Septic arthritis in children is an orthopaedic emergency. Prompt diagnosis and treatment are critical in optimising patient outcomes. Mismanagement can lead to serious adverse outcomes, including systemic sepsis, cartilage destruction, growth plate damage and avascular necrosis of the femoral head (Figure 1).
Unfortunately, diagnosing septic arthritis is not always straightforward. Transient synovitis is a benign, self-limiting condition that mimics septic arthritis. Other less common orthopaedic conditions can also present in a similar fashion, and need to be excluded.
The purpose of this article is to provide an overview of the pathophysiology, diagnosis, treatment and long-term follow-up of septic arthritis in children.
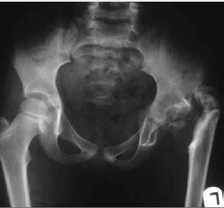 |
| Figure 1. AP pelvis X-ray demonstrating destruction of the left hip following septic arthritis |
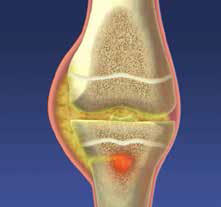 |
| Figure 2. Osteomyelitis of the proximal tibia leading to septic arthritis of the knee |
Pathophysiology
Septic arthritis involves bacterial infection of a synovial joint. Haematogenous bacterial spread is the most common cause of septic arthritis in children. Osteomyelitis of adjacent bones may also result in joint infection (Figure 2). This is particularly the case in joints where the metaphysis is intracapsular, such as the hip and shoulder. Direct inoculation via penetrating injuries or surgery can occur.
The incidence varies between studies, but septic arthritis has a predilection towards children under the age of 4 years. Septic arthritis occurs most commonly in the hip and knee joints.1 Other joints commonly affected include the shoulder and ankle, but septic arthritis can occur in any synovial joint in the body.
Staphylococcus aureus is the most common pathogen.2 Other causative organisms include group A Streptococcus and Enterobacter species. Haemophilus influenzae septic arthritis may occur in children who have not been vaccinated. The incidence of Kingella kingae septic arthritis is almost certainly significant but underreported because of its fastidious nature in culture.
Proteolytic enzymes released by host inflammatory cells and certain bacteria cause cartilage destruction. Growth plate damage and avascular necrosis of the femoral head are thought to be caused by ischaemia secondary to increased intracapsular pressure.
Differential diagnosis
A number of conditions can mimic septic arthritis in their presentation, making diagnosis difficult.
Transient synovitis is a benign, self-limiting condition that involves synovial inflammation and effusion formation. The condition is poorly understood but a viral aetiology is suspected. Although transient synovitis is more common than septic arthritis, given the serious nature of the latter condition, any child presenting with joint irritability should be considered to have septic arthritis until proven otherwise.
Osteomyelitis may also mimic septic arthritis in its presentation. Children may present with pain, limping and fevers. Ultrasonography is used to exclude a joint effusion suggesting contiguous septic arthritis. The diagnosis may be confirmed on bone scan.
Other differential diagnoses include trauma and tumours, and specific to the hip joint, Perthes disease and slipped upper femoral epiphysis (SUFE). These can generally be excluded radiographically. The child’s symptoms may also represent the first presentation of an inflammatory arthropathy or acute rheumatic fever.
Diagnosis in the general practice clinic
Children with septic arthritis generally present with an acute onset of joint pain, limited movement and fever. Limping or non-weight bearing is typical in lower limb joints. In subcutaneous joints, such as the knee or ankle, signs of an effusion including swelling and warmth may be noted. Clinical detection of an effusion in the hip or shoulder is not possible. The child will generally hold the joint in a position where the capsule is most lax. The knee will be held slightly flexed and the hip will classically be held flexed, abducted and externally rotated. Any passive movement of the joint is extremely painful.
Several studies have shown that a history of non-weight bearing and a temperature greater than 38.5°C are the most reliable clinical signs differentiating septic arthritis and transient synovitis.3–10
Any child presenting with symptoms and signs consistent with septic arthritis should be urgently referred to the emergency department (ED) of a hospital with an orthopaedic service. Antibiotics should not be administered before obtaining a synovial fluid sample for analysis. The child should be kept fasting.
For children in rural and remote settings where a significant delay to treatment is anticipated, urgent telephone advice should be obtained from the nearest orthopaedic service regarding the commencement of empiric antibiotics.
If a child presents with joint irritability or limping but no history of fever, a diagnosis of transient synovitis is more likely. They should be commenced on regular non-steroidal anti-inflammatory drugs (NSAIDs) and reviewed the following day. The parents should be instructed to present to an appropriate ED if the child develops a fever or deteriorates clinically. For ambiguous cases, or if there is any clinical concern, urgently refer the child to an appropriate ED.
Diagnosis in the ED
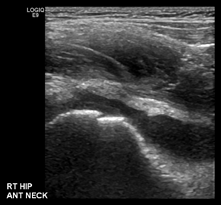 |
| Figure 3. Ultrasound of the right hip joint demonstrating an effusion |
In the ED, blood should be sent for a white cell count (WCC) and differential, erythrocyte sedimentation rate (ESR), C-reactive protein (CRP) and cultures. Several studies have shown that a WCC greater than 12.0 x 109 cells/L, ESR greater than 40 mm/hr and CRP greater than 20 mg/L are significantly more common in septic arthritis when compared to transient synovitis.3–10
X-rays of the involved joint and adjacent bones should be obtained to exclude other pathology such as fractures, osteomyelitis or tumours. In the hip, Perthes disease or a SUFE should be excluded radiographically. An ultrasound of the involved joint should be obtained (Figure 3). This is the most sensitive test for detecting a joint effusion.2
Any child with a concerning presentation, raised inflammatory markers and a joint effusion should be kept fasting and immediately referred to an orthopaedic surgeon. Again, antibiotics should not be commenced until a synovial fluid sample is obtained, unless advised otherwise by the surgeon.
At some institutions, synovial fluid aspiration can be attempted in the ED. Topical anaesthetic agents and/or nitrous inhalation can be used. The knee joint is easily aspirated without imaging, but other joints may require ultrasound guidance. Synovial fluid should be urgently sent for a cell count, Gram stain and microscopy, culture and sensitivities (MCS). Gram stain confirms the diagnosis of septic arthritis, but may only be positive in one-third of cases.11 A synovial fluid WCC greater than 50 x 109 cells/L is used in most studies to differentiate between septic arthritis and transient synovitis.3,5,6,8
The policy at our institution is not to attempt synovial fluid aspiration in the ED.
Children are taken to the operating theatre and synovial fluid aspiration is performed under general anaesthesia.
As mentioned previously, the diagnosis of septic arthritis is not always straightforward. Unless the diagnosis can be confidently excluded, one should proceed with treatment. The morbidity of a missed case far outweighs the morbidity of treatment.
Treatment
The treatment of septic arthritis involves urgent surgical drainage and lavage of the joint.2 This can be performed arthroscopically or via an open arthrotomy. In the paediatric setting, the knee and shoulder joints are often approached arthroscopically, whereas the hip and ankle joints are generally approached via an arthrotomy. In very young children, standard arthroscopic instruments are too large and, therefore, arthrotomy is generally performed.
Synovial fluid should be sent for a cell count, Gram stain and MCS. A synovial biopsy is also sent for MCS and histology. The joint is thoroughly lavaged with normal saline and a drain tube is left in situ. The limb is often immobilised post-operatively, either in a back slab or skin traction.
Once a synovial fluid sample has been obtained, high-dose, empirical, intravenous (IV) antibiotics are commenced. Unless contraindicated, flucloxacillin 50 mg/kg (max 2 g) IV every 6 hours is used.12 For patients with delayed penicillin hypersensitivity, cephazolin 50 mg/kg (max 2 g) IV every 8 hours is recommended. For patients with immediate penicillin hypersensitivity, vancomycin 30 mg/kg (max 1.5 g) IV every 12 hours is recommended.
Once culture and sensitivity results are known, antibiotic cover is adjusted accordingly, in consultation with the infectious diseases team. The causative organism is not always identified, in which case empirical treatment should be continued, depending on clinical response. A recent systematic review showed that a positive culture result was obtained in only 34–82% of cases.2
The drain tube is generally removed after 48 hours. IV antibiotics are continued until clinical improvement is seen and the inflammatory markers are normalising.1 For an uncomplicated case of septic arthritis, this generally occurs within 2 days. The child is then transitioned onto an appropriate oral antibiotic agent. Commonly, this will be flucloxacillin or cephalexin. Before discharge from hospital, one needs to ensure that the child is tolerating the oral antibiotic and that the parents are educated about the importance of regular dosing.
Follow-up
For an uncomplicated case of septic arthritis in a child, a 3-week course of oral antibiotics is generally sufficient.1 The child should be followed up with a clinical examination and repeat inflammatory markers 1 week after discharge and then 1 week after stopping antibiotics to ensure complete recovery.
Ongoing follow-up with an orthopaedic surgeon for at least 2 years is recommended to monitor for long-term sequelae of septic arthritis. These include cartilage damage, growth disturbance due to growth plate damage, and avascular necrosis of the femoral head. While these sequelae are rare, early diagnosis and intervention may improve long-term outcomes.
Key points
- Septic arthritis in children is an orthopaedic emergency that requires prompt diagnosis and treatment.
- Clinical diagnosis is based on a history of joint pain, non-weight bearing and fever.
- Any child presenting with these signs should be urgently referred to an appropriate emergency department.
- Differentiating between septic arthritis and transient synovitis can be difficult.
- Treatment involves surgical drainage and lavage of the joint, followed by an appropriate course of antibiotics.
- Long-term follow-up is necessary to detect sequelae of septic arthritis.
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.