Background
Service in the Australian Defence Force (ADF) can be physically and mentally demanding. A report on the mental health of current serving personnel found they had a similar prevalence of psychological problems as the general community, but the prevalence of specific psychological problems differed. For example, current service personnel were less likely to have an alcohol abuse disorder, but more likely to have post-traumatic stress disorder (PTSD) and depression.1 Other studies demonstrate that PTSD is managed at significantly higher rates among ADF veterans than in the general population in Australia.2,3 Veterans have also been shown to have higher rates of musculoskeletal problems associated with their occupational activities.4
The Department of Veterans’ Affairs (DVA) issues repatriation health cards (RHCs) to those who have served in the armed forces and are entitled to medical treatment for a range of reasons or are 70 years of age or older, and to the widows or widowers of service personnel. In 2015, there were 208,000 holders of an RHC,5 down from 269,000 in 2009.6 We can identify patients who hold an RHC from Bettering the Evaluation and Care of Health (BEACH) data and, for brevity, we will refer to them as ‘DVA’ patients.
Our aim was to compare the prevalence of lifestyle risk factors among, and the health problems managed in general practice for, DVA and non-DVA patients, particularly psychological and musculoskeletal problems. We also examined demographic changes among DVA patients at general practitioner (GP) encounters over time.
Method
We analysed patient encounters with DVA and non-DVA patients collected from April 2000 to March 2015 in the BEACH program. The methods of the BEACH program are described in detail elsewhere.7 For the management of problems with DVA patients, we examined the latest five years of BEACH data (April 2010 to March 2015). We used a linked sub-study of alcohol and tobacco use to compare hazardous drinking and daily smoking patterns.7 Hazardous drinking was defined using the Alcohol Use Disorders Identification Test-C (AUDIT-C) tool, which comprises the first three items of the World Health Organization’s (WHO’s) AUDIT.8 Patients were divided into three age groups: 18–54 years (which would include veterans who served in the Middle East and other recent conflicts), 55–69 (Vietnam era) and 70 years and older (Korea and earlier conflicts). The reason an age cut-off of 70 years and older was used is because all veterans in this age group are eligible for RHCs. We further analysed male and female patients separately.
Results
Demographic changes 2000–01 to 2014–15
BEACH data from April 2000 to March 2015 included information for 1,471,600 patient encounters, 43,493 of which were with DVA patients. There were 1,255,730 encounters with adult patients (aged 18 years and older), and 43,013 of those were DVA patients.
The proportion of all GP encounters that were with DVA patients decreased from a peak of 39 per 1000 encounters in 2003–04 to 21 in 2014–15 (Figure 1). The average age of DVA and non-DVA patients at encounters increased significantly across the study.
The average age of DVA patients rose from 75.7 in 2000–01 to 79.1 in 2014–15, and non-DVA patients increased from 42.8 to 48.5 years. The proportion of DVA encounters that were with males decreased significantly from 62.0% in 2000–01 to 50.9% in 2014–15. There was no significant change for non-DVA encounters.
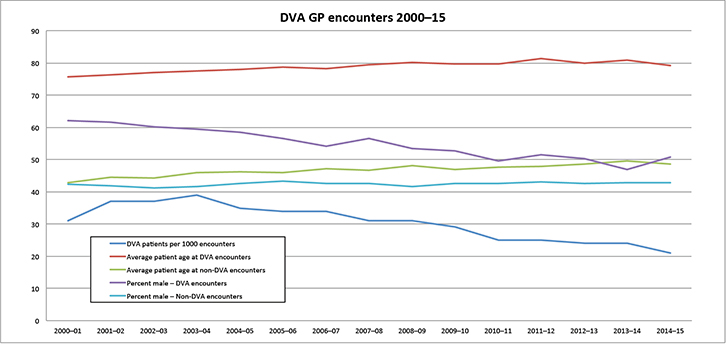 |
| Figure 1. Demographic changes in GP encounters with DVA patients 2000–15 |
Psychological problems 2010–15
Male DVA patients of all ages and female DVA patients aged 18–54 years had higher management rates of psychological problems than their non-DVA peers (Figure 2). Male DVA patients aged 18–54 years had a significantly higher rate of depression and a significantly lower rate of anxiety managed at their encounters than their peers. Male DVA patients of all ages had a significantly higher management rate of PTSD than their non-DVA peers.
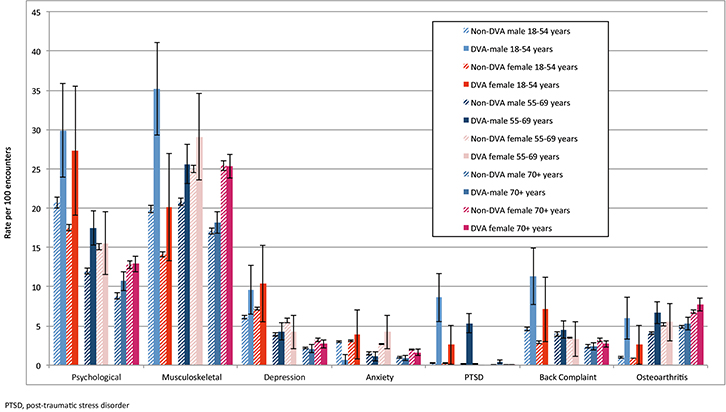 |
| Figure 2. Management rate of psychological and musculoskeletal problems in general practice, by age, sex and DVA status 2010–15 |
Musculoskeletal problems 2010–15
There was a significantly higher management rate of musculoskeletal problems in male DVA patients aged 18–69 years than in male non-DVA patients, but there was no significant difference between DVA and non-DVA patients for all other age and sex groups. However, both male and female DVA patients aged 18–54 years had significantly higher rates of back complaint management than their non-DVA peers. Osteoarthritis was managed at a significantly higher rate for male DVA patients aged 18–69 years than for their non-DVA peers.
Smoking and alcohol 2010–15
Across all age and sex groups, there was no significant difference between the proportion of DVA and non-DVA patients who were daily smokers (results not presented). Males aged 55–69 years were the only veteran age–sex group to have a larger proportion of ‘hazardous’ drinkers than their non-DVA peers.
Discussion
The results of our study support similar work by showing that DVA patients have significantly higher rates of psychological1–3 and musculoskeletal problems4 managed in general practice, especially among those in the 18–54 years age group. DVA patients aged 70 years and older were similar to their non DVA peers, with the exception of higher rates of PTSD in male veterans in this age group.
It is interesting to note that the problems managed for younger female DVA patients were similar to those of younger male DVA patients, but quite different from those among younger female non-DVA patients. By contrast, problems managed for older female DVA patients (aged 55 years and older) were not significantly different from older female non-DVA patients. A possible inference is that older female DVA patients are more likely to be widows of male cardholders and would be less likely to be former members of the ADF.
It is notable that among younger males, DVA patients had higher management rates of PTSD, whereas non-DVA patients had higher management rates of anxiety. It would be worthwhile examining whether the knowledge that someone is a veteran leads GPs to diagnose PTSD when similar symptoms in non-DVA patients may be labelled anxiety.
A previous study found that veterans had lower levels of alcohol abuse than non-veterans.1 Our study found no difference between DVA patients and non-DVA patients in levels of ‘hazardous drinking’, except for significantly higher rates among male DVA patients aged 55–69 years.
We found considerable differences between DVA and non-DVA encounters for those aged 18–69 years, but few for those aged 70 years and older. One reason for this is that 70 is the age at which all veterans are eligible for an RHC, and it is an age group for which conditions associated with ageing increase, providing uniformity of problems managed in DVA and non-DVA groups. For those younger than 70 years of age to be eligible for the card, they must fulfil certain criteria relating to their health, military service, means or specific conditions. The differences found in the veterans aged 18–69 years could therefore be linked to their eligibility for the card. For instance, DVA has recently expanded the eligibility to receive an RHC for veterans with a psychological problem. The DVA has encouraged early detection of these issues by GPs through the creation of a post-discharge assessment.9 Whether the significantly higher rate of psychological problem management in male veterans is due to having to meet this criterion or being in the ADF cannot be determined from our data.
Ideally, in future, the BEACH recording form would include an additional question to all patients asking whether they have served in the ADF at any time. This would allow us to investigate the health issues arising among service personnel (whether RHC holders or not) and compare them with those arising among patients who have not served in the ADF.
Authors
Christopher Harrison BPsych (Hons), MSocHlth, Senior Research Analyst, Family Medicine Research Centre, University of Sydney, NSW. christopher.harrison@sydney.edu.au
Janice Charles BA, MSc (Med), Senior Researcher, Family Medicine Research Centre, University of Sydney, NSW
Ying Pan BMed MCH, Senior Research Analyst, Family Medicine Research Centre, Sydney School of Public Health, Sydney Medical School, University of Sydney, NSW
Helena Britt BA, PhD, Director Family Medicine Research Centre, University of Sydney, NSW
Competing interests: None.
Provenance and peer review: Commissioned, externally peer reviewed.
Acknowledgements
We wish to thank the general practitioners who participated for their generosity. During the data collection period of this study, the BEACH program was funded by the Australian Government Department of Health, AstraZeneca Pty Ltd (Australia), Novartis Pharmaceuticals Australia Pty Ltd, bioCSL (Australia) Pty Ltd, AbbVie Pty Ltd, Sanofi-Aventis Australia Pty Ltd, Merck Sharp & Dohme (Australia) Pty Ltd, Pfizer Australia Pty Ltd, National Prescribing Service, GlaxoSmithKline Australia Pty Ltd, Bayer Australia Ltd, Janssen-Cilag Pty Ltd, Abbott Australasia Pty Ltd, Wyeth Australia Pty Ltd, Roche Products Pty Ltd, and the Australian Government Department of Veterans’ Affairs.