In the midst of these growing choices it is important to note that learning techniques differ in their clinical effectiveness and in GP preferences. With regard to the relative effectiveness of different learning techniques, previous studies have found that:
- live meetings are more effective than print media2
- individual academic detailing has greater long-term effectiveness than group detailing3
- interactive and procedural formats are more effective than lecture-based CME activities for helping participants retain information and change practice2,4,5
- web-based programs are as effective as live, small-group, interactive programs6
- programs that include multiple techniques (eg. live activities mixed with online activities) are more effective than singular methods.7
Specifically, online education following a live CME course can significantly increase the impact of a face-to-face course.7
Despite this evidence that other learning modalities are more effective, large-group CME activities continue to be predominantly lecture-based.8 In other words, there is a gap between evidence and practice9 and this could be due to a lack of fit between what is effective and what is preferred by GPs. In a previous study, 46% of responding physicians indicated a preference for lecture-based CME activities even though interactive sessions were more effective in helping to retain information: more physicians provided correct answers when attending interactive sessions (39%) than when attending CME using procedural formats (27%) or lecture formats (24%).8 To enable real educational benefits and retention of medical knowledge, CME needs to be both clinically effective and engaging to GPs. Only a handful of studies published in recent years have investigated GPs’ learning preferences10–12 and little research has addressed this issue in Australia, where there are specific CME requirements and practice contexts. This research provides a recent snapshot of the preferences of practicing GPs in Australia for type, delivery mode and motivation for choice of CME activities.
Methods
NPS MedicineWise, an independent, not-for-profit and evidence-based organisation funded by the Australian Government Department of Health, conducts regular surveys of practising GPs to evaluate program effectiveness in improving the quality use of medicines and medical tests in Australia. For the 2012 National GP Survey, a stratified random sample of 2500 GPs was drawn from the Australasian Medical Publishing Company (AMPCo) database. The sample was stratified by state and by geographical location using the Rural Remote Metropolitan Area (RRMA) classification system.13 Sample size was equivalent to 10% of the total national GP workforce.14 Paper-based and web-based versions of the questionnaire were available. The entire questionnaire took about 15 minutes to complete and respondents could opt into a prize draw to win an educational resource.
In March 2012, paper-based questionnaires were mailed to participants, together with details of alternative online completion. GPs in the sample with an email address listed in the AMPCo database (n = 755) were also emailed a link to the online questionnaire. GPs were requested to respond within 7 weeks, during which non-responding GPs were sent two reminders, at 2-week intervals.
In a matrix survey question that permitted multiple selections, GPs selected their preferences for the type of CME activity and delivery mode. We also asked GPs to select three factors from a list of options that they believed to be most influential in their choice of CME activity. Options reflected the main CME types: meetings and workshops,2 audit and feedback,15 educational outreach visits,16 small group-based learning17,18 and self-education (print and digital).19 The survey was piloted with four GPs who had previously indicated willingness to assist NPS with program development. Data were analysed using IBM SPSS Version 20 (IBM, NY). Chi-square tests were performed to examine differences between GP characteristics and GP preferences.
Ethics approval
Ethics approval for this project was granted by the RACGP National Research and Evaluation Ethics Committee (NREEC 11-12).
Results
Of the 2500 questionnaires sent, 128 were undelivered, leaving 2372 eligible GPs. Of these, 714 responded to the survey (582 used the paper-based version and 132 used the online version). Thirty GPs did not identify themselves as currently practising, leaving 684 participants in the analysis. The response rate of 29% is comparable to other Australian GP surveys.20 Respondent demographic characteristics are shown in Table 1. The proportions of GPs surveyed from each state, geographical area, age group and gender were comparable to the distribution in the Australian GP workforce.14,21,22
Table 1. Demographics of survey respondents compared to the national GP workforce
| |
Survey respondents |
National GP workforce14,21,22 |
| Participated in NPS activity in past year |
456 (68%) |
n/a |
| Gender |
| Male |
376 (56%) |
16,357 (59%) |
| Female |
295 (44%) |
11,282 (41%) |
| Age (years) |
| <45 |
182 (27%) |
9,144 (33%) |
| 45–64 |
406 (60%) |
15,051 (54%) |
| ≥65 |
84 (13%) |
3,444 (12%) |
| Years in practice |
| 0–5 |
71 (11%) |
n/a |
| 6–15 |
147 (22%) |
n/a |
| ≥16 |
452 (68%) |
n/a |
| Practice size |
| 1 GP (solo practice) |
58 (9%) |
2,456 (10%) |
| 2–5 GPs |
282 (42%) |
n/a |
| ≥6 GPs |
328 (49%) |
n/a |
| State |
| NSW and ACT |
191 (28%) |
9,070 (33%) |
| QLD |
127 (19%) |
5,810 (21%) |
| SA |
76 (11%) |
2,253 (8%) |
| TAS |
45 (7%) |
719 (3%) |
| VIC |
177 (26%) |
6,710 (24%) |
| WA |
68 (10%) |
2,614(9%) |
| Remoteness area classification25 |
| Major city |
458 (67%) |
18,398 (70%) |
| Regional areas |
215 (31%) |
7,279 (28%) |
| Remote and very remote area |
11(2%) |
633 (2%) |
GPs’ preferences for CME (which combine CME type and delivery mode) are shown in Table 2. The options selected by more than one-third of respondents are shown. Most GPs indicated a preference for learning in a group as opposed to learning on their own. Specifically, lecture-based CME was preferred most often; 83% of GPs preferred to learn in a group in a face-to-face format with an expert; 70% selected face-to-face group learning with a more interactive format; and 66% of GPs preferred an individual academic detailing style (one-to-one learning with an expert).
Table 2. GPs professional learning preferences
| Preferred learning option selected |
All GPs
N=684
n (%) |
Age of GP (years) |
Size of GP practice |
<45, N=182
n (%) |
45–64, N=406
n (%) |
≥65, N=84
n (%)
|
P value |
Solo, N=58
n (%) |
Non-solo, N=610
n (%)
|
P value |
| Learning in a group with an expert or speaker (face-to-face) |
565 (83) |
153 (84) |
337 (83) |
64 (76) |
0.261 |
44 (76) |
506 (83) |
0.157 |
| Group discussion with other health professionals (face-to-face) |
480 (70) |
132 (73) |
288 (71) |
52 (62) |
0.188 |
35 (60) |
433 (71) |
0.087 |
| One-to-one with an expert or representative (face-to-face) |
454 (66) |
131 (72) |
269 (66) |
46 (55) |
0.022 |
36 (62) |
409 (67) |
0.468 |
| Self-education (online) |
375 (55) |
131 (72) |
213 (53) |
26 (31) |
0.000 |
23 (40) |
342 (56) |
0.015 |
| Self-education (paper) |
293 (43) |
69 (38) |
180 (44) |
40 (48) |
0.229 |
25 (43) |
262 (43) |
0.966 |
| Clinical audit (online) |
243 (36) |
68 (37) |
150 (37) |
20 (24) |
0.059 |
16 (28) |
219 (36) |
0.187 |
| Clinical case study (online) |
231 (34) |
79 (43) |
133 (33) |
16 (19) |
0.000 |
13 (22) |
214 (35) |
0.056 |
| Clinical audit (paper) |
228 (33%) |
51 (28) |
143 (35) |
31 (37) |
0.180 |
20 (35) |
201 (33) |
0.846 |
With regard to online CME, 55% of GPs indicated a preference for online self-education. Older GPs were less likely to prefer online learning, particularly online self-education (Figure 1), as were GPs working in solo practices (Figure 2). Not surprisingly, respondents who chose to complete the survey online were also more likely to prefer online CME.
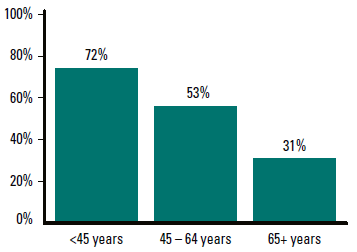
Figure 1. Percentage of GPs who prefer online self-education by age group
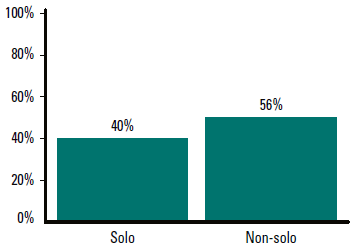
Figure 2. Percentage of GPs who prefer online self-education by practice size
Table 3 shows the frequency of factors influencing choice of CME activity. ‘Relevance to clinical practice’ was the most frequently selected reason for choosing a CME activity, whereas ‘interaction with other GPs or health professionals’ was least often selected.
Table 3. Factors influencing choice of CME activity
| Reason for choice of CME activity |
Participants
n = 684 |
| Relevance to area of practice |
544 (80%) |
| Keeping up to date |
368 (54%) |
| Convenient time, method or location |
332 (49%) |
| Educational value |
217 (32%) |
| Within my area of interest |
173 (25%) |
| Leads to immediate changes in management of individual patients |
117 (17%) |
| CME points |
82 (12%) |
| Minimal time or effort |
77 (11%) |
| Preferred delivery format |
76 (11%) |
| Interaction with other GPs or health professionals |
69 (10%) |
Discussion
In the present study, peer-group learning contexts were consistently preferred over other contexts (regardless of expert input) and clinical relevance was the most important motivator for choice of CME activity. Considering these results, it is plausible to suggest that GPs prefer group learning and believe this format is effective in providing relevant clinical learning. Although previous studies have shown group-based learning is less effective than individual academic detailing,3 other studies have shown interactive CME programs are effective in comparison to other CME types,2,4,5 as are CME programs with a discussion component.23 A limitation of this study is that this question could not be explored in greater depth as we did not specifically differentiate between interactive group learning with a speaker and non-interactive group learning with a speaker.
Nevertheless, many studies have found that GPs prefer face-to-face group learning because it allows a degree of personal interaction.12,24 Although few GPs explicitly identified ‘interaction’ as a driver for their choice of CPD activity, face-to-face group learning offers GPs an opportunity to network with other GPs and specialists, as well as to break from their normal routine, travel and seek relief from the everyday pressures of general practice.25 This may be another reason for preferring group learning formats irrespective of potential clinical effecitveness. Our finding that GPs in solo practices were least likely to prefer online learning may also support this notion. For GPs working in solo practices, online learning can be an isolating experience.
The present study also showed that more than half of the GPs surveyed have a preference for CME delivered online. While online learning can be isolating, it is generally more flexible than organised sessions and is likely to appeal to time-poor GPs.26,27 Previous research indicates online learning is convenient because it enables a level of control over how content is accessed, the depth of learning and time spent, while allowing learners to find information in a format that best suits their current needs.28 It is unlikely, however, that preferences for online CME are driven by time factors alone. In the present study, online CME was largely selected in addition to face-to-face group learning (not instead of) so it is likely that the flexibility provided by online CME is valued as an addition to the benefits of face-to-face group learning. This is likely to be an effective combination, as previous studies have shown online learning can be particularly effective when it follows live, face-to-face CME.7 Online learning was also particularly well regarded among younger GPs, which suggests that familiarity with online technologies resulting from previous educational experiences29 may be a driver of online CME preferences.
The present study indicates there is still a gap between GPs’ preferences and the clinical effectiveness of CME activities. Participating in a range of CME activities such as interactive group discussions, online self-education and one-to-one learning may provide GPs with a good balance and enable medical education that is both engaging and clinically effective.
Key points
- As we move into the digital era, conventional learning forms such as group face-to-face activities remain very popular and beneficial for both clinical learning and personal interaction with peers.
- When organising large-group CME activities, it is important for educators to use interactive styles (eg. discussions) to maximise clinical effectiveness and a combination of methods to engage GPs with varying preferences.
- Online learning is a more convenient CME option and provides value-added clinical learning, particularly when used in combination with face-to-face group learning.
- GPs are likely to benefit most from undertaking a range of CME activities, including less-preferred activities such as individual academic detailing and practice-based self-assessment.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.