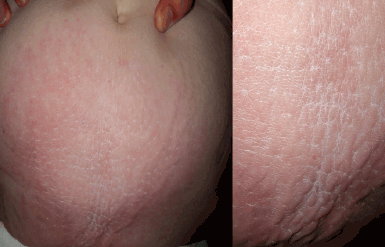
Figure 1. Area of skin on the lower abdomen with ill-defined, indurated, whitish papules
Question 1
What is the diagnosis?
Question 2
What is the differential diagnosis?
Question 3
What tests are indicated?
Question 4
What empirical treatment can be used for this condition?
Question 5
Which types of diabetes are likely to be associated with this condition?
Answer 1
Scleredema is a dermatosis caused by the accumulation of mucin in the dermis. Note that it is different from scleroderma. Clinically it consists of an area of skin with a ‘cobblestone’ appearance. It has been associated with diabetes mellitus, acute infections and monoclonal gammopathy.1,2 Scleredema was originally described by Buschke in 1902, so it is also known as scleredema de Buschke. It is divided into three groups: type 1 or associated with bacterial or viral infections; type 2 or paraproteinemia-associated; and type 3 or associated with diabetes mellitus (Table 1).
Table 1. Types of scleredema
| Type 1 | Type 2 | Type 3 |
|---|
| Age |
More common in children |
>20 years |
>40 years |
| Associated diseases |
- Streptococcus infection
- Diphtheria Typhoid fever
- CMV
- Measles
- Mumps
- HIV
|
- Paraproteinemia, multiple myeloma, blood dyscrasias
|
|
| Gender |
>Women |
>Women |
>Men |
| Systemic manifestations |
Heart, lung, liver, spleen, parotid glands, pharynx, oesophagus, pleura and peritoneum |
Occasional |
Rare complications are associated with diabetes mellitus |
Answer 2
The differential diagnosis of scleredema de Buchske includes scleroderma and scleromyxedema. In scleroderma there are several skin signs not present in scleredema, such as Raynaud’s phenomenon, telangiectasias, calcifications and characteristic facies. An anatomopathological study showed sclerosis of the dermis and loss of skin appendages.3 Scleromyxedema is an acute, rapidly evolving dermatosis. It consists of firm papules, deep wrinkles on the forehead and possible involvement of the hands and forearms. Microscopic examination reveals a diffuse deposition of mucin in the superficial and deep dermis, fibrosis, and proliferation of fibroblasts arranged regularly.
Answer 3
A punch biopsy confirmed histologically the presence of scleredema, which is characterised by increased thickness of the dermis, visualised by haematoxylin–eosin staining (Figure 2), and mucin deposits evidenced by alcian blue staining in the depth.
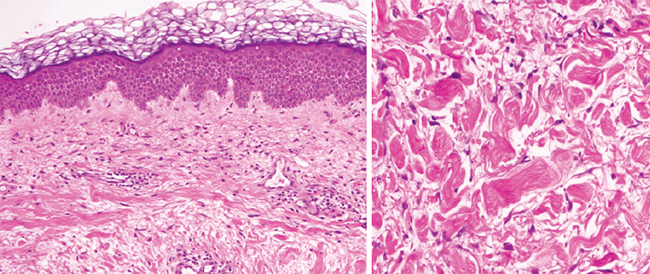
Figure 2. Haematoxylin–eosin staining showing increased thickness of the dermis (left panel, 5X; right panel 10X)
A complete evaluation of the patient, including biochemistry and blood count, proteins, autoimmunity, glycaemia, glycosylated haemoglobin, and renal and hepatic function, is required to classify the scleredema. In our patient the tests revealed only elevated blood glucose in the diabetic range, as was already known.
Answer 4
There is no specific treatment for scleredema, and in types 2 and 3 the course of the disease is usually chronic. The patient in this case was treated locally with an emollient cream of 3% polidocanol and 5% urea, which resulted in significant improvement, although without a complete resolution.
Answer 5
If scleredema is associated with diabetes mellitus, it is typically non-insulin-dependent and poorly controlled, and patients often develop diabetic complications a few years before or after the scleredema.
In conclusion, in a patient aged over 40 years with a diagnosis of scleredema, the physician should screen for diabetes, or improve the treatment of the diabetes for better control and prevention of diabetic complications.4,5
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.