Since the introduction of the National Human Papillomavirus Vaccination Program for young women in 2007, the incidence of genital warts has fallen dramatically in young Australian heterosexuals.1 With the extension of this vaccination program to young men, it is expected that the incidence of genital warts will fall further and will also decline in homosexual men: genital lumps in young adults are now less likely to be warts. This article aims to assist diagnosis by outlining some common anatomical variants and comparing them to a few pathological conditions. There are other conditions that may cause genital pathology that are not covered, and treatment is not discussed in detail.
Most anatomical variants share characteristic features that help with recognition, such as symmetry, a smooth surface and well circumscribed border. Normal variants should not produce any symptoms of pain or be associated with inguinal lymphadenopathy. Table 1 outlines some typical features that are suggestive of genital warts. Despite these features, it can sometimes still be difficult to be sure, especially if the appearance is atypical. Having access to a bank of images, such as those on the Melbourne Sexual Health Centre website (www.stiatlas.org), is very useful. These images can also be used to reassure patients and educate them on the differences between normal anatomy and conditions that would require treatment.
Table 1. Distinguishing characteristics of a genital wart compared to a normal anatomical variant
| Wart likely | Normal anatomical variant likely |
|---|
| History |
Unvaccinated
Sexual contact with genital warts |
Previous quadrivalent-HPV vaccination, especially if given before the commencement of sexual activity |
| Appearance |
- Irregular
- Rough
- Asymmetrical
- Cauliflower or cobblestone appearance
- Evidence of keratinisation
- whitening of lesion with dilute acetic acid
- white frond tips
|
- Regular
- Smooth
- Symmetrical
|
| Dermoscopy |
Irregular projections with hairpin, comma-like and irregular vasculature surrounded by a whitish band |
- Normal
- Delicate
- Central capillary dilation
|
| Over time |
New lesions appear, previous lesions increase in size |
No or minimal change |
Normal variants
Pearly penile papules
Pearly penile papules (PPPs) are tiny lumps seen in neat rows around the corona of the glans penis (Figure 1). They can occur as a single row, or in multiple orderly rings encircling the corona. PPPs are numerous, uniform, symmetrical and dome shaped, and vary from 1 to 3 mm in length. PPPs occur in up to 20% of men and are frequently mistaken for warts, but bear no relationship to them.2,3 In difficult cases dermoscopy can be useful, as PPPs will have delicate, regular vessels that are distinct from genital warts. Histologically, PPPs resemble angiokeratomas.
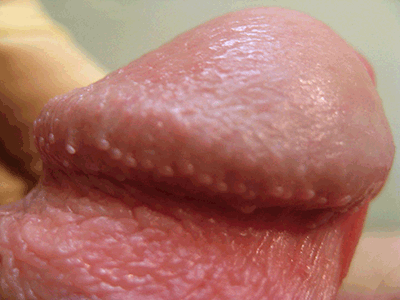
Figure 1. Pearly penile papules
Fordyce spots
Fordyce spots are visible sebaceous glands and occur along the shaft of the penis (Figure 2).4 They often appear in adolescence. Fordyce spots are more easily visible when the skin is stretched, and many patients may describe them as a lump that appears during an erection. Spots may also appear on the scrotum. Some patients may be able to express a thick, chalky discharge by squeezing the lump. Fordyce spots may also appear in other areas such as at the vermillion border of the lips when, if seen, can help reassure the patient that they are a normal anatomical variant that does not require any treatment.
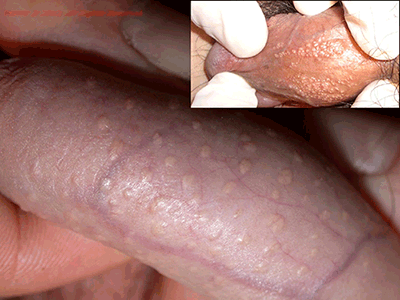
Figure 2. Fordyce spots (penile sebaceous glands)
Tyson glands
Tyson glands are ectopic sebaceous glands that appear in pairs as openings on either side of the frenulum (Figure 3). As they are normal structures, treatment is not required.5
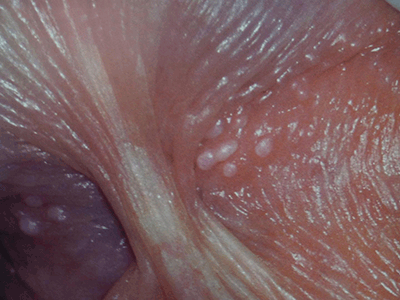
Figure 3. Tyson glands
Angiokeratomas
Angiokeratomas can occur alone or in multiples and appear as deep-red or purple papules, usually over the scrotum. They can also appear on the penis (Figure 4). Angiokeratomas advance with age and represent a collection of enlarged capillaries.6 Treatment is only required if they bleed frequently.
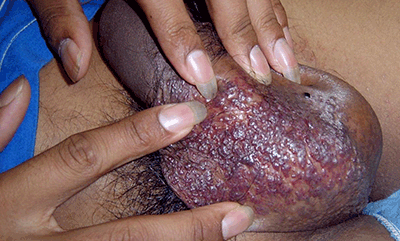
Figure 4. Angiokeratomas of the scrotum
Lymphocoeles
Lymphocoeles present as a palpable cord-like structure that can occur vertically or horizontally at the shaft of the penis (Figure 5). They are associated with friction and increased sexual activity. Lymphocoeles are probably due to sclerosing lymphangitis, an inflammatory process caused by a thrombosed vessel.7 Sclerosing lymphangitis can also occur in the presence of some sexually transmissible infections (STIs) such as Neisseria gonorrhoea or syphilis, and appropriate STI screening may be necessary. The thrombosed vessel will usually spontaneously recanalise and therefore the condition itself requires no treatment.
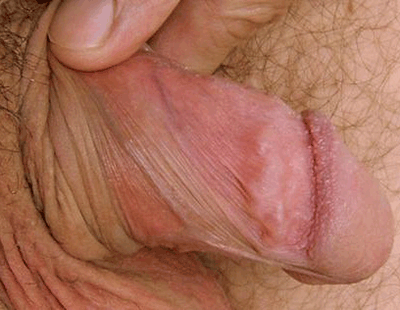
Figure 5. Lymphocoele. Also note small pearly penile papules
Skin tags
Also known as acrochordons, skin tags are common in the skin creases of the groin in middle aged men. They typically have the size and shape of a grain of rice. They are often also present in the axillae and on the lateral skin of the neck. Skin tags have a fibrovascular centre and normal overlying epidermis.
Penile lumps that may require treatment
Warts
Penile warts(Condylomata acuminata) are irregular, rough lesions that can occur anywhere along the penile shaft, glans and prepuce; they can also arise from the meatus. Warts vary in size from a millimetre to a few centimetres. Warts on the shaft of the penis or pubic area tend to be more indurated and dome shaped, whereas those under the prepuce or emerging from the urethra are softer and fronded (Figure 6). A smooth-looking wart may be difficult to distinguish from an acrochordon (skin tag) or other normal structure, but using a bright light and magnification will reveal fine dots or a cobblestone pattern. Warts are most commonly due to strains 6 and 11 of HPV.8 There are a number of options for treatment including cryotherapy, podophyllotoxin and imiquimod. All of these therapeutic options typically require multiple treatments over a number of weeks. As the natural history of HPV in immunocompetent hosts is spontaneous recovery over 12–24 months, patients may also opt to have no treatment.9,10
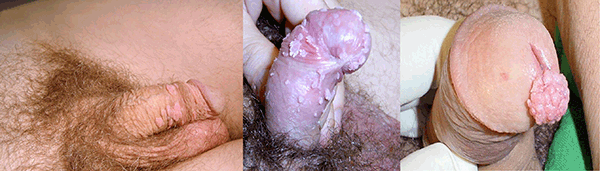
Figure 6. Penile warts
Molluscum contagiosum
Molluscum contagiosum appear as small papules with a central depression or umbilication. They are caused by a member of the poxvirus family, molluscum contagiosum virus (MCV). Molluscum contagiosum are commonly acquired by children from non-sexual skin contact, often during bathing or swimming with other infected children. In adults however, sexually transmitted molluscum may be seen on or near the genitals (Figure 7). The virus has a self limiting course over a period of months, but treatment with cryotherapy is often recommended to prevent the spread of MCV to others.11,12
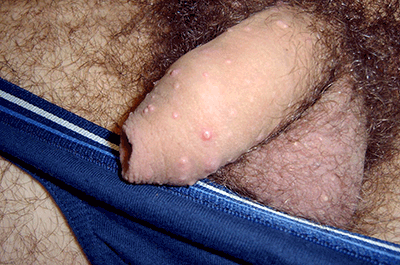
Figure 7. Molluscum contagiosum
Folliculitis
Folliculitis is an inflammation of the hair follicles, frequently seen at the base of the penis (Figure 8). Folliculitis presents as a pustule around the hair follicle, which is frequently itchy and sometimes painful. Patients are often concerned that genital herpes simplex virus (HSV) is the cause, but the association with a hair follicle and the quality of the pain helps distinguish folliculitis from HSV. If a lesion is aspirated, thick purulent material (which may be blood stained), is often seen, whereas, vesicles due to HSV express a clear or straw coloured fluid. Herpes simplex virus may also be associated with a prodrome of malaise, fatigue and paraesthesia of the affected area. Molluscum contagiosum lesions is another casue occasionally confused with folliculitis, but there is sometimes a red halo. Folliculitis is often successfully managed with topical treatments and genital hygiene measures, but may need appropriate antimicrobial therapy if there is a surrounding cellulitis or a large number of lesions.
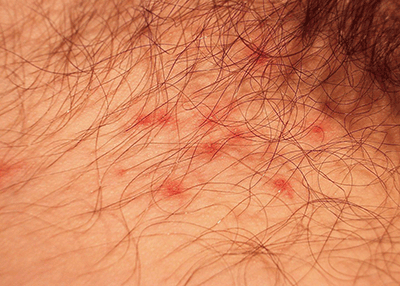
Figure 8. Folliculitis
Primary syphilis
An early syphilis chancre may present as a non-ulcerated, button shaped lump on the penile skin. Chancres are often indurated and there is usually some sign of epidermal breakdown or inguinal lymphadenopathy. Syphilis serology may be negative for the first few days of a chancre and should be repeated 2–4 weeks later if syphilis is suspected. In very early syphilis, treponemal polymerase chain reaction (PCR), using a dry cotton swab vigorously rubbed on the lesion at the time of the initial consultation, may be more likely to yield a positive result. While only some specialist laboratories perform this, most can forward the specimen on for appropriate testing.
Scabies
Genital scabies presents as intensely itchy, pink nodules (Figure 9). Patients usually have some sign of scabies elsewhere, such as the wrists, fingers and lower abdominal skin, which may include typical linear burrows.
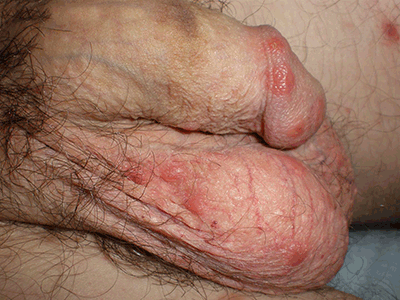
Figure 9. Scabies
Subcutaneous lumps
Lumps beneath the skin are uncommon on the penis and are more likely to represent pathology. An important diagnosis to consider is Peyronie disease, which can present as a plaque attached to the tunica albuginea, usually in the proximal half of the penis. The skin moves freely over this, and patients may have noticed curvature of the erect penis. In some cultures there is a practice of inserting steel, plastic or glass beads under the penile skin. A small lump near the hair bearing skin of the proximal penis may represent a healed furuncle.
Summary
While lumps on the penis are frequently a source of great anxiety for the patient, if it is unclear whether the lesion is a normal variant or not, there is usually no harm in asking the patient to return for review. In some cases, it is necessary to refer to a more experienced colleague, a sexual health service or dermatologist to assist with diagnosis. A second opinion is often more efficient and preferable to the patient than a biopsy or a trial of treatment.
Key points
- Genital warts are becoming less common.
- Normal variants can cause significant anxiety, but have no sequelae, do not represent an STI, cannot be passed to others, and do not require treatment.
- If the diagnosis is unclear, it may be useful to review the patient in a few weeks. A normal variant does not usually progress, and for most conditions that require treatment, there is no harm to the patient if treatment is delayed for a few weeks.
Competing interests: Tim Read has received payment from GlaxoSmithKline and Merck Sharp & Dohme for work as Site Principal Investigator for an antiretroviral trial (GSK) and HPV vaccine study (MSD).
Provenance and peer review: Commissioned; externally peer reviewed.
Acknowledgements
The authors gratefully acknowledge Ian Denham for his review of the manuscript and for contributing images. We also acknowledge the assistance of Afrizal Afrizal for the technical support of images.