With respect to urgent patient presentations, non-clinical staff should be able to: 5,6
- describe practice procedures for obtaining urgent medical attention
- identify a patient presenting with a suspected urgent medical matter
- handle an urgent medical matter by phone, or in person and with or without a general practitioner (GP) in attendance.
Australian standards require practices to demonstrate formalised triage processes and facilitate training for non-clinical staff relating to urgent medical matters.7 Despite this universal obligation, there is no ‘gold-standard’ approach to support non-clinical staff in managing patients with urgent needs, and current ‘triage tools’ have not been thoroughly evaluated.8 ‘BeAWARE of the warning signs of heart attack and stroke’ was developed to empower non-clinical practice staff to promptly identify patients presenting with suspected warning signs of heart attack and stroke. This paper describes the preliminary outcomes from the evaluation of the BeAWARE initiative.
Methods
The target audience for BeAWARE is non-clinical staff working in primary care in Australia. BeAWARE was launched on 5 May 2012, corresponding with National Heart Week, and was subsequently promoted to non-clinical staff and GPs through in-practice advertising. Participant and practice uptake was tracked from May to December 2012.
BeAWARE comprises an online learning module and optional in-practice resources (desktop reference card and posters for the patient waiting area). The online learning module takes about 20-minutes to complete and includes four topic areas:
- warning signs of heart attack
- warning signs of stroke
- watch, listen, ask
- calling triple zero (000).
More information on BeAWARE can be found at www.heartfoundation.org.au.
Integrated into the online learning module is a pre- and post-assessment. All participants were prompted to complete the pre-assessment on registration and the post-assessment directly following module completion, before receiving their certificate on completion. The assessment was delivered online and consisted of four structured questions designed to measure changes in knowledge of warning signs (one question each for heart attack and stroke, open-ended to measure unprompted recall of symptoms), confidence in knowing what to do and intended action (closed-ended questions with a response scale measuring level of confidence and intended action).
Using SPSS, 18.0, the pre- and post-assessment data were collated, coded and analysed. Paired sample t-tests were conducted to measure differences between pre- and post-assessment data, using a 95% confidence interval. Analysis was conducted for the two participant groups: non-clinical and clinical participants. Non-clinical participants were defined as practice staff whose primary role was not of a clinical nature, such as receptionists and practice managers. Clinical participants were classified as GPs, nurses and other health professionals. As this study was of aggregate, de-identified data that were collected primarily for in-house quality assurance purposes, no formal Human Research Ethics Committee approval or exemption status was required.
Results
From May 2012 to December 2012, there was a total of 2017 registrations for the online learning module (OLM) and 1865 (92%) completions. Participants originated from 815 general practices nationally. Of those completing the online learning module 64% (1189) were non-clinical participants. (Figure 1).
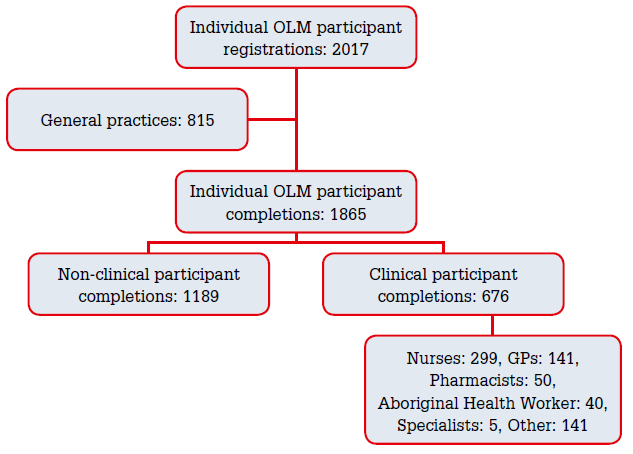
Figure 1. Uptake of BeAWARE (5 May–31 December 2012)
OLM, online learning module
Tables 1 and 2 show the pre- and post-module results in unprompted recall of heart attack and stroke symptoms among non-clinical and clinical staff. Statistically significant increases in recall were evident for the common symptoms of heart attack and stroke among both groups. Unprompted recall of ‘chest tightness’ (pre: 23.4%, post: 48.7%; P <0.05), ‘jaw pain’ (pre: 27.1%, post: 79.9%; P <0.05), ‘shoulder pain’ (pre: 15.9%, post: 41.3%; P <0.05), ‘facial droop’ (pre: 43.2%, post: 87.7%; P <0.05), ‘unable to raise arms’ (pre: 13.9%, post: 83.1%; P <0.05) and ‘slurred speech’ (pre: 69.7%, post: 90.0%; P <0.05) significantly increased among non-clinical participants. There was a significant fall in unprompted recall for several less commonly recognised and promoted heart attack and stroke symptoms.
Table 1. Warning signs of heart attack – participant recall
| Warning sign | Clinical participants (%) | Non-clinical participants (%) |
|---|
| Pre | Post | Pre | Post |
|---|
| Chest pain |
87.9 |
92.6* |
87.8 |
85.7 |
| Tightness in chest |
25.1 |
51.4* |
23.4 |
48.7* |
| Arm pain |
64.3 |
65.0 |
65.4 |
60.6* |
| Weak/heavy arms |
1.0 |
2.3 |
0.7 |
1.9 |
| Jaw pain |
34.3 |
81.3* |
27.1 |
79.9* |
| Neck pain |
20.9 |
42.9* |
15.9 |
41.0* |
| Back pain |
20.0 |
51.4* |
16.0 |
46.0* |
| Shoulder pain |
18.2 |
43.5* |
15.9 |
41.3* |
| Shortness of breath |
66.4 |
67.1 |
65.7 |
61.7 |
| Feeling dizzy |
16.4 |
40.3* |
21.2 |
42.2* |
| Feeling faint/collapsing |
10.1 |
2.1* |
8.0 |
2.3 |
| Nausea/vomiting |
27.7 |
43.5* |
25.5 |
43.3* |
| Sweating/clammy |
50.3 |
52.5 |
40.8 |
50.8* |
| Numbness |
4.3 |
1.2 |
7.5 |
1.4 |
| Palpitations |
8.4 |
0.9 |
6.5 |
0.5 |
| Paleness/greyish skin |
19.2 |
17.5 |
12.4 |
16.6* |
| Indigestion/heartburn |
6.1 |
2.1* |
4.0 |
1.2 |
| Tingling sensation |
7.8 |
1.2* |
12.0 |
2.0* |
| Fatigue |
4.4 |
2.3* |
2.7 |
1.2 |
| Anxiety |
6.2 |
2.1* |
2.1 |
0.6 |
| Pain (general) |
9.6 |
5.9* |
7.3 |
7.8 |
| Other |
14.8 |
3.0* |
11.6 |
1.6 |
| Unsure |
0.9 |
0.9 |
1.1 |
1.0 |
| Q1. What signs or symptoms would you associate with having a heart attack? *P <0.05 |
Table 2. Warning signs of stroke – participant recall
| Warning sign | Clinical participants (%) | Non-clinical participants (%) |
|---|
| Pre | Post | Pre | Post |
|---|
| Facial droop |
41.6 |
87.8* |
43.2 |
87.7* |
| Unable to raise arms |
10.5 |
74.9* |
13.9 |
83.1* |
| Slurred speech |
70.3 |
89.2* |
69.7 |
90.9* |
Weakness – face, arms
& legs |
38.8 |
23.7 |
24.2 |
13.4 |
| Persistent headache |
37.3 |
41.5 |
29.5 |
34.7* |
| Unable to understand someone |
5.0 |
12.9* |
6.1 |
15.6* |
Unresponsive
(yet conscious) |
4.9 |
0.9 |
4.5 |
2.1 |
| Blurred vision |
22.8 |
13.8 |
19.8 |
6.9 |
| Memory loss |
2.8 |
0.2 |
2.8 |
0.9 |
| Disorientation/confusion |
25.7 |
13.8 |
25.2 |
11.9 |
| Unco-ordinated/loss of balance |
13.5 |
8.1 |
13.3 |
6.0 |
| Dizziness |
13.6 |
18.2* |
15.1 |
17.3 |
| Collapse/loss of consciousness |
14.3 |
3.5 |
7.7 |
1.4 |
| Pain |
4.0 |
1.2 |
6.3 |
1.6 |
| Difficulty swallowing |
9.3 |
5.8 |
5.3 |
3.0 |
| LoM/paralysis/numbness |
43.9 |
14.1 |
47.4 |
13.4 |
| Dribbling |
4.0 |
1.8 |
1.8 |
0.1 |
| Nausea/vomiting |
3.3 |
2.3 |
2.9 |
2.7 |
| Sweating/clammy |
2.5 |
0.9 |
3.1 |
1.9 |
| Unsure |
1.2 |
0.9 |
1.2 |
0.9 |
| Q2. What signs or symptoms would you associate with having a stroke? *P <0.05 |
Figures 2 and 3 show the change from pre- to post-module in personal confidence in knowing how to respond to a patient presenting with warning signs. Non-clinical participants indicating ‘very confident’ increased from 24.5% to 81.7% (P <0.000). Clinical participants indicating ‘very confident’ increased from 30.8% to 85.9% (P <0.000).
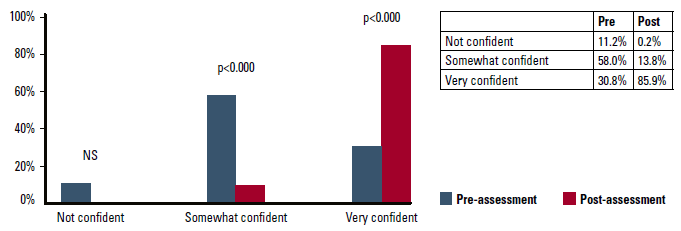
Figure 2. Confidence in knowing what to do (non-clinical staff)
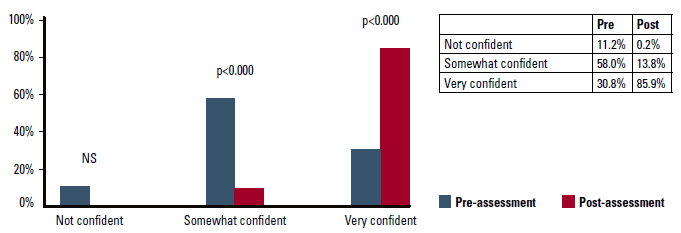
Figure 3. Confidence in knowing what to do (clinical staff)
Figures 4 and 5 show the change from pre- to post-module in intended action in response to a patient presenting with warning signs. A greater proportion of non-clinical participants indicated they would ‘tell a GP/nurse immediately’ (pre: 64.1%, post: 74.8%; P <0.000) and fewer indicating they would call 000 (pre: 32.0%, post: 24.4%; P <0.000).
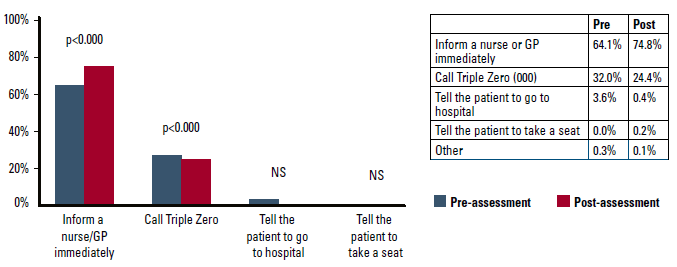
Figure 4. Intended action (non-clinical staff)
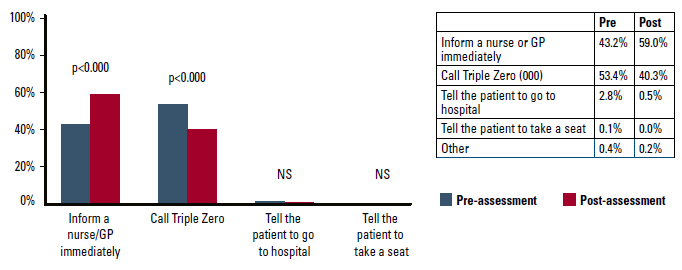
Figure 5. Intended action (clinical staff)
Discussion
The uptake of BeAWARE among general practice has exceeded expectations. Staff from 815 individual general practices participated in BeAWARE within the first 8 months, representing an estimated 12% of all practices nationally.9 Despite BeAWARE being purposefully developed for non-clinical practice staff, there were 676 clinical participants, representing 36% of total participants. The authors view the overall response as an endorsement from the sector that BeAWARE fulfils a safety 'gap' for patients presenting with suspected heart attack or stroke.
Non-clinical reception staff work in a complex, high-stress environment and are regularly required to make distinctions between routine and urgent appointments.10 With respect to emergencies, the primary role of non-clinical staff is to promptly identify patients presenting with urgent needs and immediately escalate them to a GP or nurse for rapid clinical assessment.11 It is essential, therefore, that they have the necessary knowledge of heart attack and stroke warning signs. The aim of the BeAWARE module is to provide non-clinical staff with this knowledge and support prompt identification of common heart attack and stroke symptoms. The recall of the common heart attack and stroke warning signs by non-clinical and clinical participants improved markedly post module. The significant increases were consistent with the heart attack and stroke symptoms included in the BeAWARE learning module. They also align with the campaign messaging and materials from the Heart Foundation’s ‘Warning Signs of Heart Attack Action Plan’ and the Stroke Foundation’s FAST campaign. It was not surprising that there was an accompanying decrease in recall of less common symptoms, as these were not included in the BeAWARE learning module. Further, the decrease in recall of less common symptoms may be related to the open-ended, unprompted structure of the assessment question as opposed to a lack of knowledge or awareness of less-common symptoms among participants.
Despite the significant increases in recall of common symptoms among non-clinical staff, in comparison, there was a greater increase in the recall of some symptoms among clinical staff. This may reflect the benefit of BeAWARE in assisting clinical staff to consolidate previous education and training undertaken on the clinical presentation of heart attack and stroke. These increases are encouraging, given the key role of nurses and GPs in clinically assessing the patient and determining the ultimate course of medical action.
A significant shift was observed among non-clinical participants’ intention to ‘call triple zero (000)’ to ‘engaging an onsite GP or nurse immediately’. This outcome was consistent with BeAWARE content and its intention to reinforce and support standard processes in general practice. Non-clinical staff need a certain level of knowledge of warning signs to be able to promptly identify patients and initiate the triage process, but it is the responsibility of the GP or nurse to determine the appropriate level of care patients require.12 At the point of rapid clinical assessment, the GP or nurse should then decide if an ambulance is required. On the basis of this, it is not expected that BeAWARE will result in changes to the number of patients taken to hospital but rather, will expedite this process. It is important to note however, when a GP or nurse is not present (eg. opening of the practice), non-clinical staff should call 000 immediately for patients who present with warning signs.11
Interestingly, the shift to ‘engage an onsite GP or nurse’ was more notable among clinical participants, compared with non-clinical participants. As BeAWARE was developed and promoted primarily for non-clinical staff, this outcome may reflect clinicians responding to the module assessment from a non-clinical perspective, consequently educating GPs and nurses on the role of non-clinical staff in patient triage.
Effective triage within general practice requires a whole-of-practice approach for dealing with patients who present with a broad range of needs. BeAWARE is just one component of an effective triage strategy. A triage protocol developed with input from all staff, in conjunction with appropriate staff training, will not only aid practices to adhere to accreditation standards but could ultimately safeguard against risk of medico-legal liability in the case of an adverse patient event.13
Despite the directive of practice triage standards, there remains considerable scope to improve patient triage processes through robust performance monitoring and feedback and the development of evidence-based approaches by primary healthcare agencies and regulators. The Royal Australian College of General Practitioners (RACGP) has developed universal practice indicators for the Australian setting which include patient triage, however these are currently voluntary for practices to implement.14
BeAWARE was designed to fulfil a niche, but critically important, patient safety gap in general practice. However, there are certain circumstances beyond its scope, particularly issues pertaining to patient compliance that have the potential to delay definitive treatment. Some patients may be unwilling to disclose any information, may disclose inaccurate information and/or may be unwilling to follow the advice given to them by the receptionist or nurse (eg. call 000) due to a number of socio-demographic and situational factors.15 The ‘watch, listen, ask' module of BeAWARE endeavours to make non-clinical staff aware that disclosure of information (or lack of) from patients is a potential barrier to acquiring quick and accurate information.
Practices also have an obligation to educate their patients to call 000 for an emergency and regularly inform patients on how the practice manages urgent matters to aid the likelihood of patient compliance to reduce delay to appropriate treatment.
Finally, given the variable frequency of patients presenting to general practice with warning signs of heart attack or stroke, it is possible the immediate increases in knowledge observed may not translate into appropriate action. This underpins the importance of periodic revision of warning signs knowledge and the provision of reference material at the point of patient presentation. We recommend non-clinical staff undertake the module at least once every 12 months, to maintain their knowledge base, and order a resource pack to receive the desktop reference card for their practice.
Conclusion
BeAWARE increases knowledge of heart attack and stroke warning signs and confidence in knowing how to respond among non-clinical general practice staff. This will aid practice triage processes and support prompt identification and escalation of patients presenting with heart attack and stroke warning signs in general practice. Despite the encouraging response rate for BeAWARE, ongoing promotion and support from key stakeholders is required to ensure its uptake is further extended.
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.