Case study
A Mediterranean woman aged 70 years, presented with a 2 year history of continuous itch over the left scapula and upper back. She denied application of any topical product. She was otherwise healthy and not taking any medications.
Physical examination revealed a brownish, non-infiltrated ovoid patch of 5–7 cm in diameter on the skin over the lower margin of the left scapula (Figure 1). On questioning, she admitted to pain along the T–6 and T–7 dermatomes when walking. The patient was referred to an orthopaedic surgeon to rule out spinal disease.
Magnetic resonance imaging (MRI) of the thoracic spine revealed chronic degenerative changes of the dorsal intervertebral discs, with small protrusions at level T6–T7 that were contacting and deforming the ventral aspect of the spinal cord (Figure 2).
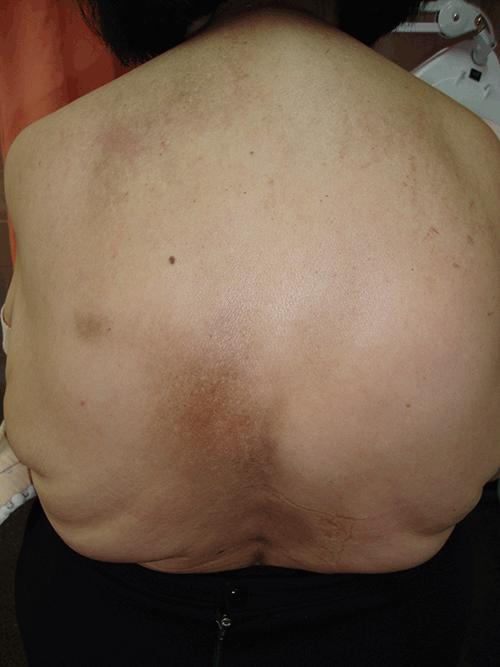
Figure 1. Brownish, ovoid patch of 5–7 cm in diameter on the skin over the lower margin of the patient’s left scapula
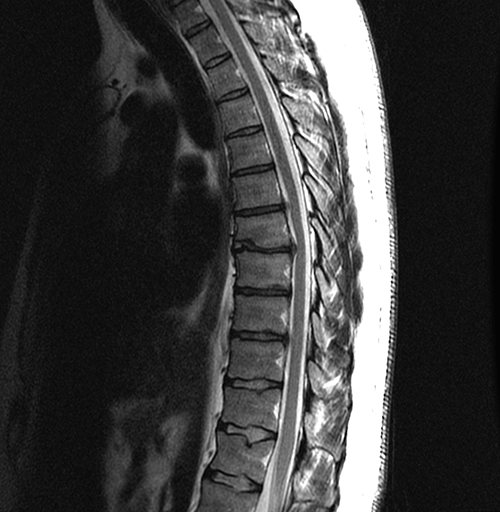
Figure 2. MRI of the thoracic spine (1.5T). Sagittal fast spin echo T2 weighted image shows chronic degenerative changes in intervertebral discs, with osteophytes, dehydration and height loss. There are small disc protrusions at T5–T6 and T8–T9 and a disc herniation at T6–T7 obliterating the anterior subarachnoid space and deforming the spinal cord without signal intensity changes
Question 1
What are the likely differential diagnoses to be considered?
Question 2
What is the diagnostic work-up?
Question 3
What are the treatment options?
Answer 1
Based on the clinical findings, a diagnosis of notalgia paresthetica (NP) can be considered. Notalgia paresthetica is a common although underdiagnosed neuropathic syndrome of the skin on the back. It presents as intense localised pruritus1–4 and is thought to be a result of spinal nerve impingement or chronic nerve trauma of the nerves which supply sensation in the T–2 to T–7 dermatomes.1,2,4 Notalgia paresthetica usually affects adults aged 40–80 years and is seen in both males and females, being more frequent in women. Clinically, NP presents as episodes of localised itch on the upper back, usually on the unilateral infrascapula.5 It can be accompanied by pain, abnormal heating, and burning or cold sensations. On physical examination, a unilateral brownish macule on the skin is common.5
Other differential diagnoses are lichen amyloidosus and lichen simplex chronicus. Lichen amyloid can occur without notalgia. It is uncertain whether it is a cause or consequence of the itch. Lichen simplex can complicate notalgia and will persist once established, regardless of the triggering condition, unless treated. Other differential diagnoses include pigmented contact dermatitis, patchy parapsoriasis and tinea versicolor. In such cases, the diagnosis is based on the morphology of the lesions, the course of the disease and the appearance of cutaneous lesions in other locations. Other non-itching disorders with increased pigmentation can be ruled out more easily: postinflammatory hyperpigmentation, Becker nevus or fixed drug eruption. In cases of uncertainty, skin biopsy may be useful.
Answer 2
Diagnosis of NP is usually made on the basis of clinical findings. Intermittent pruritus is the most common symptom. Laboratory tests are not required, and although imaging tests are usually not needed, MRI may be indicated if ‘red flag’ symptoms are present. Skin biopsy is usually not indicated for the diagnosis of NP, although if performed, macular amyloidosis or postinflammatory hyperpigmentation may be seen.
Answer 3
Treatment of NP is challenging. Standard dermatological treatments, including topical steroids or oral antihistamines, are often ineffective.5 Topical capsaicin has been shown to be efficacious, but this is only transient.3 Some patients with NP and underlying spinal disease may improve with evaluation and conservative management of the spinal disease, including progressive exercise and rehabilitation.2 Other therapies include gabapentin, transcutaneous electrical nerve stimulation,6 phototherapy7 or botulinum toxin.8 In our patient, after 6 months of conservative treatment consisting of exercise and rehabilitation, a clinical improvement of her symptoms was achieved.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.