A large European survey undertaken simultaneously in a number of countries suggested that almost 20% of people over the age of 18 years had suffered chronic pain for at least 6 months at some stage in their lives,2 with well over half affected to the extent that they were less able to work, and almost 20% of these people having lost a job because of their pain. Nearly 20% of survey respondents with chronic pain were depressed as a result of their pain and half were concerned that their pain management was inadequate. This study also suggested that only about 2% of people with long-term pain attend a pain clinic to receive specialist care.2
The role of the mind in the experience of pain
The human experience of pain is not merely somatic: it varies according to our mental, emotional and physical make-up. Pain perception involves many brain centres that register and modify pain signals. These include the regions involved with attention, beliefs, conditioning, mood, emotion, stress and cognition (Figure 1).3 The various mind-body approaches to chronic pain can be understood as working at one or more of the levels of experience of pain outlined in Figure 1. Importantly, they often work via similar mechanisms and have synergistic effects.
Interestingly, working with empathy, which can involve vicariously experiencing another’s pain, has been shown to produce similar changes in brain activation of the amygdala (indicating stress and arousal) as the person actually experiencing the pain.4 There are significant implications for vicarious stress, because when it is prolonged it can predispose to carer fatigue or carer burnout. Relaxation or mindfulness techniques may be a useful strategy for general practitioners to help carers avoid this outcome.1
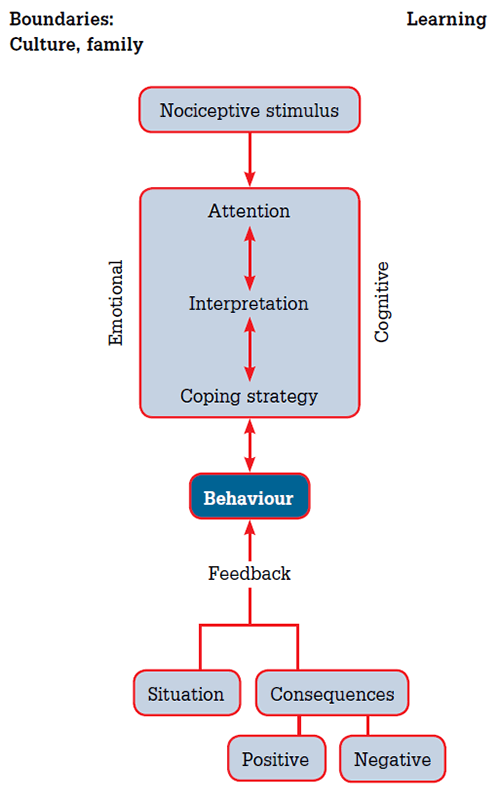
Figure 1. Pain perception pathways
Reproduced with permission from Linton SJ, Shaw WS. Impact of psychological factors in the experience of pain. Phys Ther 2011;91:700–11
Many patients with chronic pain experience stress, fear and depression. These emotions and mental states, and their associated behaviours, often also act as aggravating factors due to the potential for amplification of the perception of pain. Conditions associated with chronic pain include burnout, depression, chronic fatigue syndrome and fibromyalgia. In many of these conditions, the brain is registering pain messages even in the absence of demonstrable tissue damage, making it difficult for the GP to assess or, in some cases, even believe their patients’ stories. However, evidence suggests that neural loops in the brain are sensitised and maintained by ‘sustained attention and arousal’,5,6 meaning that the person is hypervigilant around and preoccupied with the pain and they become very emotionally reactive to it when it is noticed. As a result, over time the same stimulus produces more suffering and a vicious cycle begins.
It is also worth noting that existential or spiritual issues, such as the fear of death in cancer patients, have the potential to aggravate pain issues if they are not recognised and addressed. Furthermore, conditions such as chronic back pain may be complicated by socioeconomic factors, such as worker’s compensation or employment issues.
Attention to pain is linked to activation of the ‘fight or flight’ (stress) response and the consequent need to take action, such as escaping or avoiding it. Hypervigilance involves an amplification of this response, resulting in an abnormal focus on, or preoccupation about, possible signals of pain or injury. This explains why a relatively small injury can result in the perception of intense pain and suffering. Anyone who has sat in a dentist’s chair is likely to have noticed that in the presence of emotional distress, the level of suffering can be excessive when compared the actual level of physical injury. This exemplifies the close links between emotional and cognitive processes, attention and the perception of pain.7–9
Despite a range of psychological factors being important in the genesis and persistence of chronic pain syndromes, they are not always routinely assessed in general practice or physical therapy clinics, or utilised to enhance treatment outcomes.10 Linton et al10 reviewed the scientific evidence and laid out 10 principles that have likely implications for pain management in the clinical setting (Table 1).
Table 1. Ten guiding principles relating psychological factors to the management of pain
| Treatment phase | Number | Guiding principle | Clinical implications |
|---|
| Assessment |
1 |
Psychological factors that may affect pain outcomes are not routinely assessed by many treating clinicians |
Better methods of screening and early intervention are needed to improve feasibility and utility in usual care settings |
| 2 |
Persistent pain naturally leads to emotional and behavioural consequences for the majority of individuals |
Psychological concepts of learning can be useful to provide empathy and support without reinforcing pain behaviour |
| 3 |
Clients who are depressed or have a history of depression may have more difficulty dealing with pain |
A brief assessment of mood symptoms should be part of routine screening and intake procedures for pain conditions |
| Treatment planning |
4 |
Persistent pain problems can lead to hypervigilance and avoidance, but simple distraction techniques are not enough to counter these behaviours |
Clinicians should avoid inadvertent messages that escape or avoidance from pain is necessary in order to preserve function |
| 5 |
Individuals hold very different attitudes and beliefs about the origins of pain, the seriousness of pain, and how to react to pain |
Assessment and treatment planning should take into account individual differences in pain beliefs and attitudes |
| 6 |
Personal expectations about the course of pain recovery and treatment benefits are associated with pain outcomes |
Providing realistic expectations (positive, but frank and not overly reassuring) may be a very important aspect of treatment |
| 7 |
Catastrophic thinking about pain is an important marker for the development of long term pain problems as well as for poor treatment outcome |
Clinicians should listen for expression of catastrophic thoughts and offer less exaggerated beliefs as an alternative. A brief assessment might be part of routine intake procedures |
| Implementation |
8 |
Personal acceptance and commitment to self manage pain problems are associated with better pain outcomes |
Over attention to diagnostic details and biomedical explanations may reinforce futile searches for a cure and delay pain self management |
| 9 |
Psychosocial aspects of the workplace may represent barriers for returning to work while pain problems linger |
Return to work planning should include attention to aspects of organisational support, job stress, and workplace communication |
| 10 |
With proper instruction and support, psychological interventions can improve pain management outcomes |
Psychological approaches can be incorporated into conventional treatment methods, but require special training and support |
Reproduced with permission from Linton SJ, Shaw WS. Impact of psychological factors in the experience of pain.
Phys Ther 2011;91:700–11 |
Mind-body approaches in pain management
Any intervention that changes a person’s mental or emotional state, such as meditation, listening to music or cognitive behavioural therapy (CBT), will produce corresponding changes in the body and could therefore be called a ‘mind-body’ intervention. In addition, therapies that utilise physical movement such as yoga or tai chi, also rely on training attention or producing mental relaxation and could be described as both physical and mind-body techniques. Furthermore, there is often a great deal of overlap between different mind-body approaches, for example, in Jon Kabat-Zinn’s mindfulness based stress reduction program there is extensive use of yoga techniques.11
A range of mind-body approaches can be used in the management of chronic pain, occasionally as a sole treatment, but more commonly as adjuncts to other therapies.12
In managing chronic pain, if psychological and emotional issues are amplifying the problem, then merely increasing the dose of analgesics, rather than improving the outcome, can commonly add to the problem by leading to drug dependence or addiction. A combined approach where emotional, social and/or existential issues are being dealt with, as well as the physical problem, is far more likely to produce long-term benefits to the patient.
Evidence for the effectiveness of mind-body approaches for various conditions associated with chronic pain includes:
- psychosocial interventions had medium size effects on both pain severity and interference in patients with cancer13
- specific mind-body practices may help alleviate pain and enhance physical function in adults suffering from osteoarthritis of the knee14
- mind-body techniques may be useful in treating fibromyalgia pain15
- in rheumatoid arthritis, statistically significant improvements with mind-body approaches were seen in pain, functional disability, psychological status, coping abilities, self efficacy, and joint involvement with the greatest improvements noted in patients with a history of depression16
- psychological treatments resulted in clinically relevant improvement in around 70% of paediatric patients with headache.17
Specific mind-body interventions
The relaxation response
The ‘relaxation response’ is the opposite of the stress or ‘fight or flight’ response and can be elicited by techniques such as progressive muscle relaxation, meditation and even laughter – hence the use of ‘clown doctors’ in many children’s hospital wards.
The relaxation response may be associated with greater pain tolerance as it has the potential to:
- enhance the brain’s responsiveness to endorphins18,19
- reduce inflammation
- cause muscle relaxation
- reduce hypervigilance and desensitise central pain pathways
- enhance mood and reduce emotional reactivity to pain.
Mindfulness based approaches
Mindfulness based approaches can be very helpful in managing chronic pain, particularly considering the role of hypervigilance and emotional reactivity in the genesis of chronic pain. These encompass distraction techniques that teach patients to shift their attention to stimuli other than the pain (eg. by imagining the sound of waves hitting the shore), and interceptive exposure techniques, which shift attention toward the pain so that the signal will habituate.20
Mindfulness based approaches also aim to cultivate an attitude of acceptance toward their chronic pain symptoms. This is helpful because emotional reactivity to pain can greatly accentuate the pain due to resistance to the pain and cognitive elaboration on the pain.21 Acceptance of chronic pain is not resignation to it. Instead, the individual reduces unsuccessful attempts to avoid or control pain where that is not possible. This makes it easier to focus instead on other experiences or aspects of the environment including participation in valued activities and the pursuit of personally relevant goals. McCracken and colleagues22 report that, ‘pain related acceptance leads to enhanced emotional and physical functioning in chronic pain patients above and beyond the influence of depression, pain intensity, and coping’.1 Acceptance can be measured using instruments such as the Chronic Pain Acceptance Questionnaire (see Resources).
Acceptance cultivated through mindfulness based approaches may also help by minimising the avoidance that is often a part of the pain syndrome, which leads to secondary injury through problems such as poor posture, loss of muscle tone or maladaptive changes in gait.
Studies on brain activation show higher levels in meditators in the areas of the brain implicated in attention, cognitive control, somatic awareness and stress regulation pain related regions, including the dorsal anterior cingulate cortex, insula and thalamus. But in the same group of people, activation is dramatically reduced in areas involved in appraisal, emotional regulation, stress and memory, such as the medial prefrontal cortex, orbitofrontal cortex, amygdala and dorso-lateral prefrontal cortex.3 This suggests that mindfulness meditation has the potential to reduce pain through a number of brain mechanisms.
Mindfulness based approaches involve both meditation and a way of living that develops attentional skills and acceptance, reducing pain related arousal and reactivity. Mindfulness practice has been shown to be effective in the management of chronic pain,23,24 including in women with irritable bowel syndrome.25
Hypnosis
Hypnosis was one of the first mind-body approaches used for chronic pain and has established efficacy.26 Brief hypnotherapeutic treatment methods show encouraging results, including in children and adolescents with functional abdominal pain.27 The mechanism may be through relaxation as well as altering perception and cognitive patterns that become established in pain syndromes. Hypnosis has been shown to improve the pain associated with irritable bowel syndrome, with benefits still demonstrable after 5 years.28
Heterohypnosis and self hypnosis have been shown in some studies to be effective in reducing labour pain with other possible benefits including better infant Apgar scores and a shorter stage 1 labour.29
Guided imagery
Guided imagery in the treatment of chronic pain aims to enhance relaxation, as well as unhooking attention from the pain and the mental elaboration about it, through the use of peaceful, soothing or symbolically therapeutic mental images. In a review of nine randomised clinical trials, eight were found to suggest that guided imagery leads to a significant reduction in musculoskeletal pain. Although these results are promising, many of the studies were small or were low to medium grade in terms of methodological rigour.30
Yoga
While yoga involves physical postures, it can be considered a mind-body intervention due to the emphasis on acceptance, training attention, meditation and relaxation. Eight of nine RCTs showed that yoga leads to a significantly greater reduction in pain than control interventions such as standard care, self care, therapeutic exercises, relaxing yoga, touch and manipulation, or no intervention.31 Relaxation and yoga may also have a role in childbirth by reducing pain, increasing satisfaction with pain relief and, consequently, reducing the rate of assisted vaginal delivery due to the woman’s greater coping skills.32 Another meta-analysis on the effectiveness of yoga interventions on pain and associated disability (eg. back pain, rheumatoid arthritis, headache/migraine) concluded that, ‘yoga is a useful supplementary approach with moderate effect sizes on pain and associated disability’.33
Biofeedback
Biofeedback is a method of increasing physical awareness and inducing a relaxation response through the use of markers of the stress response, for example, learning to lower blood pressure by watching a screen mapping the blood pressure in real-time. Apart from relaxation, it provides a focus of attention and helps to promote a more objective and precise understanding of the mind-body relationship.
Biofeedback has been used as an adjunctive treatment in a number of pain settings to good effect, such as with orofacial pain,34 headache in children,35 phantom limb pain (+/- visual mirror feedback),36 and musculoskeletal pain.37
Cognitive behaviour therapy
Any strategy that changes states of mind and emotion can be considered a mind-body therapy, including CBT. Cognitive behaviour therapy has a sound evidence base for a range of chronic pain conditions,38 including chronic back pain39 and fibromyalgia,40 and has been shown to be associated with fewer days of work missed due to pain related disability.41 It has also been found to be useful for pain in children and adolescents.42 However, some authors have questioned its efficacy and use in myalgic encephalomyelitis.43
Method of delivery of mind-body interventions
A review of 46 RCTs of various aspects of delivering psychosocial interventions for chronic pain found that group-delivered courses that had healthcare professional input showed more beneficial effects.44 Courses longer than 8 weeks did not necessarily give better outcomes.
Group-delivered psychosocial interventions for chronic pain aim to provide patients with greater self-efficacy through skills that they can apply at home and work. The aim is self-sufficiency and not dependency on a therapist, but in order to do this a patient needs to be assisted through the sometimes difficult early stages of learning these skills. A supportive, experienced practitioner and a group working toward the same end help enormously. The facilitator therefore needs skills in the mind-body therapy being used, group facilitation skills and motivational skills (see Resources). Groups are also useful for breaking down isolation, enhancing motivation and providing the benefits of learning from the insights and experiences of other group members.
Mind-body therapies in general practice
Some mind-body therapies lend themselves more easily to use in general practice. For example, skills in relaxation techniques are a good starting point. More extensive training is needed to apply approaches such as mindfulness, hypnosis, imagery and CBT, but they are eminently adaptable to the general practice setting if adequate time is taken for their implementation. Yoga and biofeedback will generally require referral. Importantly, GPs are well placed to recommend or learn and provide a range of mind-body approaches to improve outcomes for patients with chronic pain.
Resources
- The Chronic Pain Acceptance Questionnaire is available at www.psychologytools.org/pain.html
- GPs wishing to set up their own mindfulness groups are advised to receive training in the technique from experienced teachers. Information on mindfulness teachers, practitioners and groups can be found by contacting the Mindfulness Practitioner Interest Group at MBSR-MBCT_ANZ@yahoogroups.com.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.