Prior to the commencement of the service outlined in this article, access to primary healthcare, let alone specialists, was very limited in the Cape York Peninsula region. As a consequence, the capacity to manage both acute illness and chronic disease in children in this area was extremely limited. In particular, any significant paediatric health issue required referral to the closest hospital with paediatric support, which was 800 km away. This was less than ideal as it meant a long time away from the community with additional stress on carers, who had to leave other children behind.
Cape York Paediatric Outreach Program
The Cape York Paediatric Outreach Program was established in 1994, with the aim of addressing some of the health needs of children living in the remote communities of Cape York Peninsula. In particular, the program aimed to increase the capacity of local clinics to manage acute medical problems and to facilitate the management of chronic disease within the community where possible. The program covers an area of more than 140 000 square km (larger than England) and extends from the Daintree Rainforest, west to the Gulf of Carpenteria and north to Torres Strait. This area comprises the traditional lands of more than 20 language groups and many languages in the region remain strong, including Guugu-Yimidiir, Kuku-Yalanji and Wik Mungkan.
In the early 1990s, Dr Clive Hadfield, a general physician, pilot and former director of medicine at Cairns Base Hospital, established an outreach program to deal with problems of chronic disease management in the adult population in the remote communities of the Cape York Peninsula. In 1994, Dr Richard Heazlewood, a rural general practitioner with extensive paediatric experience, and Patsy Bjerregaard, a paediatric occupational therapist, joined Dr Hadfield on clinic runs, thereby establishing the Cape York Paediatric Outreach Program.
Priorities for the clinic include follow up of children recently discharged from hospital and timely assessment of children with concerns regarding respiratory disease, developmental delay, failure to thrive or hearing loss, without the need for families to travel long distances. In addition, clinics are able to monitor children with rheumatic heart disease via a portable echocardiogram and provide assessment and therapy from a paediatric occupational therapist and other allied health professionals.
The clinic takes a team based approach to the healthcare of children in the communities, with many people involved in the care of a child. This includes parents, grandparents, educators, allied health workers, Indigenous health workers, the department of child safety and local clinic staff. Where possible, the clinic arranges regular case conferences with local staff, the outreach team and educators to update one another on the progress of high-needs children and to coordinate services.
Health promotion activities are also an important part of the role of the clinic. These include education sessions on the effects of smoking and alcohol on the developing fetus and the establishment of the first ‘mums and babies’ centre within a remote community. The importance of fighting for the needs of children in remote communities at a policy level was also recognised by the clinic team. They have been successful in bringing the health of children in the region to prominence within the national media2 and the government, including submissions to the Federal Senate Select Committee on Regional and Remote Aboriginal Communities and the Queensland cabinet.
Improving access
Community support
Community support is essential to the success of the Cape York Paediatric Outreach Program. When the program began, time was invested in engaging community leaders, local councils and men’s and women’s groups to outline the aims of the program and to encourage a whole of community approach to child health. Providing a regular and continuous service over years, which treats each family with dignity and respect, has helped to strengthen this trust.
Essential equipment
In general, everything that may be needed at a clinic must be flown in with the team. The most important piece of equipment is a laptop, as well maintained records are invaluable in following the treatment of children with complex care needs. Records are stored in a central database located in Cairns and a lot of work is done updating the records to ensure they contain a brief summary of significant diagnoses, hospital admissions, the results of investigations and current medications. This enables children’s records to be easily followed if they move communities and if they are admitted to hospital. The software is run in mobility mode to avoid the problems that arise from a poor (or absent) internet connection. Luckily, new technologies mean that we are rarely stranded without an appropriate reference resource. The clinic takes a range of reference books within its tablet or Smart phone.
The program also brings many educational aids on clinic runs. Patsy Bjerregaard and the Paediatric Outreach Team introduced the use of educational dolls to demonstrate the effects of tobacco,3 alcohol and drug4 use in pregnancy (Figure 1 and 2). The rheumatic heart disease program also provides DVDs and other educational material to help children and families understand their condition (Figure 3).

Figure 1. Patsy Bjerregaard, paediatric occupational therapist demonstrating the effects of smoking on a fetus with the ‘Smokey Sue Smokes for Two’3 doll
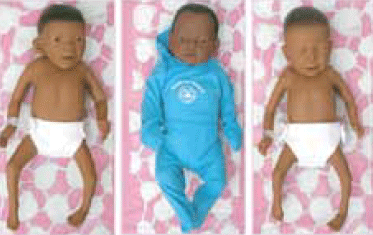
Figure 2. Educational dolls used within the clinic: showing effects of fetal alcohol syndrome (left), healthy doll (centre) and showing effects of exposure to drugs in the womb (right)4

Figure 3. Lisa Smith, an RFDS child health nurse and author Dr Jason Agostino show a patient educational material about rheumatic heart disease
Staffing
Retention of staff within remote communities has long been a difficult issue. Indigenous health workers and child health nurses are essential for the identification of at-risk children and engaging them to attend the clinic. Over the past decade a fly-in, fly-out (FIFO) model of healthcare has proven to be an effective way of maintaining staff and increasing services, with the Royal Flying Doctor Service (RFDS) increasing the provision of FIFO general practitioners and child health nurses who work in communities during the week. This model has been associated with a low turnover of staff. The RFDS is now providing one or two child health nurses within each community. The model is now being exported to underserviced regions outside Cape York with Doomadgee and Mornington Island now visited by Cairns based RFDS staff.
While FIFO healthcare has been effective, the ideal is for locally based staff. In the opinion of the authors, significant improvements in child health can come from training community members to be Indigenous child health workers and ongoing support is required for the creation of education and career pathways in this area.
Medication delivery
The regular administration of medication is an issue within this population. This applies to both acute infections and chronic diseases. To tackle this issue, the program always looks for the least demanding medication regimen for a given illness. Bicillin injections can be offered for presumed streptococcal infections or else antibiotics that can be given twice daily, such as amoxycillin, cephalexin and cotrimoxazole are preferred. For chronic conditions it has been shown that twice weekly supervised dosing of iron is more effective in the treatment of anaemia, than daily unsupervised dosing in remote Indigenous communities.5 In congenital hypothyroidism supervised weekly dosing of thyroxine has been shown to be effective and safe6 and has been used when other methods have failed.
Resources
References
- Australian Bureau of Statistics 2006. Table generated 22 Feb 2012 using 2006 Census of Population and Housing: Local government area by Indigenous status and age 10 year age groups. Data cube: Excel Spreadsheet. Available at www.abs.gov.au/ CDataOnline.
- Koch T. Packs to give indigenous infants a good start. The Australian 2008; 21 July.
- Smokey Sue Smokes for Two. Health Edco-Mentone Educational. Available at www.mentone-educational.com.au. Image reproduced with permission.
- Realityworks® Experimental learning technology. Available at www.realityworks.com. Image reproduced with permission.
- Kruske SG, Ruben AR, Brewster DR. An iron treatment trial in an aboriginal community: improving nonadherence. J Paediatr Child Health 1999;35:153–8.
- Grebe SK, Cooke RR, Ford HC, et al. Treatment of hypothyroidism with once weekly thyroxine. J Clin Endocrinol Metab 1997;82:870–5.
- Northern Territory Government. Child growth charts in the Northern Territory: discussion paper. Darwin: Department of Health and Community Services, 2008.