/ dl) and characteristic abnormal liver profile due to excessive alcohol consumption.
A skin biopsy showed a superficial dermal infiltrate with variations in thickness of epidermis, clear cytoplasm vacuolated cells in the superficial layers and compact parakeratosis, consistent with nutritional deficiency. She was treated with oral zinc supplements and given dietary advice. The lesions resolved in two weeks (Figure 2). After a 12-month follow-up, no relapses have occurred.
Question 1
What is the most likely diagnosis?
Question 2
What is the pathophysiology?
Question 3
What are the clinical manifestations of this diagnosis?
Question 4
How is this diagnosis made?
Question 5
What is the most appropriate management?
Answer 1
Acrodermatitis enteropathica or acquired zinc deficiency is the most likely diagnosis. It is a rare disorder caused by inherited or acquired zinc deficiency. Some authors prefer to use the term acrodermatitis enteropathica only for the inherited disease. It usually presents with skin lesions, diarrhoea and/or alopecia. The acquired form is secondary to lack of ingestion, altered absorption or excessive excretion of zinc.1 Zinc deficiency in adults may be associated with liver disease, alcoholism, intestinal malabsorption syndromes, pancreatic insufficiency or intake of zinc deficient enteral or parenteral nutrition.2,3 Many cases are truly a mixed nutritional deficiency.
Answer 2
Zinc, an essential mineral for humans, has three main metabolic functions: catalytic, structural and regulatory. It is involved in the metabolism of vitamins, carbohydrates and proteins, cell proliferation and tissue repair. Moreover, zinc is a cofactor of many metalloenzymes and affects various cell-mediated immune mechanisms, which are important in preventing mucocutaneous infections. In a normal diet, zinc is found in good amounts in protein-rich food especially animal protein. The world’s population at risk of inadequate zinc intake is estimated to be 17.3%.4
Answer 3
Acrodermatitis enteropathica belongs to the family of necrolytic erythemas, which include necrolytic migratory erythema, necrolytic acral erythema, pellagra and essential fatty acid deficiencies. The classic cutaneous findings include symmetric, erythematous, scaly, eczematous, vesicular-bullous or pustular eruption on the distal surfaces and periorificial areas. Without treatment, patients develop generalised alopecia and diarrhoea. Delayed wound healing, anaemia, psychological disorders and ophthalmic alterations may appear during advanced disease.5
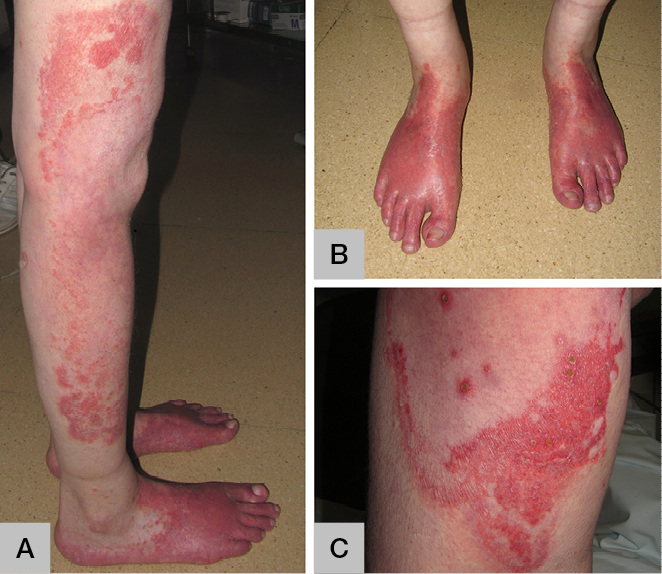 |
Figure 1.
A. Erythematous plaques on her inferior limbs,
B. Dorsa of feet symmetrically involved,
C. Detail of a plaque on her inner thigh |
 |
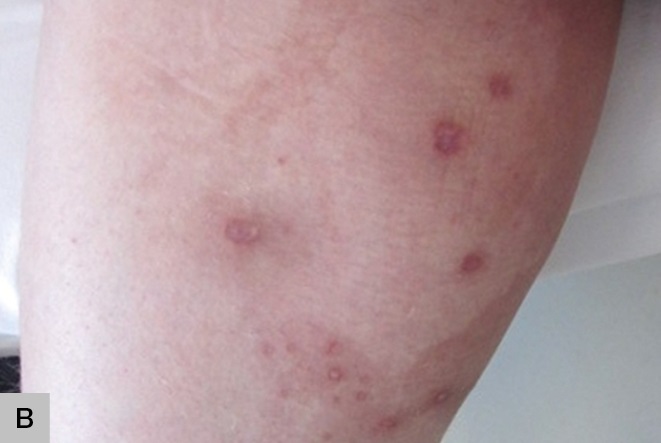 |
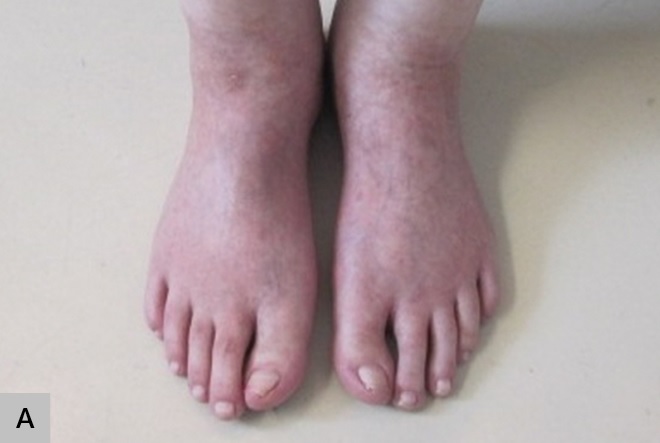
Figure 2.
Resolution after two weeks of zinc supplementation.
A. Dorsa of feet,
B. Inner thigh |
Answer 4
The diagnosis of acrodermatitis enteropathica is clinical and can be confirmed by a low concentration of zinc in the serum. However, zinc levels are a poor marker of true zinc status, so clinical features and responsiveness to a therapeutic trial of oral zinc are the best tests in suspected cases. If no clinical improvement occurs within a few days of treatment, the condition is not due to zinc deficiency, as responses are usually seen very quick (as in this case). Histological findings are non-specific and common to many nutritional deficiencies. The clinical differential diagnosis in adults should include intertrigo, necrolytic erythemas and Hailey-Hailey disease, among others.2 In the paediatric setting, there are a number of other metabolic genetic conditions that can give a similar clinical picture. Secondary infections are considered a frequent complication of acrodermatitis enteropathica.6
Answer 5
The recommended daily dose of zinc is age-related. Supplementation with elemental zinc should be started at 0.5–1 mg/kg per day. Gastric irritation, nausea and vomiting, the most well characterised side effects of zinc, should be monitored.5
Conclusion
This case illustrates the importance of considering acrodermatitis enteropathica in patients with alcohol consumption and poor diet who present with new plaques and erosions involving acral and perineal skin. The importance of acrodermatitis enteropathica is related to the consequences of an inadequate diagnosis and subsequent lack of zinc supplementation occurred. Additionally, we would like to highlight the rapid clinical improvement secondary to zinc supplementation.
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.