Atopic dermatitis, also known as atopic eczema, affects a large proportion of children and is most common in infants, where it occurs in 20% of those under two years of age.1–3 Over the past 30 years, a twofold to threefold increase in paediatric atopic dermatitis has been reported.2,4 Most children develop atopic dermatitis before the age of two years.5 Significant morbidity associated with atopic dermatitis can be prevented with early diagnosis and treatment.6
Two main theories have been proposed to explain atopic dermatitis – the skin barrier and immunological hypotheses. The immunological hypothesis focuses on an imbalance in T-helper cells such that there is a predominance of Th2 cells rather than Th1. This results in an increase in immunoglobulin E (IgE) through a pathway involving activation of interleukins.7
In the skin barrier hypothesis, atopic dermatitis is associated with filaggrin gene mutations. Filaggrin is a protein important in maintaining the integrity of the epidermis by binding keratinocytes together. Skin barrier dysfunction occurs if there is a defect in filaggrin, which leads to water loss from the skin. As the skin becomes drier, allergens enter more easily, resulting in allergic sensitisation.5,7,8
Atopic dermatitis can present in many different forms and, as such, the differential diagnoses are broad and can include contact dermatitis, impetigo, urticaria, scabies, psoriasis and seborrhoeic dermatitis.7 It is important to consider these diagnoses before a diagnosis of atopic dermatitis is established.
A complication of untreated atopic dermatitis can include eczema herpeticum. Eczema herpeticum is a dermatological emergency, particularly in children under two years of age, and needs urgent referral to an appropriate paediatric service for review and management. Eczema herpeticum can have serious sequelae such as eye or meningeal involvement resulting in scarring.2,9
Management
Atopic dermatitis is best approached with a good understanding of general and specific measures that can be undertaken to manage and prevent the condition. It is sensible to discuss with parents of children with atopic dermatitis that at the outset, atopic dermatitis is a chronic condition with periods when it will flare; the aim of treatment is complete clearance between flares.
General measures
General measures are important to prevent atopic dermatitis and lessen exacerbations. The following basic principles have been suggested:3
- avoiding environmental aggravators such as chlorine, sand and grass, and washing immediately after coming into contact with these
- wearing loose, cotton clothing and avoiding overheating
- having soap-free washes
- having short showers (two to three minutes is recommended)
- avoiding hot showers or baths; tepid water is preferred.
Effective and regular use of emollients has been found to decrease the need for topical corticosteroids.7 Emollients hydrate the epidermis by providing an occlusive layer and reducing evaporation. Effective emollient regimens are the mainstay of atopic dermatitis management.
Specific measures
Specific measures are best thought of in two distinct categories – anti-inflammatory and anti-infective measures. First-line anti-inflammatory management in the treatment of eczema is a topical corticosteroid.
The three most common formulations of topical corticosteroids for the treatment of dermatological conditions are lotions, creams and ointments. It is important to appreciate the characteristics of each in order to prescribe the most appropriate treatment.10
Lotions contain a high proportion of water, a small amount of oil and are not as hydrating as creams or ointments. They are less useful in the management of eczema and are more beneficial in providing cooling or drying effects.10
Creams predominantly contain water with an oil component. The aqueous phase evaporates readily, and the oil and medicament are absorbed into the skin. Creams can cause stinging in patients with atopic dermatitis as the water component evaporates. They are good for moisturising if the skin is not particularly dry or irritated.10
Ointments are the most appropriate option when the skin is very dry. They are effective at maintaining the skin barrier and preventing dehydration. They are much less irritating than other preparations and are more effective at delivering active ingredients into the skin. Ointments consist mainly of oil mixed with a small amount of water. They are best applied when the skin is damp, such as after a shower or bath. Patients are often put off ointments as they are greasy, sticky and messy, but they can be very effective in increasing hydration and maintaining good skin integrity.10
Table 1. Topical corticosteroid ladder25,26
|
Mild (Class I)
Hydrocortisone 0.5–1%
Hydrocortisone acetate 0.5–1%
Desonide 0.05% |
Moderate (Class II)
Betamethasone valerate 0.02–0.05%
Triamcinolone acetonide 0.02%
Clobetasone butyrate 0.05%
Methylprednisolone aceponate 0.1% |
Strong (Class III)
Bethamethasone dipropionate 0.05%
Betamethasone valerate 0.1%
Triamcinolone acetonide 0.1%
Mometasone furoate 0.1% |
Very strong (Class IV)
Betamethasone dipropionate (ointment) 0.05%
Halcinonide 0.1% |
Atopic dermatitis should be treated with the right strength (Table 1), amount and formulation of corticosteroid, which will be determined by considering the child’s age, severity of atopic dermatitis and sites involved.9 High-potency steroids should be avoided in delicate areas such as the face, neck, axillae and groin, and avoided in children under one year of age.10 Topical corticosteroids should be used until the skin is smooth, feels like normal skin, and the inflammation and itch have settled. If treatment is ceased before the skin has returned to normal, it can ‘flare’. The fingertip unit (FTU) is a useful tool to educate parents about adequate amounts of topical corticosteroid to use (Table 2).
Table 2. Fingertip unit as measure of steroid required29
|
| Age | Leg/foot | Torso front | Torso back | Arm/hand | Neck/face |
|---|
| 3–6 months |
1.5 |
1 |
1.5 |
1 |
1 |
| 1–2 years |
2 |
2 |
3 |
1.5 |
1.5 |
| 3–5 years |
3 |
3 |
3.5 |
2 |
1.5 |
| 6–10 years |
4.5 |
3.5 |
5 |
2.5 |
2 |
|
Fingertip unit (FTU) can be a helpful way to determine the amount of steroid required. It is defined as the amount of steroid preparation squeezed from a tube that will fit along an adult’s index finger to the first crease. The table shows the ranges of FTU required for children aged three months to 10 years.
|
Antihistamines have no role in the treatment of pruritus in eczema. Sedating antihistamines can be helpful if sleep is grossly affected, but pruritus is best treated with topical corticosteroids.10
The risk of side effects when treating children with atopic dermatitis with topical steroids is minimal.7 However, side effects can include stretch marks, telangiectasia and thinning of the skin. An observational study of Australian children found no thinning of the skin in a study group that was compared with an age-matched control group not using topical corticosteroids. The mean treatment time was 10 months. Ninety-three per cent of the patients were using potent topical corticosteroids and the only side effect noted was mild telangiectasia.11 Systemic steroids are generally not recommended unless advised by a specialist dermatologist or immunologist.3
Occlusive dressings involve placing topical corticosteroid on the skin and covering with either a wet or dry dressing. This technique has been used for more than 20 years in the treatment of atopic dermatitis, despite little definitive evidence for its efficacy.12,13 There are many different techniques that have been recommended. Our practice for patient-administered or parent administered wet dressing treatment at home is to use a layer of corticosteroid under a wet layer of close fitting clothing for 15–20 minutes. For in-hospital treatment, we use wet towels in place of clothing. Inpatients at the Princess Margaret Hospital receive thrice daily wet dressings followed by emollient application. For convenience of the family, this is often reduced on discharge to once daily until clear, recommencing nightly if the atopic dermatitis flares.10,14 Dry occlusive dressings are usually reserved for small patches of thickened, lichenified eczematous skin resistant to conventional application of topical corticosteroids. It is suggested that occlusive dressings are only used for up to seven to 14 days.12,13
Many children with atopic dermatitis have frequent infective exacerbations, and Staphylococcus aureus is the most common pathogen isolated. There is a positive correlation between eczema severity and density of S. aureus culture obtained from swabs.15 Short courses of oral antibiotics are recommended if there is widespread infected atopic dermatitis, but there is no evidence that topical or long-term use of antibiotics is helpful in preventing atopic dermatitis.2 Obtaining swabs from affected skin and nares may be helpful to identify infection and direct further management.
In 2009, the only placebo-controlled, randomised, single-blinded study was conducted in the use of bleach baths to treat recurrent S. aureus infection in children with atopic dermatitis. This involved 31 children with previously infected atopic dermatitis who were randomised into groups after receiving two weeks of oral cephalexin prior to beginning the study.16,17 The treatment arm received twice weekly bleach baths plus mupirocin ointment into the nose twice daily for five consecutive days per month. The placebo group received the same frequency of plain water baths and had petrolatum in their nose under the same regimen outlined.
Overall, there was a significant reduction in severity and body surface area of skin affected by atopic dermatitis from baseline in the treatment group. There were no between-group differences in the severity of atopic dermatitis for areas that were not submerged in the bath (such as head and neck).16,17 The protocol for clinical use of bleach baths is outlined in Table 3.16,18 Twice-weekly dilute bleach baths are useful when managing children who have had recurrent infective exacerbations of atopic dermatitis. If staphylococcal carriage is identified in nasal swabs, staphylococcal decolonisation should be considered.19
Table 3. Bleach bath regimen18,27,28
|
For a bleach bath, you will need:
- 45 ml household bleach, 4% sodium hypochlorite (eg White King)
- Bath oil (2–3 caps full)
- 40 L lukewarm water (1/4 adult bathtub)
- Towels
|
Steps:
- Run a bath 1/4 full with lukewarm water
- Mix in the bath oil
- Add the bleach to the bath
- Allow child to bathe in the bath for up to 10 minutes
- Crusts on the skin can be gently soaked off during bathing
- Wash the head and face
- No need to rinse after the bath, gently pat dry and avoid rubbing the skin
- Apply moisturisers and prescribed creams or ointments
- If using topical steroids, apply them before moisturising
|
| Bleach baths are usually recommended twice per week |
Food allergies
Skin prick testing and food challenges are generally only helpful in severe cases of atopic dermatitis in which there has been a poor response to first-line treatment. A modest number of children can have a food allergy trigger. This is more common in infants and children with moderate or severe eczema.20–22 Three-quarters of all cases of food-induced atopic dermatitis are due to milk, egg, soy, wheat or peanut.22
Food elimination diets should only be conducted under the supervision of a medical specialist (clinical immunology or allergy specialist) in association with an accredited practising dietitian, as nutritional deficiencies may occur.22 If a child has a food allergy proven by oral challenge, an elimination diet may be appropriate, but ongoing management of atopic dermatitis should continue.23 Parents should be discouraged from starting elimination diets on their own. There is often a discrepancy between the food parents suspect is the atopic dermatitis trigger and the true allergen.22
Other treatment options
Topical calcineurin inhibitors are second line agents in the treatment of atopic dermatitis. They do not share the side effect profile of corticosteroids; however, there is a risk of immunosuppression. A common complaint in the use of pimecrolimus is burning or stinging on application.24 Tacrolimus has efficacy similar to moderate-to-strong topical corticosteroids and pimecrolimus has efficacy akin to a mild corticosteroid.7 In Australia, pimecrolimus is available as a cream, whereas tacrolimus needs to be compounded. Topical calcineurin inhibitors cost significantly more for the patient than topical corticosteroids. Application is usually twice daily.24
Phototherapy can be a useful adjunct in the treatment of chronic atopic dermatitis and should be administered under the guidance of a dermatologist. Its use is limited to older children as the child will be required to stand alone and unassisted in a phototherapy machine.
Systemic immunosuppression may be required in patients who do not respond to standard treatment. A number of systemic agents, such as cyclosporin, azathioprine and methotrexate, are used in the treatment of severe atopic dermatitis. Cases of atopic dermatitis resistant to first-line treatment may require specialist input.7
Conclusion
Although common and often mild, atopic dermatitis can be a challenging condition to manage (Figure 1). We recommend a stepwise approach and the combination of general and specific measures in order to gain control of this condition.
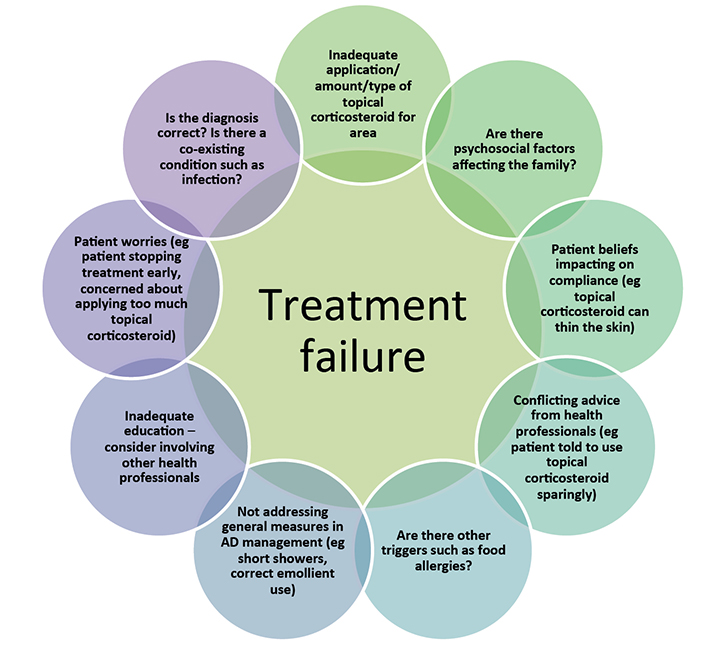 |
Figure 1. Common causes of treatment failure with topical corticosteroids6,30
Addressing these factors may aid in the management of atopic dermatitis. If management is still difficult, referral to a dermatologist or immunologist should be considered |
Authors
Sarah Strathie Page BSc, MBBS, Dermatology Registrar, Princess Margaret Hospital, Perth, WA. sarah.strathiepage@health.wa.gov.au
Stephanie Weston MBBS, FRACP, FACD, Consultant Dermatologist, Princess Margaret Hospital, Perth, WA
Richard Loh MBBS, FRACP, FAAAAI, FACAAI, Consultant Immunologist, Princess Margaret Hospital, Perth, WA
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.