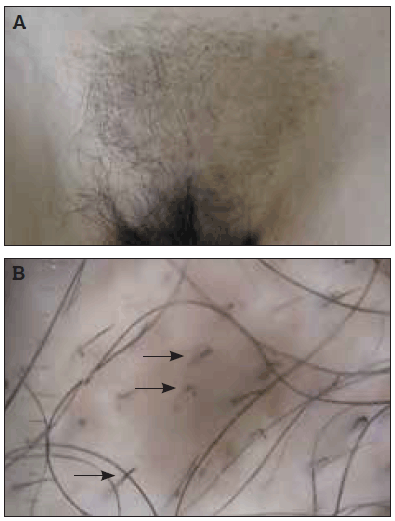
Figure 1a. An irregular patch of alopecia on the pubis with follicular hyperkeratosis and hyperpigmentation
Figure 1b. Magnified view revealing decreased hair density, broken hairs with different shaft lengths (arrows) and short vellous hairs
Question 1
What is the most likely diagnosis?
Question 2
What are the diagnostic criteria for trichotillomania?
Question 3
What are the main clinical manifestations in trichotillomania?
Question 4
What is the differential diagnosis?
Question 5
What are the treatment options for this disease?
Question 6
What is the prognosis for this disease?
Answer 1
The most likely diagnosis is trichotillomania (TTM). Trichotillomania is a primary psychiatric disorder with dermatological signs. It is considered an impulse control disorder in the Diagnostic and Statistical Manual of Mental Disorders, 4th edition (DSM-IV).1 Although TTM was previously considered an infrequent condition, it is now thought to occur in 1–4% of the general population.1
Answer 2
The disorder causes clinically significant distress or impairment in social, occupational, or other important areas of functioning. The DSM-IV criteria for TTM are:1
- periodic pulling out of the hair, resulting in visible hair loss
- an increasing sense of tension before pulling out the hair, or when trying to resist the conduct
- satisfaction or liberation when pulling out the hair.
Answer 3
Any hair surface can be affected. However, the most common areas affected are the scalp, eyebrows and eyelashes. The most affected scalp areas are the anterior regions and the vertex. The lower eyelid lashes are usually not involved, which helps to differentiate it from alopecia areata. It is quite uncommon for solely the pubic area to be affected (2–5% of cases),2 and this is usually indicative of a psychiatric disorder.3 However, it is not that unusual (17%) in people who pull hairs from multiple locations.3
The areas of hair loss are most often found on the side of the body contralateral to the dominant hand. Alopecia plaques have an artificial appearance; and are generally circular, and contain hair of various lengths, shapes and sizes. Signs of inflammation are not usually found in TTM, although in some cases, with intense scratching there may also be signs of excoriation, lichenification, erythema and postinflammatory hyperpigmentation. Most people with TTM pull their hair while in private, and generally try to hide the disorder from others. Most are consciously aware that they are pulling their hair out and may even develop elaborate rituals for doing so. Others do so unconsciously. A person may occasionally do both (pull hair consciously and unconsciously), depending on the situation and their mood. Occasionally, patients with TTM have other pathological repetitive movements, such as skin picking, cuticle or nail biting or picking, and cheek or lip biting. The term ‘repetitive self-grooming behaviours’ is used to include the disorders that result in self-body damage.4
Answer 4
Trichotillomania needs to be differentiated from other causes of patchy non-scarring hair loss. Alopecia areata is the main cause of diagnostic confusion, however this presents as oval, well demarcated plaques, and the skin may feel softer than expected (Figure 2). The hair-pull test around areas of alopecia areata will render telogenic hairs. In TTM, there will be signs of recently broken and plucked hairs and the surrounding hairs may appear artificial. The hair-pull test is negative in this condition.
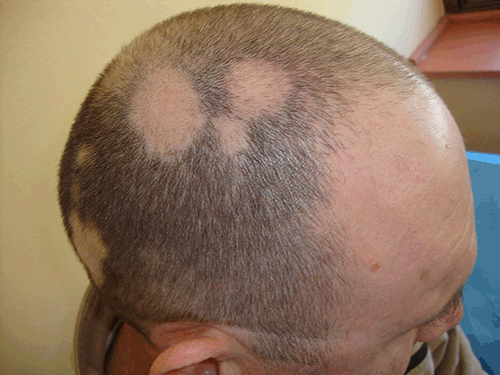
Figure 2. Multiple circular patches of alopecia areata in a man aged 42 years
Another distinguishing factor in patients with areata alopecia is that their nails may demonstrate nail pitting (dystrophic plate changes), whereas patients with TTM have normal nails. Tinea is also a common misdiagnosis. A KOH and Woods lamp examination can rule out non-inflammatory tinea. Trichotillomania in the scalp (Figure 3) must also be differentiated from androgenetic alopecia, in which the hair loss is usually bilateral and telogen effluvium, in which it is diffuse. Well defined, unilateral alopecia plaques are more characteristic of TTM. Differential diagnoses include traction alopecia, mucinous alopecia, lichen planopilaris, discoid lupus erythematous, pseudopelade, folliculitis decalvans and syphilis.
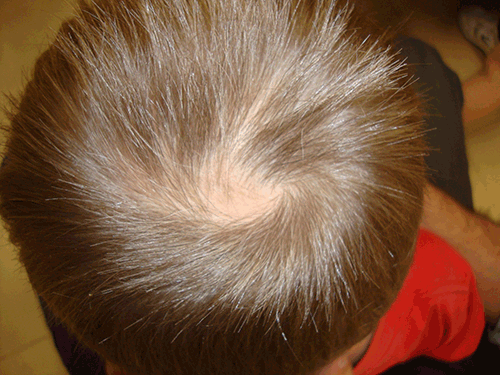
Figure 3. Patch alopecia in the occipital area in a male aged 7 years. The hair-pull test was negative. The diagnosis was consistent with TTM
Answer 5
Management depends mainly on the age of onset. In preschool aged children, where pulling or playing with the hair is a similar comfort to thumb sucking, the most effective management is to inform and advise the parents. As there is usually spontaneous resolution with increasing maturity, parents should be supportive and avoid punishing the child´s behaviour. In infants, loving care, maternal skin contact, and the availability of transitional objects (eg. toys) also work well.5
As older children and teenagers may not notice their habit, it is important to carefully establish the diagnosis. In most cases, reassuring the patient that their hair is normal and will grow when they stop pulling is enough. Carefully consider the possibility of a mental health problem and refer appropriately. Cognitive behavioural therapy (CBT) is the usual first line therapy for psychological causes.6 The three essentials of CBT are:6,7
- stimulus control
- self monitoring: the patient keeps a record of hair-touching conduct8
- habit-reversal training: the patient should establish opposing responses, which are incompatible with hair pulling.
No medication has been approved for the treatment of TTM. Drug therapy has largely been disappointing. The classes traditionally tried included selective serotonin reuptake inhibitors and tricylic antidepressants.6 A more recent very small trial using an antipsychotic was encouraging.9
Answer 6
The prognosis mainly depends on the age of onset of the problem. In young children, the prognosis is excellent. Even in late childhood and adolescence, the prognosis is usually good. In adult patients, the prognosis is poor and cure uncommon.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.