This lack of information led us to design a sub-study of the BEACH program, surveying 2654 patients from 91 general practitioners in late 2012, to determine the prevalence of NP among patients seen in Australian general practice, its most commonly described symptoms, the time between the onset of symptoms and consulting a GP, reasons prompting the patient to seek help and reasons for the patient delaying this. The prevalence of NP (or its symptoms) was 8.5% (n=226), comprising 6.6% formally diagnosed NP and 1.9% symptoms of (undiagnosed) NP. There was no difference in the prevalence between the sexes.
Patients aged 45–64 years had the highest rate of NP (15.8%, Figure 1), accounting for 109 (48.7%) of the 224 respondents with NP. There were 439 responses by 225 patients describing the nature of the NP. The three most common were ‘shooting pain’ (52.9% of patients), ‘burning’ (47.6%) and ‘pins and needles’ (44.0%). Time between NP symptom onset and first seeking GP care was reported by 205 respondents. The majority of patients (84.9%) sought help within 6 months of symptom onset. The most frequent reasons to seek GP help were intolerable pain or interference with normal routine, sleep or physical activity (Table 1). The most common single reason (given by 12 of 30 patients) for waiting more than 6 months was that the patient ‘hoped pain would self-resolve’. These results indicate a prevalence of NP similar to that of the European population surveys.
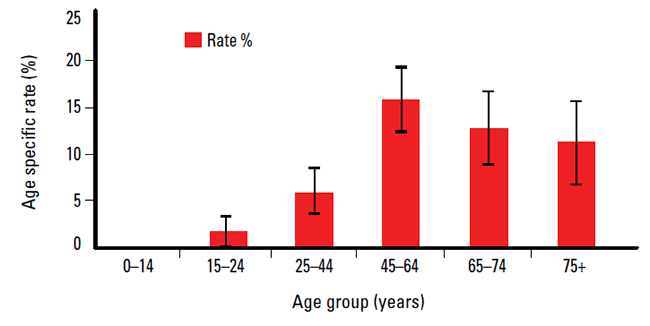
Figure 1. Age-specific rates of neuropathic pain (with 95% confidence limits)
Table 1. What finally prompted patients to seek help from their GP (multiple responses allowed)
| Reason | Responses | Proportion of 204 patients (%) |
|---|
| Unable to tolerate pain |
121 |
59 |
| Pain was interfering with: |
|
|
|
|
114 |
56 |
|
|
104 |
51 |
|
|
104 |
51 |
|
|
32 |
16 |
|
|
30 |
15 |
| Total |
505 responses |
|
Competing interests: None.
Provenance and peer review: Commissioned; not peer reviewed.
Acknowledgements
The authors thank the GP participants in the BEACH program, and all members of the BEACH team. Funding contributors to BEACH from April 2012 to March 2013: Australian Government Department of Health and Ageing; AstraZeneca Pty Ltd (Australia); CSL Biotherapies Pty Ltd; Merck, Sharp and Dohme (Australia) Pty Ltd; National Prescribing Service; Novartis Pharmaceuticals Australia Pty Ltd; Pfizer Australia Pty Ltd. This SAND sub-study was undertaken in collaboration with Pfizer Australia Pty Ltd. BEACH and all SAND sub-studies are approved by the Human Research Ethics Committee of the University of Sydney.