Lymphangiectasia:
a diagnostic challenge for the general practitioner
Breast cancer usually requires surgery, lymphadenectomy and radiotherapy as treatment. In some cases, this may result in chronic lymphoedema in the involved arm. Many years later, different cutaneous lesions can arise over the lymphoedematous arm, which general practitioners (GPs) should be familiar with in order to rule out possible malignancies. Acquired lymphangiectases represent superficial lymphatic dilatations caused by a wide range of processes and they usually develop in association with chronic arm lymphoedema, which in turn is often secondary to breast cancer treatments that obstruct or destroy lymphatic drainage.1
 |
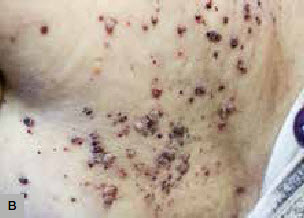 |
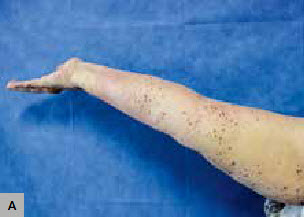
Figure 1. Multiple papules and vesicles
A. Multiple papules and vesicles over a chronic lymphoedema in the right arm
B. Vesicles with translucent and hemorrhagic content resembling frog spawn |
We report the case of a woman, 86 years of age, who presented with a 9-year history of multiple lesions arising over her right arm. Twenty-two years before, she had breast cancer, which was treated with a radical mastectomy, local radiotherapy and hormonal therapy. Since then, she had been suffering from chronic lymphoedema of her right arm, managed with a compressive bandage. On physical examination, multiple papules and vesicles of 2–10 mm with translucent and haemorrhagic content were located on the right arm and forearm, in some areas resembling frogs’ eggs (Figure 1A, B). A skin biopsy of one of the lesions showed an elevated epidermis above a group of ectatic lymphatics in the papillary dermis and the diagnosis of acquired lymphangiectases was made.
Lymphangiectases are benign tumours that can be either congenital or acquired and they tend to be stable and chronic. They can be recognised as translucent vesicles of several millimeters in diameter that can leak a clear fluid and are classically described as appearing like ‘frog spawn’ in some areas. Sometimes they can contain some blood. They occur mainly on the extremities and the genital area. They have been described in patients after lymphatic vessel obstruction, mainly due to surgery or radiotherapy, but are also related to arthrotomy, scarring from scrofuloderma and cellulitis, and they may appear in the genital region of elderly people.2 The aim of treatment is to reduce underlying lymphoedema and control infection. It is not necessary to treat them, although the use of electrocoagulation, cryotherapy, carbon dioxide laser, excisional surgery, sclerosing agent injection, physiotherapy and compressive bandages has been reported. Recurrences are frequent and prognosis is determined by the results of standard therapies.3
GPs should be aware of this entity in order to differentiate it from other conditions such as Herpes zoster infection, molluscum contagiosum and some malignant tumours, particularly angiosarcoma and lymphangiosarcoma, which are the most frequently occurring malignant tumours arising on lymphoedematous extremities.4 Diagnosis can usually be made by physical examination; however, if necessary, a skin biopsy can be performed to rule out malignant processes.
Dr Aejandro Lobato-Berezo
Madrid, Spain
Acknowledgements
Dr Aguilar-Martínez and Dr Fernández-Cogolludo
for their helpful advice
New oral anticoagulants and perioperative management of anticoagulant/antiplatelet agents
The recent article by Rahman and Latona (AFP December 2014)5 provides an excellent overview of the complex pre-operative assessment of patients receiving anticoagulant/antiplatelet therapies, when balancing the risks of perioperative stroke and myocardial infarct with that of haemorrhage.
This is certainly not an area for the unwary. Assessing risk requires expert knowledge across a range of clinical and pharmacological interventions along with detailed knowledge of the individual patient. Important factors include renal function, type of surgery and bleeding risk, history of invasive cardiac procedures, rationale for current drug treatment and target international normalised ratio (INR).
One of the problems I find as a GP is obtaining clarity regarding the location and type of prosthetic heart valve and the target INR. Another is getting information on the type of coronary artery stent and the need for ongoing antiplatelet therapy. Patients move around, GPs move on, notes are hard to trace and discharge summaries lack critical information. Assumptions may be made, errors can creep in and mistakes can be made. The consequences for the patient may, of course, be catastrophic.
I believe that clinical errors regarding target INR and duration of antiplatelet treatment may be more common than thought. Patients could help reduce such errors by wearing medic-alert bracelets, detailing the type of cardiac surgery and recommendations for warfarin and antiplatelet therapies. Cardiologists and cardiothoracic surgeons could also help by ensuring that discharge summaries include clear guidance on future management. I also feel GPs would welcome a summary table on the type and position of prosthetic heart valves, their associated risk of thromboembolism and, where indicated, the target INR.
Dr William Patterson, Shenton Park, WA
References
- Rahman A, Latona J. New oral anticoagulants and perioperative management of anticoagulant/antiplatelet agent. Aust Fam Physician 2014;43:861–66.
Marine envenomations
I used to have a practice 10 m from a beach and every summer 2–10 people, on average, would tread on a stingray and come limping in hoping for relief. This I would provide by immediately infiltrating the wound/s with lignocaine, preparatory to exploring the wound/s looking for the friable portion of the barb that was often left in the wound. The lignocaine gave immediate relief – I do not quite understand the apparent reluctance of Berling and Isbister, the authors of ‘Marine envenomations’ (AFP Jan–Feb 2015),6 to use it or only to use it down the track after ‘up to 90 minutes’ of soaking in hot water. Hot water only denatures the venom protein – the sulfhydryl bonds in the protein tend to be restored once the area is removed from hot water anyway, thereby restoring the protein’s original structure.
Dr L Anderson, Canberra
References
- Berling I, Isbister G. Marine envenomations. Aust Fam Physician 2015;44:28–32.
Reply
Thank you for your letter regarding our article, ‘Marine envenomations’. We recommend hot water first, as a simple non-invasive treatment and we agree local infiltration with lignocaine, when possible, is beneficial for wound infiltration and pain-relief. Lignocaine can be given as early after hot water as required, but hot water should not be used for longer than 90 minutes.
Dr Ingrid Berling
Emergency Staff Specialist and Clinical Toxicology Fellow
Clinical Toxicology and Pharmacology, Calvary Mater Hospital, Newcastle, NSW
Professor Geoffrey Isbister
Professor, Clinical Toxicology Reasearch Group
University of Newcastle, NSW