A study of access to health care services by Deaf people, commissioned by the Australian Government, revealed that, on average, Deaf Auslan users went to a doctor 8.7 times in the 12 months preceding the study.6 Individual GPs consulted as part of the same study acknowledged that there was a high risk of misunderstanding and incorrect treatment or management of the condition if an Auslan interpreter was not present during more complex medical consultations.6
Previous research has shown that even between patients and health care practitioners who share a common language background, misunderstandings and miscommunications may arise because patients may not fully understand the terms used by their health care practitioners.7 United States research shows that this is more often the case for Deaf people, as they typically have low proficiency in English and limited access to public health information.8 This means that the average Deaf person generally experiences a ‘lower level of English literacy, a smaller fund of healthcare knowledge, and fewer health education opportunities than his average hearing counterparts’.9
International studies have found that Deaf people generally have poorer physical health than the general population; they make more GP appointments; they are not satisfied with communication with health care providers; they do not adequately receive preventative health care messages and are less satisfied with many aspects of the service they receive.9 Higher English literacy is generally positively associated with preventative health knowledge due to healthcare information being primarily available in English, whether that be face to face, in print or via television.10 Many Deaf people may lack the requisite background information necessary to understand and evaluate health care information presented through captioned media as it is presented in English.11 Deaf people are at risk of health complications because of a lack of access to information about ongoing treatment and maintenance of their health.12-14
At present, a wealth of preventative and ongoing health care information is translated into various languages. None of this information is currently translated into Auslan. This study sought to gain an in-depth understanding of whether Deaf Australians who use Auslan as their primary language feel that they can sufficiently access preventative and on-going healthcare information, and how essential they feel it is to access information in Auslan.
Method
A qualitative, inductive approach was used, as it enabled an in-depth, phenomenological exploration of the experiences of Deaf Auslan users,15 allowing participants to discuss issues from their own perspective. The conceptual framework for the study was a participatory approach.16 Community-based participatory research is an established effective methodology for health-related research17 and has been used effectively with Deaf sign language users.18 The participatory approach included forming an advisory group with key stakeholder group representatives, including Deaf community organisations, Auslan interpreter associations and service providers, and experts in deafness, mental health, bioethics and health care research, and working with a team of five Deaf researchers located across Australia in each major city.
Sampling strategy
The Deaf researchers utilised their existing local Deaf community contacts to recruit potential participants through non-probabilistic purposeful and network sampling. The sample of interviewees in the study was just over 1% of the estimated population of Deaf Auslan users. Given that this is a qualitative study, the number of participants was not intended to be a representative sample of the Deaf community population.
Data collection technique
The Deaf researchers conducted semi-structured interviews in their local area. All the researchers attended a weekend workshop, where project objectives were discussed and the research team worked collaboratively to revise the draft interview questions; to agree on criteria for, and identify, potential participants in their home states; and to agree on a procedure for recruiting participants. The researchers also participated in interview simulations, which were video-recorded and discussed among the group in order to refine the interview procedure and to develop a consistent analytical approach. The interview procedure involved the collection of demographic information, then a series of prompt questions about participants’ experiences of accessing health care information, including how and where they access health care information, any challenges they experience and to self-report their English literacy level on a Likert scale ranging from 1 (poor) to 5 (excellent). Each interview lasted for up to 1 hour, was conducted in Auslan and filmed for later analysis.
Analysis
Video footage from each interview was uploaded into ELAN software, allowing transcription and detailed annotation to be precisely aligned with video data.19 The interview data was translated into English and analysed through a six-stage process of thematic analysis:20 (1) familiarisation with data, (2) generating initial codes, (3) searching for themes among codes, (4) reviewing themes, (5) defining and naming themes, and (6) producing the final report. Each interview was coded for key themes and then interview themes were cross-referenced to identify the most common themes.
Results
Seventy-two participants were interviewed from all six states and the ACT. Although not intended to accurately represent the population, participants were spread in terms of gender (62.5% female), age and across other variables (Table 1). In terms of English literacy, Figure 1 reveals that one-quarter of respondents rated their literacy levels as poor-to-average.
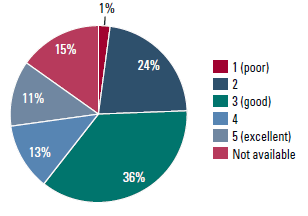
Figure 1. Self-reported English literacy
Table 1. Overview of participant characteristics
| State | Number of participants | Age range | Number of participants | Variables | Number of participants |
|---|
| ACT |
1 |
18–35 |
15 |
Indigenous |
5 |
| NSW |
22 |
36–50 |
18 |
Regional |
17 |
| QLD |
9 |
51–65 |
14 |
DeafBlind |
2 |
| SA |
1 |
≥66 |
19 |
Other disability |
5 |
| TAS |
6 |
Unknown |
6 |
Born overseas |
7 |
| VIC |
20 |
|
|
|
|
| WA |
13 |
| Total |
72 |
|
72 |
|
36 |
Eleven sub-themes were identified across the interview data, which can be collapsed into four major themes: (1) level of English literacy, (2) inadequate access to health care interpreting services, (3) inaccessible health-related services, and (4) limited access to other sources of information. For the purposes of this paper, we focus on the first theme: level of English literacy.
Sample quotes have been extracted from participant comments in order to provide insight into participants’ perceptions of their access to health care information in relation to their English skills. The quotes provided in this section are translations from Auslan into written English. Thus the quotes are not a representation of the English literacy levels of the participants. There are necessary limitations of presenting extracts of signed language data for publication in a translated written form when signed languages have no written form.21 Therefore there may be subtle aspects of the original Auslan discourse that have not been captured in written English.
Participants generally expressed limited confidence in being able to read written English notes (where they communicate with a hearing service provider in writing) or the many published and online resources and health campaigns that are assumed to be accessible by the general community. Only 9 of the 72 participants expressed confidence in their English literacy skills. Eleven participants qualified their English literacy skills, saying they could follow what they read but they commented on preferring text that was presented in bullet points or had accompanying images.
Thirty-one participants specifically expressed more significant difficulties with English and in some cases being reliant on a friend or family member to assist them to understand written information. For example:
Participant [P]: ‘I got some letters... from school and I had to get a friend to explain them to me. I also checked with a Deaf friend who works as a support worker to make sure I understood everything.’
Researcher [R]: ‘So most things you receive in writing, you request someone to sign them to you?’
P: ‘Yes, most.’
And:
‘We usually don’t understand what is written [in brochures] but we do see the pictures. If we want to understand what is written, we ask someone to explain it. That’s what most Deaf people do.’
Understandably, all participants commented on feeling more comfortable when information was accessible in Auslan. For example:
‘...sometimes, when I read information, I don’t quite understand it until it is being signed to me. I tend to understand and remember information if it was signed to me... I do read books, yes, but there are no examples. There are no explanations and I need it to be signed so I understand and remember it more easily.’
In two cases, limited English literacy was due to migration to Australia from a non-English speaking country. For example:
‘I was given a paper explaining how shingles happens and how to resolve it. But I found it hard to read because of the language and the amount of information on the page. I went home and went on the internet and found some information in [name of language]. I read that and I understood it.’
While many people may develop strategies for coping with a low level of English literacy, this also exposes the individual to potentially inaccurate information and the associated consequences of that misinformation.22 People who are DeafBlind also face the additional challenge of web-based information not being as easily accessed. For example one participant commented:
‘I have some difficulty trying to access the internet. Braille is not very convenient for the internet. Sometimes I ask people but I need to be wary of that because I am given some different information by different people. I get confused and tend to worry more because I don’t know what’s true. It is a bit of catch-22 because my English is limited and I ask people to help but [once] it went very wrong. There were misconceptions... I worried and become stressful so as a result my health deteriorated.’
Twenty-three participants expressed their frustration or inability to access desired information. One participant commented that:
‘There are barriers. Before my treatment, I was given a video. I asked if there were captions but there were none. I had to have the treatment but I didn’t have any access to the information. I only knew about the treatment from a pamphlet. The treatment was very serious and I needed full information... I am not sure if I would have taken the treatment if I had known the side effects... I would never want to go through that experience again.’
Participants were asked about the sources of information used and their preferences in relation to general information about preventative health or the maintenance of ongoing medical conditions. Table 2 summarises the sources of information mentioned according to number of participants.
Table 2. Health-related information sources
| Information source mentioned by participants | Number |
|---|
| TV |
40 |
| GP |
32 |
| Internet |
26 |
| Magazines/newspaper |
18 |
| Family |
18 |
| Deaf/signing family and friends only |
17 |
| Books |
15 |
| Friends |
14 |
| Brochures |
13 |
| Workshops |
9 |
| Deaf/signing work colleagues |
7 |
| Other health organisations |
6 |
| Deaf society/deaf club |
5 |
| Chemist |
4 |
| Community health centres |
4 |
| Work colleagues |
3 |
Forty participants mentioned television as an information source, with health-related programs such as 'Embarrassing Bodies' specifically mentioned by several participants. TV dramas such as 'Home and Away' were also referred to as a source of information when characters experienced health concerns. It was acknowledged however, that there are obvious limitations with television as a source of information, because captioning relies on English literacy. For example:
‘[Captioning on the TV] is good but it can be a bit hard to understand some of the words.’
Although mentioned by 18 participants, print media (including books, magazines and brochures) were generally not favoured because of limited English literacy. For example:
‘I do pick up brochures at the GP or the hospital. It can take me a while to fully understand them. I have to read them several times usually, to fully understand them. That's why I think we need something specific for Deaf people. Carefully worded, not quite so difficult. Plain English, with pictures.’
These findings are consistent with the literature, demonstrating that English literacy is a key barrier to Deaf sign language users in attempting to access information before, during and after a health care appointment.23,24
Discussion
It is apparent that Deaf Auslan users who participated in this study experience barriers in accessing preventative and ongoing health care information as a consequence of their English literacy skills and the lack of available information in Auslan. Deaf people rely heavily on GPs, television, family and friends. Their experiences in accessing information concerning their own health are generally problematic, in that they often feel they have a lack of information, have barriers to accessing information or do not sufficiently understand the information that they receive.
Having insight into Deaf Auslan users’ experiences of accessing health care information reveals, and confirms, the importance of:
- GPs being aware of the information access needs of Deaf patients
- interpreters being provided for all consultations
- funding being made available to provide interpreters in health service contexts outside of private medical appointments or public hospitals
- health care information being delivered in (or translated into) Auslan through the creation or translation of brochures, which could be made available through websites or on DVD.
Other recommendations to be considered include the establishment of a national online database of Auslan health-related information; considering establishing a Deaf Health Information Worker role in community service organisations; a health care information video in Auslan that explains the concepts and role of patients in preventative health and health maintenance; considering establishing a health-specific, video-based, remote interpreting service to replicate other telehealth services; and exploring the experiences of sub-groups in the Deaf community that might have different informational needs.
Limitations of the study include (1) the small sample size, which means the findings cannot be generalised to the broader Deaf community, especially Deaf children as they were not part of the sample; (2) the purposeful sampling approach may have limited the number of participants; (3) potential participants may have been reluctant to be involved as they did not want to be interviewed on film, despite assurances that the data would be anonymised; and (4) the small size of the Deaf community population may have led potential participants to decline involvement due to being an ‘over-researched’ group.
Implications for general practice
The findings of this study reveal that although great advances have been made in improving Deaf Auslan users’ access to health care services through the provision of Auslan interpreters for GP appointments, Deaf people still experience barriers in accessing preventative and ongoing health care information outside of these appointments. This is primarily due to their limited English literacy and lack of access to information provided in Auslan (either through interpreters or translated material). GPs need to be aware that English literacy of their Deaf patients may be limited, and they cannot rely on patients reading health information leaflets or attending educational workshops as a means to maintaining their health or preventing illness. GPs should ensure that Auslan interpreters are used in all medical consultations, and that their Deaf patients have the opportunity to clarify any questions about their health care during these consultations.
Competing interests: Jemina Napier has received payment from the NABS for consulting.
Ethics approval: Macquarie University Human Research Ethics Committee (reference number 5201100732).
Provenance and peer review: Not commissioned; externally peer reviewed.
Acknowledgements
This research was commissioned and funded by the NABS, and was carried out independently by the researchers who had full access to all of the data in the study. The research team included Joe Sabolcec (research coordinator) and five Deaf researchers: Josie Hodgetts, Stef Linder, Gavin Rose-Mundy, Marijana Turcinov and Linda Warby. Members of the advisory group included representatives from NABS, Deaf Australia, the Deaf Society of NSW, the Australian Sign Language Interpreters Association, and individuals who brought expertise in health communication research, health policy, indigenous Deaf people, Deaf people with mental health issues, and working with ageing Deaf people.