Multiple modalities are used with spinal imaging and with increasing access to magnetic resonance imaging and better imaging quality, primary care physicians are being exposed to nomenclature utilised by neuroradiologists and specialists in the field of spinal medicine. This article aims to clarify the terms commonly used and its clinical implications in lumbar spinal imaging.
Clinical presentation
Patients with spinal pathology often present with a range of symptoms. It is useful to differentiate the three most common symptoms – lumbar back pain, sciatica and claudication – as they can assist in determining the source of the patient's symptoms. While magnetic resonance imaging (MRI) is sensitive in detecting spinal pathology, often it discovers a multitude of conditions that may not have any significant clinical impact.
Lumbar back pain can result from several conditions ranging from facet joint arthropathy to muscular strain. The pain is mainly localised in the back as the term suggests, and tends to arise from locally affected structures.
Sciatica, on the other hand, has a different pattern of pain in terms of distribution and is caused by irritation of a nerve root. This can occur due to the direct compressive effects of an intervertebral disc herniation on a nerve root or an underlying inflammatory process, such as infection causing acute pain in the distribution of a dermatome.
Claudication is traditionally divided into two categories: neurogenic or vasogenic, depending on the underlying cause. It is often described as impaired mobility and dull aching pain in the lower limbs. Central vertebral canal stenosis is a common cause of neurogenic claudication and has a variable pattern, while vascular claudication it is more consistent and reproducible.
The importance of determining symptom chronicity and identifying 'red flags' in the history and clinical examination, such as fevers and perineum paraesthesia, are crucial in the formulation of the clinical diagnosis and differentiating benign causes, such as musculoskeletal strain, from more serious conditions such as epidural abscesses or spinal metastases. Certain risk factors such as the patient's age, medication history (eg. steroid use) and pattern of stiffness may also raise suspicion of ankylosing spondylitis or compression fractures. This would direct further investigation with appropriate serum tests and imaging. Guidelines, such as those developed by the American College of Physicians and Pain Society, can direct diagnostic testing for 'red flag' causes of lumbar back pain.2
Magnetic resonance imaging
Magnetic resonance imaging utilises proton resonance technology to obtain soft tissue cross-sectional representations of the spine. The quality of these images allows the diagnostician to make more detailed and accurate assessments of the intervertebral disc and its relation to the neural structures when compared with more traditional methods, such as lumbar and computed tomography (CT) myelograms.
A systematic review of the available literature involving spinal MRI found MRI to be a highly sensitive and but less specific imaging modality for lumbar spinal conditions.3 For example, high sensitivity ranging between 89–100% for disc herniation have been described in previous studies.4,5 The lower specificity, 43–97% for disc herniation has been highlighted in previous literature and relates to the prevalence of asymptomatic disc degeneration and protrusions resulting in a large number of false positives.6 In a group of 57 patients with unilateral lower limb radiculopathy, only 30% of these patients had MRI findings of disc herniation and nerve root compression at the same level as the clinical prediction.7 Therefore, when reviewing the imaging, one must exert a degree of care when attributing the patient's symptoms to the appearance of their lumbar spine.
Lumbar spine anatomy
The lumbar spine consists of five separate vertebrae separated by intervertebral discs and reinforced by multiple ligaments and paravertebral muscles. The thecal sac containing the conus medullaris and nerve roots are located within the central vertebral canal. The nerve roots then exit the spine via the intervertebral foraminal canal obliquely instead of at right angles, which is observed in the cervical spine. Understanding this anatomical relationship allows the clinician to isolate the exact nerve root being irritated by a herniated intervertebral disc (Figure 1).
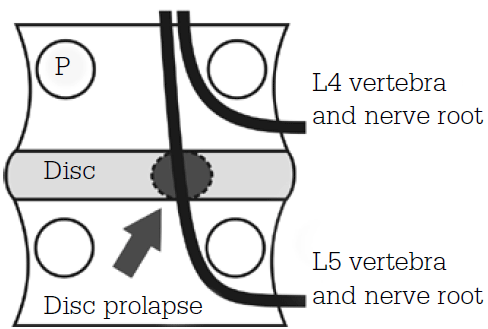
Figure 1. The relationship of the exiting nerve roots, pedicle (P) and intervertebral disc
The exiting nerve roots traverse the neural foramen and this is divided into sections based on its relationship to the pedicle and zygapophysical joint in the axial and sagittal planes (Figure 2). In the axial plane, the exiting nerve root traverses the subarticular recess from the central zone to the foraminal and extra-foraminal zones. Infra-pedicular, supra-pedicular, pedicular and disc levels are used to separate the areas along the longitudinal axis.
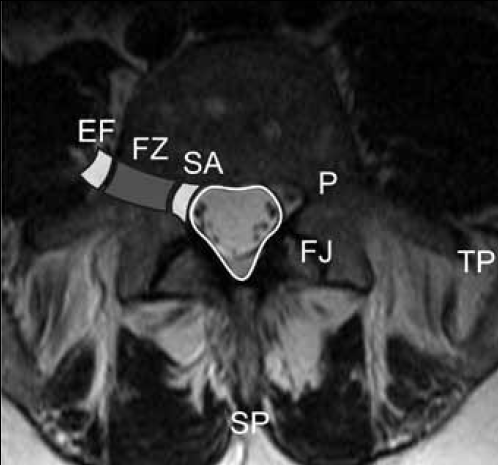
Figure 2. Axial T2-weighted slice of the lumbar spine demonstrating the various zones along the course of the exiting nerve roots from the sub-articular zone (SA) to the foraminal zone (FZ) and the extra-foraminal zone (EF)
P = pedicle; FJ = facet joint TP = transverse process SP = spinous process
Intervertebral discs have a hydrated nucleus pulposus contained within concentric rings of annulus fibrosus. With increasing age, the discs progressively dehydrate resulting in a decrease in T2 signal, which are frequently seen in asymptomatic patients.
Disc pathology
Nomenclature used in reports of spinal imaging has been confusing and inconsistent. Until a consensus review by several working groups in North America developed a recommendation on terminology8 used in describing lumbar disc pathology such as disc sequestration and fissures (Table 1).
Table 1. Classification of disc lesions
|
Normal
|
|
Congenital/developmental variant
|
|
Degenerative – annular fissure, herniation, degeneration
|
|
Inflammation/infection
|
|
Neoplasia
|
|
Morphological variant of unknown significance
|
Annular fissure
Any separation between annulus fibres or avulsion of annulus fibres from the vertebral bodies is defined as an annular fissure. These changes often occur in the setting of asymptomatic disc degeneration. Therefore the term 'annular tear' is discouraged as it implies a traumatic trigger. A review of 40 post-discography CT scans found poor correlation between the side of back pain and the side of annular tear in patients with a single level, concordantly painful and fissured discs identified during lumbar discography.9
Disc herniation
Disc herniation occurs commonly in two scenarios where the spinal column has sustained trauma in the form of abnormal axial loading or altered dynamics secondary to congenital or acquired spinal deformity. The resulting herniation results in nerve root compression and pain.
Any disc material extending beyond the vertebral bodies is considered a herniated disc. This is described further as 'disc bulge', 'protrusion', 'extrusion' and 'sequestration'. The fundamental aim of using these terms is mainly a descriptive one and allows effective communication to general practitioners.
The amount of disc extension circum-ferentially on the edges of the vertebral endplate (ring apophyses) is assessed initially; the term 'bulging disc' is used to describe extension of the disc around 50–100% of the ring apophyses. Displacement of between 25–50% is described as 'broad-based herniation' and <25% as 'focal herniation'.
A protruded disc is defined as having a wider base when compared with the extent of disc material spreading beyond the vertebral body (Figure 3). Conversely, when the extent of disc spread is greater than the base of the disc extension, it is described as being 'extruded'. When there is separation between the herniated disc and the parent disc, it is described as being 'sequestrated' (Figure 3).
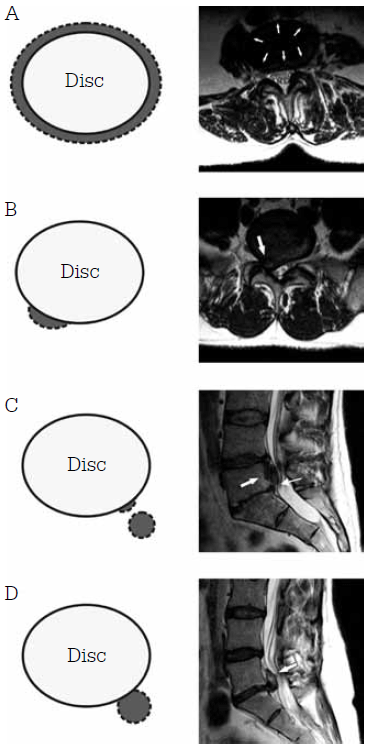
Figure 3. Axial illustration and T2- weighted MRI of the lumbar spine showing disc herniation
A = bulging disc; B = right sided broad based paracentral protrusion; C = sequestration of disc material. Line arrow: separation between the herniated disc (block arrow) and the intervertebral disc space; D = extrusion
In an attempt to correlate clinical findings and radiological evidence, the relation of the herniated disc to the nerve root is carefully examined. Any contact, displacement or inflammatory changes would be reported to allow accurate localisation of the patient's symptoms to the offending compressive disc lesion.
Central vertebral canal stenosis
Gradual development of central vertebral canal stenosis where there is compression of the nerve roots in the thecal sac (Figure 4) often results in progression of decreasing mobility and neurogenic claudication. In instances where an acute event has occurred, the initial presentation may occur as cauda equina syndrome, urgent surgical decompression is required.
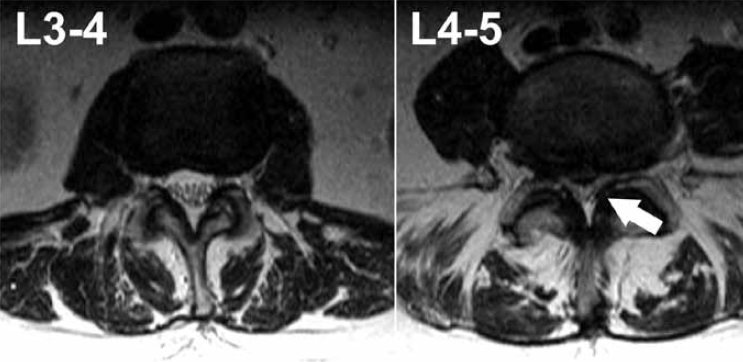
Figure 4. T2-weighted axial slices of the lumbar spine of the same patient at different levels. There is severe central vertebral canal stenosis at the L4–5 level (arrow) with no cerebrospinal fluid and crowded cauda equine nerve roots. At L3–4 the nerve roots can be seen as low signal dots surrounded by bright cerebrospinal fluid
The causes of central vertebral canal stenosis can be divided into congenital and acquired conditions, such as neoplastic and degenerative changes. Degenerative changes include facet osteophytes, ligamentum flavum hypertrophy and disc herniations. While some conditions have a specific/dominant cause, most central vertebral canal stenoses are caused by a combination of conditions.
The severity of central vertebral canal stenosis is visually graded and currently no universal grading scale is being used. Several centres have assessed various grading methods, including measuring the cross-sectional area and morphology of the thecal sac.10 However, using imaging alone to assess severity is inadequate as there is often a mismatch between the symptomology and MRI findings,11 as well as inter-observer variation between radiologists.
Ankylosing spondylitis
Plain radiography of the affected joints remains the initial imaging method for patients with suspected ankylosing spondylitis. However, clinicians are using MRI more frequently to diagnose this condition and to monitor treatment response. The main features on MRI of the lumbar spine include features demonstrating underlying inflammation and its effects, such as bone marrow oedema, squaring of the vertebral bodies (Romanus lesions), syndesmophyte formation, ankylosis and erosions (Figure 5). The clinical and imaging aspects of this condition are complex and beyond the scope of this article. They are discussed in detail by a group from the United Kingdom.12
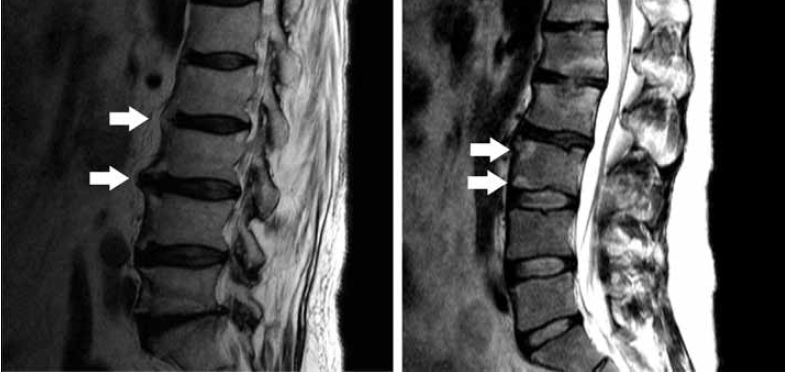
Figure 5. Sagittal T2-weighted images of the lumbar spine in two separate patients with ankylosing spondylitis. Left: arrows point toward bridging syndesmophytes; right: arrows point toward marrow changes near the endplate, consistent with inflammation
Spondylolisthesis
Spondylolisthesis is defined as a condition where there is malalignment of the lumbar spine in the form of a vertebra slipping out of its normal position relative to the inferior vertebra. This can result in narrowing of the lateral neural foramen and the central spinal canal (Figure 6). Furthermore, pars defects and lumbar spondylosis are commonly associated with spondylolisthesis. The chronic nature of pain experienced by the patient as well as the complex mechanical issues revolving spinal malalignment can often result in failure of conservative treatment and surgical fusion of the affected level maybe required.
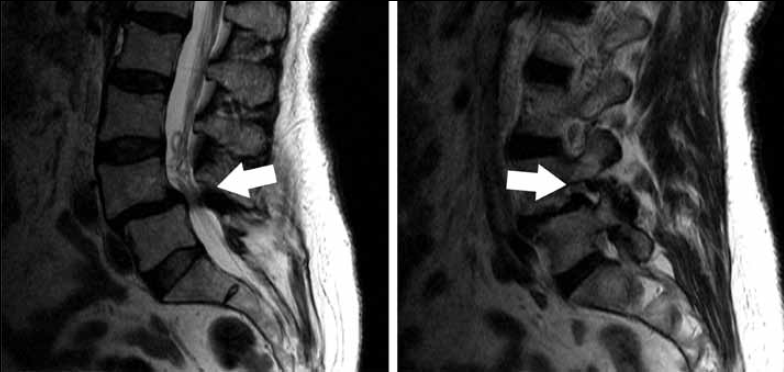
Figure 6. Sagittal T2-weighted MRI acquisitions of the lumbar spine. There is anterolisthesis at the L4–5 level, resulting in severe central canal and neural foraminal stenosis with associated nerve impingement
The role of MRI is to determine the severity of any central spinal canal stenosis or neural foramen and to identify a potential cause such as a pars defect. However, due to the static nature of MRI imaging acquired with the patient lying down, stability at the affected level is uncertain. Spinal surgeons have used dynamic lumbar spinal plain X-rays to assess any potential exaggeration of spinal malalignment, which implies further stenosis and nerve impingement. The addition of rigorous dynamic MRI spinal imaging studies in the future may offer a better alternative.
Summary
A better understanding of the benefits and limitations of MRI in evaluating lumbar back pain and the use of a universally accepted terminology by the various specialties involved in patient care, can lead to better treatment outcomes of a patient's radiologically matched clinical issues.
Conflict of interest: none declared.