Methods
A web-based survey was sent to the Review and Survey Group of the Breast Cancer Network of Australia, a national consumer group (n = 760), in May 2010. The questionnaire was informed and improved through the combined use of expert opinion, a focus group (n = 7) and single case interviews (n = 6). It was tested and retested to ensure internal consistency, content, face validity and acceptability before sending. Respondents completed sections describing their cancer treatment, presence and presentation of lymphoedema, treatments used for lymphoedema management and treatment accessibility. Validated questions for classifying the magnitude of lymphoedema were included7 to improve accuracy of reporting. The main focus of the questionnaire was to identify treatments that survivors of breast cancer used to alleviate lymphoedema and the extent to which they perceived the treatments effective.8 Additional questions on availability of treatment were included and the responses are reported here.
To determine whether the sample was representative of the population, data were compared to those of the general population from the most recent Australian Bureau of Statistics (ABS) reports. Comparisons were made on demographic factors, including education, financial status and ethnicity (attempts were made to cohort-match data by sex for education and finances). Postcodes were used to categorise respondents as resident of major cities, inner regional, outer regional and remote Australia, thus allowing us to compare state-by-state, and rural and metropolitan access.
Results
Population characteristics
Responses were received from 444 (58%) women (no male respondents); 35% of this group identified themselves as having lymphoedema (n = 154) and a further 9% were unsure (n = 40). Comparison of data from our group (n = 444) against data from the ABS revealed that our group was representative of the population by regional characteristics (rural/urban divide and state representation). However, the survey group differed from the general population by education, ethnicity and private health cover. Our group was more educated: 40% had tertiary qualifications, whereas the national average for women is 25.9%.9 The median annual household income was $60,000–69,000 and 64% were in full-time or part-time paid employment, which is similar to the national averages for women. Private health insurance was held by 333 (75%) of respondents, of whom 291 had private health cover with extras. The national average for those holding private insurance is 45%.10 In addition, country of birth was not representative of the general population. For example, 1% of respondents were born in Asia or the Middle East, whereas these groups comprise 10% of the general population. Ninety-five percent of the group surveyed spoke English as their sole language at home, compared with 81% of the population from the most recent census data.11 Population biases are likely to be linked to use of an electronic survey with a web-based group.
Lymphoedema treatment subgroup
One hundred and fifty-four women reported they had lymphoedema and 140 were treated for lymphoedema in the five years before survey deployment. Thirty-three percent (n = 46) of this sub group (n = 140) reported encountering barriers to treatment. Accessing a therapist (n = 34), cost (n = 27), distance to travel (n = 21), and not knowing how to get help (n = 20) were the most commonly reported barriers (Figure 1). Of those unable to access a therapist, 16 lived in rural areas and 16 lived in major cities. Postcode data were missing for two respondents. State distribution is shown in Figure 2. Quality-of-life indicators were similar for those who experienced no barriers in accessing treatment, compared to those who did experience barriers. The median and interquartile range (IQR) EuroQOL scores were 80 for those who experienced barriers (70–88; n = 44) and also for those who experienced no barriers (70–90; n = 89). The median EuroQOL score for those without lymphoedema (n = 248) was 85 (78.5–90).
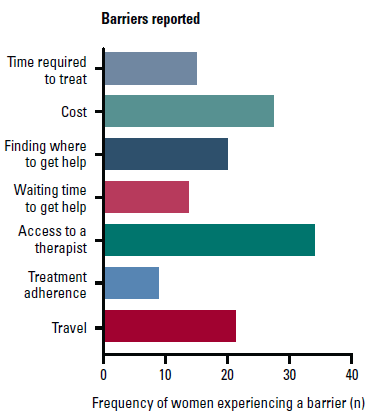
Figure 1. Barriers to treatment for
lymphoedema
The public system was accessed by 58% of respondents and the private system by 60%. Twenty-three percent of respondents used both public and private services for their lymphoedema. Most of the women received their treatment from physiotherapists (n = 88). Other sources of treatment were massage therapists (n = 52), occupational therapists (n = 27), nurses (n = 19) and doctors (n = 14). Women reported they were satisfied with both public and private services but were highly satisfied with private treatment for effectiveness of treatment received and waiting times. Satisfaction with costs incurred was low for both private and public services.
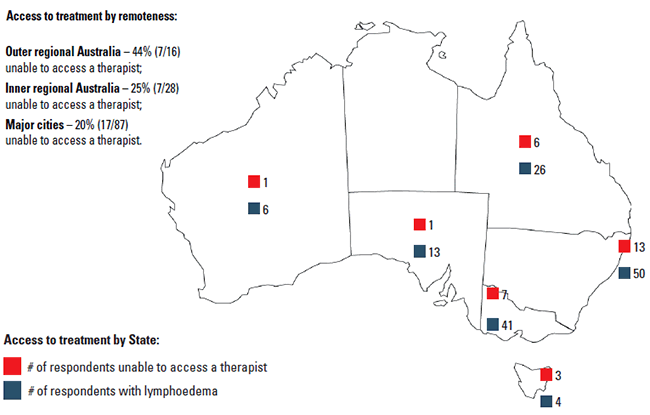
Figure 2. Reported access to treatment based on geographical factors
Discussion
This study suggests that one-third of those with breast cancer-related lymphoedema in Australia report they do not receive adequate treatment for their lymphoedema. The possible consequence of delaying treatment or not receiving treatment is progressive tissue change causing lymphoedema to become a chronic, lifelong problem.12 Treatment aims not only to reduce limb size, but also to improve comfort, as lymphoedema can cause feelings of tightness, heaviness, restricted movement and even pain. Lymphoedema can have significant effects on function and self-image.13 It also increases the risk of localised infection, particularly cellulitis. The infections can become recurrent and require treatment with high doses of intravenous antibiotics, which often involves lengthy hospital stays.14 The breadth of the problem of breast cancer-related lymphoedema is not known but a recent meta-analysis15 showed that the incidence of lymphoedema in women treated for breast cancer was 21%. We therefore estimate that of the 14,600 new cases of breast cancer diagnosed this year,16 more than 3000 women will develop breast cancer-related lymphoedema at some time in the future.
The two main barriers reported by our respondents were access to a clinician and ongoing costs associated with treatments. The 33% of women experiencing difficulty in accessing treatment for lymphoedema far exceeded the 2.6% of patients who reported difficulty accessing health services in 2011–2012.17 It remains unclear whether the problem with access is an overall lack of trained clinicians able to treat this chronic condition or whether a lack of public sector availability is perceived as an inability to access a therapist. Access to health care in rural Australia is a well-documented problem;18–20 however, the proportions of women reporting they were unable to access a clinician to treat their lymphoedema were similar in metropolitan and regional areas. For example, in Sydney, Australia’s largest metropolitan city, only eight of the 35 public hospitals in the greater Sydney metropolitan area offer lymphoedema treatment. Of these services the referral criteria either allows for the treatment of all types of lymphoedema – primary and secondary – or is limited to those with cancer-related lymphoedema. In addition, availability is limited to those living in the local district area or under management at the hospital where the service is based. As a result, residents of areas such as the eastern suburbs in Sydney have no public service available.
On the basis of representation from the national lymphoedema therapist register, the availability of lymphoedema services seems greater in the private sector. The Australian Lymphology Association (ALA) has a web-based National Lymphoedema Practitioner Register. This is a nationwide register of therapists who have undertaken specialised training and who show evidence of undertaking annual continuing professional development activities. The register is primarily representative of private sector therapists. In New South Wales, for example, the register has 45 therapists listed and only four are from the public sector. The percentage of respondents who had used public services (58%) was almost equal to those using private services (60%); 23% accessed both private and public services.
Treatment of lymphoedema in the private sector can be costly, with fees of $60–180 for each occasion of service. However, treatment from allied health practitioners has been assisted by the federally funded Medicare Benefits Schedule (MBS) for patients with chronic (or terminal) medical conditions and complex care needs. This is a general practitioner (GP) led program that provides a Medicare rebate for up to five visits per year for allied health treatment. Notably, the patient may have other needs that utilise the available visits or may require more than five visits. Similarly, private health insurance with extras covers some of the costs associated with seeing a therapist but this is often capped.
Use of compression, most commonly provided with compression garments, has the strongest evidence base for the treatment of lymphoedema.21,22 Garment use is also likely to be one of the more costly aspects of lymphoedema management. For patients who require daily garment use, two sets of garments replaced every six months is recommended.3,23 Costs can range from $50 for a standard Class 2 sleeve, to $550 for a custom-made sleeve and glove ($200–2200 annually). Some state-funded programs exist in Australia to assist with the purchase of compression garments. For example, in the Northern Territory, all permanent residents with lymphoedema are eligible for two sets of compression garments every 6 months. By contrast, only those residents on Centrelink pensions in the Australian Capital Territory and Tasmania are eligible. The New South Wales scheme has similar provision but requires a co-payment and is income-tested to provide support for those on a low income.20 There is no funding support scheme in South Australia. Some garment costs may be covered by private health insurance with extras but this also varies between schemes and rarely provides more than $500 annually. High costs may result in those with lymphoedema forgoing or compromising treatment by not replacing old garments; using ill-fitting, off-the-shelf garments to avoid the costs of custom-made garments; or avoiding review.
The group we surveyed may have overestimated availability of treatment services for the wider population diagnosed with lymphoedema. Demographic data suggest these women were likely to have better resources to investigate access and fund their own treatment. The questionnaire was in English and was accessed by a consumer group that was computer literate and had internet access. The educational level of this group of women was higher and they were more likely to have private health insurance with extras than the wider population. This was a motivated, educated group navigating a health system in their native language. Some lymphoedema services in Australia have been established within cancer services, or for specific cancer diagnoses, particularly breast cancer, and exclude access for those with primary lymphoedema or secondary lymphoedema arising from other causes. Early detection is also more likely in those with breast cancer-related lymphoedema than primary lymphoedema, as they are known to be at risk and receive education and monitoring following cancer treatment. Despite these additional resources available to these women, one-third of respondents reported significant barriers to accessing treatment for lymphoedema with inadequate accessibility to treatment in urban and rural areas.
Implications for general practice
Women reported difficulty finding appropriate treatment. As GPs are among the practitioners they may turn, GPs needs to be aware of and willing to advise on where relevant information and/or treatment can be sought. GPs need to monitor women with or at risk of lymphoedema to ensure they are being managed appropriately and, if not, direct them to appropriate services.
Cost has also been identified as a barrier. Awareness and advice on what supports might be available to fund treatments (eg. private health insurance, MBS listing for patients with chronic [or terminal] medical conditions and complex care needs, and state government garment programs) will ease the stress and treatment burden associated with lymphoedema.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.