 |
 |
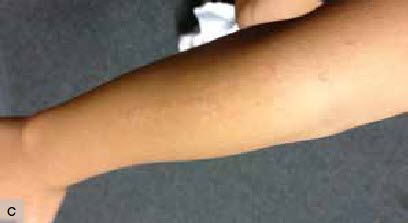 |
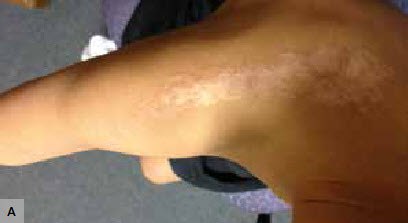
Figure 1. Skin rash
A. Distribution of the skin rash from the right scapula down the right arm
B. Close-up of the skin rash on the right upper arm
C. Extension of the skin rash down to the right forearm |
An Aboriginal and Torres Strait Islander boy, 5 years of age, presented to his general practitioner (GP) with a 5-week history of an itchy skin rash. It had commenced on his right scapula and moved in a linear distribution down his right arm. The initial area had become hypopigmented from scratching. The boy had a history of asthma, but no recent viral illness, interstate travel or other family members with skin issues. He had not previously been diagnosed with a dermatological condition. On examination, there were small linear papules that seemed to ‘track’ down his right arm and scratch marks were apparent.
Question 1
How would you describe the lesion in Figure 1 and what are the differential diagnoses?
Question 2
What is the name given to the embryological pattern reflected in this presentation?
Question 3
What causes the condition to occur?
Question 4
What is the management and prognosis of the condition?
Answer 1
Figure 1 show a unilateral, smooth topped and occasionally papular rash in a linear distribution extending from the scapula down the right arm. Areas of hypopigmentation are seen, consistent with resolution. Scratch marks consistent with pruritis are noted.
First described in the early twentieth century, lichen striatus is an uncommon, self-limiting linear inflammatory dermatitis characterised by pink, tan or hypopigmented, small flat-topped, scaly papules distributed in a linear configuration. The papules may coalesce into small plaques and into a continuous or interrupted band.1–4
Common differential diagnoses include:
- lichen planus
- lichen nitidus
- lichen simplex
- annular lichenoid dermatitis
- unilateral laterothoracic exanthema.
Answer 2
The lines of Blaschko represent pathways of epidermal cell migration and proliferation during fetal development and reflect the existence of cutaneous mosaicism.3 Lichen striatus is commonly unilateral, located on extremities (but can also occur on trunk) and can move in a proximal-to-distal direction.2
Answer 3
Lichen striatus most commonly occurs in children aged 5–15 years.5 It is usually diagnosed clinically and may require a biopsy in cases of uncertainty, although investigations and referral are often unnecessary. Histological findings show lichenoid, lymphocytic infiltrate with overlying epidermal acanthosis, dyskeratosis, hyperkeratosis, occasional parakeratosis and lymphocytic exocytosis.3
The aetiology remains largely uncertain, although a combination of genetic predisposition and environmental stimuli are thought to contribute.6 These include a history of atopy or a family history of atopy, an autoimmune response to inflamed T cells, or as a result of infection or trauma.1,2,5,7,8
Answer 4
The consensus is that lichen striatus is a self-limiting and benign condition, lasting from a few months to 2 years, before spontaneously regressing. Therefore, the role of therapy with topical steroids and non-steroidal anti-inflammatory agents in the treatment of lichen striatus is unclear.4 If topical agents are used, they would normally be for symptomatic management only (eg pruritis). A recent study did not note a reduction in the course of the disease with steroid therapy.9 Areas of hypopigmentation may be evident once resolution has occurred. Follow-up for reassurance can be useful, although recurrence is uncommon.
Outcome
At initial review, topical steroids were prescribed to assist in relieving symptoms. Dermatology review was arranged but financial stressors did not allow this to be undertaken. Instead, telephone advice and photographic review of the condition was sought from a local dermatologist, who confirmed the diagnosis. The young boy was reviewed 6 weeks later in the GP clinic and the lesion had all but resolved, with hypopigmentation evident in areas of lesion resolution.
Key points
- Lichen striatus is a benign, self-limiting skin condition.
- It is most often a clinical diagnosis that requires no investigation or management.
- Common differential diagnoses include lichen planus, lichen nitidus, lichen simplex, annular lichenoid dermatitis and unilateral laterothoracic exanthema.
- Clinical presentation and lesion location and appearance (along with histological findings if available) are the main ways to distinguish between diagnoses.
- Specialist referral is not always required.
Competing interests: None.
Provenance and peer review: Not commissioned, externally peer reviewed.