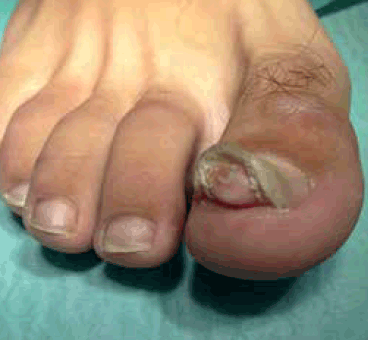
Figure 1. Clinical appearance of the lesion located on the patient’s right great toe
Question 1
What is the most likely diagnosis?
Question 2
What is the aetiology of this condition?
Question 3
How is this condition diagnosed?
Question 4
What are the differential diagnoses?
Question 5
What is the appropriate management of this condition?
Answer 1
The most likely diagnosis is subungual exostosis (SE). Subungual exostosis is an uncommon, slow growing, benign osteocartilaginous tumour arising from the distal phalanx of a digit, beneath or adjacent to the nail bed. Dupuytren first described the condition in 1817.1,2
Answer 2
The precise aetiology of SE is unknown. It was previously considered to be a rare variant of osteochondroma. However, it is a reactive metaplasia of cartilage and is clinically, developmentally, radiographically and histologically distinct from osteochondroma.3 Associated factors such as trauma, chronic irritation to the bone and longstanding infection have been documented,1,2 however, chronic infection seems to be the result rather than the cause of this lesion.2
More recently, a balanced chromosomal translocation [involving t(X;6)] has been reported in a small series of patients with SE, which supports a neoplastic rather than a reactive process.4 In some cases, SE may be a manifestation of one of two inherited conditions: multiple exostoses syndrome and multiple exostoses-mental retardation syndrome (also called Langer-Giedion syndrome, trichorhinophalangeal syndrome type II, Alè-Calò syndrome or MEMR syndrome).5
Answer 3
Clinical appearance and radiographic findings are sufficient to confirm a diagnosis of SE. Clinically, SE appears as a firm and fixed subungual nodule that elevates the nail plate and produces distal or lateral onycholysis. Due to the pressure effect on the nail bed and plate, it tends to be painful and can result in nail plate deformity or destruction. Over time, ulceration and paronychial infection can occur. Although they can involve any digit, 70–80% of lesions are found on the great toe, usually on the dorsal or dorsomedial aspect of the distal phalanx.
A higher frequency of SE is seen in children and young adults with a slight preponderance in girls and women.1,2,6 Subungual exostosis has characteristic radiographic features, and early use of radiography can prevent an incorrect diagnosis and inappropriate treatment, which can lead to recurrence or unnecessary amputation.1,2 An X-ray showing an exophytic lesion on the dorsal surface of the distal phalanx is diagnostic.2
Answer 4
Conditions to be considered in the differential diagnosis of SE are listed in Table 1.1,2,6 Most of these conditions can be easily differentiated from SE based on clinical features and/or X-ray findings. However, biopsy for histological examination may occasionally be necessary in order to establish the diagnosis.
Table 1. Conditions to consider in the differential diagnosis of subungual exostosis
| Disease | Differentiating features |
|---|
| Ingrown toenail (onychocryptosis) |
A painful, swollen, and tender toe, with crusting, purulent discharge, and friable or macerated granulation tissue at one or both sides of the nail bed |
| Verruca vulgaris (viral wart) |
Skin coloured or grayish plaque with a papillomatous, raised, thick and hyperkeratotic surface. Black dots (thrombosed superficial capillaries) may be present on the surface. Can originate from the nail folds or the hyponychium and spread to the nail bed. Onycholysis, onychodystrophy and/or pain may occur |
| Pyogenic granuloma |
Rapidly growing, exophytic papulonodule affecting the nail fold or hyponychium. Colour ranging from bright red to bluish-purple. Size may vary from millimetres to centimetres. May feature an ulcerated, erosive or friable surface, which bleeds easily |
| Glomus tumor |
Small red-bluish patch or nodule under the nail plate, usually on the fingernails and associated with paroxysmal pain, tenderness, and temperature sensitivity. Pain may be provoked by mild trauma and radiate to the limb. The nail may be ridged or dystrophic8 |
| Osteochondroma |
Subungual location is quite rare. Well defined, firm, and often painful exophytic tumour causing onycholysis of the nail plate. Usually appears more proximal than a SE, and is often larger in size. Definitive diagnosis dependant on microscopic evaluation of the excised specimen (distinctive hyaline cartilage)3 |
| Lipoma |
Extremely rare in the nail unit. May present as a soft, mobile, and usually asymptomatic nodular tumour, located subungually or in the lateral fold |
| Fibroma/fibrokeratoma |
Painless, slow growing, nodular or filiform (sausage-like) lesion, often with a keratotic surface, usually arising from beneath the proximal nail fold and causing a longitudinal depression. Subungual lesions are uncommon and usually result in onycholysis. Multiple periungual fibromas (Koenen tumors) can occur in patients with tuberous sclerosis8 |
| Keratoacanthoma |
Rapidly growing, painful, well demarcated, dome-shaped nodule with a central keratin plug. If left, spontaneous involution occurs, leaving a small, pitted scar. May involve the hyponychium or the proximal nail fold and sometimes also affects the underlying bone. May be locally destructive. Difficult to distinguish from SCC and malignant transformation to SCC occurs rarely8,9 |
| Squamous cell carcinoma (SCC) |
In situ SCC (Bowen disease): warty plaque, usually in fingernails; sometimes presents as periungual erythema associated with crusting, ulceration or fissuring, paronychia, longitudinal melanonychia or nail dystrophy8,10
SCC: slowly growing subungual nodule that eventually ulcerates and bleeds, or a wart-like periungual growth. The underlying bone is commonly involved. More common in the fingernails and after the fifth decade of life8,10 |
| Subungual malignant melanoma |
Rare form of melanoma, most common in middle aged or elderly patients, especially on the thumb or hallux. May arise within the nail matrix or bed. Longitudinal melanonychia and Hutchinson sign (periungual brown-black pigmentation) are typical. Dermatoscopic examination is useful. Lesion is amelanotic in 25% of cases. May develop a usually painless nodule under the nail plate, with ulceration, bleeding and onycholysis8,11 |
Answer 5
Surgical excision is the appropriate management of this condition. The general practitioner can perform this in the clinic, but GPs unfamiliar with the procedure may prefer to refer to a general surgeon. Excision is usually performed under digital block anesthaesia. A conservative approach under the nail and preserving nail coverage is often possible. The skin is incised and the bony lesion dissected. It is then clipped off at its base using a bone rongeur or a strong nail clipper, followed by curettage of the distal phalanx with a bone curette. The wound is closed with simple sutures.
If the exostosis is located more proximally under the nail plate, the nail plate may need to be partially or totally avulsed to facilitate the entire removal of the lesion. A technique in which nail plate is sutured back into place after removal of the exostosis has also been described.4,6,7 Incomplete surgical resection may result in local recurrence. A recurrence rate of 5–11% has been reported.2 However, no case of malignant transformation has been reported.2,6
Case study follow up
Because of the degree of nail deformity and onycholysis, the patient required a complete nail plate resection. The tumour was removed and histology showed mature trabecular bone covered by hyaline fibrocartilage tissue, confirming the diagnosis of subungual exostosis.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.