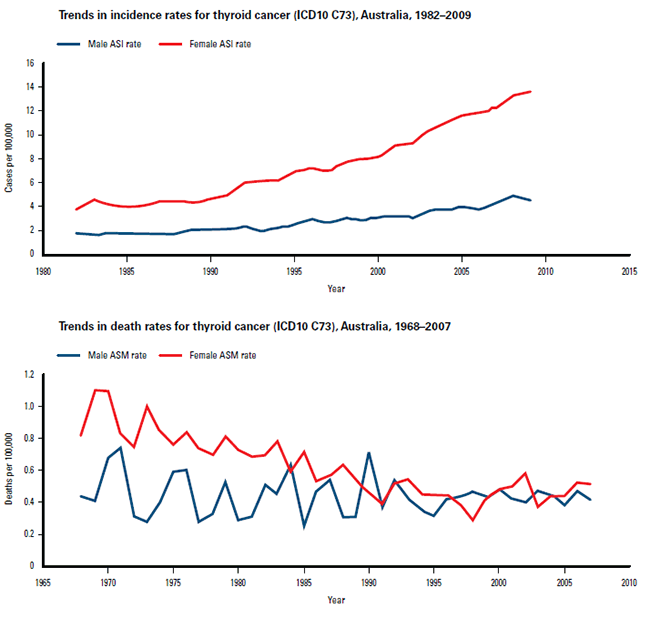
Figure 1. Incidence and mortality from thyroid cancer in Australia
Source: Australian Institute of Health and Welfare (AIHW) 2012. ACIM (Australian Cancer Incidence and Mortality) Books. AIHW: Canberra.
Ways in which overdiagnosis is occurring
Our increased detection and labelling of people as having a disease has occurred in several different ways: changes of definition or threshold, labelling of risk factors as diseases, early detection from both deliberate screening programs and incidental detection (‘incidentalomas’), and medicalisation of life, particularly in psychiatry. These changes have mostly led to increases in apparent disease, though with the occasional reduction (for example, homosexuality was removed as a diagnosis from the 1973 edition of the Diagnostic and Statistical Manual of Mental Disorders).
Lowering thresholds for treatment
The treatment of elevated blood pressure is one factor that has led to the extraordinary decline in cardiovascular deaths in the past four decades.4 The definition of hypertension in the first trial was a diastolic blood pressure of 115–1295 and only a small percentage of the population was eligible. Since then, increasingly lower thresholds for treatment have been introduced.6 But how low should the threshold go? A recent Cochrane review concluded that the treatment of mild hypertension (systolic blood pressure 140–159 mmHg and/or diastolic blood pressure 90–99 mmHg) and no history of cardiovascular disease had no effect on the number of heart attacks, strokes or death, but 9% of patients stopped taking the medication because of adverse effects.7 The trend for lower and lower thresholds for the definitions of conditions, and their subsequent treatment, is consistent across all fields of medicine.8 Even minor changes in the threshold can result in very large changes to the number of patients labelled with a disease. Lowering of the fasting glucose threshold for the diagnosis of diabetes mellitus in 1997 from 7.7 to 7.0 mmol/L almost doubled the number of people diagnosed with that disorder (Figure 2).9 Lowering the threshold of disease exposes more patients to treatments with less possibility of clinical benefit and with an increased risk of adverse events.
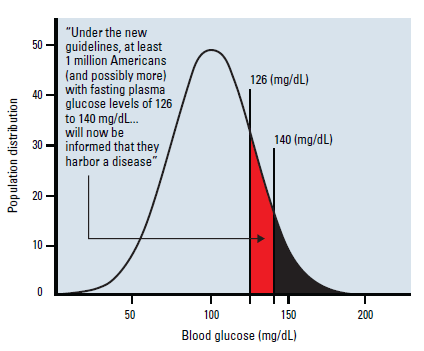
Figure 2. The effect of the change in the definition of type 2 diabetes mellitus in 1997 on disease prevalence
Labelling of risk factors as diseases
Elevated blood pressure illustrates another trend in modern medicine: patients with no detectable symptoms but who are at an increased risk of a symptomatic disease are given a diagnostic label, in this case ‘hypertension’. This labelling effect is profound. These patients now believe that they are sick, believe that they are suffering from a disease and have increased anxiety about their health.10 Other examples of risk factors that have been labelled as diseases are chronic kidney disease, non-alcoholic fatty liver disease, osteoporosis, obesity, elevated lipid levels and most cases of type 2 diabetes. It is ironic that in trying to prevent significant disease with true consequences for the patient, we are labelling more and more of the population as ‘diseased’.
Screening for disease
The success of detecting and treating elevated blood pressure before any symptomatic disease led to another modern trend: the push for more screening. The idea of detecting a disease early, before it can cause irreversible damage, is intuitively appealing and is frequently championed by patient advocates, politicians and celebrities. Despite this, only a few screening programs are clearly beneficial, primarily because screening mostly detects the mildest or most indolent forms of disease, where the benefits are more likely to be outweighed by side effects. Picking which diseases are worth screening for is not easy. Trials of screening for hypertension, atrial fibrillation and bowel cancer have shown net benefits, but to date, trials of screening for chronic kidney disease,11 diabetes12 and annual health check-ups13 have not. Opportunistic case finding (‘while you’re here let’s check your ….’) is sometimes advocated in place of screening when screening has been shown to be ineffective, but has similar problems. Screening for cancer would seem intuitively the most likely to be beneficial, detecting cancers before they have a chance to metastasise. However, trials of screening and autopsy studies have shown that most of us have evidence of cancer if we search hard enough for it and that current screening methods are unable to differentiate between indolent cancers and more aggressive forms.14,15
A working group convened by the National Cancer Institute in the United States recently called for greater recognition of this problem and for increased discussion of the problem with the public.16 Screening, or opportunistic case finding, is intrusive, uses up considerable resources and should only be instituted when benefits clearly outweigh harms.
Increased sensitivity of testing
There are certain diagnoses that doctors learn must not be missed: myocardial infarction, pulmonary embolism and cancer. To reduce the number of missed diagnoses, increasingly sensitive tests have been developed. Again, these ‘better’ tests seem to be better at picking up the mildest cases of the disease. In the eight years after the introduction of computerised tomography (CT) pulmonary angiography in the United States, the diagnosis of pulmonary embolism increased by 80%, with almost no change in the age-adjusted mortality rate and a reduction in the case-fatality rate by approximately one-third.17 Many of the patients who are diagnosed with sub-segmental pulmonary emboli using the more sensitive tests are likely to have lesions that would never have been clinically significant, and are therefore being overdiagnosed and overtreated.
Incidentalomas
The impact of incidental findings from the increased availability of imaging and pathology tests has been substantial. The rapid increase in the incidence of thyroid cancer has occurred in tandem with increased access to health care and has led to recent calls for less investigation and treatment, particularly in lesions less than a centimetre.18 Many other modern tests have similar difficulties. Roughly a quarter of CT pulmonary angiograms detect an unexpected finding, such as a pulmonary nodule, a thyroid nodule or an adenopathy. The patient then has to undergo more scans or more invasive testing to try to clarify the clinical significance of the finding.19 Increased access to MRI in the community is likely to lead to similar problems.
The increased medicalisation of life
Patients have always come to the medical profession with their pains and difficulties. In the twenty-first century, however, we are increasingly likely to label people with a disease, whether or not this is of benefit to the patient. This is occurring in all fields of medicine, but is particularly apparent in psychiatry. Unhappiness and grief become depression; shyness becomes anxiety disorder; inattention and an inability to sit still become attention deficit hyperactivity disorder. This is not to deny that some people with these symptoms will be suffering greatly, or that some of the people suffering from such symptoms are undiagnosed and would benefit from treatment. But for an increasing proportion of people, management consists of a disease label and a prescription and/or a referral, even when there is little evidence for long-term benefits. The harm from labelling and drug side effects can be substantial.20
The consequences of overdiagnosis
The consequences of overdiagnosis are not just financial. Overdiagnosis is also causing harm to patients. Patients are increasingly anxious about their health and a substantial proportion of the population is receiving medical treatment that is more likely to cause harm than benefit. One general practitioner in the UK has summed up the problem as ‘too much testing of well people and not enough care for the sick – worsens health inequalities and drains professionalism, harming both those who need treatment and those who don’t.21
The way forward
Overdiagnosis has only recently been recognised as occurring systematically across all fields of medicine, and its reach and consequences are still being studied.22 General practitioners often carry the burden of care for patients who have been overdiagnosed, while single-disease experts frequently advocate for more screening, early detection programs, lowering of disease thresholds and aggressive treatment of early disease. Patients in a general practice setting are less likely to benefit and more likely to be harmed than patients in clinical trials or patients in tertiary hospitals because of milder and earlier disease. For many conditions in general practice, it is advisable to take a wait-and-see approach, with further investigation, referral and treatment used more cautiously than advocated by disease specialists. It is likely that systematic approaches will be needed to roll back current disease labelling and consequent harms, but in the meantime we hope that general practitioners will be more aware of this issue and the potential harm it is having on their patients.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.