Table 1. beyondblue Guideline recommendations for best practice monitoring1
Young people should be monitored for the onset of or increase in suicidal thinking following initiation of selective serotonin reuptake inhibitors (SSRIs).
Monitoring
- It is primarily the responsibility of the prescribing doctor but is best done in collaboration with the young person, their parents or carers and other health professionals involved in their care.
- Monitoring of symptoms that might be subsequently interpreted as side effects should take place for 7 days before beginning medication unless it is required immediately.
- Monitoring of emergent adverse effects, including suicidal thinking and behaviour, and manic symptoms, mental state, general progress and any change in suicidal thinking or behaviour should occur within 7 days of initiating medication.
- Monitoring for clinical worsening, suicidal thinking or behaviour, or unusual changes in behaviour such as sleeplessness, agitation, withdrawal from normal social situations, or manic or psychotic symptoms should occur every week for 4 weeks.
- Particularly close monitoring may be required for young people who are not receiving psychological treatment or have existing suicidal thinking or behaviour.
|
Despite the importance of monitoring, research5,7 indicates that monitoring after the prescription of an antidepressant is vastly below recommended practice. Clinicians often rely on spontaneous reporting,6 a practice shown to insufficiently identify young people at risk of suicide.5,7
To address identified barriers to monitoring,8 we have developed an online tool for patients to self-monitor depressive symptom severity and adverse effects, including suicidal ideation and mania symptoms (Figure 1). The design and development of this tool has incorporated feedback from young people who are current and past users (The Platform Team) of Orygen Youth Health (OYH), a specialist mental health service for people aged 15–25 years in the Northwestern Metropolitan region of Melbourne, as well as clinicians from the OYH Youth Mood Clinic. Our aim in this study was to:
- understand the issues related to monitoring in the primary care context, given young people with depression often access care in such settings9,10
- ascertain if our online monitoring tool would be appropriate for this setting.
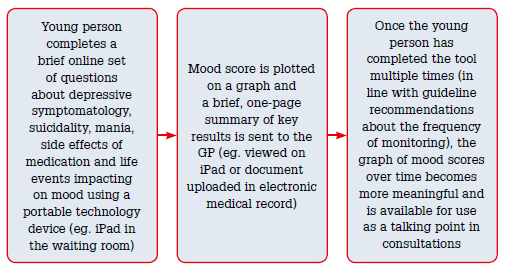
Figure 1. Features of the monitoring tool for youth depression
Methods
We undertook two focus groups with purposively selected general practitioners (GPs) from the Victorian Primary Care Practice-Based Research Network (VicREN), which comprises primary care practitioners and academic GPs. We aimed to recruit a mix of men and women, years of experience, geographical location and types of practice.
GPs on the VicREN database who self-identified as having an interest in youth and/or mental health were sent email invitations. Two dates were offered: one in September and the other in October 2012. Participants were not paid for their participation, but dinner was provided.
The focus groups, involving one facilitator (MS) and one scribe (LS), were audio-recorded and transcribed verbatim using orthographic conventions. We explored the perceptions and current practices of GPs with regard to monitoring symptoms and side effects in line with guideline recommendations.1 We specifically probed for barriers and enablers related to knowledge, skills, organisation culture, professional role, and time and resources available for monitoring. We also probed for feedback on our online monitoring tool. A semi-structured focus group schedule was used. Thematic analysis was used to analyse the data.11 Ethics approval was obtained from the relevant committee (MHREC 2010.240).
Results
The two focus groups lasted for 143 and 132 minutes. A total of 12 GPs participated: 7 in one focus group and 5 in a second focus group. The mean age of the 12 GPs was 47.9 years (SD = 8.1; range 32–59 years), they had been in practice for 5–34 years (mean = 20.9; SD = 8.9) and 58.3% were women. The results were organised according to the key themes identified during analysis.
Potential barriers to monitoring in general practice
Overall, GPs perceived that monitoring was difficult. GPs seemed to equate the process of monitoring with that of screening for illness, and thought their role was to ‘sort out’ young people who may or may not be depressed. Some GPs expressed concerns about not having the necessary skills or experience in assessing depressive symptoms and suicidality in young people.
Furthermore, GPs also considered monitoring as ‘ongoing screening’, only useful if it provided them with clinical information that informed treatment planning.
‘And what you need then in the monitoring is, I always think, “when am I going to change my management? What signs and things are going to… make me rethink the process that I am doing?”’
Young people diagnosed with depressive disorders were often referred to a specialist healthcare professional. Some GPs saw the role of monitoring as being transferred to the healthcare professional they referred to (eg. psychologist), although it was acknowledged that the patients often ‘bounce(d) back’ to general practice. Other GPs felt that monitoring was ‘all part of your role (as a GP); if you are managing them, you have to still do it’. Others said it would depend on the patient (eg. higher onus to monitor if risk issues were present). Regardless, GPs felt ‘entirely responsible’ for monitoring associated with any medication they prescribed. For some, this was stated as essential in order to know how patients were responding to the medication.
The potential benefits of monitoring tools
The main reported benefit of monitoring tools was to facilitate collaboration and dialogue with their patient.
‘If you do a (monitoring) tool, it’s an independent sort of third bit. It is not me and the patient. It is “let’s do this together”, and there is a bit more (of a) cooperative thing about it.’
GPs stated that monitoring tools provided an opportunity for young people to disclose information the young person might not feel comfortable to disclose face-to-face to the GP or that might not be asked about because of the potential for misunderstanding. Monitoring tools that generated reports for GPs were seen as activating GPs.
‘You become responsible because you get a report about this patient. So you go up to the patient and say, “look, I have got your report (would) you like to talk about it?'
The potential risks and practical concerns related to monitoring tools
A key concern was about how to respond in a timely manner to results indicating clinical risk (eg. suicidality), and whose responsibility this would be (eg. outside clinic hours). GPs suggested that a tool completed before the consultation that provided immediate results would be most useful or that suicide-related questions be asked only in face-to-face encounters. Other practical concerns included ensuring that the tool was not too long and that asking them to complete a tool did not interfere with engagement (putting a young person ‘off side’). GPs felt that engagement was important in ensuring that young people using the tool provided accurate reflections of their feelings and thought this could be achieved by asking additional questions, not in the tool.
‘Because you have actually… stopped trying to follow the recipe and you have said “okay, I am listening to you”. If you say “I am listening to you”, then people are going to tell you, I think are more likely to tell you some or all of their truth.’
Some GPs were unsure whether young people liked disclosing issues using electronic media and were concerned about the impact on engagement, compared with face-to-face methods of monitoring. Others were aware that young people often preferred electronic methods of communicating about sensitive issues.12
Challenges to and opportunities that enable the use of monitoring tools
Most GPs reported insufficient resources as a key barrier, including not having the technology (eg. iPads or computers) or a quiet space for patients to complete the tool. Some GPs also expressed concerns about not having the necessary technological skills. Other reported barriers included any costs (eg. subscriptions fees); patient ability to understand questions; and that tools were often not validated with participants from other cultures or in general practice.
On the other hand, GPs reported enablers, including that tools for depression screening were commonly available; the high prevalence of smartphones; use of iPads in the waiting rooms of some clinics; that a system for electronic storage of monitoring results and electronic prompts was in place. Some GPs reported having the opportunity to book longer appointments to allow time for young people to complete a monitoring tool; and the increasing number of practice nurses who potentially have a role in facilitating the use of a monitoring tool.
Feedback on our monitoring tool
Overall, GPs were positive about how comprehensive the tool was, stating it would bring structure to consultations, standardising practice and ensuring ‘nobody slips through the net’. GPs commented that the questions about suicidal ideation and behaviour were more thorough than those they use. In this way, GPs reported the tool could serve as a ‘teaching tool’, educating GPs and their patients. They suggested that presenting these questions and the young person’s responses would be empowering, as young people ‘like to see hard data’. Further, using standardised questions demonstrates that other young people experience similar phenomena. Administering the tool on an iPad was seen as a non-threatening and contemporary way to relate to young people. GPs stated that the tool seemed easy to complete, did not believe it would increase consultation time (if completed before the appointment) and would support their medico-legal cover in terms of documenting risk issues. GPs liked the documentation of life events contributing to mood and the graph of depression symptom and suicidal ideation scores over time, which GPs suggested would be a ‘conversation starter’.
In terms of potential negative aspects, although a brief tool was seen as important, GPs stated they wanted a meaningful summary of responses that included information beyond numerical scores. They highlighted the importance of informing patients about why they were being asked to complete the tool in order to enhance engagement. Some felt that training to use the tool might be needed for GPs with little experience in assessing depression symptoms and suicidality in young people. Some GPs stated that the tool was unlikely to allow differentiation between diagnoses, given some symptoms in the tool were common across disorders. Others highlighted that making a tool available would not ensure that GPs who prescribed antidepressant medication would engage in routine monitoring.
A range of practical suggestions was made to improve the tool including: reducing the number of items; incorporating items relating to functional impairment; asking patients about the nature of their social media status updates to facilitate them to think about their recent mental health. The most commonly raised suggestion was to ensure the tool included electronic alerts reminding GPs to undertake monitoring, and that it was incorporated into widely used practice tools and software.
Discussion
Overall, monitoring in primary care settings was viewed differently from how it might be seen in tertiary settings. GPs in our focus groups perceived monitoring to be part of a continuum of care that begins with screening and diagnosis. It is clear that any monitoring tool implemented in primary care needs to assist this, as well as monitoring symptoms and side effects after initiation of medication, for example, by disabling questions about side effects when antidepressant medication has not been prescribed.
Further, rather than automatically taking responsibility for monitoring, GPs often diagnose and refer to other clinicians who may be seen as having responsibility for this. Alternatively, they may undertake monitoring in collaboration with those to whom they have referred. Monitoring systems in general practice need to allow flexibility for these scenarios, as well as for those patients who might be referred to another clinician but who return to the GP. Therefore, although monitoring may start with screening and diagnosis, it needs to be revisited in order to meaningfully inform ongoing treatment plans.
A monitoring tool has the potential to facilitate collaborative engagement, allowing disclosure that may not be made in a face-to-face encounter. When discussing our tool specifically, it was noted that incorporating details about life events that contributed to mood might enable GPs to have a useful discussion with the young person about their symptoms. However, it was also noted that a certain level of engagement with the GP was seen as a prerequisite to the young person using the tool in the first place, as was providing young people with a clear rationale for its use, to help promote full and honest responses. Face-to-face questions were seen as critical, particularly for engagement, but also to further and comprehensively assess suicide risk.
GPs made some useful suggestions for our tool, some of which are already being implemented. For example, we are undertaking a large study to implement item reduction. Further modifications can be made in line with GP suggestions, such as including questions about functioning. For the tool to be most useful, particularly to support monitoring consistent with guidelines, it is critical that it is incorporated into the system tool(s) and software already being used in general practice. Ensuring that the tool is brief and appropriately embedded in clinical practice seem to be key factors in maximising its use by and usefulness to a large range of clinicians,13 potentially providing welcome assistance to those who do not typically work with young people who have depression.
Overall, a monitoring tool was seen as one of many tools that the GP can use, in addition to their other skills and techniques, that it can be a starting point for collaborative discussion, and provide additional information to assist in the management of young people with depression.
Acknowledgements
We would like to thank the GPs who donated their time to be involved in the focus groups. We would also like to thank the VicREN for their assistance in the undertaking of this study.
Competing interests: None
Provenance and peer review: Not commissioned; externally peer reviewed.