Diagnosis of tendon injuries is usually relatively clear on history and examination. Radiological investigations can be used judiciously for either acute injuries or recalcitrant cases. While this article outlines the principles of diagnosis and management, detail on all the specific tendon injuries is beyond the scope of this article.
In acute tendon injuries there is a history of a sudden tearing or pulling sensation, whereas in tendinopathy there is an insidious onset. Examination usually elicits pain on muscle/tendon concentric and eccentric action, which is worse with specific provocative tests such as ballistic exercise (ie. hopping for patellar or Achilles tendinopathies). The tendon is often tender and may be swollen, either focally or in a fusiform manner. Crepitus is an important sign of paratendonitis/tenosynovitis.
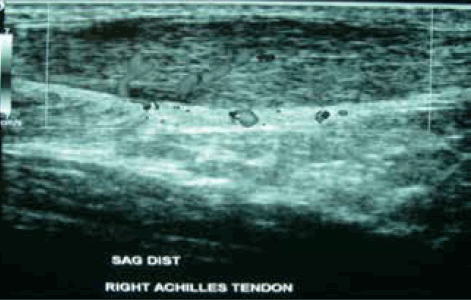
Figure 1. Doppler ultrasound showing the classic features of non-insertional Achilles tendinopathy with fusiform thickening, hypoechoic regions and neovascularisation
In chronic tendinopathies there may be apparent weakness on examination as a result of muscle atrophy secondary to pain and disuse. Unusual findings of referred distal pain, true weakness, or paraesthesia should prompt a consideration of alternate diagnoses. Investigations are generally reserved for cases with an unusual clinical picture, or where symptoms continue despite appropriate treatment (Figure 1 and 2). X-ray and ultrasound are appropriate first-line investigations, with magnetic resonance imaging (MRI) as a secondary investigation.
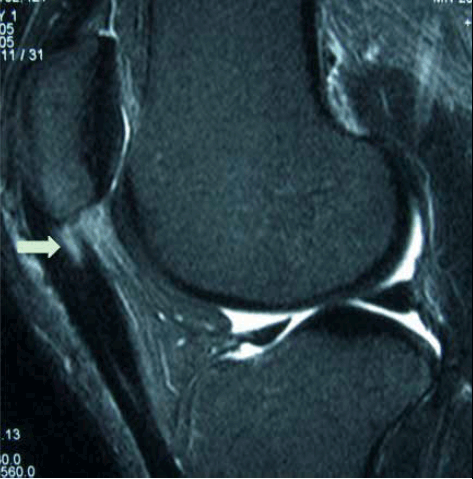
Figure 2. MRI showing deep proximal patellar tendon degeneration with underlying fat pad inflammation
Management
Pain control
In very painful tendon injuries there should be an initial treatment period aimed at pain control and tendon protection. This will involve the regular application of an icepack, 1–2 weeks of analgesia (eg. paracetamol or non-steroidal anti-inflammatory drugs [NSAIDs] depending on the pathology and diagnosis),2,3 and protection of the tendon through bracing and unloading. Non-steroidal anti-inflammatory drugs should be used with caution and are not generally recommended in chronic tendon injuries as the pathology is degnerative. Unloading and protecting most tendons involves avoiding aggravating activities. For some tendons, specific modifications are useful, such as heel raise wedges for the Achilles tendon. Bracing is rarely used. However, there is evidence of efficacy of counterforce bracing in elbow tendinopathies4,5 where gripping or use of the upper limb can be difficult to avoid. Brace straps around the forearm reduce stress through painful elbow tendons by spreading the force through other parts of the musculotendinous unit. The brace should be worn at all times (except when sleeping) for 4–6 weeks to protect the tendon from repeated aggravation. Braces should be removed when performing exercise rehabilitation.
Exercise rehabilitation
Exercise rehabilitation through musculotendinous loading and strength exercises remains the mainstay of treatment for all tendon injuries.6–9 Exercises can involve muscle/tendon shortening (concentric exercise) or muscle/tendon lengthening (eccentric exercise).
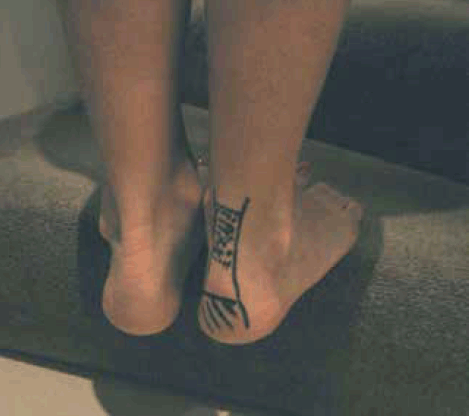
Figure 3. Achilles eccentric exercise performed as the heel drops off a step. The patient’s bodyweight is used to cause the eccentric exercise with the Achilles tendon lengthening under load
Eccentric exercise, specifically using bodyweight to achieve tendon lengthening under load (eg. Figure 3), has a long history of effective clinical use in treating tendon injury, especially chronic tendinopathy.10 The exercise must be specific to the tendon involved and should involve mainly the eccentric component with minimal concentric component (although the benefits of eccentric only exercise over a combination of concentric and eccentric exercises has not been specifically established in upper limb tendinopathies). Figures 3, 4 and 5 demonstrate eccentric exercise for three common tendinopathies:
The exercises may be painful but should not cause progressively increasing tendon pain. Repetitions should be gradually increased to gain strength and endurance (three sets of 15 repetitions twice daily). The load should not be rapidly increased. For upper limb tendinopathies, resistance exercise bands for isotonic exercise are appropriate, or light weights can be used progressively (0.5–1.5 kg). Prescribed exercises should be aligned with the function of the tendons; for elbow tendinopathies heavy loads are not appropriate as it is rare to perform wrist flexion or wrist extension with heavy loads, whereas in lower limb tendinopathies, weightbearing and heavy loading are essential.
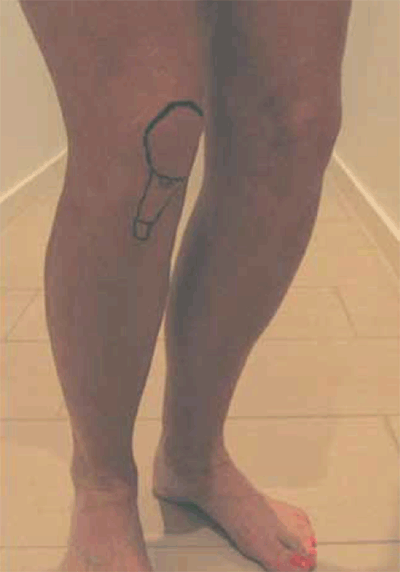
Figure 4. Patellar tendon eccentric exercise should attempt to mimic rapid deceleration movement. This is performed as a rapid drop-squat to 20 degrees knee flexion, where the quadriceps muscles are relaxed and the knee let to flex before rapidly stopping or ‘catching’ the knee flexion at the 20 degree angle. This is best performed on a 30 degree decline to minimise calf muscle use
Maintenance exercise rehabilitation should continue, even after the tendon becomes asymptomatic, to maximise muscle and tendon strength and endurance and to minimise the chance of recurrence. While there is limited evidence of efficacy, specific stretches are prescribed that focus on the affected musculotendinous unit and aim to achieve flexibility and joint range of motion similar to the unaffected side. Each stretch should be pain free, prolonged and repeated.

Figure 5. Elbow eccentric exercise using a 500 g weight (canned food). The forearm is supported on a bench and the wrist is slowly lowered. The other hand is used to help the wrist recover the position (so that there is minimal concentric component of the exercise)
One study showed that in patients where full athletic participation was continued through the competitive season, such as in elite or recreational athletes, eccentric exercise was no more beneficial than no treatment.11 This reinforces the concept that exercise programs only appear to be effective if the patient ceases other aggravating activity for a period of time (probably 4–6 weeks).
Adjunctive therapies
Adjunctive therapies may be used in addition to exercise rehabilitation in the treatment of tendon injuries. These therapies may be classified as either non-injectable modalities (including extracorporeal shockwave therapy and topical glyceryl trinitrate patches) or injectable modalities (including corticosteroid injections, prolotherapy, platelet rich plasma and Doppler ultrasound guided polidocanol injections).
Non-injectable modalities
Extracorporeal shockwave therapy (ESWT) has a long history of therapeutic use, is safe, and can be used to treat specific tendon injuries. It is probably most useful for early calcific tendinopathy, especially in the rotator cuff tendons of the shoulder, and can be effective at dispersing calcific foci (Figure 6).12 For non-calcific tendinopathy, ESWT has some evidence of efficacy in treating patellar and non-insertional Achilles tendinopathy, but the effective and optimal dose, timing and frequency of treatment has yet to be fully developed.13 Contraindications to the use of ESWT include peripheral vascular disease, previous surgical fixation, coagulopathies including warfarin treatment, and children with open growth plates.
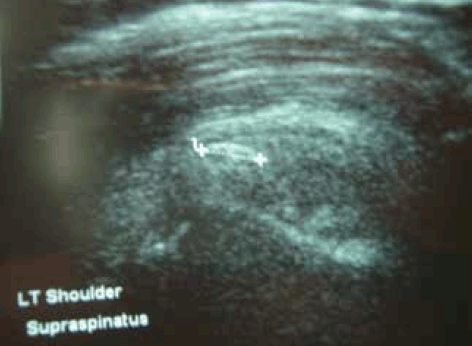
Figure 6. Ultrasound showing calcific supraspinatus tendinopathy. In the early stages, this can be effectively treated with extracorporeal shockwave therapy
Topical glyceryl trinitrate (GTN) treatment can be used in conjunction with exercise rehabilitation to decrease pain and increase functional measures in chronic tendinopathies. There is evidence of efficacy in treating chronic non-insertional Achilles tendinopathy, lateral epicondylosis and supraspinatus tendinopathy when used as a continuous topical dose of 1.25 mg/24 hour (one-quarter of a 5 mg/24 hour GTN patch).14–18 Side effects include headache and rash, and the use of topical GTN treatment is discouraged in patients with ischaemic heart disease or in patients using other vasodilator agents including sildenafil citrate (Viagra®).
Injectable modalities
Corticosteroids
Corticosteroid injections have a long history of therapeutic use in musculoskeletal medicine. They can reduce pain for up to 6–8 weeks, however there is a growing body of evidence that suggests longer term outcomes of corticosteroid injections are neutral, or possibly negative.19,20 Corticosteroid injections are most appropriate where definite inflammatory processes are associated with tendon injury, such as tenosynovitis in de Quervain syndrome, subacromial bursitis associated with supraspinatus tendinopathy, fat pad inflammation associated with patellar tendinopathy or retrocalcaneal or retro-Achilles bursitis associated with insertional Achilles tendinopathy.
Corticosteroids should never be injected into tendon substance (intratendinous) due to the risk of tendon rupture. Ultrasound guidance may be useful for accurate placement. Corticosteroid injections may assist in early pain reduction, but must be used in conjunction with exercise (this may include up to 5–7 days rest before starting or resuming exercise rehabilitation). There is no rationale for a series of corticosteroid injections and a sensible approach is to assess response after a single injection. Approximately one in 20 patients experience a steroid ‘flare’ of pain within 24–48 hours and should be warned of this possibility. Icepacks and/or NSAIDs should provide effective pain control in these cases.
Sclerosing agents
The neovascularisation associated with chronic tendinopathies may be responsible for a component of the pain in these conditions. Doppler ultrasound-guided polidocanol injections can be used to sclerose neovessels in non-insertional Achilles tendinopathy, patellar tendinopathy and supraspinatus tendinopathy.21,22 In studies, 1–5 injection episodes reduced pain by approximately 80% in the majority of cases.21,22 However, pain reduction following sclerosant injections does not directly correlate with reductions in neovascularisation. Polidocanol (also used to sclerose varicose veins) has minimal side effects and does not weaken the tendon. This is the author’s preferred treatment for chronic tendinopathy in large weightbearing tendons such as Achilles or patellar tendinopathy if neovessels are seen on Doppler ultrasound (Figure 7). An experienced operator is required as the blood vessels are 1–2 mm in size.
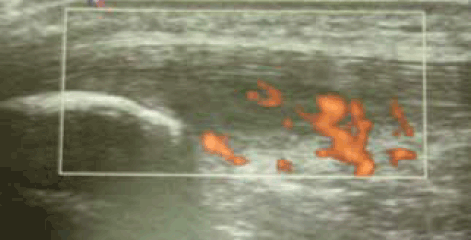
Figure 7. Doppler ultrasound of patellar tendinopathy showing the neovessels. The vessels mostly enter the tendon from the undersurface and this is where they are best sclerosed by polidocanol injections
Platelet rich plasma (PRP) injections have been used in medicine for over 50 years, although there is no research evidence that these injections are effective in treating tendon injuries.23–25 Autologous PRP injections are a second or third line agent in managing tendon injuries, typically as a series of three injection episodes over 4 weeks. Platelet rich plasma may be best delivered with ultrasound guidance to target the region of tendon degeneration; PRP injections appear to produce less postinjection pain than whole blood.
Surgery
Surgery is reserved for recalcitrant cases with failure of non-surgical management after at least 3–6 months. Success rates for surgical treatment of tendon injuries are quoted in the literature as greater than 80% and, although complete pain reduction may not occur, there is often improved function and an ability to return to work or sport.26 However, these studies all have significant limitations, many being case series with no control group.
Summary of important points
- Load management is vital in treating tendon injuries.
- Exercise based rehabilitation incorporating musculotendinous loading is important for most tendinopathies.
- Referral should be considered to a sports physician or sports physiotherapist with a special interest in tendinopathies for elite athletes, children or adolescents, or patients failing conservative treatment.
- Treatment adjuncts are often used, but a guided exercise based rehabilitation program is still essential. Adjuncts include GTN patches, ESWT and injections (blood products, corticosteroids, sclerosants).
- Chronic tendinopathies can take months to resolve, even with the best treatment.
- Patients need education about realistic timeframes and goals, and support throughout the rehabilitation process.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.