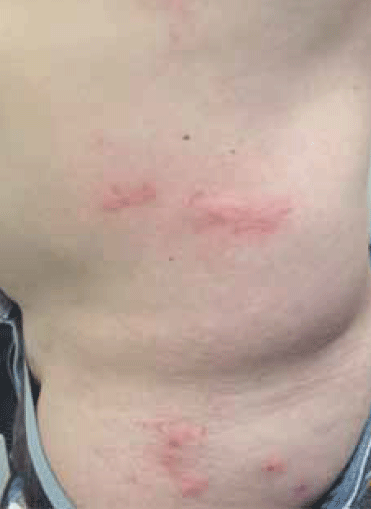
Figure 1. The patient's rash
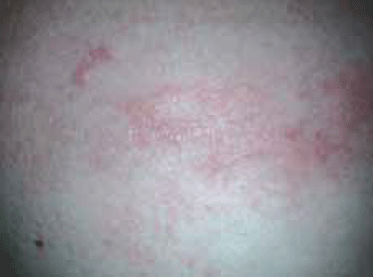
Figure 2. Close-up view of the patient's rash
Question 1
What is the most likely diagnosis?
Question 2
What is the aetiology of this condition?
Question 3
Describe the clinical features of this condition.
Question 4
How would you treat this? What are the options?
Question 5
How can this condition be prevented?
Question 6
What teledermatology services can be accessed by rural GPs in Australia?
Answer 1
Cutaneous larva migrans (CLM).
Answer 2
Cutaneous larva migrans is caused by the larva of the animal hookworms, which penetrate and migrate through the skin of accidental human hosts.1,2
The most common species is Ankylostoma braziliense followed by A. caninum, which is endemic in the developing world and is most commonly seen in ‘first world’ tourists returning from holidays in tropical countries.3,4 It also occurs across Australia with various cases reported in different population groups, although incidence is significantly lower due to the deworming of pets and other public health measures.5,6
Intestinal adult hookworms reside in dogs and cats and their eggs are passed in faeces into superficial layers of soil. The moist and warm conditions of beach soil, in particular, facilitate egg hatching and larva survival.1,7
Humans are infected when they come into contact with contaminated soil. Larva penetrate intact skin and pass through the epidermis, but lack lytic collagenases required to cross the epidermal basement membrane. As a result they are unable to complete their lifecycle in humans and die within 2–8 weeks.4
Answer 3
The most prominent symptom of CLM is pruritus at the site of the skin eruption.1,2,8 The key clinical features of CLM are the presence of erythematous, linear or serpiginous (snake-like) tracks known as ‘creeping dermatitis’. These disorganised tracks are caused by larva, which migrate through the epidermis, leaving a trail of inflamed and pruritic skin. These tracks are approximately 2–3 mm wide and stretch up to 30–40 mm from the penetration site with the larva itself being anywhere up to 1 cm or more from the end of the track.1,3,4,9,10
In rare cases, eosinophillic pneumonitis (Loeffler syndrome) has been associated with CLM infestation.1,7,8
Answer 4
The patient was prescribed a single, 21 mg dose of ivermectin. Review 5 days later demonstrated complete resolution of the rash, with pruritis remitting within 24 hours.
Cutaneous larva migrans is self limiting and, while disturbingly itchy, is benign, with lesions resolving without treatment within 4–8 weeks in most cases. Patients can be reassured regarding this.
Oral ivermectin is the drug of choice and is taken as a single dose (200 µg per kg bodyweight). It is highly efficacious, killing the migrating larvae and relieving itching, with symptoms resolving within 1 week of treatment.1,2,7
In the event of treatment failure, this dose can be repeated and usually provides a cure. It is contraindicated in children (weight <15 kg or <5 years) and in pregnant and breastfeeding women.
Albendazole 400 mg/day for 3 days is also effective. Albendazole can be given to children >6 months of age and is safe for use in breastfeeding women.1,2,7,9
Bacterial infections secondary to scratching can complicate the condition and should be treated with appropriate antibiotics.1,2,7,10
Cryotherapy with liquid nitrogen has been described and studied but is not recommended as it is both painful and ineffective. The larva are commonly located several centimetres ahead of the visible track and are capable of surviving temperatures as low as minus 21°C for more than 5 minutes, conditions which would lead to painful ulceration of the patient’s skin.1,2,7,8
Answer 5
Travellers to tropical and subtropical countries should be advised to avoid skin coming into contact with contaminated soil. This can be minimised by directing travellers to avoid beach areas where dogs and cats are seen roaming, and prevented by wearing appropriate footwear when walking on the beach and by using deck chairs or mattresses when lying on the beach.
Answer 6
There are several regional and two well-known national services. Tele-Derm is a free service that can be accessed through the ACRRM education portal ‘RRMEO’ by members and rural doctors, which provides education through online cases, a condition index and a case discussion forum (www.acrrm.org.au/tele-medicine).
‘Skinconsult’ provides both a teledermatology service and a web based educational site for GPs interested in furthering education in dermatology. Teledermatology consultations are privately billed to patients, or billed to Medicare for pensioners (www.skinconsult.com.au/index.htm).
Conflict of interest: none declared.