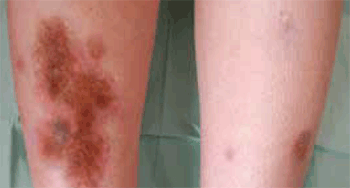
Figure 1a. Brownish, sharply demarcated, indurated plaque on the right shin. Three similar smaller lesions can be observed on the left shin
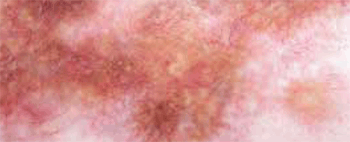
Figure 1b. A close-up view of the plaque. Telangiectatic vessels can be observed on a yellow background
The lesions observed in the patient are typical, which allowed us to make the clinical diagnosis of necrobiosis lipoidica (NL). NL usually presents as small papules or nodules that expand sharply into red-brown-to-yellow plaques that are typically located on the anterior pretibial region. The lesions have a violaceous, irregular border that may be raised and indurated. Commonly, telangiectasias are visible, taking on the characteristic ‘glazed-porcelain’ sheen.
In 1932 Urbach coined the term necrobiosis lipoidica diabeticorum for this disease because it was first described in patients with DM. As it can also appear in non-diabetic patients, the term was shortened to NL. Mean age of onset is 30 years and the incidence is three times higher in women. The prevalence of NL has been reported in different studies to be around 1–2% of patients with type 1 DM.1
Although lacking complete concordance, NL has a solid association with DM and remains a valid marker of the disease. About one-third of patients with NL have DM, and about two-thirds have glucose tolerance abnormalities.2 However, the presence of this skin lesion does not correlate with the level of glycaemic control.1
Differential diagnosis
Granuloma annulare (GA) is a relatively common disorder. Superficial annular lesions can resemble NL. However, GA lesions lack the typical fatty appearance of the yellow NL plaques.
Erythema nodosum is an inflammation of the fat cells in the subcutaneous tissue. Erythema nodosum presents with bilateral, tender, erythematous nodules that lack epidermal change, atrophy or ulceration.
Necrobiotic xanthogranuloma is a very rare, chronic, progressive granulomatous disorder that manifests as yellowish plaques and nodules that can resemble NL. However, in contrast to NL, necrobiotic xanthogranuloma typically presents periorbitally and is associated with paraproteinaemia.3
Sarcoidosis is mainly a diagnosis of exclusion. Although the hallmark of sarcoidosis is a granulomatous plaque, cutaneous lesions rarely ulcerate or show atrophy.
How to make the diagnosis
Diagnosis of NL is usually made clinically, but a skin biopsy might be necessary in atypical lesions. Laboratory findings are unhelpful in the diagnosis of NL. Given the relationship between NL and impaired glucose regulation, patients should be screened for diabetes.4
Management
At present, only small, uncontrolled trials and case reports provide guidance for the management of this disorder. Most authors consider the early application of potent topical glucocorticoids, monitoring for excessive atrophy, as first-line treatment (evidence level: C – expert opinion).5 Intralesional injections of glucocorticoids in the active border have been reported to be useful, although the risk of ulceration with this treatment modality should be considered (evidence level: C).5
Isolated reports support the use of topical retinoids and topical psoralen combined with ultraviolet A (PUVA) treatment.6,7 Recently, photodynamic therapy has been described as another option for the management of NL.8
Calcineurin inhibitors have also been used successfully in some cases. Their effectiveness seems to be higher in ulcerated lesions.9 Similarly, cyclosporine (2.5 mg/kg/day)10 has also been used successfully in ulcerated lesions. The mechanism of action is similar to that of calcineurin inhibitors, preventing T-cell activation.
Aspirin and dipyridamole have produced variable results.11 Other drugs that have been used are clofazimine,12 ticlopidine13 and nicotinamide.14
Various types of laser treatment have been described (pulsed dye laser, CO2 fractional laser);15,16 however, scientific evidence for the effectiveness of these treatments is still too scarce to formally recommend them.
Unfortunately, none of the proposed treatments has achieved a sustained effective response. Surgical excision down to the fascia and split thickness skin grafting remain as the last treatment option for recalcitrant ulcers in NL.17
In some cases, owing to the benign nature of the lesions, a conservative ‘wait and see’ strategy is also acceptable. In all patients, the focus should be on prevention of ulcers. In the event of ulceration, wound care principles for all diabetic ulcers apply.
Complications
The main and most serious complication is ulceration, which occurs on the legs in about one third of NL cases. In addition, a few cases of squamous cell carcinoma on chronic ulcerative lesions of NL have been described.18
Evolution
Given the risk of ulceration, we decided to treat our patient with 0.1% topical tacrolimus. Clinical improvement was slight but the lesions remained stable. After a 1-year follow up, the disease is controlled and has not become ulcerated.
Our case shows a patient with DM who developed typical lesions of NL. The therapeutic management of these lesions is difficult. Our efforts should focus on preventing ulceration and if possible improve aesthetic appearance.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.