Case study
A woman, 84 years of age, presented to our southeastern Queensland general practice for removal of an engorged tick from her right external auditory meatus, thought to have been present for several days. She re-presented 3 days later with a right facial nerve palsy that affected her frontalis muscle only (Figure 1). The facial nerve palsy resolved spontaneously over the next 7 days (Figure 2).

Figure 1. Patient with right facial nerve palsy
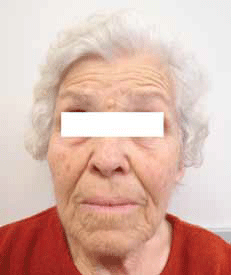
Figure 2. Patient 7 days after presentation
Question 1
What are the possible causes of this presentation?
Question 2
What species of tick affects humans residing in southeast Queensland?
Question 3
What are the possible complications of being bitten by a tick?
Answer 1
Possible causes of this presentation include:
- local diffusion of tick neurotoxin
- Ramsay-Hunt syndrome (viral infection of the ear and geniculate ganglion associated with facial paralysis)
- idiopathic Bell palsy (idiopathic facial paralysis).
In this case, we attributed the patient's facial nerve palsy to local diffusion of a potent neurotoxin secreted from tick saliva, which affected the upper fibres of the temporal branch of the facial nerve. There were no herpetic lesions within the ear canal and the paralysis affected only the right frontalis muscle with orbicularis and the lower facial muscles spared. With other lower motor neuron lesions such as Bell palsy and Ramsay-Hunt syndrome usually all three divisions of the nerve are affected.
In this case, extraocular movements were preserved, as was the function of other cranial nerves. The patient's involutional brow ptosis was more marked due to the lack of frontalis action leading to apparent fullness of the right upper lid, but there was no true lid ptosis. Mild subjective reduction of sensation in the distribution of the first branch of the trigeminal nerve (V1) including corneal sensation was elucidated. Confounding the patient's presentation was that 3 weeks earlier she presented with V1 shingles, which had since resolved. At 1 week, her frontalis action had almost completely resolved and V1 sensation was improved but not fully recovered.
Despite affecting a purely motor nerve, there are reports of dysaesthesia in idiopathic Bell palsy,1 however we postulate that in this case the dysaesthesia was most likely residual to the V1 shingles based on the corneal involvement and delayed recovery compared to motor function. Direct diffusion of the toxin to the trigeminal nerve is unlikely due to its anatomical course.2
Answer 2
Ixodes holocyclus (paralysis tick) is endemic to southeast Queensland and is distributed along a 20 km wide band which runs along the eastern coastline of Australia.3 It is virtually the only tick that affects humans residing in this area.4
Answer 3
The prolonged attachment of the gravid female is known to cause ascending flaccid paralysis in domestic pets, and rarely, in young children (usually under 3 years of age) by injecting a potent neurotoxin intermittently while feeding.4,5 In this case, it was later reported that the patient's dog had recently been affected by paralysis from a tick bite.
In children, ataxia and weakness are the first signs of tick bite, which can progress to bulbar palsy and respiratory depression. Headache and visual disturbance can occur in adults.4 Ticks have a predilection for embedding in the scalp, body creases and orifices. The facial nerve is the most reported nerve palsy due to ticks embedding in and around the ear.1,5–7
All ticks (regardless of the stage of lifecycle) crawl onto vegetation and wait for passing hosts. Adult ticks are more common in summer, but all stages can occur at any time of the year. Bandicoots and wallabies are the major reservoir hosts. The initial bite is usually painless, with patients noting a hard pruritic lump 24 hours later.
Ticks should be removed with fine curved forceps without squeezing the body of the tick. Stretching of the skin can facilitate grasping the mouth parts, which can result in a foreign body reaction if retained. The application of topical chemicals to aid removal is considered ineffective. It is prudent to search for more ticks if one is detected. A scabicide cream such as crotamiton will kill ticks in situations where removal is impractical, such as in extensive infestation. The itch usually settles after 2 days but local swelling tends to be more prolonged.4
Ticks can also transmit Queensland tick typhus (Rickettsia australis) which manifests with a black eschar at the bite site, localised lymphadenopathy, transient generalised macular rash, fever, headache, myalgia and sometimes pneumonitis or encephalitis. It is treated with doxycycline. Prevention by way of protective clothing and insect repellent is the best measure against tick bite.4
Lyme disease is a tick borne infection (Borrelia burgdorferi) common in the northern hemisphere, with symptoms similar to tick typhus together with an erythema migrans rash. Despite possible clinical cases being reported, there has been no confirmation that the disease occurs in Australia.3,8
Allergy, including anaphylaxis, can occur as a result of tick bite.3
Conflict of interest: none declared.
References