In this article we look at what makes a good appointment system for patients, staff and clinicians and describe the five appointment strategies we have seen through our work with the APCC program. Because it is a basic introduction to these systems, we have called this article ‘Appointments 101’.
Maximising the effectiveness of appointment systems in general practice has the potential to connect patients and clinicians for timely care and create a sustainable working environment. Your appointment system sets the rules of engagement between you and your patients. It reflects your philosophy of general practice. Your system impacts on quality of care, safety, staff happiness and retention, profitability, clinician satisfaction and patient experience.
What makes a good appointment system?
For patients,2–7 a good appointment system will:
- give an appointment at the right time (Urgently? Before work? At the weekend?)
- allow booking ahead to suit work or transport requirements
- run on time so there is little waiting
- give access to the preferred clinician (continuity gives better outcomes)
- allow quick access with no wait when desired
- provide short or long appointments as needed.
For receptionists,8 a good appointment system will:
- enable them to say yes almost always, rather than no
- be simple (no complicated rules or multiple types of appointments)
- have no delay which reduces the need for triage
- run on time and so reduce tension in the reception area
- reduce stress for clinicians so the workplace is a happier place.
For clinicians,8,9 a good appointment system will:
- provide predictability – confidence that their time is well used
- provide continuity – it is more effective and quicker to see patients you know
- run on time and so reduce stress
- be flexible to respond to patient emergencies, clinician personal crises, family issues or educational opportunities
- facilitate booked structured review
- finish the day on time
- permit breaks for lunch or other as required
- match current Medicare financing arrangements so income is sustainable.
Monitoring your appointment system
Is your appointment system running efficiently? In order to assess this you need measures that are easy to collect, easy to understand and validly reflect improvements to indicate whether changes you make are working. You could consider using the following measures.
Third available appointment
This is the most internationally recognised and reliable measure of appointment delay.10 To calculate it, count up the number of days from today until the next available routine appointment (ie. don’t use reserved emergency appointments), then look for the next and then the next. In practices with more than one doctor you can average the third available appointment to give measure of delay for the entire practice. As you reduce delay this measure will reduce.
Unmet demand
To monitor unmet demand, practices make a weekly tally of how many patients could not be given an appointment. In the APCC program, some practices reviewed their systems after finding unmet demand rates of around 200 per week.
Patient satisfaction
Participating APCC practices use a simple survey of a random sample of 50 patients 1 week per month. Patients indicate on a scale from 1 to 5 their agreement with the statement ‘I was able to make an appointment on the day I wanted with the clinician I wanted to see.’
Waiting times
Some billing software programs can record time of arrival and time of opening of the patient record, giving a measure of waiting time. Improvements to running on time should result in a reduction of this measure.
Doorknob to doorknob time
The ‘value’ for a patient is face-to-face time with their doctor or nurse. Waiting is waste. Patients wait to see the receptionist, the doctor, the nurse and then the receptionist again. Quantify this waste by tracking a patient’s journey from the time they walk in until the time they walk out.
Appointment systems seen in the APCC program
Open access
In an open access system there are no appointments. Patients simply turn up and wait to be seen. Once a practice is well established, people learn when they are likely to get in quickly.
Some variations designed to manage the inconveniences and negatives include:
- a queuing system allowing patients to do other things and come back when they estimate they will get in
- ringing or paging the patient when their turn is up
- strategies to provide some continuity with preferred doctors.
Advantages
You start the day with full capacity (all consultation time) available. Patients know they will see the doctor: they just need to be able to wait. Doctors do ‘shifts’ and know they can finish on time.
Consultation length is flexible and theoretically can be matched to need. More doctors can be rostered on at identified high demand times.
The ‘central queue’ of open access increases efficiency and removes bottlenecks. The practice is not booked out weeks in advance with chronic problems. There are no complicated rules for appointments and less triaging. Open access particularly suits some populations and local circumstances. An example is shown in Table 1.
Table 1. Example of the open access appointment system
In 2010, general practices in Albany were approached by the GP Network through the Close the Gap initiative to start clinics aimed at increasing service to Aboriginal and Torres Strait Islander communities.
Our practice, Pioneer Health, started with four sessions focused on working with this community: two based in the local Aboriginal Medical Service and two in our practice. We made a conscious decision to use open access rather than the appointment system we run in our mainstream practice to minimise barriers. In retrospect we realise we tried to make our clinics more ‘permeable’ to Indigenous people, as described in an article by Dixon-Woods,15 which analysed the access of vulnerable groups to healthcare. Using Aboriginal outreach workers also helped with this. We have seen our registered Aboriginal and Torres Strait Islander patients increase from 126 to 583 in 14 months. Open access is just part of a package of strategies that have made the clinics a success. Interestingly, many patients now seem comfortable moving over to using our more traditional appointment system. |
| Dr Andrew P Knight, Pioneer Health Albany, Western Australia |
Disadvantages
People who work and people who depend on others for transport or translation cannot timetable their appointments and tend to be the losers in this system.2
In addition, the clinic loses the ability to influence when people come in, and this makes it harder to shape demand. Central queuing can reduce continuity in large practices that use an open access system. It is also difficult to timetable structured care in the absence of appointments.
Patients of practices that use an open access system can face delays of hours if it is busy or a doctor is absent. If the waiting room is full, clinicians may feel pressure to be quick or not deal with all problems. Long delays may provoke patient anger.
Book on the day
In ‘book on the day’ models, there is a flood of phone calls each morning and the appointments fill up. When the day is full, people are told to ring tomorrow for an appointment.
Advantages
Disabled, elderly and working people get more opportunity to plan compared with open access systems. Doctors have more flexibility for contingencies such as delivering babies (or playing golf) as the day can be rearranged at short notice without inconveniencing booked patients. People with acute problems can get in on the day.
Disadvantages
This system can lead to nonsensical conversations such as, ‘Yes I know it is 5.30 in the afternoon but I can’t give you an appointment for tomorrow morning. You will have to ring back at 8 am.’ Also, structured chronic disease care is more difficult. Telephone traffic peaks in the morning and may overwhelm system and staff capacity.
Supersaturate
Appointments are booked according to the patient’s request. Acute appointments are ‘squeezed in’ by double booking or in lunch times, or at the end of the day. This common system has usually grown over years as a response to evolving challenges. Each practice considers their system original, but approaches are in fact remarkably similar. Emergency appointments are reserved, which are shaded a different colour. When these fill, ‘follow up’ appointments are created in a different colour. Later ‘catch up’ appointments, and possibly ‘do not book under any circumstances’ appointments, in yet other colours are reserved. The appointment book becomes as colourful as a Christmas tree; working with so many different types of appointments can become incredibly complex with local unwritten rules and quirks for each clinician.
Advantages
It is an honest attempt to make the system work for everyone and can be made to work some of the time. It reflects an appropriate philosophy that seeks to accommodate people with chronic predictable care needs while recognising the practice must respond to acute needs.
Disadvantages
Complexity results in inefficiency and gaming (Do reception staff relatives often take emergency appointments?). Doctors try to see too many patients in the time allocated, causing stress and delay with tense, full waiting rooms. Reception staff members explain, triage, seek non-existent appointments and liaise with clinicians. Increased traffic in emails, messages or telephone calls to clinicians are needed to cope with lack of access and there is spurious demand as patients make appointments ‘just in case’.
Appointment length blows out, as patients want to do a lot of tasks in each precious appointment with the doctor. There is a pressure-cooker feel in the practice reducing capacity for reflection on systems or to complete structured chronic disease care. Receptionists are often very unhappy in their work and there may be high turnover with loss of important corporate systems knowledge.
Carve out
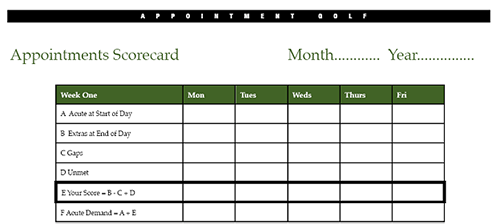
Figure 1. Appointment golf scorecard
Practices deliberately ‘carve out’ a number of their appointments each day for acute care. A rule of thumb is that if you start the day with about one-third of your appointments available you will be able to deal with acute care demand. You may measure the daily acute demand of the practice (see our earlier article ‘Appointment systems: getting it right’, AFP January/February 2011).1 It is remarkably predictable and you can confidently carve out the right amount. Playing ‘appointment golf’ will give you further evidence to adjust your carve out. An example is shown in Table 2. Some practices combine this with a ‘jeopardy doctor’ system. An example is shown in Table 3.
Table 2. How to play ‘appointment golf’
Appointment golf helps you carve out the right number of appointments each day without the labour of measuring acute demand.
The scorecard we use can be found at http://practiceimprovement.com.au/wp-content/uploads/2009/10/appointment_golf.pdf (see Figure 1 for an example) |
Before the day (before switching on the telephones) count:
- The number of free appointments (= A for acutes available)
- After the day count
- The number of extra fit-ins (= B extras)
- The number of gaps where no one was booked (= C fit-ins – an unusual event)
- The number turned away if any (= D unmet demand)
|
Your score for the day is:
Number of extras (B) – number of gaps (C) + number turned away (D)
(The lower the score, the better!)
An eagle is 0; a birdie is between 1 and 3; par is 4–6; a bogie is 7–9; a double bogie starts from 10
A tip to improve your score
The number of appointments you need to carve out to get zero on the same day of the week in 1 weeks time will be:
Number of free appointments at the start of the day (A) + your score for the day (E):
this is the demand for acute appointments
(We have found that this number is amazingly consistent from Monday to Monday, Tuesday to Tuesday, etc) |
| Dr Tony Lembke, Alstonville Clinic, Alstonville, New South Wales |
Advantages
With this system you will be able to deal with acute care on the day. It allows planning ahead for transport, work commitments and structured chronic disease care.
Disadvantages
The acute care ‘carve out’ increases the waiting time for other appointments. This can cause pressure to use carved out appointments for follow-ups. There may sometimes be mismatches, resulting in carved out appointments unfilled.
Table 3. Example of the jeopardy doctor appointment system
We started out many years ago with a ‘designated doctor’ or jeopardy doctor who took all emergencies on top of their own bookings. As this got busier, we made that doctor unbooked and broke it into two daily sessions in the treatment room with a nurse for dressings and immunisations. The treatment room now has 2.5 nurses, 9 hours daily and a GP am, pm and evening. When you are not there, you are protected from emergencies.
We use it to introduce new general practice registrars and international medical graduates to the practice. It’s great for students – currently medical, nursing and pharmacy. Patients love the flexibility and being seen quickly for urgent things. Nurses like the significant freedom and autonomy they have in this space. General practitioners enjoy the change from ‘routine’ general practice. It’s a place where GPs and nurses learn to work well together and it has been used to teach extra practical skills. |
| Dr Richard Bills, Brooke Street Medical Centre, Woodend, Victoria |
Advanced access
This is perhaps the most internationally recognised best practice in primary care appointment systems.11–13 When demand equals capacity and there is no backlog you have enough appointments to accommodate all demand now, and as it arises. There are five steps to advanced access:
- Measure demand and capacity
- Shape the measured demand
- Match the practice capacity to the reshaped demand
- Work down the backlog
- Plan for contingencies.
The aims are:
- start the day with enough appointments to meet demand on the day
- no restriction on making future appointments
- prioritise continuity (improving outcomes and reducing demand).
This approach was developed in the United States in large managed care organisations. It can be very effective in improving working conditions and patient experience.11–13
Advantages
When demand and capacity are matched and third available appointment is less than one you can be confident of meeting the demand on any given day. You start the day with most of your appointments free and they fill up progressively as patients call. Patients are confident of timely access to their preferred clinician. There is flexibility for clinicians and patients. Continuity is maximised. Acute care is dealt with without delay and chronic care is structured without delay.
Disadvantages
Advanced access requires commitment and time to implement. Some of the ideas are counterintuitive and require a lot of education for staff and clinicians to be willing to commit to change. It has been poorly implemented around the world, raising doubts about its practicality.14 It requires major changes in clinician, staff and patient behaviour. Achieving and maintaining advanced access requires a level of practice leadership, administrative support and clinician cooperation rarely available to general practices in Australia.
Conclusion
Your appointment system is an important factor in the quality and safety of the care you provide. It may be useful to consider the following questions:
- Why have you selected the system you are running?
- Is this system meeting the needs of your practice and your patients?
- Do you need to change what you are doing in order to improve your care?
- Do you actively manage your appointment book to improve your access?
Einstein declared that insanity is ‘doing the same thing over and over again and expecting different results’. No matter what your appointment system, there are many changes you can make to improve its performance.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.
Acknowledgement
The Australian Primary Care Collaboratives program is delivered by the Improvement Foundation (Australia) and supported by funding from the Australian Government Department of Health and Ageing.