Coronary artery disease (CAD) affects over 600 000 Australians and is implicated in approximately one in 5 deaths. Coronary angiography is the gold standard for identifying CAD, although it is invasive and not without risk of complication. Cardiac stress testing is useful in the risk stratification of chest pain; noting that 15–39% of angiograms performed are normal.1,2
Cardiac stress testing includes stress electrocardiography (ECG) – also known as exercise stress test (EST) – and stress echocardiography. A detailed discussion of other tests for the noninvasive assessment of CAD, such as nuclear stress testing or computerised tomography (CT) coronary angiography, is beyond the scope of this article.
When should cardiac stress testing be ordered?
The main reason for cardiac stress testing is the risk stratification of known or possible CAD. The annual risk of cardiovascular mortality can be quantified from stress test results by measures such as the Duke treadmill score (low risk equating to <1% per year cardiovascular mortality, high risk >5% per year cardiovascular mortality). Other indications include work-up for potential cardiac causes of dyspnoea (noting dyspnoea can be a cardiac equivalent symptom of CAD), and evaluation of the effects of exercise on valvular dysfunction, pulmonary pressures or arrhythmia (eg. chronotropic incompetence), as well as risk assessment in the postinfarct, preoperative or high risk patient populations. There are advantages and limitations to each of the different testing modalities for the evaluation of myocardial ischaemia (Table 1).
| Table 1. Cardiac stress test cost, performance, advantages and disadvantages1,3,5,6 |
| Stress test |
MBS rebate $ |
Sensitivity % |
Specificity % |
Advantages |
Disadvantages |
| Electrocardiography (EST) |
149 |
68 |
70-77 |
- Assessment of exercise capacity
- Cost effective
- First line test in absence of contraindications
|
- Lowest sensitivity of all stress tests: risk of false negative test
- Lower diagnostic accuracy in women
|
| Echocardiography (exercise) |
310 |
80-85 |
84-86 |
- Assessment of exercise capacity, cardiac structure/function
- No radiation
- High specificity
|
- False negatives in single vessel/circumflex territory ischaemia (increased sensitivity with cycle ergometry)
|
| Nuclear perfusion study |
449-834 |
85-90 |
70-75 |
- Exercise capacity can be assessed
- High sensitivity
|
- Radiation
- False positives due to higher sensitivity/ diaphragmatic attenuation
|
| CT coronary angiogram |
700
(Requires referral from specialist or consultant physician) |
85-90 |
64-90 |
- High negative predictive value (especially in low to intermediate risk subjects)
|
- Radiation
- Functional effect of stenosis not usually assessed, nor exercise capacity
|
| Coronary angiogram |
522-900 |
-100 |
-100 |
|
- Invasive
- Radiation
- Functional effect of stenosis not routinely assessed
|
| MBS = Medicare Benefits Schedule |
Are there any contra-indications to testing?
Absolute contraindications to cardiac stress testing include acute myocardial infarction (including the presence of new left bundle branch block [LBBB]), high risk unstable angina, symptomatic severe aortic stenosis, uncontrolled arrhythmia causing symptoms or haemodynamic instability, unstable heart failure, acute pulmonary embolus and acute aortic dissection.3
What are the precautions?
Relative contraindications include left main coronary stenosis, severe arterial hypertension, electrolyte abnormalities, hypertrophic obstructive cardiomyopathy and uncontrolled arrhythmia.3 In the presence of a relative contraindication the test may still proceed if the benefit of identifying ischaemia outweighs the risk of performing the test.
It is important to ensure that the appropriate stress modality is ordered: if patients cannot walk at a reasonable workload, order an imaging pharmacological stress test (eg. dobutamine stress echocardiogram or persantin nuclear stress test), noting that a stress ECG cannot be done on its own using pharmacological stress.
Where does cardiac stress testing fit clinically?
Stress testing is most valuable in patients of intermediate pretest probability (10% < pretest probability <90%), as it is in this group that a change in risk stratification is most likely, ie. to low or high risk. It is not unreasonable in some patients with high pretest probability (eg. typical angina in men aged >50 years or in women aged >60 years) to consider coronary angiography as an initial diagnostic test.
As stress ECG should not be ordered when the baseline ECG shows a complete LBBB, paced ventricular rhythm, pre-excitation syndrome (Wolf-Parkinson-White syndrome), or more than 1 mm ST segment depression (eg. associated with left ventricular hypertrophy or digitalis effect). In these cases, ischaemic ECG changes cannot be identified and an imaging stress test should be considered.
What are the risks?
Although the test is generally safe, there is a small risk of acute myocardial infarction (~1:5000 tests) and death (~1:10 000 tests).4 Patients need to consent to this risk.
Are there any special requirements?
Withholding rate-controlling medications such as beta-blockers is standard practice before stress testing (withhold the night before and morning of the test for twice daily beta-blocker, and the morning of the test for once daily beta-blocker); 85% of maximal predicted heart rate (MPHR = 220 bpm – age) must be achieved for the test to be diagnostically accurate. The decision to withhold medicines must be tailored to the individual patient's risk of rebound hypertension, ischaemia or tachyarrhythmia.
What do I tell my patient?
Before the stress test you will be connected to a 12-lead ECG and a baseline ECG recording will be performed (Figure 1). If you are undergoing a stress echocardiogram, a baseline echocardiogram (ultrasound) will also be performed to assess the structure and function of your heart. A staff member will discuss your medical history before the test and measure your resting blood pressure. It is useful to bring your medications (or a list of your medications) on the day of the test.
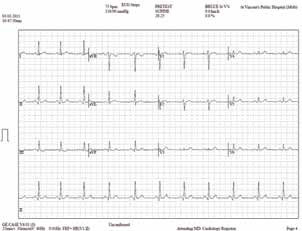
Figure 1. Pretest electrocardiogram
The stress test usually involves walking on a treadmill, although some centres use a stationary bicycle. If you are unable to exercise, a pharmacological (medication) stress test will be arranged that mimics the heart's response to increasing levels of exercise.
The treadmill (or bicycle) will start on a low incline at a slow speed and will usually increase in incline or speed every 2–3 minutes (the Bruce protocol is most commonly used in treadmill stress testing: it commences at 2.7 km/hr on a flat slope and increases every 3 minutes in speed, incline or both). Your ECG and blood pressure response to exercise are monitored during the test. It is important to report any symptoms during the test to the supervising doctor.
The test will continue until you reach your maximum level of exercise, although it can be terminated at any stage if you experience chest pain, dizziness, shortness of breath or concerning signs are noted on ECG or blood pressure analysis.
In the standard EST, the ECG is continuously monitored during exercise, and then for a period after exercise (usually 5–10 minutes), as important signs may be elicited during the recovery period.
In stress echocardiography, a baseline echocardiogram is performed, and then the stress test is undertaken followed by an immediate poststress echocardiogram (Figure 2). It is essential to take the poststress images quickly as the heart rate usually recovers rapidly (the maximum time in the standard imaging protocol is only 90 seconds). The team performing the test will encourage you to move rapidly from the treadmill to the bed for this reason.
A Medicare rebate may be available (Table 1).
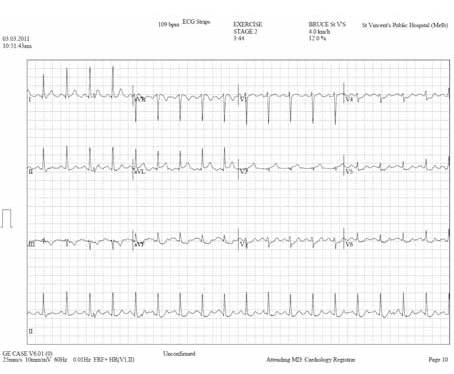
Figure 2. Peak stress electrocardiogram
At stage 2 of the Bruce protocol (3 min 44 seconds into the test), there is significant horizontal ST depression (~2 mm) in leads V4–V6, down-sloping ST depression in leads aVF and III, and ST elevation in aVL and aVR (~1 mm). These findings are highly predictive of ischaemia
How does the test work?
Coronary ischaemia is caused by a mismatch between supply (coronary blood flow) and demand (myocardial oxygen consumption) as workload increases. This is commonly caused by coronary stenosis. Cardiac stress testing works on the principle of demonstrating inducible ischaemia as workload increases (either through exercise or pharmacological stress). A reduction in blood pressure with exercise is one of the most significant signs of ischaemia.
Stress ECG identifies ischaemia if horizontal or down-sloping ST depression of ≥1 mm at 80 m/sec after the J-point is induced with exercise.
Stress echocardiography assesses the ECG response to stress as well as obtaining an immediate poststress echocardiogram to assess for inducible wall motion abnormalities as a marker of ischaemia. The cardiologist will analyse the pre- and post-images to assess for alterations in wall motion based on a standard 17-wall segment model.
What do the results mean?
The report should include an indication for the test and may comment on medications (particularly heart rate lowering medications) taken on the day of the test.
The results should describe the exercise protocol used, the exercise capacity in terms of time and workload achieved (protocol level, workload in watts or metabolic equivalent [METs] achieved), the haemodynamic response to stress (baseline and maximum blood pressure), at what heart rate and at what percentage of maximum heart rate the test was ceased, for what reason the test was ceased, presence of left ventricular hypertrophy or inducible ischaemia (in terms of ST segment shift or wall motion abnormalities on echocardiography), presence or absence of arrhythmia and heart rate response during recovery. The report may also comment on chronotropic incompetence and oxygen saturation during the test. An example of a stress echocardiogram report is shown in Figure 3.

Figure 3. Example of a stress echocardiogram report
Metabolic equivalent is a multiple of basal oxygen consumption, which is 3.5 mLO2/kg/min, and is the most robust assessment of exercise capacity as it is standard between the different forms of stress and protocols used. There is a very low risk of a cardiac event (<1% per year) if seven METs are achieved for men or five for women.
A stress echocardiogram report may additionally comment on the effect of exercise on valvular function (eg. degree of stenosis or regurgitation), pulmonary pressure, inducibility of outflow tract gradients (obstruction) and cardiac shunting.
What won't the results tell you?
Stress ECG and stress echocardiography are functional tests, they cannot state a percentage of coronary stenosis (as commonly reported in CT coronary angiography). While stress echocardiography can imply which artery may be stenosed, stress ECG does not specify which coronary artery is the culprit vessel.
What are the next steps?
Depending on the clinical scenario, a positive EST or ESE may be an indication for cardiology referral to consider coronary angiography or optimise medical therapy for coronary artery disease (Figure 4, 5).
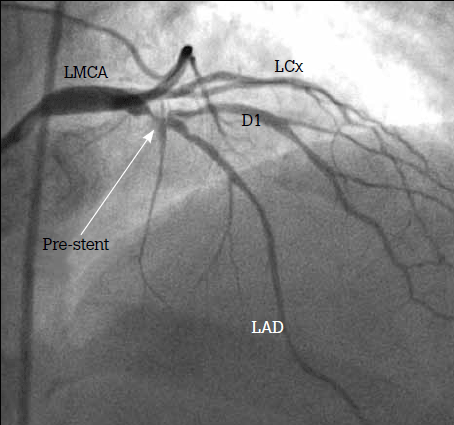
Figure 4. Angiogram showing severe bifurcating stenosis involving the proximal LAD and its first diagonal branch
LMCA = left main coronary artery; LAD = left anterior descending artery; LCx = left circumflex artery; D1 = first diagonal branch of the LAD
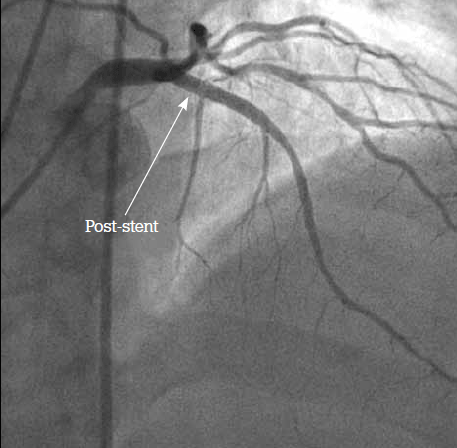
Figure 5. Angiogram postangioplasty. Successful insertion of 3.5 x 23 mm drug eluting stent to the proximal LAD. Some residual plaque at the origin of D1 was accepted as flow down this side branch was normal
A negative test may be reassuring, although is not conclusive, as no stress test has 100% sensitivity. If the clinical scenario does not correlate with the negative stress test, a repeat test, alternative imaging modality or coronary angiogram may be indicated.
The presence of an inconclusive test is most commonly due to submaximal heart rate achieved (eg. due to beta-blockade) or intermediate ECG changes (eg. T-wave changes without ST segment shift). This usually leads to a repeat stress test without the rate retardants, or an alternative modality to noninvasively assess ischaemia. Sometimes an inconclusive test with a good clinical history leads directly to a coronary angiogram.
Summary
Stress testing is a cost effective method to identify significant myocardial ischaemia due to CAD. In most cases, exercise stress testing will be sufficient, however in some cases, a stress echocardiogram using either exercise or pharmacological stress may be more appropriate. Results should always be interpreted in the context of the patient's clinical history.
Resource
The Cardiac Society of Australia and New Zealand: www.csanz.edu.au.
Conflict of interest: David Prior has received funding for lectures, consultancy and travel from Servier, Boehringer Ingleheim, CSL, Merck Sharp & Dohme and Sanofi Aventis.
References