Most smokers would like to quit and approximately 40% have made at least one attempt to do so in the past year.7 The good news is that smoking cessation has substantial and rapid health benefits.4 Primary care has a major role in helping smokers to quit successfully. Brief advice from a general practitioner (GP) increases cessation rates by about two-thirds, compared with no advice, and is highly cost-effective.8 Practice nurses also have an important role in providing this support.9
The 5As approach
The 5As provide health professionals with a framework for structuring smoking cessation support. The elements of the 5As are ask, assess, advise, assist and arrange follow-up.10 Figure 1 shows this approach in detail. The key features are:
- Ask: regularly ask all patients if they smoke and record the information in the medical record.
- Advise: advise all smokers to quit in a clear, unambiguous way such as ‘the best thing you can do for your health is to stop smoking’.
- Assess: assessment of interest in quitting helps to tailor advice to each smoker’s needs and stage of change. Nicotine dependence should also be assessed as this helps to guide treatment. Assessment of other relevant problems, such as mental health conditions, other drug dependencies and comorbidities, is necessary to develop a comprehensive treatment plan.
- Assist: all smokers should be offered help to quit.
- Arrange: follow-up visits have been shown to increase the likelihood of long-term abstinence and are especially useful in the first few weeks after quitting.
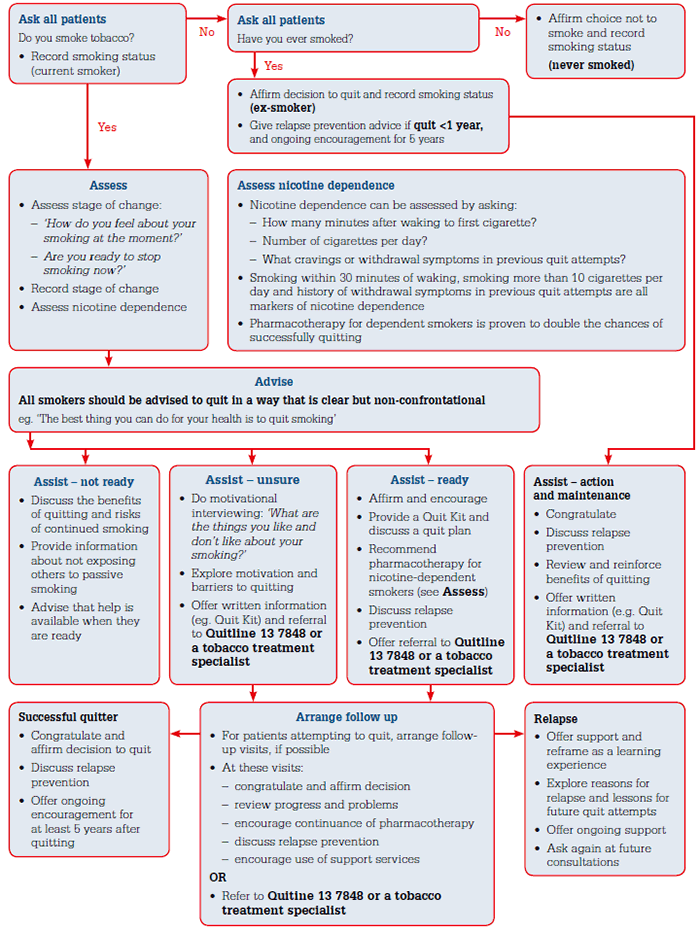
Figure 1. The 5As structure for health professionals for smoking cessation.
Adapted with permission from the Royal Australian College of General Practitioners10
When time is short, the approach of ‘very brief advice’ developed by the United Kingdom National Centre for Smoking Cessation and Training (see Resources) is an alternative. The steps for this are: establish smoking status (ASK), ADVISE that the best way of quitting is with a combination of behavioural support and drug treatment, REFER – provide a referral to a specialised service.
In the Australian context, referral options outside the general practice include:
- Quitline (137 848), which provides free telephone counselling Australia-wide. Referral from general practice to the local state or territory Quitline can be provided by fax or email (Victoria and SA) and some states (Victoria, SA and NSW) now provide feedback to the referring practitioner.
- The Australian Association of Smoking Cessation Professionals website (www.aascp.org.au) has a searchable listing of accredited tobacco treatment specialists.
Counselling and behavioural therapy
If support is being provided in the practice by the GP or practice nurse, the following counselling and behavioural strategies can assist smokers to quit successfully.11,12
- Build rapport and boost motivation.
- Describe withdrawal symptoms and cravings and explore ways of managing these (eg distraction strategies such as doing exercise).
- Agree on a quit date and promote the ‘not-a-puff’ rule.
- Address barriers to quitting and how to overcome these (Table 1).
- Assist with choice of medicines and ensure that patients have a realistic expectation of how these medicines can aid quit attempts, for example, by reducing withdrawal symptoms.
- Identify smoking triggers and discuss strategies to cope with them. For example, minimal or no alcohol in the early weeks of a quit attempt is advised.
- Get support from family and friends, patient support services and printed materials.
- Promote lifestyle changes, such as exercise and avoiding high-risk situations.
- Provide relapse prevention advice.
Relapse is defined as a return to regular smoking. It is most common early in the quit attempt (in the first 8 days).13 Follow up with professional and social support is encouraged to try to prevent relapses but there are currently no proven behavioural interventions.14 Most smokers make repeated attempts to quit before finally achieving long-term abstinence. Each attempt is a valuable learning experience, making the next attempt more likely to succeed. Smokers should be encouraged to keep trying to quit and to make use of evidence-based support to maximise their chance of success.
Table 1. Barriers to quitting smoking
| Barrier | Discussion |
|---|
| Weight gain |
Weight gain after quitting is, on average, 4–5 kg after 12 months. The health benefits of quitting is almost always greater than the health effect of the extra weight. Drinking water and choosing low-calorie foods can help minimise weight gain. Suggest focus on stopping smoking in the short term and deal with any weight gain later. About 1 in 5 quitters do not gain weight. |
| Coping with stress |
Explain to smokers that smoking actually increases stress and that they will be more relaxed after quitting. Some smokers experience repeated episodes of anxiety and restlessness during the day due to nicotine withdrawal between cigarettes. Understandably, when a cigarette relieves these symptoms they assume that the cigarette is relaxing them. Other healthier and more effective ways to relax include breathing and progressive muscle relaxation techniques. |
| Withdrawal from nicotine |
Cravings last only 2–3 minutes, although that may feel like forever! Cravings get weaker and less frequent over time but can persist for many years. Nicotine withdrawal symptoms are at their worst in the first week and typically last 2–4 weeks. They can usually be controlled with stop-smoking medications and behavioural strategies such as distraction techniques and avoiding smoking triggers. |
| Fear of failure |
Explain that most ex-smokers made a number of quitting attempts before finally being successful. Unsuccessful attempts at quitting can be reframed as learning experiences and can increase the chance of success next time. Furthermore, with the right professional counselling, support and medication, the odds of success are much higher. |
| Peer or social pressure |
It may be best to avoid friends who smoke for the first few weeks. Suggest asking friends not to offer cigarettes and, if possible, not to smoke around your patient. If necessary, leave the room while they smoke. Discuss how to respond if offered a cigarette. If the partner smokes, ask him or her to smoke outside. |
Smoking cessation pharmacotherapy
Meta-analyses of clinical trials provide high-level evidence that medicines can assist smoking cessation.15 Pharmacotherapy should be offered to people who are nicotine-dependent and is most effective when used in combination with behavioural support. The medicines approved for smoking cessation in Australia are nicotine replacement therapy (NRT), varenicline and bupropion. These medicines have been shown to be effective in a range of patient populations including smokers with depression, schizophrenia, and cardiac and respiratory diseases. A recent Cochrane network analysis concluded that combination NRT (nicotine patch combined with a fast-acting oral form) and varenicline are the most effective forms of drug treatment and work equally well.15 Bupropion and NRT monotherapy are equivalent in efficacy.15 The choice of pharmacotherapy should be guided by clinical suitability and patient preference (Figure 2).10 Even when smokers receive pharmacotherapy and professional support, overall cessation rates from treatment are modest: 25–30% of smokers quit on any given attempt10,15 (Figure 3).
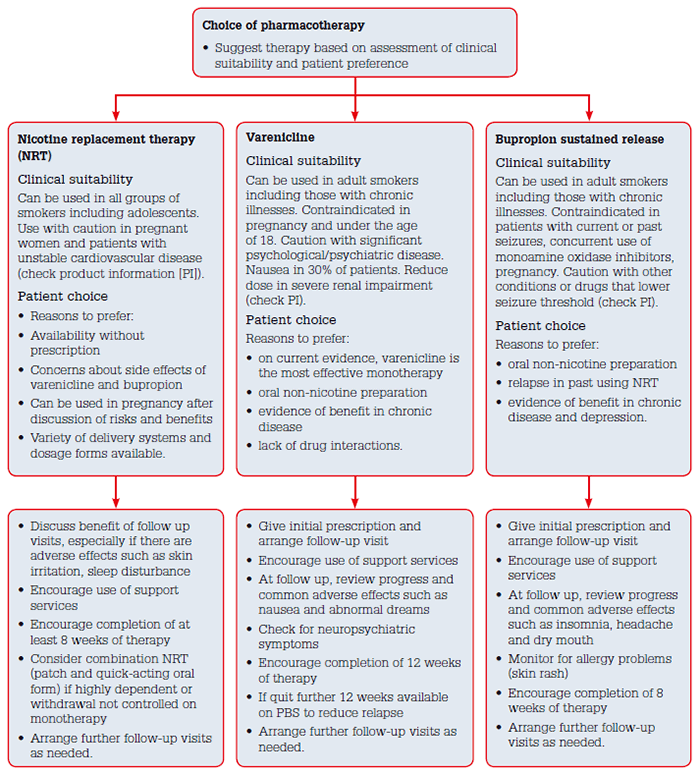
Figure 2. Pharmacotherapy treatment algorithm for nicotine dependent smokers.
Reproduced with permission from the Royal Australian College of General Practitioners10
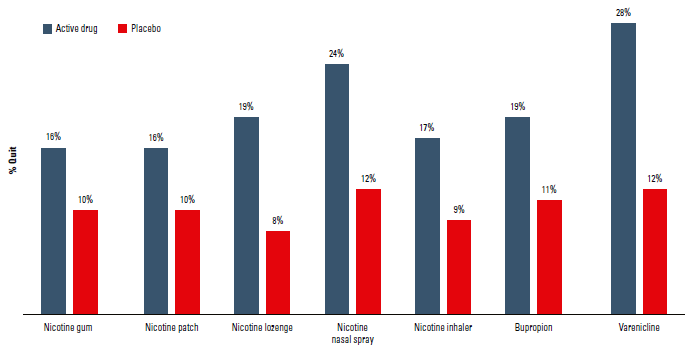
Figure 3. Long-term (>6 month) quit rates for widely available cessation medications15–17
Nicotine replacement therapy
NRT is available in a long-acting form (nicotine patch) and a variety of fast-acting oral forms (gum, inhalator, mouth spray, lozenge, oral strip). All forms of NRT monotherapy have similar efficacy in increasing long-term cessation, compared with placebo (relative risk 1.60, 95% confidence interval 1.53–1.68).16 There is increasing evidence, however, that combining the patch with an oral form of NRT is more effective than monotherapy and should be offered to all nicotine-dependent smokers using NRT.16 Pre-cessation treatment with a nicotine patch (usually started 2 weeks before quit day) has also been shown to improve success rates, compared with starting the patch on quit day. As is the case with all forms of pharmacotherapy for smoking cessation, it is important to help patients understand that to gain maximum benefit they need to take a sufficient dose of NRT to relieve cravings and withdrawal symptoms. NRT should also be taken for a sufficient length of time, generally at least 8–12 weeks. A helpful analogy is a plaster for a fracture – the support needs to be in place for long enough for the healing process to occur.
Varenicline
Varenicline is a nicotinic receptor partial agonist, which acts centrally to relieve cravings and withdrawal symptoms as well as reducing the rewarding effect of smoking. Varenicline is the most effective monotherapy currently available – a Cochrane network meta-analysis found it more than doubled sustained abstinence rates at 6 months follow-up, compared with placebo (risk ratio 2.88, 95% CI 2.40–3.47).15 Nausea occurs in about 30% of users but can be minimised by gradually up-titrating the dose and having the tablets with food.17 Although there have been concerns about neuropsychiatric adverse effects with varenicline, the evidence from a recent meta-analysis is that, compared with placebo, there is no increase in rates of suicidal events, depression or aggression/agitation in patients taking varenicline. This was the case in smokers with and without a history of psychiatric disorders.18 The usual duration of treatment is 12 weeks and for those who have quit successfully at the end of treatment, a second course of 12 weeks can be prescribed to reduce relapse.
Bupropion
Bupropion is another effective medicine with similar efficacy as NRT monotherapy.15 The major concern is a small risk of seizure (approximately 1 in 1000). Bupropion is contraindicated in patients with a history of seizures, eating disorders and in patients taking monoamine oxidase inhibitors. It should be used with caution in people taking medications that can lower seizure threshold, such as antidepressants and oral hypoglycaemic agents.10 The duration of treatment is 8 weeks.
What are other approaches to supporting smoking cessation?
Currently, there is considerable debate about whether e-cigarettes have a role in assisting smoking cessation. E-cigarettes are battery-powered devices that deliver nicotine in a vapour. There is some evidence that e-cigarettes can relieve cravings and other symptoms of nicotine withdrawal but there is limited evidence so far on their efficacy as aids to cessation and major concerns about their current unregulated status.19,20 E-cigarettes have the potential to act as a gateway to smoking and undermine progress on tobacco control by renormalising smoking behaviour.21
Promising areas of research include the use of exercise to assist smoking cessation and the role of mindfulness strategies.22,23
Special groups
Several population groups have either higher rates of smoking or greater risk of adverse effects. One in two Aboriginal and Torres Strait Islander adults smokes and smoking is the largest single risk factor contributing to the health gap between Aboriginal and Torres Strait Islander and non-Indigenous populations. Smoking rates in prisoners are around 83%.24 One in three people with mental illness smokes and the level of nicotine-dependence is usually higher than in the general population.3 There is evidence that people with mental health problems are just as motivated to quit but the intensity and duration of support needed is greater.25–27
Pregnant women are in an important group due to the adverse effects of smoking on the fetus and the increased risk of pregnancy complications. Counselling interventions reduce the proportion of women who continue to smoke in late pregnancy by about 6%.28 There is inconclusive evidence on the efficacy of NRT in pregnancy.29 However, expert opinion is that use of NRT in pregnancy is less harmful than continued smoking.30 If NRT is used, the possible risks and benefits should be discussed. Fast-acting oral forms are generally preferred to reduce total nicotine dose. For a more detailed discussion of smoking in pregnancy see the article by Mendelsohn in the January/February 2014 edition of AFP.31
Effects of smoking and smoking cessation on drug metabolism
Chemicals in tobacco smoke accelerate the metabolism of many commonly used drugs by inducing the cytochrome P450 enzyme CYP1A2. This can substantially lower serum concentrations and effectiveness of these drugs in smokers (Table 2). Conversely, blood levels of these medications may rise when smoking is stopped. Patients should be monitored for adverse effects, and dose reductions may be required. Particular care is needed for drugs with a narrow therapeutic index, such as clozapine, olanzapine and warfarin.32
Table 2. Drugs that interact with smoking: blood levels rise after cessation of smoking
| Class | Medication |
|---|
| Antipsychotics |
Olanzapine, clozapine, |
| Antidepressants |
Duloxetine, fluvoxamine, tricyclic antidepressants, mirtazapine |
| Antianxiety agents |
Alprazolam, oxazepam, diazepam |
| Cardiovascular drugs |
Warfarin, propranolol, verapamil, flecainideClopidogrel (efficacy increased in smokers) |
| Diabetes |
Insulin, metformin |
| Other |
Naratriptan, oestradiol, ondansetron, theophylline, dextropropoxyphene |
| Others |
Caffeine, alcohol |
Harm reduction
Simply cutting down on smoking has not been shown to be sustainable or have health benefits but there is some evidence to support harm reduction using NRT. The most important finding is that in smokers unwilling or unable to quit, cutting down with NRT nearly doubles the chances of smokers progressing to quitting altogether.33
Conclusion
The general practice team has much to offer in helping smokers to quit. This can range from a very brief intervention where smokers are identified and referred for treatment, to a structured program of evidence-based support provided within the practice. The chances of successful quitting are maximised if the patient receives a combination of behavioural support and drug treatment.
Competing interests: Nicholas Zwar has received honoraria for providing advice on smoking cessation programs to Pfizer and GlaxoSmithKline Australia and has received support to attend smoking cessation conferences; Colin Mendelsohn has received honoraria for teaching, consulting and conference expenses from Pfizer, GlaxoSmithKline and Johnson & Johnson Pacific.
Provenance and peer review: Commissioned, externally peer reviewed.
Resources