Kawasaki disease mainly affects children aged 6 months to 4 years and has surpassed acute rheumatic fever as the most common cause of paediatric acquired heart disease in the industrialised world, causing cardiac complications in up to 25% of untreated individuals.3 Timely treatment reduces coronary artery damage by up to 75%.4
The aetiology of Kawasaki disease is unknown. It is believed that ubiquitous infection(s) trigger an abnormal host inflammatory response, leading to Kawasaki disease in genetically predisposed children. The diagnostic criteria include fever of at least 5 days duration, together with four of five cardinal clinical criteria,5 which are often sequential and may appear over a number of days.6 Although 80% of cases occur between 6 months and 4 years of age, it is important to remember the diagnosis in infants and older children. Occasionally Kawasaki disease is reported in neonates, adolescents and adults.3
The diagnosis is often delayed or may be missed entirely, as it relies on clinical features, some of which are common in children with fever due to other infections.2 In addition to the classic or cardinal diagnostic features, Kawasaki disease is often accompanied by concurrent infections, as well as diarrhoea, abdominal pain and arthralgia; common clinical features that may mislead clinicians.7
Why is Kawasaki disease important?
With the potential for significant long term cardiac sequelae, it is imperative that Kawasaki disease be considered, diagnosed and treated promptly. Several cases of myocardial infarction in young adults have been attributed to ‘missed’ Kawasaki disease in childhood,8 which resulted in coronary artery aneurysms.
Mild, diffuse dilatation of coronary arteries usually begins on day 10 from fever onset. If left untreated, 25% of these patients progress to true aneurysms, with 1% becoming ‘giant aneurysms’ (>8 mm internal diameter). These giant aneurysms have the worst prognosis, with risk of acute thrombosis and long term risk of myocardial ischaemia. Aneurysms may occasionally occur in other arteries, particularly the axillary artery. In addition to coronary artery involvement, children may develop other acute cardiac complications, including myocarditis, ventricular dysfunction, valvular regurgitation,9 pericardial effusion and although rare, cardiac tamponade.10
The in-hospital mortality rate with Kawasaki disease is low (~0.17%), with almost all attributed to cardiac sequelae. Peak mortality occurs at 15–45 days from fever onset11 – the time when coronary artery vasculitis coincides with marked thrombophilia and a hypercoagulable state.
What are the diagnostic criteria?
The diagnosis is made by the presence of fever for at least 5 days (onset of fever considered day one of illness) and at least four out of the following five diagnostic criteria that often appear sequentially:
- conjunctival injection – redness without exudate, typically bilateral with perilimbal sparing (a ring of normal conjunctiva around the iris). This appears early in the illness and due to its transitory nature should be sought on history as well as clinical examination. Photophobia and eye pain are seldom present
- erythema of oral and/or pharyngeal mucosa – may include strawberry tongue, red pharynx and/or red and cracked lips, but no tonsillar exudates or ulcers
- erythema and oedema of hands and feet – this is a common feature but may only manifest as failure or refusal to weight-bear. In the sub-acute phase of Kawasaki disease (from about day 10 onward), there may be desquamation of the fingers and toes
- polymorphous skin rash – usually begins in the nappy area (where there may be desquamation early in the disease) and spreads to involve the trunk, extremities and face. Rash may be maculopapular, annular or scarlatiniform. Non-blanching or vesicular rashes are not usually seen
- cervical lymphadenopathy – often unilateral and large, with node size >1.5 cm. This is the least frequently seen criteria, but is more common in older children.
What is incomplete Kawasaki disease?
Incomplete Kawasaki disease refers to infants satisfying fewer than four classic diagnostic criteria. It is sometimes incorrectly referred to as ‘atypical’ Kawasaki disease, but this term is reserved for cases with unusual features, such as shock or renal failure. Incomplete Kawasaki disease occurs in approximately 15% of cases, although it may be missed and the true incidence is likely higher.6 Incomplete Kawasaki disease is more prevalent in children aged less than 1 year, and these patients have a higher risk of developing cardiac sequelae.12 The overall incidence of coronary complications in incomplete Kawasaki disease is at least similar to that of the complete disease,13 highlighting the importance of a high index of suspicion, together with prompt referral when Kawasaki disease is suspected, even if the full diagnostic criteria are not met.
When should I suspect Kawasaki disease?
Fever
Kawasaki disease should be suspected in any child with a persistent fever with no other likely explanation. The pyrexia associated with Kawasaki disease is typically high (often greater than 39°C), remittent and unresponsive to antibiotic therapy, and usually also unresponsive to antipyretics. This pattern of fever may help to distinguish Kawasaki disease from a common viral exanthem.
Skin manifestations
Rash and peeling (desquamation) of the nappy area rash is common in the acute phase. Periungal (fingers and toes) desquamation appears 1–3 weeks after fever onset (convalescent phase), by which time treatment would be delayed. The clinical features may develop over days and are not always present concurrently. Frequent review and careful and repeated history, specifically asking about suggestive features, are important in making the diagnosis. Figures 1 to 3 provide examples of Kawasaki disease presentations.
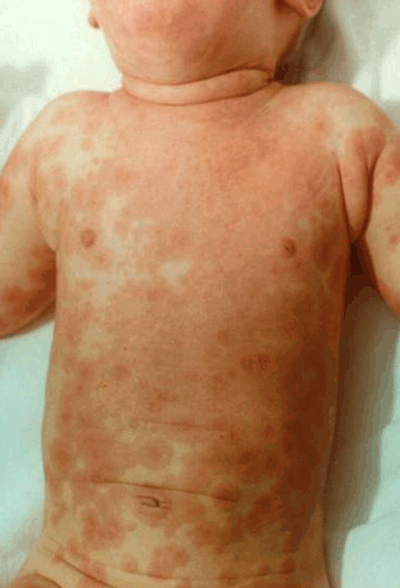
Figure 1. Polymorphous skin rash affecting the trunk in a child with confirmed Kawasaki disease
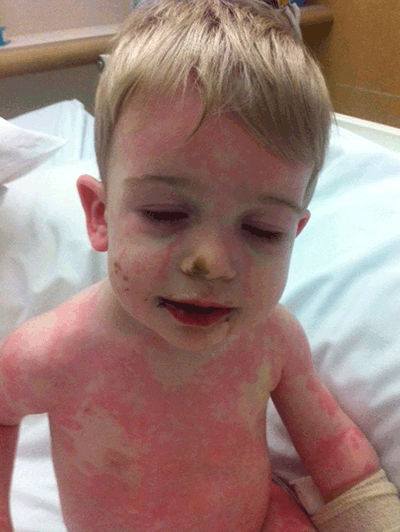
Figure 2. Dry, red lips and polymorphous rash in a child with confirmed Kawasaki disease
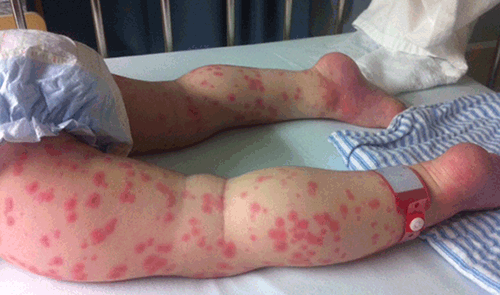
Figure 3. Extremities demonstrating erythema, oedema and rash in a child with Kawasaki disease
Irritability
Extreme irritability – more so than in other febrile illnesses – is characteristic of Kawasaki disease. Other suggestive features include inflammation of a recent Bacille Calmette-Guerin (BCG) scar and sterile pyuria (leucocytes on urine microscopy but sterile by standard culturing techniques).14
Features that make the diagnosis less likely include non-blanching rash, bullous or vesicular lesions, oral ulceration, generalised lymphadenopathy, and a prompt response to antibiotics.
General practitioners should not wait for the fever to persist and may make the diagnosis and referral before 5 days if other clinical features are present, prompting a strong index of suspicion.
What are the common pitfalls in the diagnosis of Kawasaki disease?
Early clinical features of Kawasaki disease mimic other self-limiting febrile illnesses and the diagnosis may be difficult. Non-cardinal diagnostic features (eg. diarrhoea, vomiting, abdominal pain and arthralgia) are common and do not exclude the diagnosis.7 Furthermore, microbiologically confirmed concurrent infections may be present in up to one-third of cases at presentation.15 Antibiotics are often given for presumed bacterial lymphadenitis, without effect, and as the rash may take some days to develop, it is often mistaken as a drug reaction. Sterile pyuria may be mistaken for a urinary tract infection.
Important differential diagnoses for a rash in the aforementioned regions in the setting of fever are toxic shock syndrome and group A streptococcal infections, particularly scarlet fever. Staphylococcal scalded skin syndrome also shares some features with Kawasaki disease, but usually spares the mucous membranes.16
What should I do when Kawasaki disease is suspected?
There is no specific diagnostic test. However, certain laboratory findings are characteristic, although none have a high individual positive predictive value. Referral should not be delayed by awaiting results if there is reasonable clinical suspicion or concern.
Characteristic laboratory findings include:
- raised white cell count (predominantly a neutrophilia)
- markedly elevated erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP)2
- hypoalbuminaemia
- anaemia (normocytic, normochromic)
- mildly raised liver enzymes (predominantly alanine aminotransferase)17
- normal platelet count that increases markedly by the second week of illness.
Thrombocytosis – like periungual desquamation – is a late feature and is not helpful in the acute diagnosis.
Indications for referral to a paediatric emergency department include:
- high fever in an irritable child with skin manifestations
- prolonged fever and at least four of the five diagnostic criteria
- prolonged fever but less than four clinical criteria and no alternative explanation or diagnosis
- if desquamation develops 1–2 weeks post-onset of fever
- any child aged less than 6 months with fever lasting more than 7 days, even if other features are absent
- high clinical index of suspicion for Kawasaki disease.
What is the treatment?
Kawasaki disease should be treated in an inpatient paediatric facility by those familiar with the condition and its management. Intravenous immunoglobulin (IVIG) is the only proven therapy that improves coronary artery outcomes, reducing the incidence of coronary artery aneurysms to 2–5%.4 It is preferably given within 10 days of fever onset, but should be given at any time if the child is febrile or there are laboratory features of persisting inflammation. Intravenous immunoglobulin usually causes rapid defervescence and clinical improvement in the majority (~80%) of cases.18
Aspirin is usually given in addition to this treatment, although its use has never been subjected to a randomised controlled trial and the dosing regimen is somewhat controversial.19 Kawasaki disease that does not respond to the initial IVIG is usually treated with a further IVIG dose, then (if necessary), with pulsed methylprednisolone20 or consideration of anti-TNF therapy.21 Expert advice should be sought in these cases. It should be noted that following commencement of IVIG, the ESR is usually elevated and cannot be used to monitor response;18 CRP is a better indicator of acute inflammation.
Echocardiography (ECHO) may be performed during the initial admission and is used as a baseline for coronary artery dimensions and morphology. Occasionally large aneurysms are identified at presentation, although aneurysms are usually not evident on ECHO within 10 days of fever onset. Other features on initial assessment in the acute phase include coronary artery ectasia, perivascular brightness, and lack of normal coronary artery tapering.22 Some patients may also have evidence of myocarditis and/or myocardial dysfunction. The frequency of echocardiographic assessment is determined by local practice and findings, but they are usually performed at least at presentation, and after 6–8 weeks of the illness. Serial ECHOs are performed to monitor progression, and long term treatment is dictated by the extent of coronary artery involvement.
Following resolution of fever, aspirin is continued in a low ‘anti-platelet’ dose (3–5 mg/kg once per day), at least until the ECHO at 6–8 weeks demonstrates no evidence of cardiac pathology.23 Some children may need long term treatment with aspirin or additional anticoagulation. It should also be noted that there is a theoretical risk of non-steroidal anti-inflammatory drugs (NSAIDs) antagonising the anti-platelet effect of low-dose aspirin; however, new adult data suggest this may not be the case, and it is yet to be studied in the paediatric setting. Furthermore, there is a small risk that salicylates are associated with an increased risk of Reye syndrome in the setting of active viral infection, although only two cases of Reye syndrome in patients with previous Kawasaki disease have been reported in the literature. Varicella and annual influenza immunisation should be considered in children on long term aspirin therapy; expert advice should be sought.
In addition, anti-viral IgG in IVIG may interfere with the efficacy of live vaccines (measles, mumps, rubella [MMR], and varicella). The current recommendation is to administer varicella and annual influenza vaccines immediately and to delay MMR vaccination for 11 months after the administration of IVIG, at which point varicella vaccine should be readministered to ensure adequate immunogenicity. Parents should be advised to visit their local immunisation centre for further advice and to re-present if an unimmunised child is exposed to varicella.
What is the long term management?
Parents should be reassured that Kawasaki disease is not contagious and that most children recover fully, without any long term cardiac or other sequelae. Some patients may require long term treatment under specialist supervision. Approximately half of the coronary artery aneurysms resolve within 1–2 years,24 but stenosis of the affected vessel (at entrance and exit to aneurysmal area) may occur with healing.25 Occasionally this necessitates more intensive medical or surgical therapy. The long term effects of Kawasaki disease on adult coronary artery disease are unclear, as data from cohort studies are not yet available. The opportunity should be taken to advise families of the potentially increased long term cardiovascular risk and the need for minimisation of risk factors. It is prudent to advise families to reduce known, modifiable factors for cardiovascular disease, such as obesity, smoking and lack of exercise, and to consider measuring plasma lipids and blood pressure in early adulthood, or earlier if there is a family history. Mild behavioural disturbances in the weeks following Kawasaki disease usually resolve without specific therapy. Children with previous Kawasaki disease may desquamate with subsequent febrile illnesses, although in the absence of other features this does not represent a true recurrence, which is rare. Expert advice may be sought if the diagnosis is unclear.
Key points for practice
- Kawasaki disease is characterised by a prolonged fever plus four of the following five diagnostic criteria: polymorphous rash, non-exudative conjunctivitis, oral-mucosal involvement, extremity desquamation and cervical lymphadenopathy.
- The diagnosis should be considered in any highly irritable, febrile child with skin manifestations.
- Treatment with IVIG reduces coronary sequelae significantly and should be initiated promptly.
Resource
Parent information sheets and support groups are available via The Royal Children’s Hospital website at www.rch.org.au/kidsinfo/fact_sheets/Kawasaki_Disease/.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.