Case
A previously healthy woman, 22 years of age, presented to her general practitioner (GP) with a small, painless ulcer of 1 cm in diameter on her right ankle, which had developed after she expressed a small pustule at that site a few weeks earlier. She could not recall any preceding trauma or insect bite. She travelled extensively throughout Australia for work, but remained exclusively in urban areas of major cities. Her only other travel of note in the previous year was an overnight holiday on the Mornington peninsula in Victoria four months prior to presentation.
Routine wound swabs showed scant polymorphs and grew mixed coagulase-negative Staphylococci. There was no clinical response to courses of oral cephalexin and dicloxacillin. The ulcer slowly enlarged – four months after her initial presentation it was 2 cm in diameter, had extended to muscle and suddenly became painful (Figure 1). This prompted referral to a plastic surgeon. Surgical debridement to healthy tissue was performed (Figure 2) and a vacuum-assisted closure (VAC) dressing applied. Histopathology demonstrated necrotising non-granulomatous inflammation associated with numerous acid-fast bacilli. The diagnosis was confirmed on polymerase chain reaction (PCR) testing.
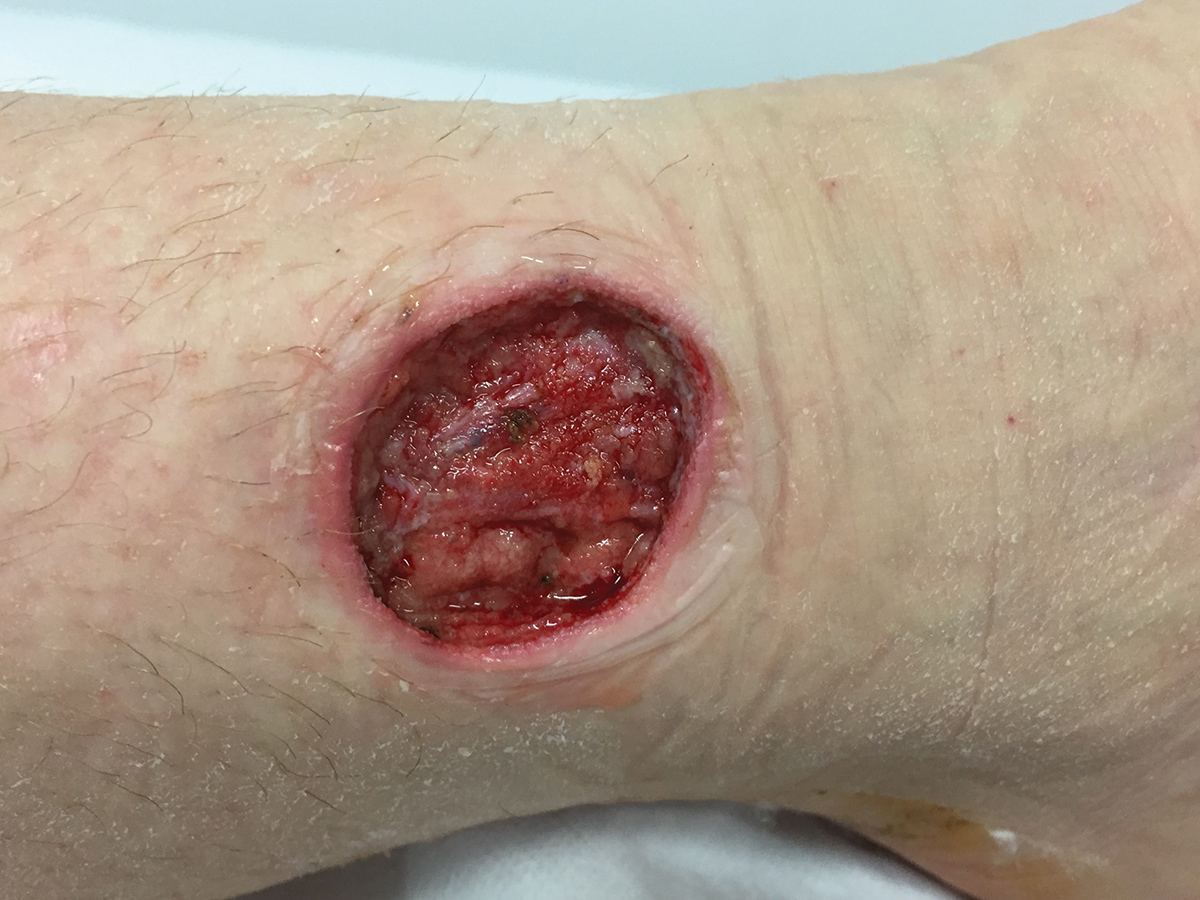
Figure 1. Ulcer four months following initial presentation
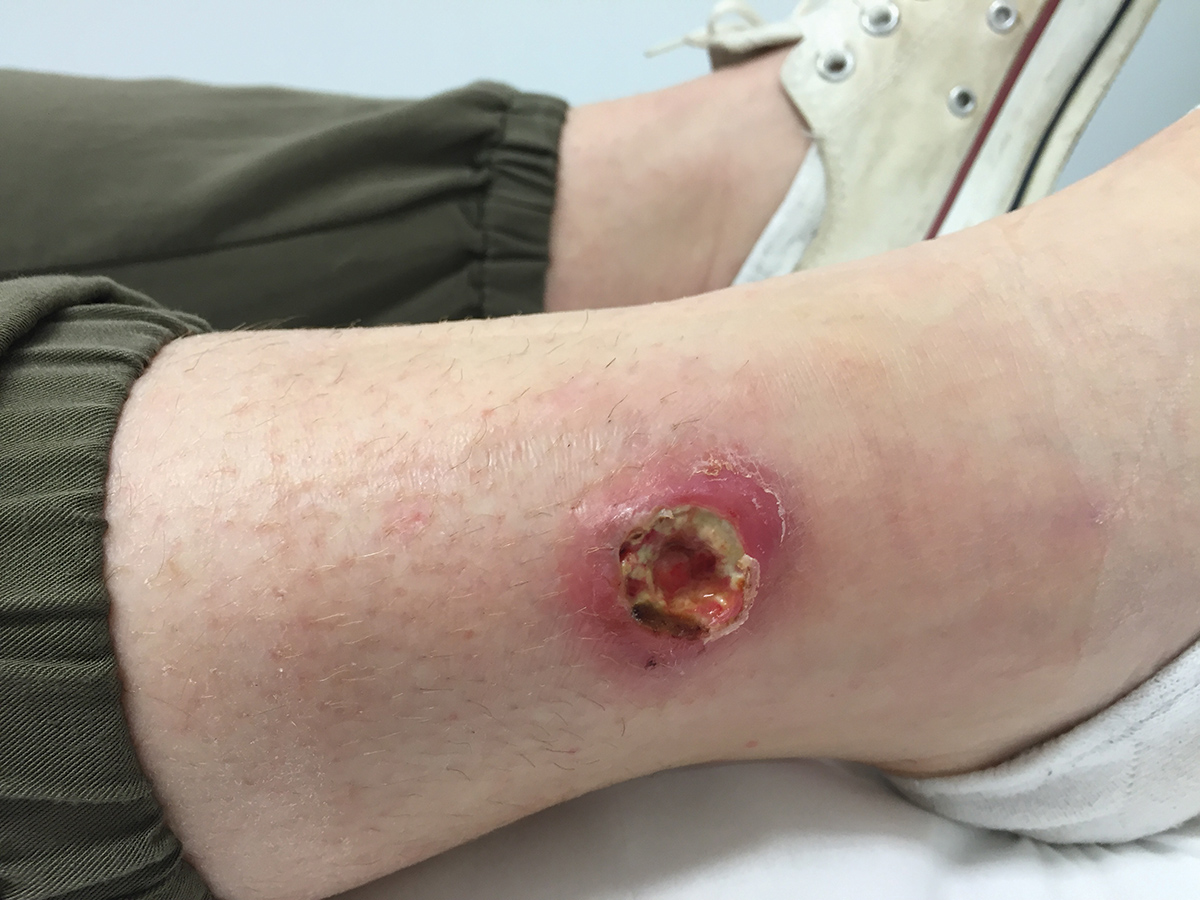
Figure 2. Ulcer following surgical debridement
Question 1
What is the diagnosis?
Question 2
How has the epidemiology of this condition changed in Australia in recent years?
Question 3
Why can this condition be difficult to diagnose?
Question 4
Do all cases with this condition require surgery?
Answer 1
The patient has Buruli ulcer, a destructive skin and soft tissue infection caused by Mycobacterium ulcerans. In Australia, the condition is also known as ‘Bairnsdale ulcer’ and ‘Daintree ulcer’. It usually manifests as an ulcer but can also present as cellulitis, a plaque or nodular disease. Differential diagnoses for a painless ulcer include venous ulceration, or squamous or basal cell carcinoma; however, these are unlikely in an otherwise healthy young patient.
Answer 2
Buruli ulcer is a geographically restricted infection that occurs only among residents or visitors to specific endemic areas. It is most common in sub-Saharan Africa; however, cases have been reported from more than 30 countries.1 In Australia, the two major endemic regions are coastal Victoria and a small segment of Far North Queensland near Mossman.2 In Victoria, sporadic cases are linked to East Gippsland and Phillip Island. However, the major endemic regions are the Bellarine and Mornington peninsulas, with the disease now encroaching into some south-eastern bayside suburbs of Melbourne.3 Recently, Victoria has witnessed a significant increase in cases of Buruli ulcer, from an annual average of 30 cases between 2001 and 2010, to 100 cases between 2011 and 2016. A record high of 182 cases were notified in 2016.4 Although the exact mechanism of transmission to humans is incompletely understood, it has been proposed that, in Victoria, possums may act as environmental reservoirs and biting insects as vectors.5
Answer 3
Buruli ulcer can be difficult to diagnose as M. ulcerans will not grow on routine wound cultures. Additionally, the growth of skin flora that are merely colonising a wound may falsely suggest an alternative diagnosis. Buruli ulcer has an average incubation period of 4.5 months (range 2–9 months).6 The long incubation period together with the fact that as little as one hour in an endemic region is enough to potentially become infected – meaning that patients may present with symptoms long after their relevant exposure – hinders diagnosis. Buruli ulcer can be rapidly and accurately diagnosed by a PCR test from a wound swab;7 however, this test must be specifically requested.
Answer 4
Historically, most cases of Buruli ulcer were managed surgically, and surgical excision of small lesions can be curative, as in this case. However, antibiotics are highly active against M. ulcerans and reduce the risk of relapse. Many patients are now managed medically with an eight-week course of rifampicin combined with clarithromycin,8 although paradoxical, inflammatory reactions9 and adverse drug reactions10 may complicate antibiotic treatment. Surgery may also assist healing through removal of necrotic tissue and repair of large skin defects.
Case continued
The patient’s wound healed well with the assistance of VAC dressings; no skin graft was required. Adjuvant antibiotic therapy, which reduces recurrence rates of Buruli ulcer, was discussed with the patient; however, this was decided against, given her good surgical outcome and an imminent extended overseas holiday.
Key points
- Buruli ulcer is a destructive skin and soft tissue infection endemic to select coastal regions of Australia. There is a current outbreak in Victoria; major endemic foci include the Bellarine and Mornington peninsulas and some south-eastern bayside suburbs of Melbourne.
- Buruli ulcer has a prolonged average incubation period of 4.5 months, and the diagnosis is frequently delayed even after patients present with symptoms.
- Clinicians should consider requesting a PCR test for M. ulcerans on a wound swab in patients with lesions suggestive of Buruli ulcer who have travelled to an endemic region in the preceding year
- Antibiotics, such as rifampicin plus clarithromycin, are increasingly used as first-line therapy for Buruli ulcer; however, surgery can still play an important role.
Authors
Michael J Loftus MBBS, Infectious Diseases Registrar, Department of Infectious Diseases, Austin Health, Heidelberg, Vic; Project Officer, Victorian Department of Health and Human Services, Melbourne, Vic. michael.loftus@austin.org.au
Robert J Gates MBBS, FRACS, Plastic Surgeon, Department of Plastic and Reconstructive Surgery, Royal North Shore Hospital, St Leonards, NSW
Simon Crouch BA, MBBS, MA, MPH, PhD, FAFPHM, Senior Medical Advisor, Victorian Department of Health and Human Services, Melbourne, Vic
Brett Sutton MBBS, MPHTM, FACTM, MFTM, FRSPH, Deputy Chief Health Officer, Victorian Department of Health and Human Services, Melbourne, Vic
Paul DR Johnson MBBS, PhD, FRACP, Infectious Diseases Physician, Department of Infectious Diseases, Austin Health, Heidelberg, Vic; Professor of Medicine, Department of Microbiology and Immunology, The University of Melbourne, Parkville, Vic
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.
Authors’ note
The Victorian Department of Health and Human Services became aware of this case in the course of routine follow-up for a received notification of M. ulcerans infection, a mandatory notifiable condition in Victoria.