Given these challenges it is important to evaluate the quality of care in multimorbidity. However, while many measures assessing quality of care in primary care have been validated for evaluating the care of specific diseases, little work has been done to evaluate the use of these measures in the context of multimorbidity. Much of the published research tends to focus on specific comorbidities and reports on outcome measures based on one chronic disease against a background of another chronic disease.8 This paper aims to explore the methods used to assess the quality of care in research on primary care patients with multimorbidity. Specifically, our research questions are, for patients with multimorbidity in general practice:
- What measures have been used to evaluate the quality of care?
- What are the limitations experienced when using these measures?
- What other measures should be considered?
Methods
Medline, Scopus, Embase and CINAHL were searched using the search terms identified in Table 1. Snowballing was also used. Articles were subsequently screened by title, abstract and full text to include only quantitative studies that assessed the quality of care in primary care patients with more than one chronic condition (Figure 1).
Table 1. Search terms and definitions
| Search field | Definition | Search terms |
|---|
| Multimorbidity |
The presence of more than one chronic disease in one individual4 |
Multimorbidity, comorbidity; co-morbidity, multi-morbidity |
| Primary healthcare |
Based on the WHO Alma Ata Declaration (1979) definition:55 ‘universally accessible healthcare that addresses the health problems in the community, providing preventive, curative and rehabilitative services accordingly. It is the first level of contact of individuals with the health system’ |
Primary healthcare, family practice, general practice, family medicine |
| Quality of care |
Campbell, Roland & Beutow (2000) definition:56
‘Whether individuals can access the health structures and processes of care which they need and whether the care received is effective’ |
Quality assurance (healthcare), quality of healthcare, patient satisfaction, quality of care, quality indicators (healthcare), healthcare quality, quality control, process assessment (healthcare), outcome assessment (healthcare), health impact assessment, symptom assessment, nursing assessment, self-assessment, needs assessment, outcome and process assessment (healthcare) |
Data were extracted from the 27 studies included. The Donabedian framework of healthcare quality assessment is a useful conceptual framework to examine aspects of quality of care.9 This framework separates quality of care into three interrelated aspects of care: structure, process and outcomes. Structure aspects of care describe the attributes of the healthcare system in which care is delivered. These attributes include access to care and availability of resources, such as medical facilities. The context in which care is provided affects the activities undertaken by the provider and patients. These activities are described under the process heading. Processes of care include the actions of providers when they make a diagnosis, implement treatment or perform cycle-of-care activities, such as routine investigations. These processes ultimately affect the health status of the patient. Measures that describe the patients’ health status, such as the level of disease control, lifestyle modification and functional outcomes, are described under the outcome heading. The quality of care measures identified in the studies included were categorised under the headings of structure, process and outcome used in the Donabedian framework.
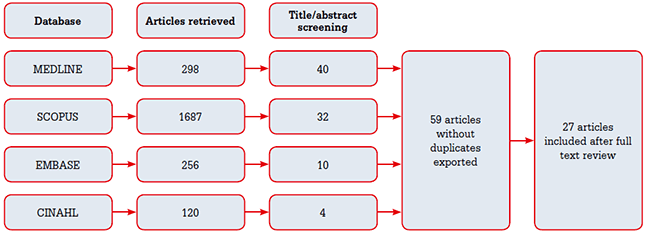
Figure 1. Flow diagram of study inclusion
Other frameworks, such as the Hogg et al10 framework for primary care organisation, can also be used to categorise quality of care measures.The Hogg et al framework separates primary care into structural and performance domains. The structural domain includes characteristics of healthcare systems, the context of the practice and its location, and the organisation of the practice. The performance domain includes technical quality of care and aspects of health service delivery, such as access, the patient–provider relationship, continuity, service integration, comprehensiveness and provider satisfaction. However, this framework does not include patients’ experience of care or patient enablement and empowerment, which are core dimensions of quality of care.11
Results
Quality of care measures from the 27 studies were categorised under the headings ‘structure’, ‘process’ and ‘outcome’. Structure aspects of quality of care were limited to continuity of care measures. Process of care measures included providers’ actions across the care pathway, from recognition of a condition, initiation of care, intensity of treatment and the providers’ adherence to recommended care guidelines. Outcome measures included intermediate outcomes, symptom measures, functional outcomes, appropriate healthcare use and patient rated outcome measures.
Structure
Continuity of care was the only health system attribute assessed. This was assessed in one study using the Usual Provider Continuity of Care Index and the Continuity of Care Index.12 These measures consider referrals, number of providers and number of visits.13 However, they did not consider specific aspects of continuity, such as information continuity, management continuity or relational continuity, which are important care factors in patients with multimorbidity.14
Process
Process measures assess activities across the care pathway.
Recognition of condition
Four studies used recognition of depression to assess the quality of care specifically for depression in patients with multimorbidity.15–18 This was assessed using medical records or patient and provider interviews on the use of mental health services or treatment.
Initiation of care
Initiation of mental healthcare was assessed in one study to measure the quality of care in patients with other physical comorbidities.19 This involved identifying patients who may benefit from mental healthcare and subsequently assessing if mental healthcare was initiated after a primary care visit.
Treatment intensity
Receipt of adequate depression treatment was used to assess the quality of care specifically for depression in patients with multimorbidity.15,17,18,20–23 This involved assessing the number and dosage of medications and number of psychotherapy visits. Treatment processes were also used to assess the quality of care in patients multimorbidity including hypertension24,25 and hyperlipidaemia,26 and in patients receiving care following myocardial infarction.27 These measures assessed whether appropriate follow-up care was received or if treatment was intensified, defined as increasing a medication dosage or changing the medications prescribed. However, competing treatments or contraindications that may have been present in patients with multimorbidity were not considered when using these measures. Additionally cases where failure to intensify treatment is clinically justifiable were not identified.
Recommended care processes
These measures assessed activities that were necessary for the management of chronic disease, including providing advice, screening for and preventing complications. An example was performing retinal examinations on patients with diabetes. These measures were used to evaluate the care of specific conditions such as diabetes in patients with other comorbidities.16,28–33 Recommended care processes were also used to assess the quality of care of multiple conditions in patients with multimorbidity.34,35 This involved using multiple guidelines to obtain relevant care processes and calculating the percentage of indicators that were satisfied. A limitation of these measures is their reliance on care guidelines for specific diseases. While multiple guidelines were used to assess overall quality of care, the majority of care guidelines do not consider patients with multimorbidity.36 Furthermore, these patients are often excluded from clinical trials on which guideline recommendations are made.37
Outcome
Intermediate outcomes
These measures are disease-specific biochemical or physiological indicators of disease severity and control. For example, intermediate diabetes outcomes include HbA1c, LDL-cholesterol levels and blood pressure. These measures were used to assess the quality of care of specific conditions including diabetes, depression and cardiovascular risk management in patients with multimorbidity.16,22,31–33,38–40 A weakness of these measures in patients with multimorbidity is their focus on one disease, not considering the effects of pathological processes or side effects of treatments for other conditions. However, they may identify areas of interactions between conditions.
Symptom measures
These tools measured the symptomatic effects of specific diseases.16,21–23,38 For example, the Hopkins Symptom Checklist was used to evaluate the quality of care for patients with depression care on the basis of changes in depression symptoms.
Functional outcomes
These measured the impact of a chronic condition on a patient’s daily function and quality of life. A number of measures from the Medical Outcomes Study41 have been used in studies of multimorbidity in primary healthcare. For example, the Short-Form Health Surveys 12 and 20 (SF 12 and SF 20) were used to assess social and emotion functioning, general health and pain in patients with depression and physical comorbidities.42 An advantage of using these measures in patients with multimorbidity is that it is not dependent on the care of specific diseases.
Appropriate use of healthcare
Overuse of healthcare was assessed by measuring the rates of inpatient hospitalisation for ambulatory care sensitive conditions (ACSC). These are conditions in which it is thought that good primary care may prevent the need for hospitalisation.29 Overuse of healthcare was also measured by the frequency of inpatient hospitalisation and emergency department attendance by patients with multimorbidity.21,43 Measures of healthcare use are not disease-specific. Therefore, they could be used to assess the overall quality of care for patients with multimorbidity. However, there are concerns surrounding the validity of ACSC as an indicator of quality of care in primary care.44,45
Patient-rated measures
Five studies used patient-rated measures to assess the quality of care. Likert scales were used to assess patients’ satisfaction with the care they received from their GP.16,22 Additionally, patients’ rating of their improvement was assessed in the global impression score.22 Patients’ perceived quality of care was assessed through questionnaires38,46 and the Survey of Health Experience.24 One study used this to determine predictors of quality of care ratings by patients with multimorbidity. Predictors included empathy for the family physician and not having functional limitations.46
Patient-rated measures are important indicators of care outcomes. As Donabedian suggests,9 they may provide an assessment of all aspects of care quality, including providers’ interpersonal skills. While one study found that the patients’ ratings of quality were concordant with intermediate outcomes,38 another study found that patients’ ratings of care were not related to process measures.24
Discussion
Many of the measures reported in the literature to assess the quality of care in primary care patients with more than one chronic condition were disease-specific. These measures may be more appropriate in assessing the influence of a comorbidity on an index condition than in patients with multimorbidity. The search terms used for the databases highlight the problem in this area, as there is a MESH term for comorbidity but not for multimorbidity.
A number of broader measures were not seen in the included studies. These included the General Practice Assessment Survey (GPAS), the General Practice Assessment Questionnaire (GPAQ) and the Primary Care Assessment Survey (PCAS). These tools measure other aspects of care, such as interpersonal care, including physician–patient communication, trust and the GP’s knowledge of the patient, as well as involvement of other members of the healthcare team.47,48 It is unclear why these measures of care were not seen. One possibility is that more objective aspects of care, such as levels of disease control, were valued over other interpersonal attributes of care. However the GPAS has been used recently in a pilot study to determine if guided care improved the quality of primary care experiences in older patients with a high risk of heavy health service use.49
A variety of measures has been used to assess quality of life and functional status in patients with multimorbidity in primary care. Instrumental activities of daily living and the physical health components of the SF 12 and SF 20 have been used to assess the effect of changes to the organisation of care on functional outcomes in patients with multimorbidity in a number of studies with mixed results.8,50,51 While these are particularly valuable in comparing the cost-effectiveness of interventions, they do not measure patient engagement or patient enablement and empowerment. Other more recent measures may provide a better assessment of the patient experience aspect of quality of care in the management of multimorbidity. These include the Patient Reported Outcome Measures (PROMS) of physical, mental and social wellbeing,52,53 and the Treatment Burden Questionnaire which has been recently validated for use in patients with multimorbidity.54Treatment burden is an important aspect of care for patients with multimorbidity, as it may affect treatment adherence, quality of life and other outcomes.
If these are included, a more comprehensive range of assessment measures that are not disease-specific can be used for patients with multimorbidity, as shown in Figure 2. However, through the use of the Donabedian framework, gaps in the use of quality of care measures have been identified. For example, the processes of personalising and prioritising are important elements of the care of patients with multiple chronic conditions that are not addressed.52 A possible direction for future research includes the development of measures that assess these aspects of care. Additionally, studies assessing quality of care through other patient-centred aspects of care, such as patients’ level of trust in their GP and the level of patient empowerment and enablement, are also needed in the context of multimorbidity.
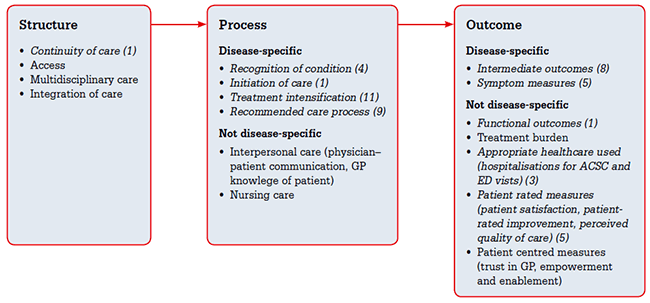
Figure 2. Quality-of-care measures appropriate for use in patients with multimorbidity.
Measures in italics were reported in the studies identified in our review
Conclusion
A variety of measures have been used to assess the quality of care in patients with multiple chronic conditions. However, the reliance on measures oriented towards single conditions has been a major deficiency. Furthermore, there remain gaps across the quality framework after more recent measures are considered. Other measures are needed to provide a more comprehensive way of evaluating quality of care in this group of patients.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.