Question 1
What is the differential diagnosis?
Question 2
What investigations should be ordered?
Case study continued
The patient’s thyroid function test revealed hyperthyroidism:
- Decreased TSH <0.01 mU/L (0. 27–4.20)
- Elevated free T4 at 23 pmol/L (12–22)
- Elevated free T3 at 7.04 pmol/L (4.0–6.8).
Computed tomography (CT) scan of the orbit shown in Figure 1 revealed asymmetric bilateral ophthalmopathy involving predominantly the left orbit and inferior rectus muscle. A CT scan of the brain was unremarkable.
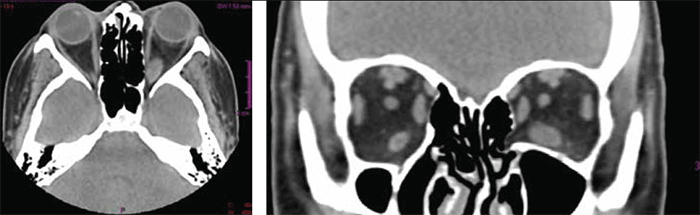
Figure 1. CT scan of the orbit revealing asymmetric bilateral opthalmopathy
Question 3
What is the diagnosis?
Question 4
What management options are available for this patient?
Answer 1
Diplopia is divided into monocular and binocular. Monocular diplopia is determined by the persistence of double vision when the unaffected eye is covered. The lesion can be localised to intraocular structures including refractive error, cataracts, lens dislocation and corneal opacity.1
Binocular diplopia is determined by the absence of diplopia when either eye is covered. Causes include:1
- Orbital (trauma, tumour, infection)
- Neurological
- cranial nerve nucleus damage (infarct)
- cranial nerve injury (CN III, IV, VI secondary to trauma, tumour, diabetes, sarcoidosis, vasculitis, aneurysm)
- neuromuscular junction (myasthenia gravis)
- muscle disorders (Graves’ ophthalmopathy).
Answer 2
First-line investigations in the general practice setting may include a full blood count, erythrocyte sedimentation rate (ESR), blood glucose and thyroid-stimulating hormone (TSH). Neuro-imaging such as CT or magnetic resonance imaging (MRI) of the brain or orbit may be required if there is clinical suspicion of a space-occupying lesion or neurological lesions such as multiple sclerosis.2 Further investigations such as electromyography (EMG), nerve conduction studies, tests for autoantibodies against acetylcholine receptors and follow-up investigations for any derangement in first-line tests may be ordered if indications exist.
Answer 3
Ophthalmopathy due to Graves’ hyperthyroidism.
Answer 4
Management of a patient with Graves’ ophthalmopathy should always first address the reversal of hyperthyroidism with antithyroid drug therapy, even though this has little-to-no effect in improving the ocular disease process.3 Prevention of corneal damage due to exposure includes artificial tears by day, ocular lubrication by night, punctal plugs, eyeshades and elevation of the bedhead at night.4,5 Severe or deteriorating orbitopathy may benefit from the anti-inflammatory properties of corticosteroids, and methylprednisolone is the drug of choice.3,4 Orbital radiation and surgical intervention may be required if medical treatment fails.6,7
Discussion
Hyperthyroidism is a condition commonly encountered and managed in the general practice setting. The classical constellation of symptoms includes weight loss, increased appetite, sweating, tremor, anxiety, heat intolerance, palpitations, dyspnoea and diarrhoea.8 Depending on the cause, other manifestations may include the development of a goitre or ophthalmopathy unique to Graves’ disease.
Graves’ ophthalmopathy is an autoantibody-mediated process, whereby inflammation and fibrosis can occur and lead to an increase in volume of extra-ocular muscles and retro-orbital tissues.9 Patients may complain of eye irritation, retro-orbital pressure and pain, excessive teariness, blurriness, diplopia and visual loss. Signs of ophthalmopathy include proptosis, periorbital oedema and restriction of ocular movements. Smoking is a major modifiable risk factor with an odds ratio of 7.7 when compared with non-smokers.10 The likely pathology involves an increase in the volume of connective tissue in the orbit rather than an effect on the extraocular muscles.11 The time course of Graves’ ophthalmopathy is variable, and is noted to precede any other symptom of hyperthyroidism in 20% of cases, in conjunction in 40% of cases and 40% following other symptoms.4
In Murtagh’s General Practice, seven ’masquerades’ are identified as diagnoses that are commonly missed; these include depression, diabetes, drugs, anaemia, thyroid disorder, spinal dysfunction and urinary tract infection.12 In line with Murtagh’s model, this case elucidates the importance of considering hyperthyroidism in patients presenting solely with diplopia. In essence, remembering to screen for masquerades, especially in the general practice setting, would save patients from unnecessary referrals and time spent within the medical system.
Key points
- Diplopia is divided into monocular and binocular.
- Monocular diplopia indicates pathology of intraocular structures.
- Binocular diplopia is usually caused by pathology of the orbit, cranial nerve palsy, neuromuscular junction disease, myopathy or systemic disease.
- Thyroid disease should be excluded in patients with binocular diplopia since Graves’ disease can present with ophthalmopathy as its only clinical feature.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.