While there is some evidence that patients with a HBPM machine achieve better BP control than those without,10 little is known about the effect of HBPM education on BP control among patients with HBPM machines. The aim of this study was to evaluate the effectiveness of a one-to-one structured education program in the primary care setting for hypertensive patients who owned a HBPM machine. The hypothesis was that patients who had an understanding of HBPM and were able to perform accurate measurements would be more engaged in the self care of their condition, resulting in better BP control.
Methods
Sample frame and size
A cluster randomised controlled trial was conducted in four general outpatient clinics (GOPCs) in the public sector in Hong Kong. General outpatient clinics are operated by a government subsidised public organisation, the Hospital Authority, to provide primary healthcare to the public. Many patients with chronic disease, including hypertension, receive their care in such clinics. Four GOPCs were randomly assigned so that two were in the intervention group and two were in the control group. To account for the clustering effect by clinics, the intra-class correlation coefficient was taken as 0.010, as reported previously.11 In order to have 80% power and two-sided alpha of 0.05 to detect a systolic BP difference of 6.0 mmHg12 with standard deviation of 7.2, 85 patients were required in each group13 and a total of 212 patients were to be recruited at baseline to allow for a dropout rate of 20%.
Inclusion and exclusion criteria
Included patients were:
- aged ≥40 years
- capable of informed consent
- diagnosed with uncomplicated hypertension as recorded in the clinic management system with the International Classification of Primary Care (ICPC) code K86
- currently receiving at least one anti-hypertensive medication
- regularly followed up for hypertension in the participating clinics
- using their own upper arm-type HBPM machine to measure BP at home.
Participation was voluntary and written consent was obtained from all participants. Exclusion criteria are listed in Table 1.
Table 1. Exclusion criteria
- A diagnosis of complicated hypertension (ICPC code K87)
- Malignant hypertension with systolic BP >220 mmHg or diastolic BP >120 mmHg on the day of recruitment
- Known secondary hypertension
- Co-existing diagnosis of atrial fibrillation
- Residence in an aged care facility
- Use of wrist or finger HBPM machines
|
Procedures
Doctors working in the four GOPCs were blinded to the clinic randomisation. A research assistant approached eligible patients over a 3 week recruitment period in each GOPC. Patients’ baseline information including age, gender, duration (in years) of hypertension, and types and dosages of anti-hypertensive drugs were obtained. During visit 1 (baseline), visit 2 (12–14 weeks) and visit 3 (24–28 weeks), systolic blood pressure (SBP) and diastolic blood pressure (DBP) from both upper limbs were measured using the same mercury sphygmomanometer. Two measurements, 15 minutes apart, were made to obtain an average reading for recording.
The structured HBPM education program
Before the start of the study, the research assistant was provided with a protocol and trained to teach and assess patients’ monitoring techniques using a standardised automated BP machine (Omron T9P). Participants in the intervention group were educated by the research assistant at visit 1 and visit 2 on operation of the Omron T9P. Practise self measurements were made under supervision until all the checklist points (recommended by the American Heart Association) were satisfactorily completed (Table 2).14 Patients were told to measure and record their BP at home at least 3–4 times weekly, and to bring their records to each follow up visit. Conversely, patients in the control group received usual care, the nature of which was physician dependent and variable.
Table 2. Checklist score on correct use of automated home blood pressure monitoring machine
| | Checklist points | Score (0 or 1) |
|---|
| 1 |
Do not use caffeine products 30 minutes before measuring BP |
|
| 2 |
Do not use tobacco products 30 minutes before measuring BP |
|
| 3 |
Do not use alcohol products 30 minutes before measuring BP |
|
| 4 |
No exercise 30 minutes before measurement of BP |
|
| 5 |
Rest for 5 minutes before the first reading is to be taken and patient should be relaxed as measurement is taking place |
|
| 6 |
No full bladder before measuring BP |
|
| 7 |
Appropriate cuff size: the bladder length should be 80% of arm circumference |
|
| 8 |
Appropriate cuff size: the bladder width should be at least 40% of arm circumference (ie. a length-to-width ratio of 2:1) |
|
| 9 |
Sit in a comfortable position, with legs and ankles uncrossed, and back and arm supported |
|
| 10 |
All clothing that covers the location of cuff placement should be removed. Long sleeves should not be rolled up to avoid tourniquet effect |
|
| 11 |
Wrap the correctly sized cuff smoothly and snugly around the upper part of the bare arm |
|
| 12 |
The cuff should fit snugly, but there should be enough room to slip one fingertip under the cuff |
|
| 13 |
The lower end of the cuff should be 2–3 cm above the antecubital fossa |
|
| 14 |
The middle of the cuff on the upper arm should be at the level of the right atrium (the midpoint of the sternum) |
|
| 15 |
No talking during BP measurement |
|
| 16 |
No moving during BP measurement |
|
| 17 |
A minimum of two readings should be taken at intervals of at least 1 minute, and the average of those readings should be used to represent the patient’s BP |
|
| 18 |
If there is a >5 mmHg difference between the first and second readings, an additional two readings should be obtained, and then the average of these multiple readings should be used (ask patient if it is not applicable during the patient demonstration) |
|
| 19 |
Ask patient how frequently they will measure their BP at home. (There is no strict rule on the frequency of HBPM. Many suggested the frequency should depend on the control of the BP itself. For our study, we suggested patients measure their home BP two times per day (once in the morning and once in the evening) and measure at least 3–4 days per week) |
|
| 20 |
Properly record the BP reading in the log book |
|
In general, reminders from physicians to bring any HBPM record to follow up visits are fairly common, however the operation of the machine is rarely demonstrated, primarily due to time constraints. Patients in both groups were reminded of follow up appointments via telephone 1 week before their scheduled clinic visits.
Outcome measures
The primary outcome measures were SBP and DBP as measured at follow up visits. The change in SBP and DBP over time was compared, both within and between groups.
Data analysis
Data were analysed by an intention-to-treat approach using SPSS 18.0. Independent t-tests were employed as goodness-of-fit testing confirmed a normal distribution of data. Differences in BP changes between and within the intervention and control groups over the 6 month period were assessed. Blood pressure change of more than 4 mmHg was considered to be clinically significant.
Results
Two hundred and forty hypertensive patients were recruited between October 2007 and July 2008, with 120 patients in each group. The dropout rate was 12.5% and 5.8% in the intervention and control group respectively (Figure 1). This translated to 105 completed in the intervention group and 113 in the control group. No significant difference was found in any of the baseline characteristics of the two groups (Table 3). Over half had less than 3 years of experience in using HBPM machines.
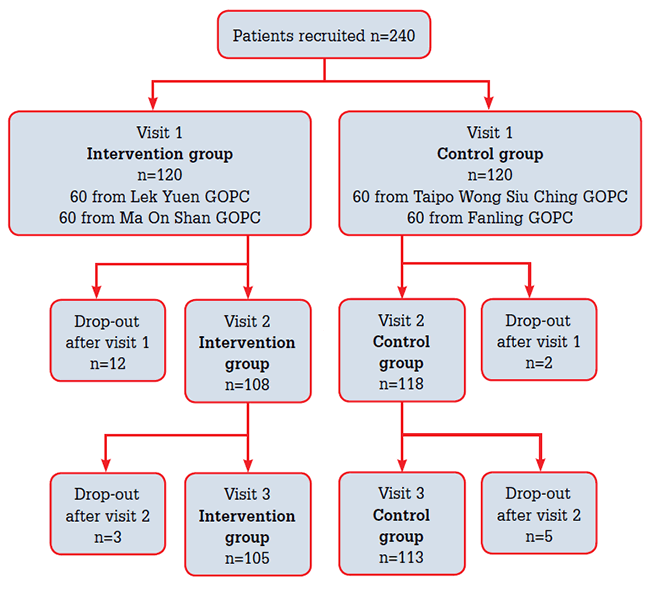
Figure 1. Number of participants in the study
Table 3. Comparison of baseline information of patients in the intervention and control groups
| | Intervention group (n=120) | Control group (n=120) | p value |
|---|
| Gender (n, %) |
|
|
0.069 |
| Male |
46 (38.3%) |
60 (50.0%) |
|
| Female |
74 (61.7%) |
60 (50.0%) |
|
| Age (mean ± SD) |
58.89 ± 8.25 |
58.35 ± 9.71 |
0.646 |
| Year(s) of hypertension (mean ± SD) |
7.45 ± 7.26 |
6.03 ± 5.92 |
0.102 |
| Year(s) of using home BP machine (n, %) |
|
|
0.309 |
| <1 year |
31 (26.3%) |
31 (26.1%) |
|
| 1 to <3 years |
41 (34.7%) |
49 (41.2%) |
|
| 3 to <5 years |
13 (11.0%) |
18 (15.1%) |
|
| ≥5 years |
32 (27.1%) |
21 (17.6%) |
|
| Unknown |
1 (0.8%) |
0 (0.0%) |
|
| Advised on using home BP monitoring from (n, %) |
|
|
|
| Medical professionals |
32 (27.4%) |
34 (28.3%) |
0.866 |
| Family or friends |
24 (20.5%) |
23 (19.5%) |
0.845 |
| No advice |
79 (67.5%) |
71 (60.2%) |
0.241 |
| Diabetes mellitus (n, %) |
|
|
0.739 |
| Yes |
23 (19.2%) |
21 (17.5%) |
|
| No |
97 (80.8%) |
99 (82.5%) |
|
| Blood pressure control (n, %) |
|
|
0.739 |
| Systolic BP (mmHg) (mean ± SD) |
143.33 ± 14.38 |
145.44 ± 16.77 |
0.295 |
| Diastolic BP (mmHg) (mean ± SD) |
87.74 ± 9.60 |
88.00 ± 11.75 |
0.855 |
| Patients achieving target (n, %)†‡ |
28 (23.3%) |
27 (22.5%) |
0.878 |
| Checklist score (mean ± SD) |
14.52 ± 1.68 |
13.66 ± 1.67 |
<0.001* |
| Home BP monitoring frequency (n, %) |
|
|
|
| ≥3–4 times per week |
50 (43.5%) |
51 (44.0%) |
0.940 |
| <3–4 times per week |
65 (56.5%) |
65 (56.0%) |
|
| Record down home BP (n, %) |
|
|
|
| Every time |
44 (37.0%) |
39 (32.8%) |
0.496 |
| Not every time |
75 (63.0%) |
39 (67.2%) |
|
| Give doctor HBPM record on follow up (n, %) |
|
|
|
| Give |
72 (60.5%) |
69 (59.5%) |
0.873 |
| Not give |
47 (39.5%) |
47 (40.5%) |
|
* Significant difference between intervention and control groups by independent t-test or chi-square test
† The target is SBP <130 mmHg and DBP <80 mmHg for hypertensive patients with DM
‡ The target is SBP <140 mmHg and DBP <90 mmHg for hypertensive patients without DM |
The mean SBP and DBP of both groups at the three visits are shown in Table 4. Both groups showed a decreasing trend in mean SBP and DBP from visits 1 to 3. Table 5 shows the changes in mean BP within respective groups from visits 1 to 2 and from visits 1 to 3, and the difference in the reduction in BP between the two groups. The reduction in DBP from visits 1 to 2 was significantly greater (an extra 3.84 mmHg, p=0.004) in the intervention group than in the control group. There was no statistically significant change in types and doses of anti-hypertensive medications used between the two groups over the three visits (data not shown).
Table 4. Comparison of the blood pressure readings between the intervention and control groups throughout the three visits
| | Visit 1 | Visit 2 | Visit 3 |
|---|
| Systolic BP (mmHg) |
|
|
|
| Intervention group |
143.33 ± 14.38 |
136.09 ± 15.06 |
133.40 ± 16.09 |
| Control group |
145.44 ± 16.77 |
140.50 ± 17.61 |
134.23 ± 15.68 |
| Total |
144.38 ± 15.62 |
138.38 ± 16.54 |
133.83 ± 15.85 |
| Diastolic BP (mmHg) |
|
|
|
| Intervention group |
87.74 ± 9.60 |
80.64 ± 8.93 |
79.25 ± 9.07 |
| Control group |
88.00 ± 11.75 |
84.82 ± 11.10 |
79.75 ± 9.92 |
| Total |
87.87 ± 10.71 |
82.81 ± 10.31 |
79.51 ± 9.50 |
Table 5. Mean changes of blood pressure in the intervention and control groups from baseline to 3 and 6 month follow up visits
| Mean difference of change in BP between interval (95% confidence interval) |
|---|
|
|
Visit 2 to visit 1
|
Visit 3 to visit 1
|
| Systolic BP (mmHg) |
|
|
Intervention
Control
Difference† |
–7.24 (–9.86, –4.62)
–5.36 (–8.56, –2.16)
–1.88 (–6.03, 2.26) p=0.372 |
–9.51 (–12.55, –6.47)
–11.21 (–13.99, –8.43)
1.70 (–2.38, 5.78) p=0.413 |
| Diastolic BP (mmHg) |
|
|
Intervention
Control
Difference† |
–6.97 (–8.66, –5.28)
–3.13 (–5.11, –1.14)
–3.84 (–6.45, –1.23) p=0.004* |
–8.15 (–10.00, –6.30)
–7.96 (–9.65, –6.27)
–0.19 (–2.67, 2.29) p=0.881 |
* Significant difference between intervention and control groups by independent t-test
† Difference between the reduction in SBP and DBP from baseline visit 1 between the intervention and control groups
Positive negative value means greater reduction in BP in the intervention group |
Discussion
While HBPM appears to have the potential to enhance the management and control of BP,15–19 our study found that a one-to-one HBPM education program provided in the primary care setting has the potential to produce greater reductions in the BP of hypertensive patients with statistical significance for DBP. However, the difference between the intervention and control groups was no longer significant by visit 3 (6 months from baseline), as a result of an apparent catch-up effect in the control group. It is possible that the act of regular checking of technique for the use of automated BP machines, even without any coaching or education, helps patients to focus on their BP and results in improved control. Alternatively, the impact of the HBPM education program may wane over time. Another large randomised controlled trial on HBPM education found similar results.20 Measures to augment and sustain the benefit of the program need to be further explored. Specifically, targeting patients with poorly controlled hypertension may show a more prominent benefit.
The decreasing trends of SBP and DBP in both groups were highly significant and were consistent with the findings of a meta-analysis that supported the benefits of home BP monitoring.15 The regular reminders for follow up visits and extra assessment of HBPM technique during these visits are likely to have created a Hawthorne effect. This may explain why the drop in SBP and DBP in our study is much greater than the weighted mean decrease in SBP and DBP in a systematic review on the topic.21 It is likely that the educational intervention made the patients more aware of the benefits of monitoring their own BP and equipped them with the skills to do this properly. The presumed flow on effect is empowerment and greater motivation for other activities that enhance BP control, such as increased medication compliance.22 Further studies could help establish these associations. Treating doctor attitudes toward and the use of HBPM to guide management decisions may also influence patient self care behaviour, including HBPM.2
The fact that the effect of the program was not sustained at 6 months, a finding similar to other intervention programs for BP,23 is another area that needs to be addressed.
Strengths and weaknesses
The cluster randomised controlled trial design was used to reduce contamination. The dropout rate was low and there was adequate power in the sample size estimation for analysis. We used the BP readings measured at follow up visits instead of patients’ home BP readings to avoid inconsistencies that may arise due to use of different HBPM machine models. This strategy also helped to minimise the potential overestimation of the effect of the education program.
This study recruited patients from four public sector primary care clinics, so the results might not be representative of all patients with hypertension. The research assistant was not blinded to the randomisation. Voluntary participation of patients who already owned a HBPM machine may have resulted in self-selection of more motivated patients. Further studies could assess the effect of HBPM education in patients who have not previously used HBPM.
Conclusion
Methods of obtaining accurate BP readings in general practice is important for clinicians,24 and having both a regular system of follow up together with HBPM is crucial. A structured one-to-one HBPM education program appears to be able to enhance the short term improvement in BP control in HBPM machine owners, although this benefit was not sustained. The exact mode of delivery of such care demands further exploration and evaluation so as to enhance and prolong the improvement in BP control.
Competing interests: None.
Ethics approval: The Joint Chinese University of Hong Kong – New Territories East Cluster Clinical Research Ethics Committee.
Provenance and peer review: Not commissioned; externally peer reviewed.
Acknowledgements
We would like to thank Ms Lucia Tam for patient recruitment and data collection, Ms Mansy Sham for editorial assistance, Mr Eric Wan for his help in data analysis, Dr Weng Chin for proofreading, and Dr Augustine Lam and colleagues in the New Territories East cluster of the Family Medicine and Primary Healthcare Department of the Hospital Authority who facilitated patient recruitment.