In Australia, notifiable zoonotic diseases include brucellosis, leptospirosis and Q fever. Exposure to the infectious agent is usually through contact with affected animals or their waste products.3 Brucellosis is almost invariably caused by Brucella suis in Australia, feral pig hunting being the most common risk factor.4–6 Leptospirosis is transmitted through the infected urine of domestic or wild animals and is associated with certain agricultural sectors (eg. banana plantations, dairy farming, dairy cattle) and, very occasionally, contact with contaminated water, particularly floodwater.3,4 Transmission of Q fever is usually airborne through dust contaminated with tissue, birth fluids or excretions from infected animals. The main reservoirs are goats, cattle and sheep.3,4 Roll out of the national Q fever vaccination program between 2001 and 2006 has reduced prevalence in abattoir workers targeted by the program. However, an increasing proportion of Q fever notifications occur in people exposed to livestock, many in non-work settings.7,8
Across Australia in 2010, there were 323 cases of Q fever reported, 131 of leptospirosis and 21 of brucellosis. Overall, 76% of reported brucellosis cases and 64% of leptospirosis cases were in Queensland, while Queensland and NSW had 46% and 41% of Q fever cases, respectively. Patients with these diseases were predominantly male and aged 15–59 years; however, an increasing number of women with Q fever were reported between 2001 and 2010.4,9 Zoonoses are more common in rural and remote areas such as northwest New South Wales and western Queensland.10
Clinical presentation and consequences
The clinical presentation of brucellosis, leptospirosis and Q fever is summarised in Table 1 and a case study is provided. Morbidity can be severe, particularly if the infections are not diagnosed and treated promptly. Acute Q fever progresses to chronic infection in 1–5% of patients. Endocarditis is the most serious consequence and patients with immunosuppression or underlying valvular disease are at the greatest risk.10,11 Without treatment chronic Q fever endocarditis is fatal in most cases, and even with treatment the mortality rate is about 10%.11
Endocarditis is also a complication of brucellosis, whereas leptospirosis progresses to serious disease such as Weil’s syndrome or meningitis in 5–15% of patients.14,15 Leptospirosis can also occasionally be fatal. Patients with zoonotic infections can suffer from chronic fatigue-like illness which lasts for months (leptospirosis) or years (Q fever).12,15,16 Similarly, patients with brucellosis can continue to experience symptoms for extended periods.16
These diseases can also have serious social and economic impacts. A study in northern Australia found that between 1996 and 2009 almost two-thirds of patients with brucellosis had to take more than 1 month off work.6 Manifestations such as post-Q fever chronic fatigue have also been documented, but their exact pathogenesis is unknown.17
Table 1. Clinical presentation of brucellosis, leptospirosis and Q fever4,24
| Disease | Clinical presentation |
|---|
| Brucellosis |
- Typically begins with acute non-specific symptoms. These may include fever, headache, weakness, profuse sweating, chills, weight loss, joint pain, muscle pain and generalised aches.
- Inflammation of the liver or spleen, or gastrointestinal or respiratory signs may occur. In men, the testicles and epididymis may become inflamed. Suppurative infections of organs, osteoarticular complications and neurobrucellosis may also occur.
- Typically symptoms last for 2–4 weeks and are followed by spontaneous recovery. Some infected people may develop an intermittent fever, known as ‘undulant fever’, and other symptoms that fluctuate at 2–14 day intervals. Occasionally symptoms last for a year or more, patients may become chronically ill and symptoms may recur even after successful treatment.
|
| Leptospirosis |
- The usual clinical presentation is fever, chills, headache, severe myalgia (particularly of the calves, thighs and lumbar region) and conjunctival suffusion. Severity varies with the infecting serovar. About 5–15% of cases progress to severe disease:
- Weil’s disease (jaundice, renal failure, haemorrhage and myocarditis)
- Meningitis and meningoencephalitis
- Pulmonary haemorrhage and acute respiratory distress syndrome.
- The case fatality rate increases with increasing age and comorbidities.
|
| Q Fever |
- Clinical presentation is highly variable. It is estimated that 50–60% of cases are asymptomatic. Acute cases may present with fever, sweating and chills, severe headache, myalgia and arthralgia, extreme fatigue, weakness and malaise. Clinical syndromes associated with acute Q fever include pneumonia, hepatitis, osteomyelitis and meningitis or encephalitis.
- Chronic Q fever, defined as an infection lasting more than 6 months, is estimated to occur in 1–5% of those infected. Chronic Q fever presents most commonly as endocarditis or hepatitis and can occur up to 2 years after initial infection. Persons with underlying valvular heart disease have a significantly higher risk of developing chronic Q fever endocarditis.
|
Development of a GP-based algorithm tool for diagnosis and management of zoonoses
Hunter New England Health (HNEH) and a group of GPs in rural NSW who regularly collaborate with HNEH and have an interest in zoonoses, undertook to develop an algorithm tool to assist with diagnosing and treating Q fever, brucellosis and leptospirosis. There were four stages to the development of the tool. First, a literature review was carried out to understand risk factors, clinical presentation, complications, diagnosis and treatment protocols. Second, semi-structured interviews were conducted with five rural GPs who were known to have an interest in zoonotic diseases, and information was analysed using the thematic analysis approach.19 Third, laboratory and infectious disease specialists were consulted regarding alternative diagnoses associated with non-specific presentations that could include zoonoses, and appropriate pathology tests. They were also consulted on laboratory and other direct costs associated with parallel as opposed to serial testing. Finally, a late draft of the algorithm was used to obtain feedback from GPs and infectious disease physicians regarding the application of the tool and possible areas for improvement.
A zoonoses algorithm
The algorithm (Figure 1) for the diagnosis and management of common zoonoses has been developed, incorporating the advice and comments of GPs and laboratory and infectious disease specialists. The GPs involved with the development of the tool reported that the relative rarity of brucellosis, leptospirosis and Q fever was the biggest challenge and most significant issue in documenting the appropriate diagnostic pathways.
Our literature review and survey of GPs failed to locate an existing diagnostic and management tool for zoonotic infections. All the clinicians involved with the project agreed that such a tool would be helpful, and should be brief and available in electronic and paper format. Such a tool could act as an aide-memoire to guide GPs with collection of a clinical history and pathology testing. Management of uncommon but important sequelae are included in the algorithm. GPs requested links to further information, including the Australian antibiotic guidelines and relevant information sheets, as well as contact details for pathology and public health services.
Limitations of the algorithm
The algorithm (Figure 1) is not designed as an exhaustive resource but rather to draw GPs’ attention to the more important elements of diagnosing and managing a patient with brucellosis, leptospirosis or Q fever. It is essential to appreciate that many medical conditions may present with signs and symptoms that could mimic zoonoses and particularly in urban settings other causes should be excluded. However, where a zoonotic infection is suspected, treatment should be started as soon as possible without waiting for the seroconversion to confirm diagnosis, as this may take several weeks.20,21 In the case of Q fever, for example, administration of doxycycline soon after the appearance of symptoms can reduce the length of illness and likelihood of complications.20
There is also individual variability in the presentation of a zoonotic illness, as there is with the time to seroconversion, appropriate treatment protocols and complications. In the case of Q fever, for example, children and pregnant women require specific treatment regimens.22 Cotrimoxazole can be used in children aged 8 years or under, and in pregnant women up until birth to prevent fetal and maternal complications, even if they have recovered from Q fever.22 GPs may see larger numbers of presentations in these groups, given relative increases in the proportion of women, and of non-occupational exposures among Q fever cases.8,9
Finally, it was not possible in a single algorithm to capture all zoonotic infections. Brucellosis, leptospirosis and Q fever were chosen as they are the most common in Australia, but other infectious diseases, such as those caused by rickettsiae, should be considered when testing results for brucellosis, leptospirosis and Q fever prove negative.
Prevention of zoonotic infections is also important and GPs can encourage vaccination against Q fever of patients with regular occupational or non-occupational exposure to C. burnetii. Precise recommendations are provided in the Australian Immunisation Handbook.23 GPs are urged to consult infectious disease specialists and medical microbiologists for further guidance on the prevention, diagnosis and management of zoonotic infections.
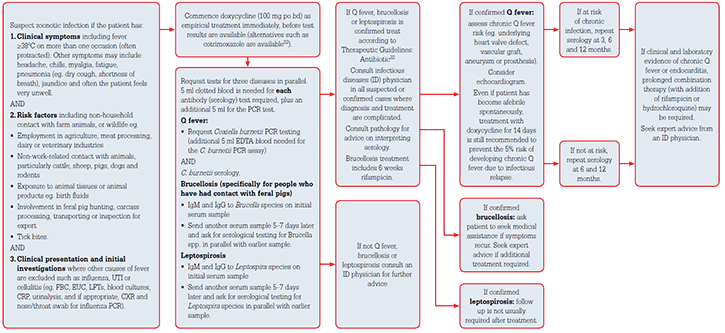
Figure 1. Algorithm for diagnosis and management of zoonotic infections (brucellosis, Q fever, leptospirosis)
UTI = urinary tract infection; FBC = full blood count; LFTs = liver function tests; CRP = C-reative protein; CXR = chest X-ray; EUC = electrolytes, urea, creatinine; PCR = polymerase chain reaction
Conclusion
Zoonotic infections, such as brucellosis, leptospirosis and Q fever, can cause significant morbidity and in some cases death. This article provides a tool to assist GPs with timely and effective diagnosis and management of zoonotic illnesses, when used alongside relevant guidelines and with advice from infectious disease and laboratory specialists.
Case study
A man from northwest NSW, aged 45 years, presented to his GP with fever, chills, muscle pain and night sweats. Questioning revealed that the patient regularly engaged in feral pig hunting at most weekends. Cuts and abrasions were commonly experienced during hunting. He remembered having a particularly bad cut with a contaminated knife 4 months before his current visit to the GP. Symptoms began 6 weeks after this injury. The patient was treated with doxycycline 100 mg bd while serology testing was undertaken.
Following confirmation of brucellosis, doxycycline treatment would need to be continued for a total of 6 weeks. Intravenous gentamicin, 4–6 mg/kg, would also need to be administered for 7 days and plasma concentrations monitored while adjusting the dose accordingly. However, as the patient had not been admitted to hospital and lived a long way from care, the GP chose to prescribe oral rifampicin as an alternative to intravenous gentamicin in addition to doxycycline. The GP was concerned that the patient would elect not to pay for the prescribed course of rifampicin (600 mg daily for 6 weeks) as ‘he doesn’t earn much money’. Brucellosis treatment costs approximately $150 and is not subsidised by the Pharmaceutical Benefits Scheme. The local health service agreed to cover this cost, although the patient still had to make a co-payment.
A year later the same patient presented with fevers and sweats. He had continued to hunt feral pigs. Further serological testing revealed a Brucella species antibody titre of 1:320. A new 6-week course of doxycycline and rifampicin was commenced and the patient’s condition improved.
Competing interests: None.
Ethics approval: Ethics approval was granted by the Hunter New England Local Health District Human Research Ethics Committee (Reference number 13/03/20/5.06).
Provenance and peer review: Not commissioned; externally peer reviewed.