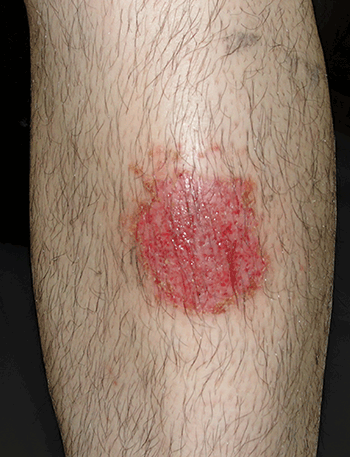
Figure 1. Erythematous plaque with cribriform erosions on its surface
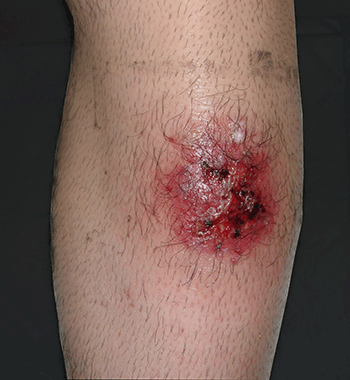
Figure 2. Poor response to topical antifungal treatment
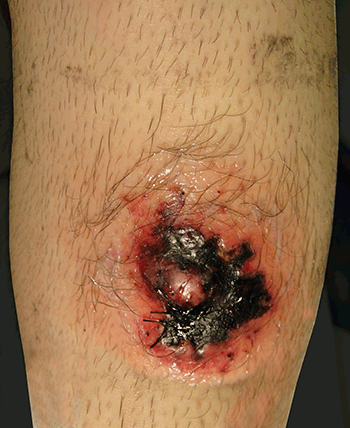
Figure 3. The lesion appears necrotic 3 days postbiopsy
Question 1
What is the most likely diagnosis?
Question 2
What differential diagnoses should be considered?
Question 3
Why did the necrotic ulceration appear after the biopsy?
Question 4
What are the treatment options for pyoderma gangrenosum?
Answer 1
Pyoderma gangrenosum (PG) is a painful, ulcerative, necrotic skin lesion with distinctive clinical features. The aetiology is uncertain and the pathophysiology is poorly understood, but dysfunction of the immune system is believed to play a role. Approximately one-half of cases are associated with an underlying systemic disease (Table 1), most commonly inflammatory bowel disease, arthritis, or a lymphoproliferative disorder.1 The diagnosis is made by excluding differential diagnoses (see Question 2).2 The lesions may be single or multiple; they are usually chronic and/or recurrent. They occur most commonly on the legs, especially the pretibial area, but can develop on any area of the body (eg. the abdominal wall adjacent to a stoma following a colectomy).
Table 1. Systemic diseases associated with pyoderma gangrenosum
| Inflammatory bowel disease: ulcerative colitis, Crohn disease |
| Arthritis: classic rheumatoid arthritis (RA), seronegative RA-like syndrome, non-destructive monoarticular arthritis of large joints |
| Monoclonal gammopathy: 75% IgA, 25% IgG, rarely myeloma |
| Immunologic dysfunction: leukaemia, transplants, HIV infection, congenital and acquired hypogammaglobulinaemia |
| Haematologic and malignant: leukaemia, IgA myeloma, myelofibrosis, polycythaemia rubra vera, lymphoma, solid tumours of colon, adrenal gland, bladder, breast, lung, ovary |
| Others: acne conglobate, Behçet disease, chronic active hepatitis, gastric ulceration, Hashimoto thyroiditis, Hidradenitis suppurativa, hyperthyroidism, primary billary cirrhosis, sarcoidosis, systemic lupus erythematosis, Wegener granulomatosis |
Answer 2
The differential diagnoses of PG include deep mycoses, bacterial infections (including mycobacteria), chronic ulcerative herpes simplex virus, vasculitis and insect bite reaction among others (Table 2). Histopathologic findings may help distinguish between these disorders, but there are no investigation results that are pathognomonic for PG.
Table 2. Differential diagnosis of pyoderma gangrenosum
| Infectious | Non-infectious |
|---|
| Bacterial infections (including mycobacteria)2 |
Halogenodermas |
| Syphilis |
Drugs |
| Deep fungal infections |
Antiphospholipid syndrome |
| Necrotising fasciitis |
Insect bite: spider |
| Amoebiasis |
Facticial |
| Viral infections (herpes simplex virus, varicella-zoster virus in immunosuppressed patients) |
Neoplasms:
- lymphoma
- systemic vasculitis
|
| Cutaneous leishmaniasis |
Warfarin skin necrosis |
Answer 3
This event is explained by the phenomenon of pathergy that was first described by Blobner in 1937.3 Pathergy refers to the formation of a papule, sterile pustule or ulceration 24–48 hours after a needleprick to the skin. It has long been used in the diagnosis of Behçet disease, but the phenomenon is also associated with PG, eosinophilic pustular folliculitis, cutaneous ulcerative lichen planus, bowel-associated dermatosis-arthritis syndrome, rheumatoid arthritis, leukocytoclastic vasculitis, non-Hodgkin lymphoma and chronic myeloid leukaemia treated with interferon alfa.4 Many patients with PG report previous trauma to the sites of their lesions, however, pathergy, in the absence of other clinical criteria, is not sufficient to make a diagnosis of PG.
Answer 4
Treatments for PG include local and systemic approaches (Figure 4). Local or topical therapies include colloidal membrane occlusive dressings, whirlpool baths, topical antiseptics (benzoyl peroxide, silver sulfadiazine), topical or intralesional glucocorticoids5 and topical tacrolimus ointment. Where systemic treatments are required, systemic glucocorticoids are generally first line (eg. prednisolone 0.5–2.0 mg/kg/day).6
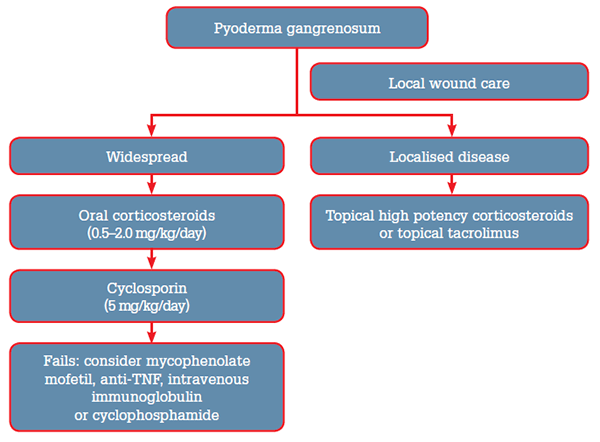
Figure 4. Treatment algorithm for pyoderma gangrenosum
For lesions that are refractory to oral glucocorticoids alone, additional treatment options include azathioprine (50–150 mg/day), mycophenolate mofetil (1–2 g twice daily),7,8 cyclophosphamide (2–3 mg/kg/day), cyclosporin (5 mg/kg/day, with target trough serum levels of 150–350 ng/mL).9,10
High dose intravenous immunoglobulin has been reported to be effective in some cases.11 In addition, biologic agents have shown efficacy in the treatment of PG. Infliximab therapy was superior to placebo in a randomised trial of 30 patients.12 Clinical improvement has also been reported in several patients treated with adalimumab and in one patient who received ustekinumab.13,14
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.