Early detection and treatment improves vision outcomes and psychosocial wellbeing for children with strabismus. Nonetheless, many cases of strabismus go unrecognised. As patients with paediatric strabismus usually present before school age (with an average onset at 1–4 years), population-based pre-school screening programs have been advocated as a way to reduce the rate of untreated strabismus and amblyopia.3,6 Nonetheless, the cost–benefit value of these public health programs is the subject of ongoing debate,6 and the lack of a national Australian screening program necessitates that individual assessment of children currently falls into the realms of primary care clinicians, such as general practitioners (GPs), and maternal and child health nurses. For this reason, GPs should be alert to this common problem and be familiar with practical screening tests that may unmask situations requiring specialist referral.
Causes of strabismus
Strabismus can be either primary or secondary (acquired). Common causes of childhood strabismus are listed in Table 1. Recognised risk factors for primary strabismus include a family history of strabismus, premature birth and a low birth weight.7 Secondary strabismus is often associated with neurological pathology, such as intracranial tumours, head trauma, infection and autoimmune disorders.1
Table 1. Common causes of strabismus1
| Primary causes of strabismus | Secondary causes of strabismus |
|---|
Idiopathic strabismus
Congenital syndromes |
Cranial nerve palsies (CNIII, IV, VI)
Orbital fracture
Intracranial bleed
Intracranial/intraorbital/intraocular mass (benign or malignant)
Intracranial infection
Grave’s disease
Myasthenia gravis
Diabetes mellitus
Amblyopia
Toxins and heavy metal poisoning
Post-vaccination |
Amblyopia is a recognised consequence of established strabismus (either primary or secondary). However, amblyopia can paradoxically also be a cause of secondary strabismus, as a degraded visual experience in one eye may result in that eye drifting out of correct alignment.3 Uncorrected refractive abnormalities, such as myopia and hyperopia, may also result in secondary strabismus via a similar mechanism.6
Types of strabismus
The most common type of strabismus involves horizontal misalignment of the eyes, although vertical misalignment also occurs.7 Ocular deviation may be manifest (tropia) or latent (phoria). Manifest ocular deviation can be present in all directions of gaze (comitant) or only present in specific directions of gaze (incomitant) (Table 2).
Table 2. Strabismus terminology1
| Terminology |
|---|
eso- = Nasal horizontal deviation (relative to fixing eye)
exo- = Temporal horizontal deviation (relative to fixing eye)
hyper- = Superior vertical deviation (relative to fixing eye)
hypo- = Inferior vertical deviation (relative to fixing eye)
tropia = Manifest disorder of ocular alignment
phoria = Latent disorder of ocular alignment
comitant = Ocular deviation present in all directions of gaze
incomitant = Ocular deviation only present in specific directions of gaze
amblyopia = Clinically defined as a 2-line difference from best corrected visual acuity in a structurally healthy eye |
Manifest symptoms may be either constant or intermittent. Intermittent strabismus can follow a fluctuating course, with symptoms often exaggerated by fatigue. Symptoms may also vary over time, and ocular misalignment that seemed well controlled in early childhood may become more apparent and frequent as the patient grows older.7 For this reason, all patients with a known diagnosis of strabismus require ongoing evaluation.
Differential diagnosis
The most common differentials for strabismus in a general practice setting are ocular instability of infancy and pseudostrabismus.
Newborns often present with unsteady ocular alignment, which is referred to as ocular instability of infancy. This may last up to 3 months and usually presents as a lateral ocular deviation of less than 15°. Any ocular deviation greater than 15° or persisting for more than 3 months is considered abnormal.3
Pseudostrabismus is a condition where unusual facial architecture creates the optical illusion of strabismus, such as when telecanthus (a broad nasal bridge) or epicanthal folds obscure the nasal sclera. If in doubt, a GP is advised to refer the patient to a specialist for assessment.
History
The history aims to distinguish between primary and secondary causes of strabismus, and to screen for red flag features suggesting recent trauma or serious intracranial pathology. New strabismus in a school-aged child is uncommon and necessitates further neurological investigations.3
The key areas on history to explore include the obstetric and developmental history. The medical history should include a focus on any history of malignancy or autoimmune conditions, exposures, vaccinations, and whether the child has been generally well or if there has been unexplained illness. Any history of trauma, particularly to the head, orbit or periorbital area should be elicited.
In regards to vision, any previous visual testing and the outcome are relevant. A detailed history of the onset of symptoms, including any associated signs, such as gait disturbance, nystagmus, decreased visual acuity or diplopia is relevant. The pattern of symptoms is important, such as whether the strabismus is constant or intermittent. If intermittent, consider whether the symptoms have been changing in frequency, and whether they are dependent on direction of gaze, or exaggerated by fatigue.
Screening tests
In the general practice setting, screening for strabismus involves four practical tests: the light reflex test, the red reflex test, the cover test and the uncover test.1 The only equipment required is a direct ophthalmoscope and a torchlight.
The light reflex test1
The child is placed on their parent’s lap. The doctor stands at a distance of 1 m in front of the child, holding a small light. The child’s attention is directed to the light. The position of the light’s reflection in each of the child’s eyes is noted and compared. Normal ocular alignment will generate an identical light reflection in each eye. Deflection of the light reflex indicates abnormal ocular alignment, with each 1 mm of deflection equivalent to 15–20 prism diopters deviation (Figure 1).
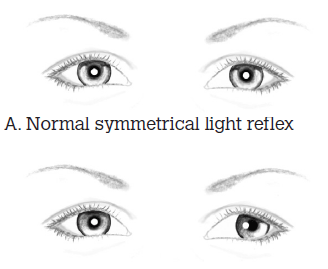
Figure 1. The light reflex test
The red reflex test1
The doctor stands at a distance of 0.5 m in front of the child, holding a direct ophthalmoscope (set at 0). The child’s attention is directed to the ophthalmoscope and the doctor attempts to visualise the red reflex of both eyes simultaneously. Both red reflexes should be identical. Inequality in size, shape or colour is abnormal (Figure 2).
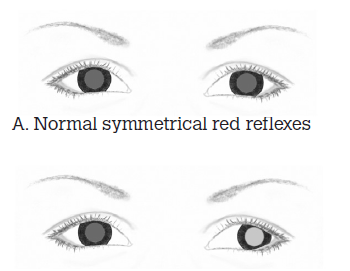
Figure 2. The red reflex test
The cover test1,8
The doctor stands in front of the child and directs the child’s attention to a target (eg. a light or a toy). The doctor covers one of the child’s eyes and closely observes the uncovered eye for corrective movement. When the fixating normal eye is covered, a manifest abnormal eye must move from its deviated position and take up correct fixation. Accordingly, movement indicates that manifest strabismus is present in the uncovered eye (a tropia). The cover test is repeated on each eye (Figure 3).
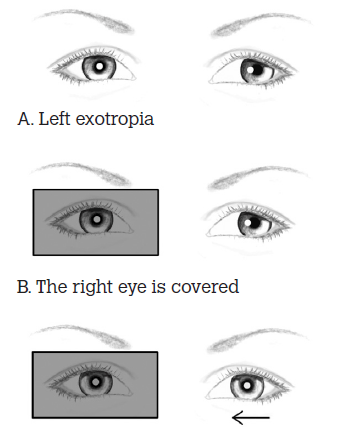
Figure 3. The cover test
The uncover test1
The doctor covers one of the child’s eyes for 5 seconds and directs the child’s attention to a target. The cover is then quickly removed. The newly uncovered eye is closely observed for corrective movement. A latent abnormal eye will drift into a deviated position when covered. After it is uncovered, the abnormal eye must then return to correct fixation. Accordingly, movement indicates that latent strabismus is present in the newly uncovered eye (a phoria). The uncover test is repeated on each eye (Figure 4).
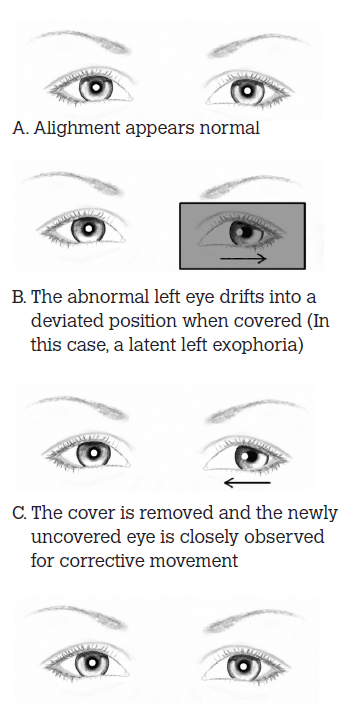
Figure 4. The uncover test
Management of strabismus
All paediatric patients with newly diagnosed strabismus require timely referral to an ophthalmologist for a comprehensive assessment of visual function. Any patient with red flags on history or examination should be referred urgently for specialist investigation.
Specific visual rehabilitation programs will depend on a number of factors, including the precise type of ocular deviation involved and whether the strabismus is primary or secondary.3 Non-surgical interventions commonly include refractive error correction with spectacles or contact lenses, and amblyopia therapy with patching or atropine penalisation. Other uncommon interventions include the use of prisms in glasses, behavioural eye exercises and the use of intramuscular botulinum A neurotoxin.3,5 Surgical correction of ocular alignment is commonly recommended and is well tolerated as a day procedure, with minimal post-operative discomfort. Treatment goals are primarily to prevent amblyopia and achieve binocular vision with functional depth perception (stereopsis), and secondarily to achieve better cosmesis.4
Key points for practice
- Patients with strabismus may suffer functional and psychosocial problems related to their condition.
- Early recognition and referral by GPs is important as visual pathways may become permanently impaired if not addressed early.
- All children with strabismus should be referred to an ophthalmologist for further assessment and visual rehabilitation.
- The new onset of strabismus may be a red flag for serious intracranial or intraocular pathology.
Competing interests: None.
Provenance and peer review: Not commissioned; externally peer reviewed.
Acknowledgments
The author wishes to thank Foad Botan for creating all the medical illustrations used in this article.