Most chronic wound care is now managed in the community rather than the hospital setting.1,4 Audits conducted in public health services in Australia and internationally show that inconsistencies in wound management practice and outdated methods of practice contribute to high costs and poor patient outcomes.3,5,6 Only a small number of international studies have assessed the factors contributing to wound care costs; most show nursing time as the major cost, whereas dressing materials contribute less than one-quarter of the total expenditure.5–8 However, much of this research was conducted in the public health service setting and may not translate to Australian general practice, where funding and delivery of care models differ substantially.
Australia’s universal health insurance scheme, Medicare, provides access to free treatment in public hospitals and free or subsidised treatment by selected health professionals outside of hospital, as outlined in the Medicare Benefits Schedule (MBS).9 At the time of this study, wound care was topical in Australian general practice owing to the announcement of plans to remove the fee-for-service item for nurse provision of wound care from the MBS. This study aimed to determine the cost of wound care in general practice by conducting an audit of current wound management practices, including an assessment of the major cost contributors.
Methods
This cross-sectional study involved 18 general practices from the Sunshine Coast Clinical Research Network. Practices were recruited after responding to an expression-of-interest flyer. Participating practices recorded data for every wound care episode over a 14-day period during December 2011.
A survey form developed for this study was completed by practice nurses at the time of each participant presentation for wound care. Information collected included practice name, participant age and gender, type of wound, type of dressing products used, time spent by the nurse and general practitioner (GP), and billing items claimed. Wound type was classified by the practice nurse as surgical, traumatic, pressure ulcer, venous or arterial leg ulcer, or other.
The cost of wound care was calculated for each individual episode of care by aggregating product cost, nurse care and GP care. Dressing product costs were obtained from SSS Australia.10 Nursing costs were calculated on the basis of the time spent by a nurse multiplied by an hourly rate of $31.11.11 The cost of GP care was calculated as 65% of all items billed, which was reported by local practices as the minimum earnings for a GP contractor. Items billed were recorded and income generated from billing items sourced from Medicare.9 Table 1 provides an explanation of commonly billed items for wound care. Net income was calculated by subtracting the total cost of each wound care episode from the total items billed. Episodes of care where ‘other’ items were billed were excluded from cost and income analysis. Data were entered into Excel and then uploaded to the statistical software package, Stata/SE 10.1 for Windows for analysis.
Table 1. MBS Items billed for wound care episodes in general practice (n = 332)
| Benefit ($) | n | % |
|---|
| Standard GP consultation |
Item 3 |
Professional attendance by a GP for an obvious problem characterised by the straightforward nature of the task that requires a short patient history and, if required, limited examination and management. |
16.30 |
20 |
6.0 |
| Item 23 |
Professional attendance by a GP lasting less than 20 minutes. |
35.60 |
231 |
69.6 |
| Item 36 |
Professional attendance by a GP lasting at least 20 minutes. |
69.00 |
10 |
3.0 |
| Item 44 |
Professional attendance by a GP lasting at least 40 minutes. |
101.55 |
1 |
0.3 |
| Total |
|
– |
262 |
78.9 |
| Other |
Item 10996 |
Wound care service provided by a practice nurse. |
11.80 |
244 |
73.5 |
| Item 10991 |
Service is provided to a person who is under the age of 16 or is a Commonwealth concession card holder; and the service is bulk-billed. |
8.90 |
198 |
59.6 |
| Item 10997 |
Service provided to a person with a chronic disease by a practice nurse or an Aboriginal and Torres Strait Islander health practitioner if the person has a GP Management Plan, Team Care Arrangements or Multidisciplinary Care Plan in place. |
11.80 |
2 |
0.6 |
| GPMP (General Practitioner Management Plan) |
Chronic Disease Management service for a patient who has at least one medical condition that has been (or is likely to be) present for at least 6 months or is terminal. |
104.10 |
2 |
0.6 |
TCA
(Team Care Arrangement) |
Chronic Disease Management service as in GPMP, where patient requires ongoing care from at least three collaborating health or care providers, each of whom provides a different kind of treatment or service to the patient, and at least one of whom is a medical practitioner. |
82.50 |
1 |
0.3 |
| Other |
MBS item not specified. |
– |
12 |
3.6 |
| Patient payment |
Patient payment for dressings used. |
– |
33 |
10.0 |
Results
Across the 18 practices, a total of 336 occasions of service (OOS) for wound care were recorded during the study period, involving 195 wounds in 159 participants. Four OOS were excluded: three were ineligible and one incomplete. The average age of participants was 68.6 years; 53.5% were male and 46.5% were female, and 68 (43%) were treated more than once for the same wound.
Thirty-one patients (19.5%) had more than one wound, and nine of these patients (29.0%) had more than one type of wound. The most common type of wound was surgical (43.6%), followed by traumatic (37.9%). Chronic wounds (venous/arterial or pressure ulcer) accounted for only 11.9% of total wounds (Table 2).
Table 2. Wound type by participant and by total wounds
| Participants | Wounds |
|---|
| |
n |
% |
n |
% |
| Surgical |
72 |
45.3 |
85 |
43.6 |
| Traumatic |
64 |
40.3 |
74 |
37.9 |
| Venous or arterial ulcer |
12 |
7.5 |
15 |
7.8 |
| Pressure ulcer |
7 |
4.4 |
8 |
4.1 |
| Other |
13 |
8.2 |
13 |
6.7 |
|
Total
|
159
|
100
|
195
|
100
|
|---|
| Participants with >1 wound |
31 |
19.5 |
– |
– |
In most cases, the total cost for a wound care episode was greater than the total income, resulting in a net loss to the practice. The median net practice income was –$6.60 (IQR = –$18.67–$3.58). The greatest net loss for a practice on a single episode of wound care during the study period was $178.02, whereas the maximum net income was $33.42 (Figure 1). There was no correlation between the net practice income per episode of care and the type of wound, number of wounds, individual practices, the age or gender of the patient.
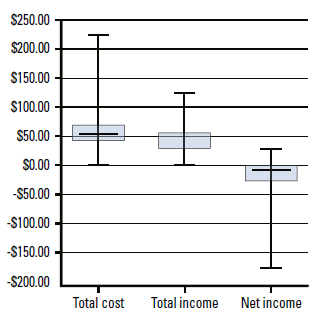
Figure 1. Cost and income for wound care episodes in general practice
GP care was the greatest contributor to the total cost of wound care episodes at 51.8%; products contributed 28.4% and nurse care 19.9%. The median cost of GP care was $31.10 (IQR = $24.10–$37.02), compared with $9.92 for wound care products (IQR = $4.05–$21.57) and $10.37 for nurse care (IQR = $10.37–$10.37).
The single most frequently billed item was 10996, which was used in 73.5% of wound care episodes (n = 244). Standard GP consultation items were also billed in 78.9% of occasions (n = 262). Participants paid for dressings on only 3.6% of occasions (Table 1).
Discussion
The findings of this study indicate that in most cases general practices are not recouping the costs of wound care. The care and time spent by the GP contributes over half of the total cost and almost all practice income for wound care is from MBS billing items.
A major strength of this study is the use of a practice-based research network to select and answer a question that was directly relevant to general practice. The assessment of cost in this study was limited to dressing materials and clinician time, and did not include practice overheads or pharmaceutical and pathology costs, as these were difficult to quantify and attribute to individual episodes of care. Although based on the best evidence available, the costs of practitioner time are estimates only and, particularly in the case of GPs, rates of pay may be higher, resulting in an underestimate of costs. As this study did not examine the patient outcomes of wound care, such as length of time to heal, nor the indirect costs of productivity, travel, hospitalisation and morbidity,12 and the intangible costs of pain, suffering and grief,1,13 it cannot claim to make an assessment of cost effectiveness.
Studies in other countries found that nurse time contributed the greatest proportion of wound care costs.5,6,8 However, although nurses spent the greatest amount of time with participants in these studies, their contribution to cost of care was relatively small. This reflects the funding model for general practice in Australia, where most funding comes from fee-for-service items claimed by GPs, who are in turn paid as a percentage of items billed. However, this study does confirm that practitioner time, whether provided by the nurse or GP, contributes a much greater proportion to the cost of wound care, compared with wound care products.
This study raises concerns that general practice is not currently being adequately remunerated for wound care treatment. Private general practice will need to source additional funds to operate an effective business model for wound treatment. While GP care was the greatest cost it was also the main source of income; therefore it is not a viable target for cost savings, although practices may consider increasing patient co-payments for GP services.
Nurses may provide a more cost-effective option for delivering wound care. However, removal of nurse billing item 10996, the most frequently billed item for wound care episodes in this study, is likely to have made wound care for general practice in Australia even less financially viable. Although the Practice Nurse Incentive Program (PNIP) introduced in January 2012 was intended to ‘consolidate practice nurse funding arrangements into a simplified, single funding stream’ and ‘support an expanded and enhanced role for nurses in general practice’,14 feedback from Sunshine Coast practices that participated in this study has been that nurses now have a reduced role in wound care, compared with that under the previous fee-for-service funding arrangement.15 Block grants, such as the PNIP, have the potential to achieve improved teamwork and enhanced scope of practice, but this is dependent on the organisational climate in each general practice.16 Further investigation is required to determine whether changes to funding nurse time have negatively affected wound care income or practice.
Although product costs made up less than one-third of the total cost of wound care episodes, the product cost per episode of care varied considerably and was quite significant in some cases. Given the limited potential for reducing practitioner time in response to budgetary restrictions, healthcare workers and managers are likely to look to wound care materials to improve the net financial cost, either by charging patients for products or by using less expensive dressings.1,12 However, this avenue of cost saving may not support the delivery of best practice wound care, given the cheapest options are not necessarily the best.1,2
The ability of general practices in Australia to deliver care to their patients is limited by economic factors, with recent federal government policy changes relating to wound care raising further concerns about the financial viability of the already difficult area. Australian general practice faces a dilemma over how best to use GPs and practice nurses in treating wounds and in choosing between lower quality dressings that are more affordable, or higher quality dressings that present a cost access barrier to patients.
Implications for general practice
- The current funding model for wound care in general practice is likely to represent a financial burden for care providers.
- Policy makers need to review how wound care is funded and consider providing subsidies for wound dressings, to ensure that general practice is able to adequately care for high need patients.
- General practices need to review their wound care service delivery and ensure they are providing best practice care while maintaining the financial viability of their practice.
- Further investigation is needed to determine what impact the changes to funding for practice nurses has had on the delivery of wound care in general practice.
Competing interests: None.
Ethics approval: Ethical approval was obtained from the University of Queensland Behavioural and Social Sciences Ethical Review Committee (Reference number: 2011001180).
Provenance and peer review: Not commissioned; externally peer reviewed.