The clinical symptoms, signs and investigation findings of MFF include fever, chills, myalgia, chest pain, nonproductive cough, metallic taste in the mouth, leucocytosis, headache and malaise. These clinical features are similar to those caused by respiratory viruses such as influenza or the common cold, which are seen frequently in general practice and can be misdiagnosed if an occupational history is not taken or the differential diagnosis not considered.2 Symptoms present within 48 hours of exposure and resolve by 1–2 days. Symptom recognition and occupational history taking are keys to making a diagnosis.
Chronic respiratory disease is the fourth (in men) and sixth (in women) leading cause of death in Australasia.3 Repetitive exposure to metal fumes has been correlated with the development of occupational asthma in welders.4 There has also been an association with a small reduction in lung function with chronic exposure.5 Episodes of MFF, although self limiting, may be the first warning sign in individuals who have poor safety prevention practices at home or in the workplace and may ultimately predispose them to developing chronic respiratory disease. Theories of pathogenesis relate to release of cytokines causing pulmonary and systemic inflammatory reactions, and others suggest an allergic response.6
In 2009, there were 554 calls regarding MFF to poison centres in the United States of America.7 Of these, one-quarter were treated in a healthcare facility with minor to moderate symptoms in the majority of exposures. Epidemiological characteristics of MFF in Victoria and Australia are not well described.
This study aimed to retrospectively review MFF related calls to the Victorian Poisons Information Centre (VPIC) in order to better understand the prevalence, severity and pattern of clinical toxicity related to MFF in Victoria.
Methods
Study design
This study was a retrospective case review of data from the VPIC database (a purpose-designed electronic database). Information is added to the database in real-time by poison information specialists.
The VPIC is located in the emergency department of the Austin Hospital in Melbourne, Victoria. It receives approximately 40 000 calls related to poison exposures in Victoria per annum. Calls for advice regarding MFF come from a range of individuals, including the person affected, their family or carer, and nursing and medical staff.
Ethics approval for use of this data was obtained from the Austin Health Human Research Ethics Committee.
Inclusion/exclusion criteria
Data from the VPIC call database were included in the study. For inclusion, a call must have been received between June 2005 and December 2010 (inclusive) and have an exposure and symptoms consistent with the diagnosis of MFF. There are no widely accepted diagnostic criteria for MFF. Criteria used by VPIC are outlined in Table 1. Calls not related to poisoning (eg. unrelated symptoms, no recent metal fume inhalational exposure, other diagnosis more likely) were excluded. Calls regarding patients of all ages were included.
| Table 1. VPIC diagnostic criteria for metal fume fever |
History of exposure to metal fumes within previous 48 hours
AND
Febrile illness OR respiratory symptoms PLUS at least one symptoms of:
- malaise
- myalgias
- arthralgias
- headache
- nausea
AND
Other illnesses less likely to be cause of symptoms |
Case search strategy
The VPIC database was interrogated using the terms 'metal fume fever' and 'MFF' to identify cases. The narrative description of the call for each case identified was then accessed. Calls not meeting the inclusion criteria were excluded. Electronic pre-formatted case reports were generated for each case identified. From these, data was transferred manually to the study database and subsequently analysed using Microsoft Excel® (version 12).
Data points collected
For each VPIC case meeting the inclusion criteria, the following data was extracted:
- date and time of call
- gender
- age group (adult, child, elderly)
- designation of the caller (patient, family, carer)
- metal type, activity, route of exposure, time since exposure
- Symptomology and Poisoning Severity Score (PSS)8
- advice given.
The PSS is an overall evaluation of the patient's symptoms at the time of the call, taking into account the most severe clinical features.
All data in the VPIC database is de-identified. The only demographic data recorded is patient gender and age group (adult, child, elderly). No potentially identifiable data (for either patient or caller) is recorded (eg. name, date of birth, address, hospital record number). Hence, it was not possible to trace any data back to an individual patient or caller.
Most data are reported descriptively with 95% confidence intervals fitted around point estimates. EpiCalc® (version 1.02) was used for all statistical analyses.
Results
Of the 90 calls, 85 cases met the inclusion criteria. The majority of these were male (n=82, 96%), compared with female (n=3, 4%). Eighty-four (99%) of the cases involved adults and one (1%) involved an adolescent who had been soldering while at school. There were no exposures in children or elderly people (>65 years of age).
Eighty-one (95%) of calls reported symptoms occurring within 24 hours of metal fume exposure. Three (5%) of these calls were about repeated exposures at work, hence symptoms lasted longer. Forty-five (53%) exposures occurred in the workplace, 39 (46%) included a mix of home welders and workshops, and as described above, there was one exposure at school.
Most symptoms occurred on Mondays (n=20, 24%) and Tuesdays (n=18, 21%). Sunday had the least number, three (4%) (Figure 1).
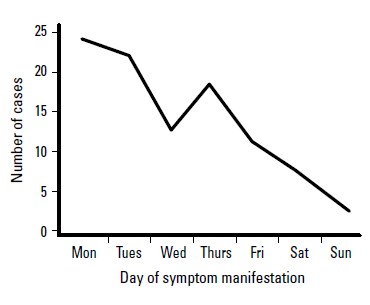
Figure 1. Number of cases per day of symptom manifestation
The most common symptoms were fever, chills, headache and myalgia (Table 2).
| Table 2. Symptoms from calls relating to metal fume fever |
| Symptom |
Number of cases (%) |
Fever
Chills
Headache
Myalgia
Malaise
Cough
Nausea
Abdominal discomfort
Dyspnoea
Paraesthesia tongue |
51 (60)
25 (29)
23 (27)
19 (22)
14 (16)
11 (13)
11 (13)
8 (9)
8 (9)
1 (1) |
All of the callers had inhaled fumes while welding metal. The most common metal involved was zinc (40% of known cases) (Table 3).
| Table 3. Metals reported in calls relating to metal fume fever |
| Metal |
Number of cases (%) |
| Zinc |
26 (31) |
| Steel |
15 (18) |
| Iron |
12 (14) |
| Aluminium |
8 (9) |
| Cadmium |
4 (5) |
| Type not specified |
20 (23) |
In 48 (56%, 95% CI: 43–65%) of the calls, advice was given that the patient need not seek medical attention unless the symptoms got worse or did not resolve. Individual preventive advice was given at the time of the call. Five cases (6%) were referred to a hospital or a general practitioner for further evaluation of symptom severity, such as worsening respiratory symptoms. Ten (12%) calls were about patients already in hospital and 22 (26%) were at their GP's practice. The majority (n=78, 92%) of patients had minor symptoms, five (6%) had moderate symptoms and two (2%) were asymptomatic by the time the call was made.
Twenty-seven (32%) of the callers identified were family, followed by self (n=25, 29%), doctors (n=22, 26%), nurses (n=6, 7%), friends (n=4, 5%) and ambulance paramedics (n=1, 1%).
Discussion
Metal fume fever was reported in a male majority in this study and all were related to inhalation of metal fumes following welding. The large percentage of occupational exposures highlights the importance of workplace safety and prevention. This includes the use of mask respirators, better workplace ventilation and education of employees about the disease. The possibility of developing chronic lung disease from repeated metal fume exposure, heralded by MFF presentations, means the medical profession has a role in prevention via education. In addition, MFF can occur at home in the garage or at school in class, meaning a wide range of individuals may be affected.
Metal fume fever symptoms were reported by over 35% of shipyard welders during the Monday cross-shift in a study by Kilburn.9 Our study supports the increased incidence of MFF at the start of the week, in keeping with the term 'Monday morning fever'. Acute tolerance develops during daily exposure and the weekend away from work contributes to the syndrome's reoccurrence when welding is recommenced on a Monday. One theory of tolerance is that metallothionein protein synthesis is induced, which binds heavy metals and prevents accumulation.6
In most cases, metal fume fever symptoms were present within 24 hours of exposure, as reported in other studies.6 Fever or chills were present in 81% of callers compared to 91.8%10 and 13.1%4 in two studies that looked at welding related MFF. People are seen with a spectrum of symptoms, the commonest being fever in our study, however, there is variability. In addition, callers may have gone on to develop fever and other related symptoms. A clinical diagnosis based on a combination of symptoms, metal exposure, exposure time and resolution increases the likelihood of a diagnosis of MFF. A differential diagnosis including occupational asthma needs to be kept in mind.
Zinc is the commonest metal involved in MFF. This was found in our study and has been recognised in others.11 Steel (an iron/carbon or other metal alloy), then iron were the next two most frequently reported metal reported in our study. The metal type involved was not specified in just under a quarter of cases, but is not essential in making the diagnosis.
The large proportion of minor PSS scores meant that half of the callers were advised they could stay at home, while the other half sought medical attention. Symptomatic care including bed rest, antipyretics, oral fluids, removal from exposure and in certain cases oxygen, is all that is required in acute presentations.
Limitations of this study
The VPIC data only related to calls to the poisons centre and does not reflect all MFF exposures in Victoria in the study period. Calls record symptoms at that particular time, hence people may have developed other symptoms at a later time. Also it is acknowledged that this condition can sometimes be undiagnosed, hence under-reporting is an issue and the incidence of the disease is likely to be higher than reported. On the other hand, clinical examination and evaluation could not be done to rule out other diagnoses, reflecting the nature of a poisons information service.
Conclusion
Enquiries to VPIC regarding MFF are relatively rare, but do occur despite modern workplace practices. Calls were most common at the beginning of the week, reflecting the previously described phenomena of increased symptoms occurring after a period of nonexposure (loss of tolerance). Metal fume fever can go unrecognised by the patient or medical practitioner as a flu-like illness and, because of its general spontaneous resolution of symptoms within 48 hours, treated as such. An occupational history and knowledge of the condition are crucial for a diagnosis to be made.
Key points
- Metal fume fever is a diagnosed with exposure to metal fumes within the last 48 hours and 'flu-like' symptom development with resolution within 1–2 days.
- Metal fume fever is most likely to present on Monday due to loss of tolerance over the weekend in occupational welders.
- Medical profession and patient awareness are crucial to aid diagnosis and help prevent occurrences at home, school and the workplace.
- Repeated MFF presentations may indicate poor workplace practices and ultimately lead to development of chronic respiratory disease.
Conflict of interest: none declared.
References