There has been much discussion recently about chlamydia testing for asymptomatic women, both with and without a routine Pap test in general practice.4,5,7,8 However, while GPs believe general practice is an appropriate place for chlamydia testing, there are currently barriers which can prevent this taking place.5,8 These barriers include deficiencies in public knowledge and lack of formal recall systems. Workload, time and cost are factors identified by GPs specifically.5
The Australian Collaboration for Chlamydia Enhanced Sentinel Surveillance (ACCESS) was established to trial the monitoring of the uptake and outcome of chlamydia testing in Australia. An evaluation of the program, undertaken 2 years after it was funded, found the program can be used to provide 'a better understanding of long term trends in chlamydia notifications and to support policy and program delivery'.9
The North Queensland Practice Based Research Network (NQPBRN) undertakes research with general practices in northern Queensland. This study was undertaken by the NQPBRN to gain an understanding of chlamydia management in general practice in northern Queensland. The study had three components: a clinical audit of chlamydia-positive cases; a prospective audit of patients referred for a chlamydia test; and a GP survey of usual management of chlamydia infection and preferred methods of contact tracing.10 This article reports on the prospective audit of patients referred for any type of chlamydia testing (ie. asymptomatic testing or testing for symptomatic women) and aims to describe the reasons for testing for chlamydia in general practice encounters and plans for follow up of test results. Re-testing was explored in other components of the study, namely the GP survey of usual management of chlamydia infection10 and the clinical audit of chlamydia positive cases.
Method
Eighteen practices within the NQPBRN were invited to participate and nine general practices agreed to take part. Five practices in Townsville and four in Mackay participated; practice sizes varied from 3–9 GPs. An audit sheet was developed for the prospective audit which included patient gender, date of birth, date chlamydia test ordered, reason for referral, and if a follow up visit for test results was recommended and entered on the practice recall system. Practice nurses collected the audit data from clinical records before the requested tests went to the laboratory. Patient data were de-identified and analysed using simple descriptive statistics. Age was summarised using median values and inter-quartile ranges (IQR). Reason for referral for testing was presented together with 95% confidence intervals. Statistical analyses utilised SPSS for Windows (Version 17, SPSS Inc, Chicago, Illinois). Adjustments for clusters were calculated using STATA/SE for Windows (STATA Corporation, College Station, Texas).
Data was collected for 3 months per practice or up to 100 referrals if 100 referrals were reached before 3 months. Two practices collected 100 referrals in under 3 months; these practices were centrally located in regional towns with multiple doctors, including female doctors.
James Cook University Human Research Ethics Committee granted ethics approval for the study (approval number H3577).
Results
A total of 521 patients had chlamydia testing recorded with females comprising over threequarters of patients (77.0%; 401/521). The median age was 24 years and the inter-quartile age range was 20–30 years. The majority of patients referred for testing were in the 20–24 years age group (37.4%; 195/521) and three-quarters of patients referred for testing were aged 29 years or less (74.9%; 390/521).
Asymptomatic presentations accounted for 50.1% of total referrals for testing (95% CI: 36.0%; 64.1%). Asymptomatic tests for females were fairly evenly split between a GP initiated test with a Pap test (23.8%; 95/400) and female patients presenting for a general sexual health check (27.5%; 110/400). Tests due to contact with a known positive case were 3.7% of tests for both genders (95% CI: 1.9% to 5.4%) with 7.5% male (95% CI: 1.1% to 13.9%) and 2.5% female (95% CI: 1.6% to 3.4%). Nearly a third of tests (29.8%) were in response to symptoms (95% CI: 22.1% to 37.4%) with similar rates for both males and females. The remaining tests were for other reasons (11.7%) or there was no record (5%). Reasons for chlamydia testing are summarised in Table 1.
Of the patients referred for chlamydia testing, less than half had a recommendation for follow up of test results recorded (41.4%; 207/500). Patients with a known positive case contact were most often recommended for a follow up visit (58.8%; 10/17), followed by patients presenting with symptoms (59.3%; 89/150). Patients presenting with 'other' reasons had similar follow up rates (59.6%; 34/57, Figure 1).
Table 1. Reason for chlamydia testing referral (n=496) by gender
| Reason for referral | % (n) | 95% CI of proportion |
|---|
| Asymptomatic
|
50.1 (261)
46.7 (56)
51.1 (205) |
36.0 to 64.1
36.6 to 56.8
35.8 to 66.5 |
| Contact with chlamydia case
|
3.7 (19)
7.5 (9)
2.5 (10) |
1.9 to 5.4
1.1 to 13.9
1.6 to 3.4 |
| Symptomatic
|
29.8 (155)
29.2 (35)
30.0 (120) |
22.1 to 37.4
22.7 to 35.6
20.1 to 39.7 |
| Other reason
|
11.7 (61)
10.8 (13)
12.0 (48) |
5.2 to 18.2
1.5 to 20.1
4.0 to 20.0 |
| Note: n=496 due to 25 replies having no record of the reason for testing |
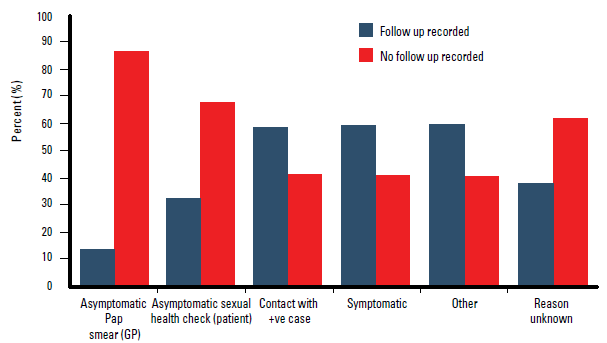
Figure 1. Reason patient was referred for chlamydia test
Discussion
The largest numbers of patients undergoing chlamydia testing were in the 20–24 years age group and there were more females than males, which reflect findings in the literature.6 This suggests relative undertesting of sexually active teenagers as, according to Australian epidemiological data, chlamydia is also highly prevalent in younger age groups (16–19 years).11
Half of those having a chlamydia test were asymptomatic, with a third of this group screened at the time of a Pap test, suggesting GPs are appropriately initiating chlamydia screening with Pap testing. A survey of Victorian GPs found that GPs are more likely to test patients who report symptoms or a recent risk event.12 While almost a third of patients in this study were symptomatic, very few reported contact with a known positive case (3.7%; 19/520) and this might have been expected to be higher. Possibly patients are not discussing contacts with their GP and even if they are, 'Australian surveys have indicated that contact tracing in general practice is inconsistent, and suffers from many barriers'.3 Thus, positive patient contacts are probably not being tested,2,10 although partner delivered treatment for contacts 'on spec' may be provided.13
One of the practices that contributed almost a fifth of the study data has a standard policy to recommend a follow up visit to obtain results. Despite this, 58.6% of patients had no follow up recorded. Doubt remains as to whether this is a failure of advice or documentation, however, if a positive result was returned, these patients and their contacts may be at risk of not being diagnosed or treated.
Limitation of this study
This research was limited to nine practices in northern Queensland, although practices varied in size and location. Data collection was limited to what was recorded in medical records, regardless of overall practice policy. For example, based on the data for this study, we are unable to comment specifically on whether GPs performed the appropriate test for chlamydia for symptomatic or asymptomatic patients. Practices were asked if recommended follow up visits were entered on the practice recall system as a separate question. Practice policy for use of their recall system varied at the data collection point, eg. one practice advised a recall is only placed if there is an abnormal result, therefore data for the practice recall system was excluded. Data was collected for a maximum 3 month period by each practice over a timeframe of 5 months for all practices in the study. While we did not collect data on the resident status of patients, the 5 month timeframe reduces the possible impact of patients who were transient.
Implications for general practice
The age and gender of patients tested for chlamydia in this study is consistent with national data and suggests that GPs are utilising chlamydia testing appropriately. However, there is potential to increase rates of opportunistic testing for asymptomatic women, particularly in young, sexually active people. The low number of patients presenting due to contact with a known positive case warrants further investigation.
Constraints within general practice may partly explain the number of patients not recorded as recommended for follow up of their chlamydia test, however, if chlamydia is to be controlled, increasing follow up, treatment and retesting will be an essential component.
Conflict of interest: none declared.
References