The recognition of the benefits of providing a coordinated multidisciplinary approach has been highlighted in the National Palliative Care Strategy, which has coordinated models of palliative care as a primary focus.5 Case conferences have been shown to be associated with maintenance of higher mean performance status in people with a life limiting illness compared to those who did not have a case conference (average daily Australian Modified Karnofsky Performance Status Scale [AKPS], 54% vs 46%, p=0.0106) and a reduction in the number of hospitalisations (1.07 vs 1.65, p=0.0317).6
This article reports on a substudy of a larger trial of case conferences in southern Adelaide (South Australia) that occurred in a palliative care setting. The larger trial was designed to identify ways to maximise the effectiveness of care coordination activities that occurred within palliative care and two types of care coordination; case conferencing and care planning that comprised general practitioner management plans and team care arrangements (TCA).7 The substudy aimed to describe the content and process of case conferences, focusing on information exchanged, cues given, questions and responses and roles within the conference including leadership. Findings from the leadership analysis have been described elsewhere.8
Methods
Study participants
Adult patients referred to the palliative care service were eligible to participate in the larger study. Patients who did not live in the region, those expected to die within 48 hours or who withheld consent were excluded. Patient and GP consent were required for enrolment in the study.
The primary study was a cluster randomised control trial where the unit of randomisation was the GP's practice. This was chosen to avoid GPs within one practice being allocated to different interventions and potentially influencing behaviours of their fellow practitioners, possibly randomised to the other arm. Practices were randomised to provide either a care plan or a case conference followed by a care plan. Randomisation was undertaken by an independent administrative officer using a computer generated random number sequence using block sizes of four. Due to the nature of the intervention, blinding was not possible.
Case conferences
A comprehensive case conference kit was developed at the beginning of the study based on previous work9 derived from documentation produced by The Royal Australian College of General Practitioners (RACGP). The kit conformed to Medicare Australia's requirements for reimbursement.
The conference was timed to coincide with the patients' functional status declining to AKPS 60 or less. This threshold was based on previous work, which found that the benefit of a case conference was significantly greater for people at or below AKPS 60.6 This threshold is where people require some help with the activities of daily living.
The case conference was arranged by the research officer in consultation with the GP and palliative care nurse assigned to the patient and minimally comprised the patient and/or their caregiver, the patient's GP, palliative care nurse and the palliative care consultant. Other participants could include health practitioners such as a registered nurse from a residential aged care facility or community based allied health workers.
Analysis
All case conferences were audiotaped and transcribed for qualitative and interaction analyses. The transcripts were read repeatedly and coded by three independent, experienced researchers.
Two separate analyses were undertaken. Interaction analysis was employed to allow quantitative coding of information transfer, interactions between participants and key themes that arose during the case conferences. Two interaction analysis systems were used. CanCode,10 which was developed in Australia to capture interactions between cancer patients and doctors, was adapted in this study for the context of palliative care case conferences, and emotional cues and responses which were coded using a system based on earlier work with people with cancer.11
CanCode comprises two parts: micro-analysis of speech and macro-analysis of consultation style and affect. Units of speech change when a person stops speaking. Each unit of speech receives three codes while audiotape and transcript are consulted: 'source' (eg. patient, carer, palliative care nurse); 'content' (eg. history of condition, current symptoms and concerns, end-of-life issues); and 'function' (eg. disclose, inform, express feelings). Codes are entered into a database for summative coding. The total units of speech emitted by each participant is calculated as a proxy of time spent talking. Total units of speech spent discussing each content category and function are also calculated. These are averaged across case conferences to provide a picture of typical interactions and used to explore systematic differences between conferences. This system has been shown to be valid and to have good inter- and intra-rater reliability.10
Emotional cue coding assesses the relational atmosphere of consultations by coding patients' and carers' emotional expression, their strength (weak, moderate and strong) and degree of empathy given by health professionals in response (ignored or delayed response, content responded to only, content responded to and empathy expressed). The average level of empathy over all cues is calculated.
Coder training for this study was provided by one author (PB) who developed and validated the coding systems. Coders coded a number of transcripts and discussed discrepancies until resolution was reached and the main coder coded the full set of transcripts. One author (PB) coded a random five consultations at the end of the coding to establish inter-rater reliability.
This study was approved by the Repatriation General Hospital Ethics Committee.
Results
Of the 52 people who consented to the primary study, 29 were randomised to receive a case conference and 21 conferences were held. Three patients died before a conference could be held, three patients became too unwell to participate and two GPs withdrew their consent to participate. Of the 21 case conferences held, 17 transcripts and documents were available for analysis as four conferences had technical difficulties with recording equipment.
Participant demographics
The median age of participants was 73 years (range 41–85 years); most were married and had completed some level of high school edcuation (Table 1). The demographics of people in the substudy were similar to those of the primary study population.
Table 1. Patient demographics
| | Total sample N=52 | Individuals receiving a case conference N=17 |
|---|
Age (years)
Mean
Median
Range
Standard deviation |
69.9
72
41–89
11.5 |
67.4
73
41–85
12.9 |
Gender (%)
Male
Female |
58
42 |
53
47 |
Marital status (%)
Never married
Widowed
Divorced/separated
Married/de facto |
3
11
9
77 |
6
12
6
76 |
Level of education (%)
Year 8 or less
Some high school
Completed Year 12
Some university
Completed university
Postgraduate qualifications
Trade certificate
TAFE
Missing
Other |
11
47
17
3
7
3
6
5
3
1 |
6
65
6
6
18
0
0
0
0
0 |
Characteristics of the case conference
All case conferences included the GP, patient and/or family member(s). A palliative care representative was present at every case conference: a consultant at 11 of the 17 (65%) conferences and a palliative care nurse at 15 of the 17 (88%) conferences. The number of participants at the conferences ranged from five to eight.
The length of the conferences ranged 20–58 minutes with a median time of 36 minutes. The main trigger for a conference was a review based on performance status reaching a predetermined threshold. Rapid patient deterioration was the trigger for five conferences.
The meetings were chaired by either the GP, consultant, another health professional or palliative care nurse.
Interaction analysis
The proportion of words spoken by each participant is shown in Figure 1. The patient, GP and palliative care consultant spoke the most, with carers next. Palliative care nurses, though present more often than palliative care consultants, spoke less. Almost half of the conference was spent discussing management of physical concerns (Figure 2). Psychosocial concerns were rarely discussed, although management of psychosocial concerns was discussed nearly as commonly as management of physical concerns. Prognosis, end-of-life issues and previous experiences of death and dying were rarely discussed.
The proportion of total units of speech spent discussing each function area is shown in Figure 3. The largest proportion of time was spent informing and educating participants.
Patients gave on average 2.9 emotive cues (range 0–9). Carers gave on average 2.1 cues (range 0–6). Cues were often in reference to feeling exhausted, sad about the patient's condition or worried about the future. The most common response to an emotive cue was to respond to the content by providing information; empathic responses were given only after a quarter of cues.
Key findings from the interaction analysis are listed in Table 2.
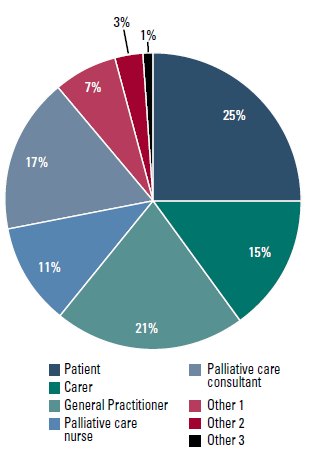
Figure 1. Mean percentage of total words spoken by each participant
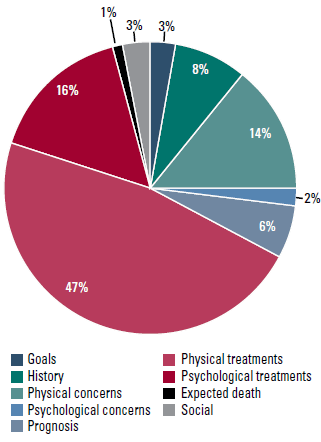
Figure 2. Average proportion of total units of speech spent discussing each content area
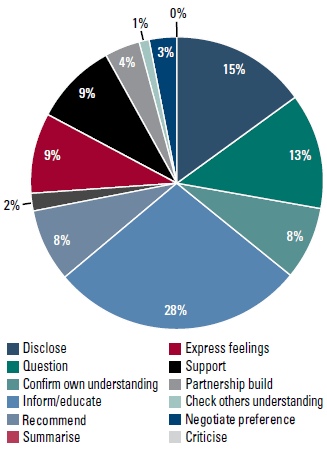
Figure 3. Average proportion of total units of speech talking within each function area
Table 2. Key findings from the interaction analysis
| Management of physical concerns was a dominant focus for each case conference (45%) |
| Management of psychosocial concerns was less common (15%) |
| Patients/carers expressed emotional issues relatively rarely |
| Discussion of prognosis and end-of-life issues were rare |
| Healthcare professionals tended to respond to the content of patient concerns, but not the emotion |
| Leadership of the case conferences tended to be medical but this was not explicitly negotiated and there was uncertainty regarding roles within the case conference that required clarification during the case conference |
| Health professional participants rarely summarised information or checked that patients and carers had understood the information provided |
Discussion
Information exchange versus care coordination
Case conferences have been shown to be an effective mechanism for increasing communication.12–13 However, while information exchange is an important aspect of clinical care, in this study it dominated the care coordination activities reducing the amount of time available for coordinating a plan of care for the patient. Often the GP did not have recent clinical information about the patient and requested further information.
The effectiveness of case conferences could be improved significantly if all participants were provided with a summary of recent clinical history (including tests, medications, involvement of other healthcare services and current or future needs) beforehand. This could reduce the need to 'bring everyone up to speed' as a major component of the conference. Potentially, the summary could be tailored to the needs of each participant. The ability to provide summary documents has cost implications as it relies on someone producing and circulating the document. This person should have ready access to all relevant information. From a logistical perspective this would most likely be the palliative care nurse.
Emotive cues
The expression of emotive cues in the case conference was not common. This lack of emotive cues is similar to other oncology studies,11 but a little lower than a previous study of patients seeing a nurse for chemotherapy education.14 Within the transcripts, discussions regarding prognosis and end-of-life issues were rare. It is likely that some participants may not have felt comfortable discussing intimate and emotional topics with a larger group of people. Patients and carers may not be the only people who feel uncomfortable discussing emotive topics, a concern given evidence that responding to emotive cues is a crucial factor of a successful conference.15
Within the transcripts, the response of health professionals to emotive cues usually involved providing information rather than empathy. Providing information can be an effective way of blocking further expressions of emotion. In a study of genetic counselling it was found that if the first emotional cue expressed by the patient was not responded to with empathy, the patient was significantly less likely to show further emotion.16 Legitimising the place of emotion in the case conference and training staff in empathic responses may be an important way to improve the utility of these meetings.
Involvement of patients and their families
The presence of the patient and carer at the case conference enabled their perspectives to be included in the discussion. Previous work has demonstrated the effectiveness of including the patient and/or family in case conferences.7,8,17A qualitative study on people who had experienced a stroke and families at the end-of-life experiences found an increased need for communication between patients, families and healthcare providers.18 Word counts from the transcripts showed that patients spoke on average slightly more than the other participants. This contrasts with a similar study conducted in oncology consultations, which found that discussion was dominated by the oncologist.19 Despite the complexity of many discussions, health professional participants rarely summarised information or checked that patients and carers had understood the information provided. This may be an avenue for further training and support.
Study limitations
Twenty-nine participants were randomised into the intervention, however only 17 case conferences were available for analysis. The high rate of drop-out is common for studies in palliative care and needs to be factored into the design of any study in a palliative care population.20 Importantly, the two methods of analysis produced similar outcomes and it appears that thematic saturation occurred. Future larger studies would be needed to explore outcomes quantitatively.
This study was undertaken at a single site in southern Adelaide that has over 1200 patients referred per year, more than 80% of whom have cancer. This service spans both metropolitan and peri-urban populations and may not reflect all other services. Each service should consider its own needs and populations.
Study strengths
Audiotaping and coding the case conferences provided rich data that has not been reported in many other studies examining case conferences. Most studies to date have focused on quantitative aspects to examine effectiveness which may not capture the complexity of the issues involved in care coordination. The themes discussed, how those themes are addressed, or, in some cases, ignored, allows recommendations to be made on the conduct and effectiveness of the case conference.
Implications for policy
Benefits of care coordination have been demonstrated in a number of studies.21 Patients are able to maintain their functional status for a longer period of time while reducing the number of hospitalisations. Effective implementation of care coordination within palliative care requires focus on case conferences within the broader policy framework of care for people at the end-of-life. Changes are required within each palliative care service to make care coordination part of the routine care they provide to their patients.
Implications for general practice
This substudy provides insights into case conferences for people with a life limiting illness and can inform palliative care services wanting to conduct case conferences. The analysis suggests a number of ways in which the case conference process could be improved.
A large proportion of the conferences were spent providing information to participants to ensure that all participants were fully aware of the current issues. One strategy that may maximise the efficiency of the case conference is to provide prior information to participants.
Future research directions
This study highlights the need for tailored information to be provided to people involved in the case conferences before the conference, along with training in effective communication. Future research is needed to evaluate the effectiveness of such strategies to ensure that case conferences move from an information transfer exercise to a care coordination activity. More research is needed to determine what training model should be used and the target audience for that training model.
Conflict of interest: none declared.
Acknowledgements
The authors would like to thank all the GPs, patients and families who generously agreed to participate in this study. The authors also thank the trial staff who recruited participants into the study and all the community palliative care nurses and consultants involved in the trial for organising and participating in the case conferences.
Funding
This study was funded by the Palliative Care Branch of the Australian Government Department of Health and Ageing under the Local Palliative Care Grant Program (Round 4).