Clinical presentations of pain
Gallstones
Gallstones are a common problem, with an estimated prevalence of 25–30% in Australians over the age of 50 years.1 Risk factors for the development of gallstones include:
- female gender
- increasing age
- family history
- rapid changes in weight
- ethnicity.
Most people with gallstones do not experience pain, with only about 6% undergoing a cholecystectomy over a 30 year period in one observational study.2 Confirming that the gallbladder is the source of pain can be challenging.
Typical biliary colic is pain that increases in intensity following the ingestion of fat. The colic lasts for minutes to hours, and is sometimes associated with nausea, bloating and, occasionally, vomiting. The pain may also radiate around to the back. Simple analgesics will usually control the pain. Biliary colic is self-limiting and dissipates over time. For most patients, the colic does recur, but the interval is extremely variable between patients and can be days to months. Occasionally, patients will experience a pattern of rapid relapses and remission of symptoms over several days, which is often associated with an impacted stone at the gallbladder neck.
Some patients with gallstone-derived pain present with atypical features. The location, duration, radiation and food associations of the pain can be atypical. The more atypical the pain, the less likely that it will be relieved by cholecystectomy. Patients with atypical pain and gallstones should have differential diagnoses considered before proceeding with cholecystectomy.
Acute cholecystitis
Acute cholecystitis presents with severe pain associated with a raised temperature, tachycardia, tenderness in the right upper quadrant (especially on inspiration) and occasionally, positive blood cultures. Early cholecystectomy is usually recommended for acute cholecystitis.3,4
Acalculous cholecystitis
Acute acalculous cholecystitis is sometimes seen in the very ill inpatient, often in the setting of diabetes. It is caused by ischaemia and a degree of acute gallbladder distension associated with fasting.
Chronic acalculous cholecystitis presents with typical biliary pain, but no stones on ultrasound. If the ultrasound shows sludge, polyp(s), or evidence of inflammation, the patient should be referred for cholecystectomy. If the ultrasound is normal, a nuclear medicine gallbladder excretion study can help differentiate those patients who might benefit from cholecystectomy. These patients should have differential diagnoses considered before surgery.
Common bile duct stones
The passage of stones into the common bile duct (CBD) occurs in some patients who have small stones. Very small stones can pass unnoticed through the Ampulla of Vater, with some stones causing enough disruption of flow to cause pancreatitis. Larger stones present with jaundice with or without cholangitis, or as an incidental finding of abnormal liver function tests (LFTs), or on imaging.
The management of CBD stones depends on local expertise. Many patients with CBD stones without cholangitis are managed laparoscopically at the time of cholecystectomy. Peri-operative endoscopic retrograde cholangiopancreatography (ERCP) is an alternative strategy.5
Cholangitis
Cholangitis presents as acute biliary pain associated with sepsis and jaundice. Patients with cholangitis require urgent ERCP to drain the biliary system. Patients with stones should proceed to cholecystectomy once their sepsis has settled.
Mirizzi syndrome
Mirizzi syndrome is dilated bile ducts caused by a stone impacted in the gallbladder neck, with inflammation and swelling that compresses the common hepatic duct. The stone can erode into the common hepatic duct, making surgery complicated and necessitating biliary reconstruction. Mirizzi syndrome can often be temporarily managed with ERCP, stenting and antibiotics.
Gallstone pancreatitis
Patients presenting with pancreatitis due to gallstones usually have abnormal LFTs. Those with co-existing cholangitis should have an urgent ERCP to decompress the biliary tree. Cholecystectomy is performed as soon as possible after resolution of the pancreatitis.
Porcelain gallbladder
Porcelain gallbladder refers to calcification in the wall of the gallbladder, and presents a substantial risk for gallbladder cancer. Cholecystectomy is recommended in fit patients.
Asymptomatic gallstones
Patients with gallstones without symptoms should not be treated. They should be advised as to what symptoms to watch for. Cholecystectomy in asymptomatic cases is more hazardous than expectant care, as most patients do not develop symptoms.2 Cholecystectomy is reasonable in some asymptomatic patients (particularly those who are diabetic) already undergoing other abdominal surgery, and in rare cases where there is a high risk for gallbladder cancer.
Gallbladder polyps
The ultrasound finding of a non-shadowing polypoid lesion attached to the wall of the gallbladder is termed a ‘polyp’. Most are a complex of small cholesterol crystals. Occasional adenomatous polyps occur, and a fraction of these may progress to cancer. The polyps with greatest concern are those that are larger than 1 cm, have a wide base, or are associated with focal thickening, distortion or mass of the gallbladder. Polyps found in elderly patients are more concerning than those found in younger patients. Polyps without gallstones are less concerning than those with them. A general recommendation is that polyps less than 10 mm can be observed by an ultrasound every 6 months for 2 years.6 Patients with polyps larger than 1 cm, or larger than 5 mm in those with primary sclerosing cholangitis or inflammatory bowel disease, should be referred for cholecystectomy.
Work-up for suspected gallstones
Figure 1 illustrates the management of patients with biliary pain. An ultrasound determines the presence of gallstones, and can also assess the size of the bile ducts, gallbladder morphology and calcification, and other organs. It may also identify stones within the bile duct.
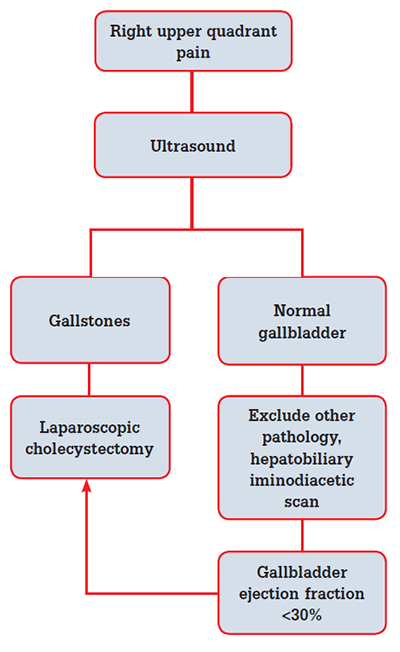
Figure 1. Management of patients presenting with biliary pain
Ultrasound findings consistent with inflammation of the gallbladder include inducible pain on direct compression (sonographic Murphy’s sign), thickened gallbladder wall, adenomyomatosis and peri-cholecystic fluid.
Patients with symptomatic gallstones should have LFTs before surgery. Liver function abnormalities are sometimes reflective of stones within the CBD.
Treatment of gallstones
Cholecystectomy is usually performed laparoscopically. Laparoscopic cholecystectomy has been refined over the past 20 years, but the principles are the same. Identification and control of the cystic duct early in the operation without damage to the hepatic ducts or arteries is the most important step. Cholangiography at the time of cholecystectomy helps to diagnose choledocholithiasis, or abnormal anatomy, and assists with the identification of a duct injury.
The difficult gallbladder
During surgery it may become apparent that a formal cholecystectomy would be dangerous to the patient. When severe inflammation makes the identification of anatomical structures difficult or impossible, a sub-total cholecystectomy is often performed. This leaves some of the gallbladder behind at the neck and on the liver. All stones are removed if possible. Postoperative issues after sub-total cholecystectomy are rare.
Patients with acute cholecystitis who are unfit for surgery can have their gallbladder decompressed by percutaneous cholecystostomy. This is a radiologically placed drain that passes through the liver into the gallbladder. It is possible to dilate the tract and remove stones until the gallbladder is draining normally.
Complications of cholecystectomy
Bile leak
Bile leak usually presents early, often before discharge from hospital. It is considered when there is worsening pain within the first week after cholecystectomy. Bile leak occurs in 1–2% of patients having a laparoscopic cholecystectomy, and is usually due to a ‘pin hole’ leak at the cystic duct stump or a ‘twig’ of the hepatic biliary tree within the gallbladder fossa. In the presence of peritonitis, washout and drainage is mandatory, followed by endoscopic trans-papillary stenting. The stent prevents pressure build-up within the ducts, and allows small leaks to heal.
Bile duct injury
Bile duct injury is an injury to a major bile duct draining the liver. The rate of these injuries has been reported to be as high as 1 in 200 cases of laparoscopic cholecystectomy. Pre-disposing factors are surgical inexperience, acute pathology and unrecognised abnormal anatomy. Managing this bile duct injury is complex, and is best carried out in a hepatobiliary unit.
Conversion to open cholecystectomy
Conversion to open cholecystectomy is used when there is uncertainty about the anatomy or pathology, or because of bleeding or adhesions. Typical conversion to open cholecystectomy rates in the elective setting are less than 5%.
Life after cholecystectomy
The vast majority of patients will lead a normal life after cholecystectomy. It can take up to 6 weeks for intestinal symptoms, such as mild indigestion, gas and loose stools, to settle completely. Over time, the storage of bile is affected by dilation of the biliary tree, with the papilla still opening in response to fat.
Some patients experience more frequency of stool, but rarely outside the normal range. New troublesome diarrhoea is a common concern, but there is conflicting data about its incidence, with studies suggesting an incidence as low as 1% or as high as 17%.7 Rare cases that do not resolve with simple measures, such as increased fibre and fat reduction, should be referred to a gastroenterologist to rule out other conditions and to consider a trial of bile acid therapy.
Recurrent pain
Recurrent pain after cholecystectomy is often termed ‘post-cholecystectomy syndrome’. It is important to differentiate patients who have ‘new’ pain from those whose pain has persisted despite cholecystectomy. The onset of new pain soon after cholecystectomy will sometimes be due to a bile leak or, occasionally, a retained CBD stone. Those with persisting pain may have had asymptomatic gallstones co-existing with another cause of pain.
Investigations for post-cholecystectomy pain are listed in Table 1. While a referral back to the operating surgeon is indicated, a gastroenterologist referral is also helpful to assist with both the diagnosis and treatment.
Table 1. Timing of recurrent pain with possible diagnoses and useful investigations
| Early (within 1–2 weeks of surgery) |
- Retained common bile duct stone
- Bile leak
- Postoperative infection
|
- Ultrasound
- Liver function tests
- Surgical review
|
| Late |
- Retained stone
- Peptic ulcer disease
- Colonic pathology
- Biliary dyskinesia (spasm of the sphincter of Oddi)
|
- Ultrasound
- Liver function tests
- Surgical, gastroenterologist review
- CT scan, magnetic resonance cholangiopancreatography
- Upper and lower gastrointestinal endoscopy
|
Differential diagnoses include bile leak, retained stone, abscess, biliary dyskinesia, peptic ulcer disease, irritable bowel syndrome, non-ulcer dyspepsia and colonic problems.
Key points
- Gallstones are a common presentation in general practice.
- The link between abdominal pain and gallstones is sometimes difficult.
- Elective cholecystectomy for asymptomatic gallstones is not usually indicated. Work-up for symptomatic gallstones should include an ultrasound and liver function tests.
- Laparoscopic cholecystectomy is the best treatment for symptomatic stones.
- Early cholecystectomy in the setting of acute cholecystitis is the most cost effective approach.
- Recurrent or new post-cholecystectomy pain often requires specialist referral to diagnose and manage.
Competing interests: None.
Provenance and peer review: Commissioned; externally peer reviewed.