Case discussion
A computed tomography (CT) scan revealed a right-sided osteolytic mass at C1 with erosion of the right occipital condyle; features more suggestive of an infective process with malignancy being less likely.
A whole body radionuclide bone scan revealed abnormal uptake at several other osseous sites: right sacrum, right ilium, superior to the acetabulum and T12 (Figure 1). These polyostotic foci could be suggestive of infective or malignant aetiology.
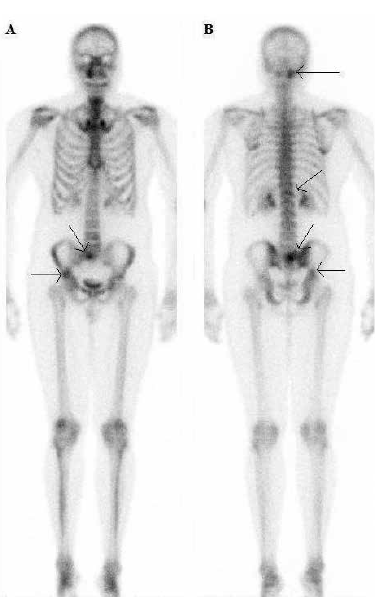
Figure 1. A) Anterior: Intense abnormal uptake by the right sacrum and the ilium (arrows). B) Posterior: Intense abnormal uptake by the right atlantoccipital joint (arrow) and mild uptake by T12 (arrow)
A gallium whole body scan was also performed, which showed intense uptake at the already mentioned sites and the right hilar and paratracheal lymph nodes. Increased uptake can be seen in lymphomas and granulomatous diseases. The lungs were normal (Figure 2).
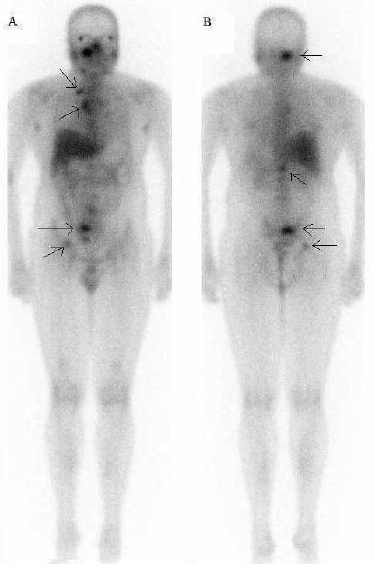
Figure 2. A) Anterior: Intense gallium uptake is seen within a right node and the right hilum (arrows). B) Posterior: Intense gallium by the right atlantooccipital joint, right upper sacrum, body of T12 and the right ilium (arrows)
Polyostotic and joint involvement, together with mediastinal nodal disease is suspicious of extrapulmonary tuberculosis (EPTB) rather than lymphoma. While other causes of polyostotic osteomyelitis and septic arthritis could cause this scan pattern, they were less likely to be present in a patient who was not septic or severely unwell.
The first fine needle aspiration biopsy (FNAB) of the right cervical mass was insufficient for culture. A second FNAB was positive on nucleic acid testing for Mycobacterium tuberculosis. A Ziehl-Neelsen stain found one acid-fast bacillus at histology. The sample ultimately cultured M. tuberculosis. Neurosurgical opinion was the neck lesion at C1 was stable and did not require intervention. A HIV test was negative.
The patient was commenced on standard quadruple anti-TB therapy 2 days after the bone scan was taken. A subsequent culture revealed isoniazid resistance, so this was then ceased.
At follow up, the patient reported decreasing neck pain with no side-effects from therapy. He remained on therapy for 1 year.
Case study 2
An Indian woman, 30 years of age, presented with a 1 month history of severe, left lower neck pain with radiation to both arms. She also reported vague lumbar pain. The patient had cervical tenderness on examination, but was otherwise well with no malaise, weight loss or night sweats. She had been resident in Australia for about 5 years.
Case discussion
A CT scan of the neck revealed a destructive mass lesion of the C7 vertebral body with invasion of the prevertebral space of the spinal canal; placing her at risk of quadraplegia. Further lesions at T11 and L1 vertebral bodies and a left psoas abscess were also found on radionuclide, hybrid single photon emission computed tomography (SPECT)/CT and abdominal CT scans (Figures 3–5).
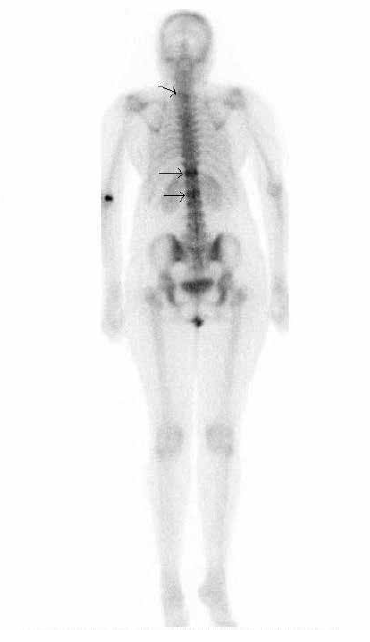
Figure 3. Abnormal uptake by C7, on left (arrow), T11 and L1 (arrows). L1 uptake less due to extensive destruction (see Figure 5)
Aspiration of the left psoas abscess revealed M. tuberculosis. The patient was HIV negative. She was commenced on quadruple anti-TB therapy 9 days after the bone scan was taken. A hard collar was prescribed due to neurosurgical concern for the stability of C7 and possible spinal cord damage. At follow up, the patient was well, with decreasing neck and arm pain and with no side-effects from therapy. Anti-TB therapy was continued for 10 months and she wore the hard neck brace for 4 months.
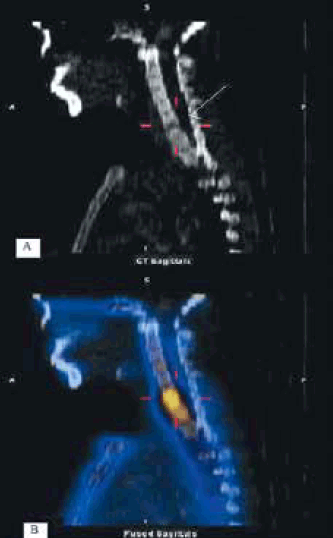
Figure 4. A) Erosive lesion of C7 body invading superior endplate and C6–7 disc (arrow) on CT sagittal slice B) Fused CT and nuclear image showing intense uptake on both sides C6–7 disc and body of C7
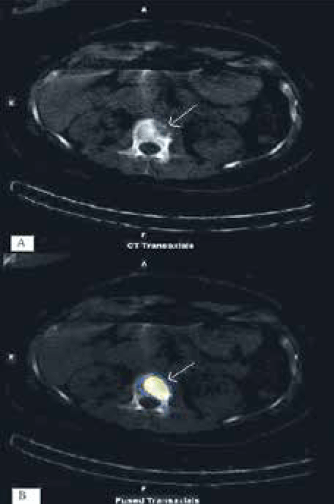
Figure 5. A) CT transaxial slice L1 vertebral body showing extensive right sided destruction. B) Fused CT and nuclear image showing intense uptake by bone surrounding the lesion
Case study 3
A middle aged Indian man presented with mid thoracic spine pain with radiation to the left chest wall. He denied fever, night sweats, malaise or weight loss. There was mild tenderness of the mid thoracic spine. A chest X-ray was reported as normal. He had been resident in Australia for nearly a decade.
Case discussion
Although the radionuclide scan showed only minor hyperaemia of the mid-thoracic spine, the hybrid SPECT/CT scan of the thoracic spine revealed marked bony erosion and extensive paravertebral soft tissue masses at T6 and T7. There were no lung lesions. He was HIV negative.
A CT guided biopsy of the paravertebral collection confirmed M. tuberculosis. Neurosurgical consultation prescribed the wearing of a back brace for 4 months to prevent compression fractures. The patient has been on quadruple anti-TB therapy for 7 months at the time of this report. The patient has been pain free at follow up with no side-effects from therapy.
Discussion
Tuberculosis is the second most common fatal infectious disease in the world, after HIV/AIDS. In 2010, there were around 8.8 million cases of TB, about 1.1 million deaths from TB among HIV negative people and an additional 0.35 million deaths from HIV-associated TB.1 As many as 50% of HIV positive people may have TB. Hence, all patients with EPTB should be tested for HIV.2
In Australia in 2007, there were 1086 new cases of TB (5.4 cases per 100 000), a rate similar to 1986. Of these, 938 (86.4%) were born in TB endemic countries. New South Wales accounted for 437 cases (40.2%). The highest numbers by country of birth were from India, which had 189 cases.3
Extrapulmonary TB presents at a range of sites in the body. In most series, the order of occurrence is lymph nodes, pleural, genitourinary, bones and joints, meninges, bowel and peritoneum, pericardium and the skin. The incidence of osseous EPTB varies from being the most common site of EPTB (24.5%) in Taiwan4 to the third most common site in the United States (11.3%).5
The three case studies presented here were all migrants from India, aged in their 30s or 40s who were HIV negative and had no constitutional symptoms. All had multiple sites of vertebral involvement and soft tissue extensions of the disease. None of the patients had systemic symptoms, but they can occur.6 Two of the patients were neurologically at risk. Neurological complications may require immobilisation or surgery, and EPTB in the craniovertebral junction7 and thoracic spine8 often requires surgical intervention.
The definitive diagnosis of osseous EPTB may be difficult. This was exemplified in Case 1 where two FNABs were required before a single acid-fast bacillus was found. Nevertheless, culture and drug resistance profiling for M. tuberculosis is important.
Imaging can play an important role in the diagnosis of EPTB.9 In Case 1, the initial CT scan identified a destructive cervical lesion and soft tissue mass. The bone scan confirmed its inflammatory nature and identified further sites of osseous disease – all clinically asymptomatic. In Case 2, the CT scan identified a previously unsuspected psoas abscess, which was suitable for biopsy. Hybrid SPECT/low dose CT scanning helped determine the risk of neurological compromise from vertebral lesions.
An issue that may arise in female patients in this age group is tuberculosis in a pregnant woman, which is challenging to manage. Maternal TB is associated with an increased risk of complications (from spontaneous abortion to low birth weight).10 Several first line drug regimens have been approved as being safe for use in pregnant women by the World Health Organization.11 Others, such as the Centres for Disease Control, do not specifically endorse certain drugs in pregnancy.12 The international consensus is that untreated TB poses a greater risk to the pregnant woman and the fetus than
any treatment regimen.12
The time taken for spinal EPTB to resolve was reported in a retrospective series of around 30 cases in 1992.13 All patients had radiological evidence of bony destruction and responded well to standard medical treatment; 70% showed progressive destruction for up to 14 months after treatment was commenced; and radiological changes took an average of 31 months to return to normal.
Key points
- Extrapulmonary TB is unusual, but may be considered in presentations in migrants from TB endemic countries.
- Imaging such as CT scans and radionuclide whole body scans can be useful in the diagnosis and assessment of EPTB.
- HIV testing is recommended if a diagnosis of EPTB is considered.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.